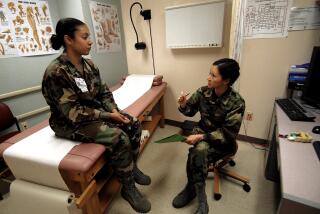
Physician burnout affects patients too
- Share via
My husband, Dave, works harder than anyone else I know. He often gets up so early — 3:30 or 4 a.m. — that I don’t even have a memory of him rising. Like me, Dave is a doctor.
He spends most of his day caring for patients at the hospital where he’s a pediatric orthopedic surgeon but manages to find time to write research papers, teach medical students and residents, and serve on a variety of hospital committees. And he wouldn’t give up any of it.
Dave simply loves his job. After 20 years in medicine, he still feels it’s a privilege to care for people. Not all physicians are so fortunate, however; many ultimately burn out.
Burnout doesn’t just create professional, and personal, problems for physicians — it affects patients too.
Obviously, extreme job fatigue isn’t a physician-only problem, but in the medical profession, physician performance can truly be a matter of life and death. And research suggests that doctors suffer from high rates of the condition.
In 2009, researchers at Johns Hopkins University surveyed almost 8,000 surgeons and found that approximately 40% were burned out in their jobs; studies of doctors working in primary care medicine reveal comparable rates.
Some doctors become so disillusioned with their careers that they opt to leave medicine entirely. After the years of training required to become a doctor — seven years for pediatricians, for example, 11 years for cardiothoracid surgeons — it’s hard to imagine that someone would quit. But, in fact, rates of attrition among doctors are surprisingly high. A recent survey conducted by the American College of Physicians and the American Board of Internal Medicine found that 17% of general internists are no longer working in their field of practice about a decade after their original certification.
Sometimes a doctor’s lack of interest in the profession will have an immediate effect; at other times, inattention and a tendency to go through the emotions will take a more insidious toll. Perhaps a patient’s high blood pressure will be less well-controlled than it should be; perhaps potentially dangerous side effects will go unnoticed; perhaps lifestyle advice will be skipped. In any case, patients pay part of the price for doctor burnout.
Empty tank
The term “burnout” is often used to describe the attitude of anyone who’s tired of their job. But burnout is more than simply dreading the idea of going to work each day — it’s a syndrome with several distinct characteristics. People who burn out at work describe feeling emotionally exhausted, stretched beyond what they can possibly do.
“It’s like a tank that’s been drained and there’s nothing left,” says Christina Maslach, a social psychologist at UC Berkeley and co-author of “Banishing Burnout.”
Emotional exhaustion is just the tip of the iceberg — it’s how people feel and what they do when they’re exhausted that distinguishes burnout from simply being tired of one’s job. People who burn out tend to become cynical; they question both the importance of their work and their ability to do their job well.
Then there’s the matter of drive. Burnout causes people to lose their focus on the job.
“They may shift from doing their very best to doing the bare minimum,” says Maslach.
Being a physician is undoubtedly emotionally exhausting work. It’s stressful and demanding on many levels. Doctors are under constant pressure to deliver outstanding care to their patients. These days that involves far more than sharp diagnostic skills. Doctors can’t just be competent; they need to be compassionate, supportive and respectful of their patients’ preferences too. To do their job well, doctors must be active listeners and good communicators; they need to be able to bridge cultural differences and navigate language barriers.
Physicians also have to work collaboratively with their patients and involve them in the decision-making process. Many might look back with fondness on the days of issuing orders — brusquely or not — and expecting patients to follow them.
Even under the best circumstances, today’s expectations create a tall order to fill, and many doctors work in settings where it’s almost impossible to do so.
In some cases, doctors don’t have the resources to do their job properly; in others, they’re hampered by almost insurmountable barriers. Hospitals and insurance companies can impose constraints that interfere with physicians’ ability to provide necessary medical services; busy office schedules can prevent them from having sufficient time with their patients.
Eventually, work strain and lack of adequate workplace support wear down many doctors and undermine their physical and emotional health. Burnout can trigger headaches, disrupt sleep, and contribute to a variety of mental health problems, including anxiety, depression and alcohol and drug addiction. On a personal level, burnout damages relationships and interferes with job satisfaction.
Endangered patients
Patients cared for by physicians who are burned out tend to be less satisfied with their care than those who are tended to by doctors more engaged in their work.
Of greater concern, however, than a disengaged attitude is that burned-out doctors may be more likely to make mistakes.
A study published earlier this year in the Journal of the American Medical Assn. found that internal medicine residents suffering from high levels of stress and fatigue were more likely to report making medical errors. A similar study appearing in the Annals of Surgery in 2009 found that burnout had the same effect among surgeons.
There’s no clear-cut way for patients to determine whether their physician is suffering from burnout. Beyond avoiding doctors who come across as frankly disinterested or overtly cynical, there’s little that they can do except trust their intuition.
As for my husband, the way he feels about his job is obvious to almost everyone. It’s apparent in the compassion he shows his patients and their families and in the smile he wears on his face. It’s the way he gets out of bed, however, that is perhaps most telling. Regardless of the hour, he’s eager to start his day.
He’s living proof that burnout isn’t simply about working hard.
Ulene is a board-certified specialist in preventive medicine practicing in Los Angeles. She can be reached at themd@att.net. The M.D. appears the first Monday of the month.