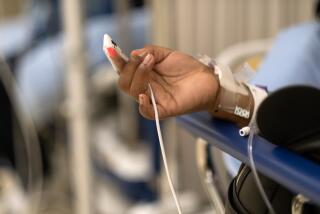
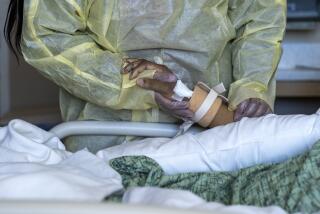
Pain, fear and isolation. COVID-19 made his hospital stay even more surreal and sad

- Share via
The pain, like a knife, had been stabbing his insides for three days when my son-in-law finally called the nurse hotline for advice. By then he could barely move from the bed and couldn’t even keep a glass of water down.
The nurse directed him to head to the emergency room right away. And that unleashed a tag team of worries in his mind: Something very wrong was going on inside his body. But might something worse contaminate him in a medical setting swamped by COVID-19?
“I didn’t want to get caught up in the mayhem of a hospital,” recalls TJ, my son-in-law. “I knew everything was different; I didn’t know what to expect.”
For weeks health officials had been warning the public that unless absolutely necessary, emergency rooms should be avoided; they might be overrun with contagious coronavirus cases.

But staying home had undoubtedly escalated the seriousness of TJ’s condition, complicating its prognosis. His stomachache signaled an abscess near his appendix; the delay in treatment allowed the infection to spread.
My son-in-law is now a part of what some doctors consider an under-the-radar epidemic of patients who delay seeking care for what turn out to be dangerous medical issues.
Emergency room visits have dropped dramatically, and many people don’t show up until they’re critically ill. Even people with heart attacks and strokes are trying to wait it out, hoping their problem will resolve.
“I worry people are suffering at home because they’re afraid our emergency rooms are radioactive,” Antelope Valley physician Larry Stock told Times reporter Joel Rubin.
By the time my son-in-law drove himself to the hospital, the virulent infection coursing through his abdomen had invaded his appendix.
And what might have been routine surgery and a one-night hospital stay would turn into two torturous weeks of fear, pain and paranoia, in a setting transformed by the coronavirus crisis.

When he arrived at the hospital on the morning of April 1, the check-in procedure in the parking lot was enough to shake TJ up. He had to drive through a maze of checkpoints; an hourlong process that took him through four different screening tents.
When he made it into the building, there were blood tests, X-rays, IVs, more X-rays, and finally a diagnosis: appendicitis and an abscess that needed draining.
“They told me, ‘You can probably be back home by tomorrow evening, if all goes well,’” he recalled.
All did not go well. The abscess wouldn’t drain. The infection spread. His fever spiked. His appendix ruptured. His asthma kicked in.
And not only would he not be going home anytime soon, no one would be allowed to visit him. “That just about broke me,” he told me. “I was already scared …. For a million reasons, it would have been nice to have my wife there.”
The no-visit rule is a pandemic creation, to protect patients, guests and hospital employees from unnecessary exposure to COVID-19. It applies to every patient — and takes a toll on them and their families.
“The darkest thing is you wake up and you stare at the same four walls every day,” TJ said. And you know that no one is going to show up to break the monotony of that.

TJ had left home with nothing but his keys and wallet, so my daughter went to the hospital the next day to drop off his phone charger, toiletries and a fresh T-shirt
Ahead of her in the drop-off line was a man bringing supplies for his wife. The receptionist asked him what she was in the hospital for. “A miscarriage,” he said, his voice soft and wobbly with grief.
That just about broke my daughter. She tried not to cry when the man turned to leave and she saw the pain in his eyes. And then she did something that she still can’t quite explain: She pulled off her T-shirt and stuffed it in the bag with her husband’s things.
She knew people were staring as she dashed back to her car, in sweat pants and a sports bra. But it seemed desperately important in that moment that TJ have a bit of her to hold on to.
TJ came home three weeks ago, after 13 days in the hospital. He’s still recovering from the ordeal. His care was good and his surgeon first rate, but the precautions required by the pandemic made the whole experience surreal.
“I didn’t feel human for a while,” he told me in his living room as he tried to keep his 18-month-old daughter from head-butting his tender belly.
Everyone he encountered in that first week at the hospital was garbed head to toe in protective gear, he said. “I couldn’t see a face; I only saw eyes.” He learned to recognize his nurses by their disembodied voices, “because everyone was wearing that same blue onesie outfit” that covers everything.
“That’s one of the hardest things to talk about,” he said. “Not seeing the people who were taking care of me. Not knowing if they were smiling. Not having anyone touch me. It’s very cold to just be there and without all of that .... I didn’t realize how much it meant to have contact with somebody.”
I thought about my own brief stints in hospitals years ago. The demeanor of the nurses meant everything. When I was feeling scared or worried, a smile from my nurse could unburden me. TJ had to buck himself up, absent that overt show of humanity.
So he seized on small familiar things: The jovial nurse who sometimes called him “my son.” The bald-headed guy whose voice called to mind his friend Greg. They made him feel less alone.
But there are darker things he won’t easily forget. They remind him of his blessings, even as they bind us to this bleak season, when health seems fragile and happiness fleeting.
After his surgery, TJ would practice walking up and down the hall outside his room. One room away was an elderly woman. He’d heard her nurse say something about a “bypass” as he shuffled by one day.
Another day he heard her crying into the phone. Her daughter had driven a long way to see her, she said. She pleaded for one brief visit with her daughter before she went into surgery. The daughter was in the parking lot, but not allowed to enter the hospital. The mother was inconsolable.
He imagined himself in her place. “It put into perspective what I was going through,” he said.
Two days later, there was a cleaning cart outside the woman’s room when TJ walked by. And taped to the door was a red notice with one word, handwritten in block letters: DECEASED.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.