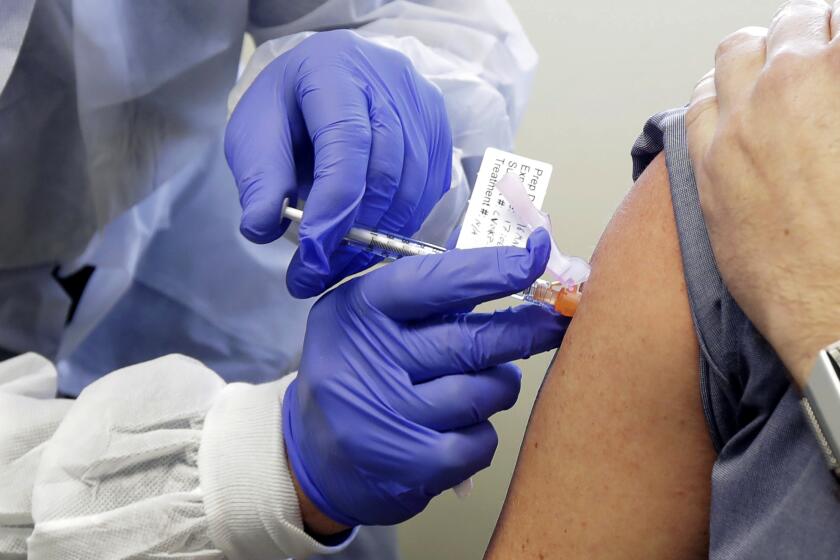
Developing a coronavirus vaccine should not be rushed. Here’s why

More than 130 labs around the world are working to develop a COVID-19 vaccine. But what would it take to vaccinate everyone by early next year?
- Share via
If anything is known for sure about the scientific battle against the novel coronavirus, it’s that the quest for a vaccine has been unprecedentedly intense, with rapid development and speedy production the paramount goals.
But some medical experts are raising a yellow flag. Given the stakes — the virus has caused more than 100,000 deaths in the U.S., among more than 350,000 worldwide — they’re cautioning that the process of developing a vaccine should be slowed down, not sped up.
“History tells us that speed kills,” says Arthur Caplan, a bioethicist at NYU Langone Medical Center and a co-author of an article in the Journal of the American Medical Assn. warning that missteps under Operation Warp Speed, the vaccine development initiative in the Trump White House, could undermine public confidence in vaccines broadly.
In this world, where there’s so much vaccine hesitancy and doubt, you better get it right, out of the box.
— Arthur Caplan, NYU Langone Medical Center
“For scientists and physicians, the term ‘warp speed’ should trigger concern,” Caplan and his colleagues observed. “Good science requires rigor, discipline, and deliberate caution.”
An overly hasty rollout could place a vaccine with disappointing immunological action or unexpected side effects in the hands of a public thirsting for a miracle cure, Caplan told me.
“There’s a huge danger of provoking doubt on the part of the public about the safety of vaccines,” he said, noting that just before the emergence of the current pandemic, “the anti-vaccine movement was growing, and we were seeing more vaccine hesitancy” — that is, parents reluctant to give their children the full panoply of recommended childhood immunizations.
Within 48 hours of Moderna’s vaccine announcement, its execs sold $29 million in shares.
He added, “The basis for doubt could be that people think you didn’t do the research properly or the vaccine was not manufactured safely.”
Caplan might have added: Doubt kills. Defeating the virus will require not merely a vaccine that works, but also one that is broadly accepted so that almost everyone takes it, creating the “herd immunity” that serves as a bulwark against the virus’ spread.
The National Institutes of Health has created what it calls a “coordinated strategy” to streamline the vaccine development process for the novel coronavirus, including multiple research threads proceeding simultaneously. The World Health Organization is overseeing a global trial of several candidate vaccines at once.
But that doesn’t necessarily mean the current timeline of a year to 18 months before a vaccine can be approved and distributed can be significantly shortened.
There’s strong historical precedent for concern about shortcuts.
The key lesson about the hazards of rushing a vaccine into production comes to us from Berkeley, where a small pharmaceutical company named Cutter Laboratories was chosen by the government in 1955 as one of five private manufacturers of the Salk polio vaccine.
