Why the ‘beginning of the end’ of COVID-19 is further away than some think

- Share via
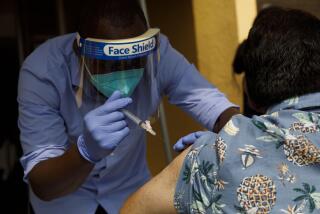
For all of the front-line healthcare workers who eagerly rolled up their sleeves for the COVID-19 vaccine on Monday, there’s something a little disingenuous — or maybe Pollyannaish — about the chorus of insistence that we’re at “the beginning of the end” of the pandemic.
Gov. Gavin Newsom tweeted as much on Sunday, as trucks and planes carrying millions of doses packed in dry ice fanned out across the country. His words echoed those of Louisiana Gov. John Bel Edwards and of Army Gen. Gustave Perna, who compared the Trump administration’s massive vaccine distribution operation to D-day, as if it was the beginning of the end of World War II.
For the record:
9:06 a.m. Dec. 16, 2020An earlier version of this column incorrectly identified Martin Luther King Jr. Community Hospital as a partner in running a COVID-19 testing site with Charles R. Drew University and L.A. County. The partnership is with the Martin Luther King Jr. Outpatient Center.
The truth is, the hardest work is just beginning — and, contrary to what seems to be popular belief, there’s no real end in sight.
Few people understand this more than Dr. Roberto Vargas, an assistant dean of health policy and inter-professional education at Charles R. Drew University of Medicine and Science.
For months now, he and his colleagues at the historically Black university have been doing intensive outreach in Watts and the surrounding communities about COVID-19, hoping that when a vaccine is finally widely available, they will be in a unique position to help persuade the people who need it most to take it.
Already the roughly 1 million people who live in South Los Angeles, most of whom are Latino or Black, are at a disproportionate risk of dying of COVID-19.
Reversing that trend, as Vargas and his colleagues are attempting to do, is slow and complicated work. It requires navigating a maze of past and present institutional failures, and processing human fears and distrust. But it’s also extremely necessary work.
Nationally, only about half of all Americans say they plan to join the millions of nurses, doctors and residents of long-term care facilities who, starting this week, are getting the first doses of the vaccine developed by Pfizer and BioNTech. That drops to 24% among Black adults and to 34% among Latino adults, according to the Associated Press-NORC Center for Public Health Research.
In California, only 29% of Black adults and 54% of Latino adults told the Public Policy Institute of California that they probably or definitely will take a vaccine.
That’s far short of the percentage of the population, roughly 70%, that must be vaccinated to achieve herd immunity from COVID-19.
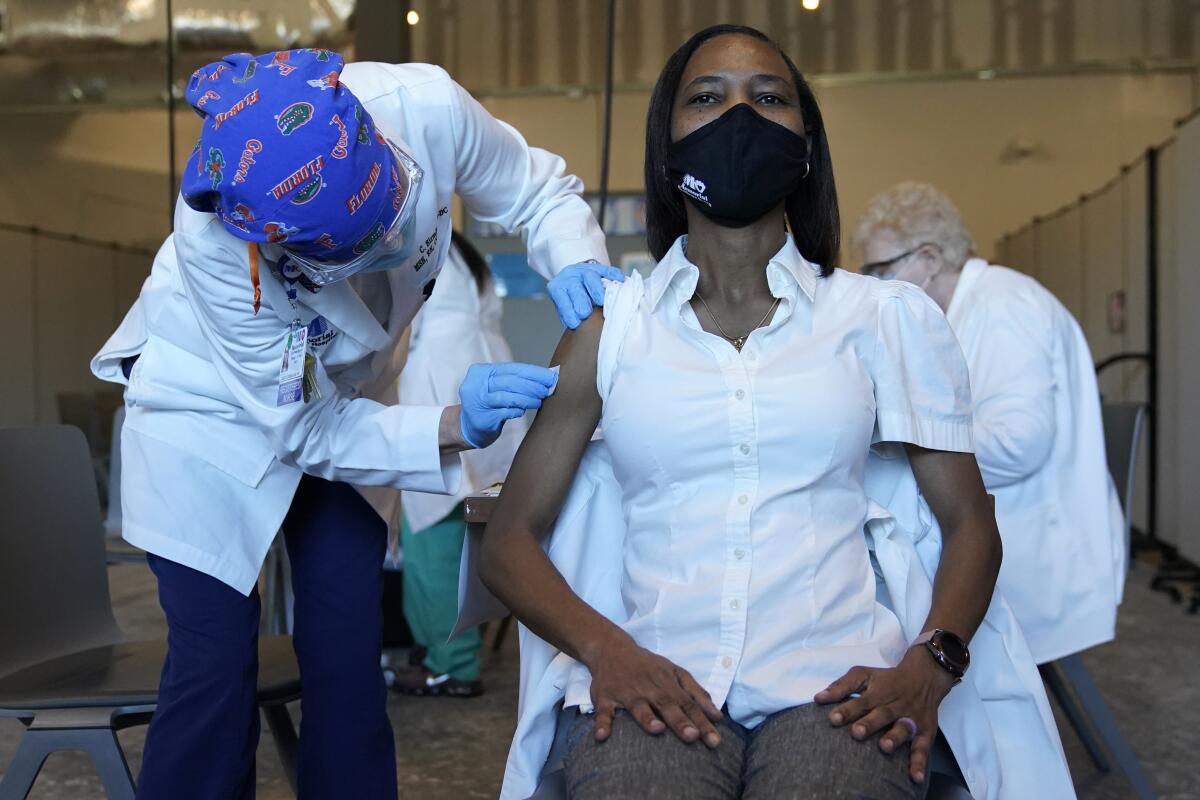
Some Americans will change their minds — hopefully — as they see others get vaccinated and walk away with nothing more than a sore arm. Sandra Lindsay, a Black critical care nurse at a Long Island hospital, became the first American to be vaccinated outside of a clinical trial on Monday for this very purpose. Others will never get over the very real horrors of the Tuskegee Syphilis Study, fearing that the government will once again use people — specifically Black people — like guinea pigs.
“This is gonna be tough,” Vargas said, “and so one has got to be multifactorial.”
Charles R. Drew University has done that throughout the pandemic with some success, persuading thousands to get tested and connecting many of them with the healthcare system for the first time.
