Here’s why some high-risk patients aren’t getting drugs to combat COVID
- Share via
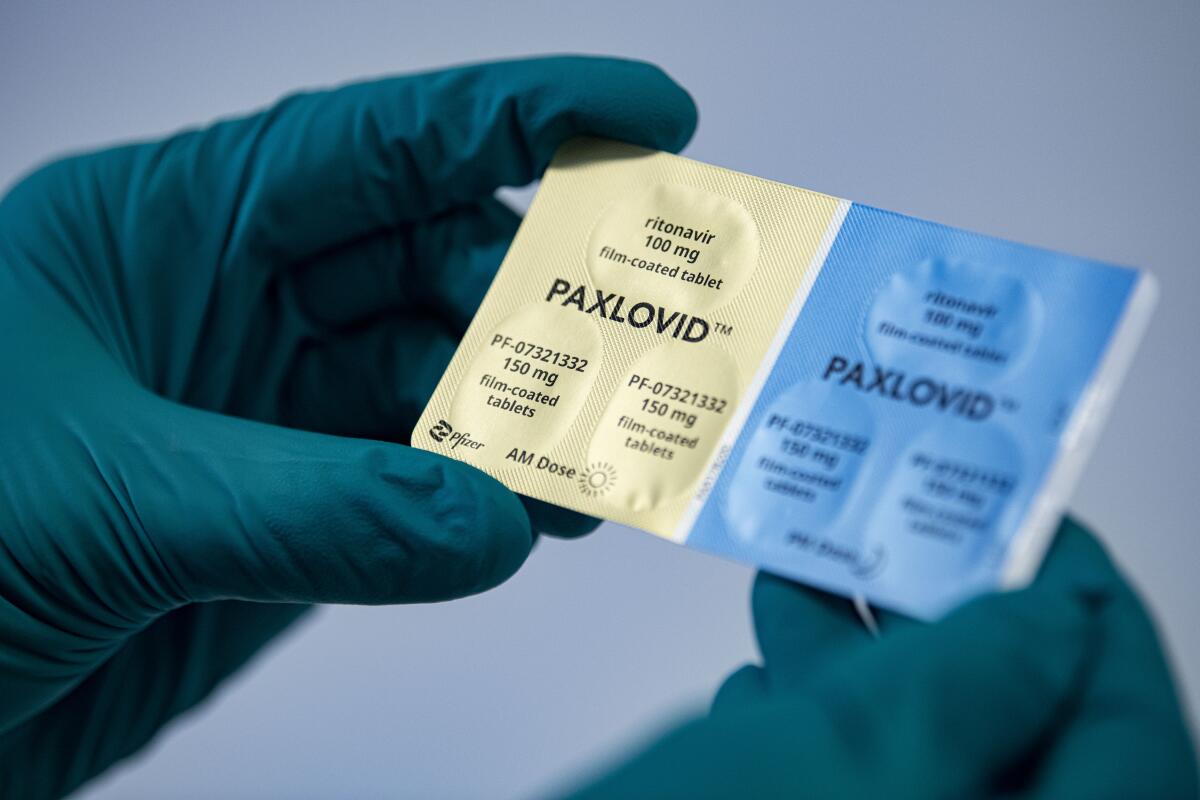
As the toll from the COVID-19 pandemic continued to mount, antiviral medications such as Paxlovid were hailed by health officials as an important way to reduce the risk of severe illness or death.
Yet the drugs have remained underused, studies have found. In Boston, a group of researchers wanted to know why — and what could be done about it.
Their new findings, published Thursday by the U.S. Centers for Disease Control and Prevention, suggest that some vulnerable patients were not offered the prescription medicines at all, and that doctors need more education to make sure the drugs get to patients who could benefit.
Researchers from the VA Cooperative Studies Program delved into records from the Veterans Health Administration to look more closely at what happened to high-risk patients who never got Paxlovid, remdesivir or molnupiravir. They focused on 110 patients who received organ transplants or had other medical conditions such as chronic lymphocytic leukemia that were likely to leave them immunocompromised and thus at greater risk from COVID-19 despite being vaccinated.
When everyone around them stops taking pandemic precautions, it gets harder for immunocompromised Americans to protect themselves against COVID.
Their analysis in the CDC’s Morbidity and Mortality Weekly Report found that 20% of those patients turned down the drugs when they were offered. But the remaining 80% of patients were never offered such treatment in the first place.
In some cases, medical providers decided not to give patients the COVID-19 drugs because they were worried about how they could interact with other medications patients were already taking, including cholesterol-lowering statins and a drug used to reduce the risk that a transplanted organ would be rejected. In other cases, doctors demurred because their patients had experienced COVID-19 symptoms for more than five days, beyond the recommended window for getting Paxlovid.