The Salk vaccine incorporated a dead polio virus, potent enough in its active guise to produce a strong antibody reaction in humans but inactivated through treatment with formaldehyde so it wouldn’t cause disease.
Because of a series of manufacturing errors and poor government oversight, however, some of Cutter’s vaccine lots were contaminated with the live virus. An estimated 40,000 children contracted polio from Cutter’s vaccine. Many family members who had not been inoculated contracted the virus from their vaccinated children. About 200 victims were permanently paralyzed, and 10 died.
The stock market is euphoric over news of a possible coronavirus vaccine. But for now, you shouldn’t be.
The so-called Cutter incident was “one of the worst biological disasters in American history, exploded the myth of the invulnerability of science and destroyed faith in the vaccine enterprise,” observed Paul Offit, a vaccine expert at the University of Pennsylvania whose 2005 book is the definitive account of the episode.
The outbreak was so severe that the nation’s polio vaccination program, which up to then had enjoyed nearly universal public support, was halted in its tracks.
Public confidence in the vaccine was shattered. “The summer of 1955 came and went with few children getting their shots,” historian David Oshinsky, a co-author of the JAMA article, recounted in his 2005 history of the epidemic. Major outbreaks occurred in Boston and Chicago. “It seemed like old times, with beaches and movie theaters once again deserted and people fleeing the cities to escape the evil germs.”
Four of the five companies licensed to produce the Salk vaccine were big pharmaceutical firms, including Eli Lilly and Parke-Davis. Cutter was not. It had been founded in the rear of a San Jacinto, Calif., drugstore by E.A. Cutter. By the 1950s, it had moved to Berkeley and from veterinary drugs to vaccines for smallpox, tetanus and rabies.
Cutter’s reputation for innovative manufacturing got it the polio contract. As it turned out, even the big drug companies found the process of inactivating the polio virus to be a challenge, and one — Wyeth Laboratories — also shipped out some lots of contaminated vaccines. But the Cutter effect was much greater.
Cutter “didn’t have the internal expertise that was available to other companies,” Offit writes. “As a result, it made a vaccine that was far more dangerous than any other polio vaccine made in the United States or in the world.”
Among the errors Offit identified as factors in the Cutter debacle, the company used inadequate filters that allowed cells from the monkey kidneys on which the virus was grown — but on which it had not been inactivated — to infiltrate the vaccine.
The U.S. is suffering shutdown fatigue because the COVID-19 war has stagnated.
Cutter also subjected its vaccine lots to the bare minimum of testing required by the government, much less than the bigger companies, and didn’t monitor its own manufacturing standards to ensure that its vaccines were free of live viruses.
Finally, although Cutter knew it was having trouble producing uncontaminated vaccines — it was simply discarding the suspect lots — it didn’t notify the government or polio researchers such as Salk.
Cutter ultimately spent millions to settle a sheaf of lawsuits brought by vaccine victims. But it survived financially — “We have licked a nightmare!” its then-CEO proclaimed to shareholders in 1961. The firm was bought by the German pharmaceutical giant Bayer in 1978.
The Cutter incident led to a tightening of federal vaccine standards and oversight that in most respects continues today. Federal bureaucrats in the direct line of regulation were fired, up to and including Oveta Culp Hobby, the Houston businesswoman and socialite whom President Eisenhower had installed as secretary of Health, Education and Welfare.
The drug industry learned a lot from the incident, and has learned more since then. “We’re much better educated about how to mass-produce vaccines than we were then,” Offit told me.
Still, some of the same mistakes from the 1950s were repeated in 1976, when President Ford called for a warp-speed vaccination of the entire U.S. against the swine flu. The effort “failed in virtually every respect,” the JAMA article reports. Safety lapses led one manufacturer to produce a vaccine for the wrong virus, the approved vaccine failed to immunize many children, and troubling side effects appeared.
All this “added to the early momentum of the anti-vaccine movement,” the JAMA article observes.
There are disquieting parallels between the atmosphere swirling around the polio epidemic of the 1950s and today’s COVID-19 pandemic.
