California slams insurers for discriminating against users of HIV-prevention drug
- Share via
Major insurance companies have denied policies to Californians who take a medication to shield themselves from contracting HIV, the state Department of Insurance announced Thursday, warning insurers that such discrimination is illegal.
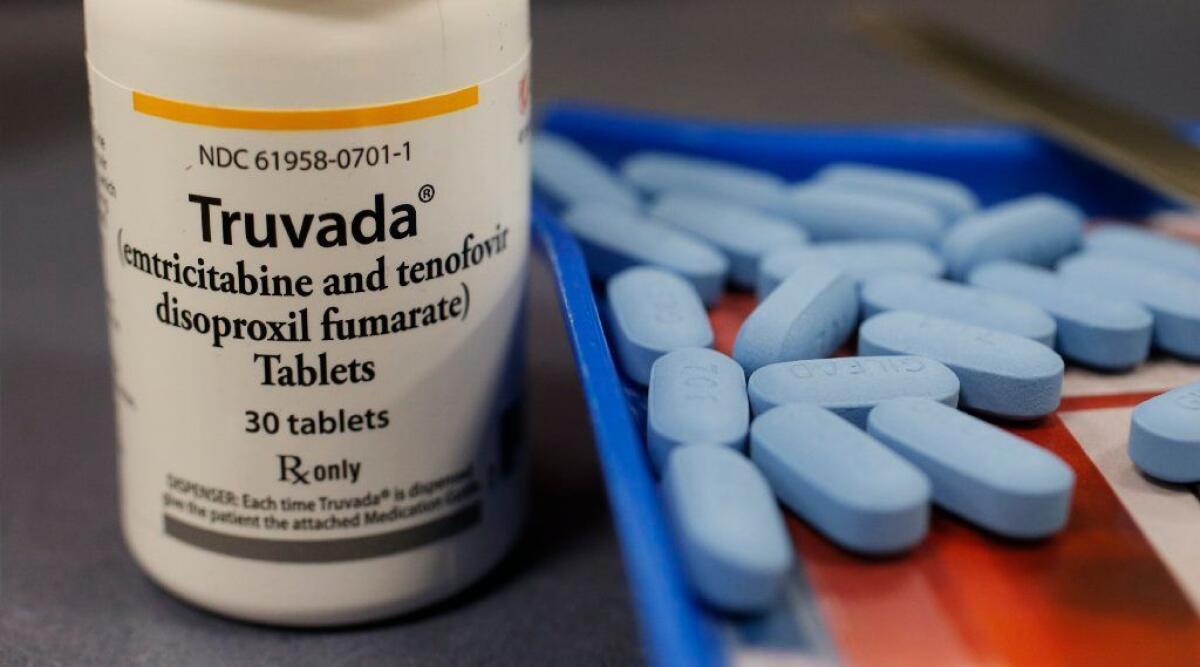
The department said that its investigation, which began in February 2018, found that several insurers had denied, limited or charged higher rates for life, disability and long-term care coverage for people who took the HIV-preventative medication Truvada, also known as pre-exposure prophylaxis or PrEP.
A department spokesman declined to name the specific insurers but described the discrimination as “frequent enough that we felt the need to send out an industry-wide notice.”
The findings were no surprise to Ged Kenslea of the AIDS Healthcare Foundation, who said his organization is aware of this type of discrimination by insurance companies.
“It’s wrong. People are just trying to protect themselves,” Kenslea said. “This is punishing people for taking care of their health.”
About 1.1 million people in the United States have HIV, according to the Centers for Disease Control and Prevention. In 2017, the most recent year for which information is available, more than 38,000 cases were diagnosed.
Citing the CDC, the California Department of Insurance said that when taken daily, the medication is “highly effective in reducing the risk of contracting HIV.”
The department said that many insurers have reported that they’ve already stopped discriminating against people who take PrEP. It said it is following up to make sure.
“As we embrace PrEP as a vital part of preventing HIV, making sure that there aren’t barriers to use or discrimination is critical or people won’t use it,” the department spokesman said. He said there is particular urgency since the federal government recently decided to require health insurers to provide PrEP to policyholders free of charge as part of the fight against the spread of HIV.
John Mangan, regional vice president of the American Council of Life Insurers, which represents many of the industry’s largest players, said that his organization was aware of the California insurance commissioner’s concerns and that companies constantly review their practices to ensure compliance with state laws.
Kenslea said that although he is glad that the state is holding companies responsible, he doubts that Thursday’s announcement will end discrimination against PrEP users.
“That’s putting a lot of faith of insurance companies to do the right thing,” he said.
Trump pledged to end the HIV epidemic. San Francisco could get there first »
More to Read
Inside the business of entertainment
The Wide Shot brings you news, analysis and insights on everything from streaming wars to production — and what it all means for the future.
You may occasionally receive promotional content from the Los Angeles Times.