Building on a long history of community-based healthcare in Watts, the faculty zigged when others in Los Angeles County mostly zagged. While drive-through coronavirus testing sites were being set up in parking lots, requiring people to make appointments online, the university, in partnership with the county and Martin Luther King Jr. Outpatient Center, decided to offer appointment-free, walk-up testing.
When that didn’t draw enough people, Dr. Sheila Young, an assistant professor of Charles R. Drew University, decided to try a more direct approach. She and several students took to the streets to tell people about the availability of coronavirus testing, reassuring them that it was free and would be painless.
It worked. The number of tests conducted per day shot up from about 250 to 1,000. There were lines around the block some mornings. And as spring turned into summer, the South L.A. testing site quickly became the most popular for Black and Latino residents in L.A. County, representing about 87% of everyone tested.
“One of the things that’s important, especially when you’re looking at working with individuals who may have certain fears, is realizing that their fears are valid,” Young said. “So we went out into the community, and we heard about what their fears were and we addressed them.”
What they heard should prompt anyone who thinks we’re at the beginning of the end of the pandemic to think again.
In addition to the common fear of losing part of one’s brain to a nasal swab — a fear I very much share — many thought they had to pay or have insurance to get tested. So they didn’t try. Never mind the signs around South L.A. that say otherwise.
“You have to understand,” Young said, “that individuals have gone to either free clinics or they’ve gone to county hospitals, and then they’ll get a $3,000 or $5,000 bill after we’ve told them, ‘No, you can go and get services and that there are programs to cover you.’”
Some thought that if they tested positive for the coronavirus, the government will take their children away. Or that they would be deported.
Still others said they had never got tested because, while they had seen the signs for it, they had assumed that the advertising was targeted at other people.
“There was a sense of, it’s not going to be made available to us,” Young said. “That was something that was actually heartbreaking because what it demonstrated was their feeling that they weren’t important and that they were not valued in the community.”
None of this bodes well for getting Black and Latino people to take a vaccine, the first of which has been deemed safe by multiple agencies at multiple levels of government. The side effects are minimal, especially compared to the life-threatening consequences of getting COVID-19.
And in a statistic that’s likely to complicate matters even further in the coming months, about 30% of the people who showed up to get tested at the university-run site didn’t have a primary care physician to consult or an emergency clinic where they would usually go for help. They are invisible to the healthcare system at exactly the time when the public health officials need people to be visible.
“You’re asking somebody to get an injection when they’re healthy,” Vargas explained. “And they’re going to take a risk — and there is a risk associated with it — to give them some individual benefit, but more so to benefit other people. And you never gave them healthcare in the first place. So really addressing some of the preexisting disparities needs to be part of that conversation.”
Of course, Charles R. Drew University is in a unique position do just that, being that it was founded after the Watts revolt to address that very problem of access to healthcare. Its faculty, many of whom are from South L.A., have been embedded in the community ever since. Lucky us.
Other cities are going to have to work that much harder before we truly get to the beginning of the end.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.