To begin with, the Eisenhower White House took a largely hands-off approach to dealing with polio. The administration left the task of developing and testing the vaccine largely to private industry and remained offstage after it was developed and massive nationwide shortages occurred.
“No one could have foreseen the public demand,” Hobby said, a statement that earned the White House official widespread ridicule, and serves as a spooky foretokening of the Trump administration’s defense of its own unpreparedness.
Claims were made that the polio epidemic had been exaggerated, just as one hears today that the COVID-19 pandemic is mythical. One target was the National Foundation for Infantile Paralysis (the March of Dimes), which had helped to fund Salk’s research and found itself accused of inflating the danger to attract more contributions.
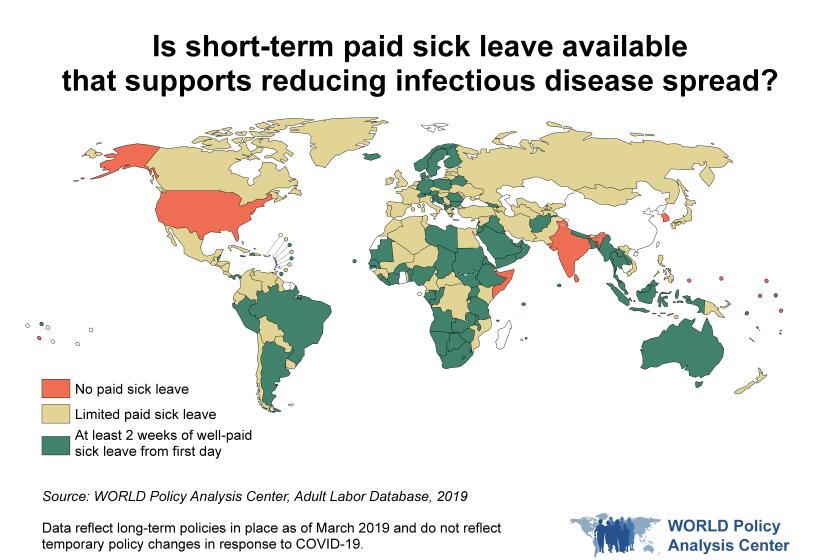
America lags the world in paid sick leave, hobbling our fight against COVID-19.
“A vaccine is a good thing to have. So is a bulletproof vest,” smirked the St. Louis Post-Dispatch. “Statistically, more than three times as many people in this country die of homicide than die of polio.”
Students of the polio era say that its errors can be avoided if COVID-19 vaccine candidates are subjected to modern scientific standards. Those require randomized trials of the vaccine on thousands of volunteers, some of whom are given placebos, to judge whether it is genuinely effective.
“As long as every vaccine that is to be put into the arms of Americans or people across the globe is tested the right way, which means large, placebo-controlled safety and efficacy trials, I’m good,” Offit said.
“What worries me a little bit is that there would be an interest by the administration come October to say, ‘Look, we see that these vaccines appear to be safe, they’ve been tested, let’s just start to give it,’” he said. “I hope that doesn’t happen.”
Desperation for a cure isn’t an excuse for reckless corner-cutting: “We were no less terrified by polio than we are by this virus,” Offit said. The Salk vaccine wasn’t approved for use until after its effect on more than a million children, including a control group, had been tested.
“Polio permanently paralyzed tens of thousands of children every year and killed 1,500,” Offit says. “Still, we waited for that trial, and similarly we should wait for these trials.”
Clinical trials won’t be the final hurdle in bringing vaccines to the world. Managing the public’s expectations will be crucial, since no vaccine for anything is 100% effective. So will ensuring that the manufacturing process is airtight.
With anti-vaxxers and conspiracy theorists already spreading wild stories about the coronavirus, it would be a shame to give them more ammunition.
“In this world, where there’s so much vaccine hesitancy and doubt,” Caplan said, “you better get it right, out of the box. You can’t afford a failure. Even knowing that we’re in desperate need of a vaccine and the deaths are happening, I worry that if we don’t do it right, it’s going to be worse.”
More to Read
Inside the business of entertainment
The Wide Shot brings you news, analysis and insights on everything from streaming wars to production — and what it all means for the future.
You may occasionally receive promotional content from the Los Angeles Times.