Despite public alarm about “Paxlovid rebound,” in which symptoms recur after treatment, none of the medical records noted it as a reason not to give the drug, the study found. But in almost half of the cases in which people weren’t offered the medication, no reason was given by medical providers other than patients having mild symptoms, the researchers found.
Drugs such as Paxlovid and molnupiravir are free and widely available, but officials say doctors are not prescribing them as much as they should.
But people with mild symptoms early in their illness are “exactly the target group for getting the treatment,” said Dr. Paul Monach, who heads the rheumatology section at the Veterans Affairs Boston Healthcare System and was the study’s lead author.
The drugs are recommended for people with mild to moderate COVID-19 who are at high risk of severe illness because of their age or medical conditions — the same kind of patients that the Boston researchers were scrutinizing. The CDC urges doctors to treat high-risk patients within five days rather than waiting for their symptoms to worsen.
“Every case starts off mild,” and it’s unpredictable whether it will become more severe, said Dr. Davey Smith, an infectious-disease specialist at UC San Diego who was not involved in the study. “It might not be until the fifth or sixth day that you get into trouble — and by that time it’s too late to take these medications.”
Smith said he was especially alarmed that people whose immune systems were weakened were not getting the drugs. “Those are the people who are still coming into our hospital. And those are the ones who are dying. ... It breaks my heart every time I see them in the hospital, and they just didn’t get the medication.”
It breaks my heart every time I see them in the hospital and they just didn’t get the medication.
— Dr. Davey Smith, infectious disease specialist at UC San Diego
The Boston researchers said their findings suggest that physicians need more education about when to consider using the drugs. Patients, in turn, could be encouraged to reach out to medical providers sooner after symptoms first appear.
Monach said that some Veterans Health Administration patients who weren’t offered the drugs had gone home before their coronavirus test results had been returned. Clinical staff such as nurses had phoned them to follow up, but did not appear to have mentioned the possibility of antiviral medication, based on the records reviewed by the researchers.
“That doesn’t mean that people weren’t doing their jobs,” Monach said, “but I don’t think those people had been informed, as part of their normal jobs, what the indication would be for giving Paxlovid.”
Concerns about Paxlovid and other COVID-19 medications not reaching patients who could benefit have persisted since soon after the drugs became available. Just months after Paxlovid received emergency use authorization from the Food and Drug Administration, a national survey from the COVID States Project found that among people infected with the coronavirus between May and early July 2022, only 11% reported having taken antivirals. Among a higher-risk group of people — those 65 and older — the rate was 20%, “higher, but still low.”
Another study of patients in the Veterans Affairs health system found that as of early 2023, less than a quarter of outpatients who tested positive for coronavirus infections were receiving any kind of anti-COVID medication. And researchers have also found alarming gaps in who is getting Paxlovid, with Black and Latino patients obtaining such treatment at markedly lower rates than white and other non-Latino patients, even among the immuno-compromised.
“I have been banging my head against the wall for my colleagues not using medications,” Smith said.
If physicians or patients are concerned about “rebound,” he said, “COVID has this waxing and waning of symptoms anyway,” whether you take medication or not. “And we know this medication, in higher-risk individuals, keeps people out of the hospital and from dying.”
Americans have embraced the idea that Paxlovid is to blame for COVID-19 relapses in people who’ve seemingly recovered. Scientists aren’t so sure.
One patient recently told him, “Well, the last time I got COVID, I didn’t take the medicine and I was fine,” Smith said. The problem, he said, is “that’s true until it’s not. You can only dodge the bullet so many times,” and the risks grow for an individual as they age. “Every time that you get COVID, you are getting it at a time when you are older.”
Last month, the California Department of Public Health issued an advisory to physicians and other healthcare providers, lamenting the underuse of such medications despite an “ample supply.” It faulted unfamiliarity with new medications and misperceptions that the drugs were scarce.
“Once an individual is diagnosed with COVID-19, early treatment with antivirals is the only existing strategy to decrease the risk of serious illness and prevent hospitalization,” the state agency said in a written remark. “The greatest benefit of antiviral treatment is seen in those at highest risk for severe disease. ... Risks including Paxlovid rebound, are minimal, especially when weighed against benefits.”
Dr. Richard Dang, an assistant professor of clinical pharmacy at USC, said that “it’s always worth the conversation” about whether to take Paxlovid or another antiviral drug when someone tests positive.
The medicines are most effective for people at high risk, but that is a broader swath of the adult population than many people realize, including people who are overweight, have asthma or heart conditions, and even people from racial and ethnic groups that have had worse outcomes from COVID-19, Dang said. Since the risks increase with age, “if you’re above 50 years old, you should definitely consider Paxlovid,” he said.
“At the end of the day, having some potentially unpleasant side effects that some people report — maybe like stomach upset or metallic taste — is far better than going to the hospital because of COVID,” he said.