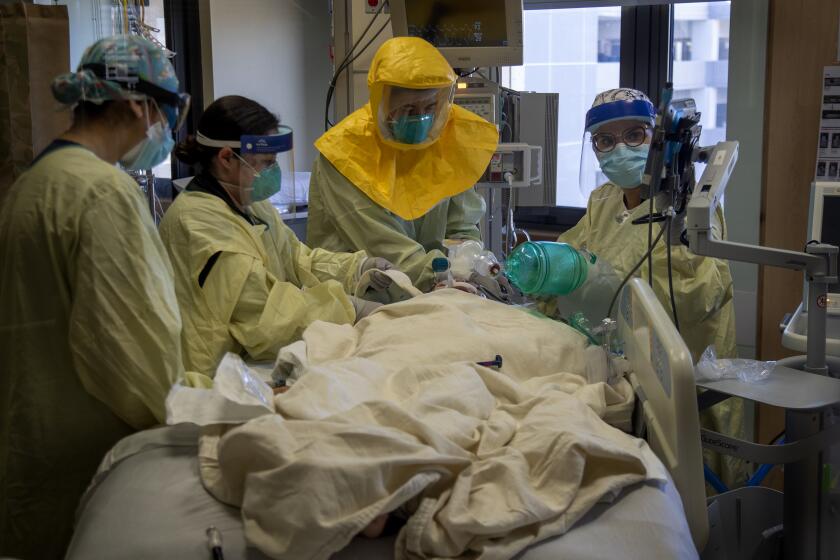
Orange County deploys field hospitals as COVID-19 cases soar

- Share via
With the number of local COVID-19 patients soaring to record levels, Orange County officials announced Tuesday they will deploy mobile field hospitals to relieve some of the stress on the region’s healthcare system.
Three hospitals — Fountain Valley Regional, St. Jude Medical Center and UC Irvine — have already requested the mobile units, which will add between 25 and 50 beds to their existing capacities, officials said.
The rollout comes as Orange County, like much of the state and nation, has been besieged by record numbers of COVID-19 infections that, in turn, have flooded its hospitals with unprecedented numbers of coronavirus-positive patients.
“Every day we break the record of the number of people who have been infected,” Dr. Clayton Chau, Orange County’s health officer and Health Care Agency director, told the county Board of Supervisors on Tuesday. “So I’m pleading with the community: Please, please do not gather, and make sure you follow the public health guidance, because our hospitals are now bombarded.”
Orange County is far from alone in that regard. California as a whole is wrestling with its most significant wave of the pandemic to date — prompting the state to open temporary field hospitals in Costa Mesa, Porterville, Sacramento and Imperial, with other facilities on standby in Riverside, Richmond, Fresno, San Diego and San Francisco.
The field hospitals will care for non-ICU patients in places including Costa Mesa, Porterville, Sacramento and Imperial. More are on standby.
According to the latest state data, there were 1,486 coronavirus-positive patients hospitalized in Orange County on Tuesday — an all-time high that’s more than doubled from just two weeks ago.
The number of COVID-19 patients in intensive care had risen to 319 countywide on Tuesday. A month ago, there were 85.
“I think what we’re seeing is not a surge — more like a tsunami, I’m sorry to say,” said County Supervisor Doug Chaffee.
Healthcare officials have some options to preserve ICU capacity, such as canceling scheduled surgeries, keeping critically ill patients in emergency rooms, sending ICU patients into step-down units earlier, training nurses from other units to help with intensive care, and increasing the number of patients each ICU nurse cares for.
However, those steps are only a Band-Aid, and officials emphasize that they are neither sustainable for the long term nor sufficient if the patient load continues rising at the rate seen over the last few weeks.
“I am afraid,” Chau said. “I have never been so afraid of Christmas and New Year’s in my life like I have now, because ... I can’t imagine what it would be like after the holiday if people are not listening, if people are not complying, if people are in defiance and get together.”
The most precious, and increasingly stretched, resource is the pool of trained professionals whose job it is to treat patients.
The months-long pandemic has taken a severe toll on California’s healthcare workforce. Many have become burned out caring for those with COVID-19, or contracted the disease themselves.
With the entire nation in the throes of the most severe coronavirus surge to date, many states are looking for additional ways to bolster their staffs.
“There’s tremendous demand,” state Sen. Richard Pan (D-Sacramento), a physician, told The Times this week. “This is not a California-only problem. We are competing with every other state. Our country is one entire hot spot. There is no place to draw staff from.”
That’s the case in Orange County, where Chau emphasized that “the crisis here is not that we don’t have enough beds,” but rather “we don’t have enough staff ... because all our nurses, all our respiratory therapists — they’re tired.”
Hospitalizations are continuing to rise at unprecedented levels, and officials have limited options for boosting capacity. Among the tools: Canceling scheduled surgeries; keeping critically ill patients in emergency rooms; training nurses from elsewhere in hospitals to help with intensive care; and increasing the numbers of patients an ICU nurse can treat.
Though there are undoubtedly dark days ahead, California — and the rest of the world — has received a glimmer of hope with the recent arrival of a COVID-19 vaccine.
A handful of healthcare workers at Providence St. Joseph Hospital in Orange were among the first in the county to receive the Pfizer-BioNTech vaccine Wednesday. The initial inoculations were streamed live, and each was greeted with a round of applause.
“On March 25, our county announced our first COVID death,” Supervisor Don Wagner said just before the first recipients rolled up their sleeves. “Today, less than nine months after that tragic day, we administer a vaccine.”
The vaccine’s arrival, he said, means “we’re poised to take the next step in response to this pandemic.”
“I join with everyone here in eager anticipation of what the months to come will mean in terms of a return to health and wellness for all of our citizens,” he said.
The vaccines will do little to stem the new infections flooding California. Initial supplies will be steered toward healthcare workers and residents of long-term care facilities.
For now, though, the stakes remain higher than they have ever been — both in Orange County and throughout the state.
More Californians died from COVID-19 on Tuesday — 295 — than on any one day of the entire pandemic. Over the last week, an average of about 175 people have died statewide from the disease every day.
Nationwide, the surge has become so severe in recent days that roughly two Americans have been dying from the disease every minute — a rate Chau called both astounding and embarrassing “from a world perspective, because we’re supposed to be the best of the best in what we have in medical care.”
The message going forward, he said, is simple: “Don’t gather. Wear your mask when you’re out. Stay six feet apart” from those you don’t live with.
“The vaccine is coming. It will be a sad day if you don’t have a chance to get the vaccine because you accidentally died from behavior that could have saved you from COVID,” he said.
Times staff writer Melody Gutierrez contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.