- Share via
It wasn’t long past noon and Dr. Anita Sircar found herself again saying the phrase she had repeated in the halls of Providence Little Company of Mary Medical Center in Torrance, like the chorus to a rueful song: “Here we go again.”
Twelve new patients suffering from the virus had come in overnight, including a 19-year-old whose parents were already hospitalized for COVID-19. And they kept coming in that morning, one after the next.
Nurses were strategizing about how to expand the isolated segment of the intensive care unit that they had set aside for the sickest of their COVID-19 patients as room after room was occupied — the kind of planning that the hospital has had to refine for pandemic surges as it juggles the needs of other patients.
“Do we have a bed yet?” Sircar called out as doctors and nurses flurried around a 48-year-old man who had been rushed in and intubated in the emergency room. They wanted to bring him upstairs to intensive care.
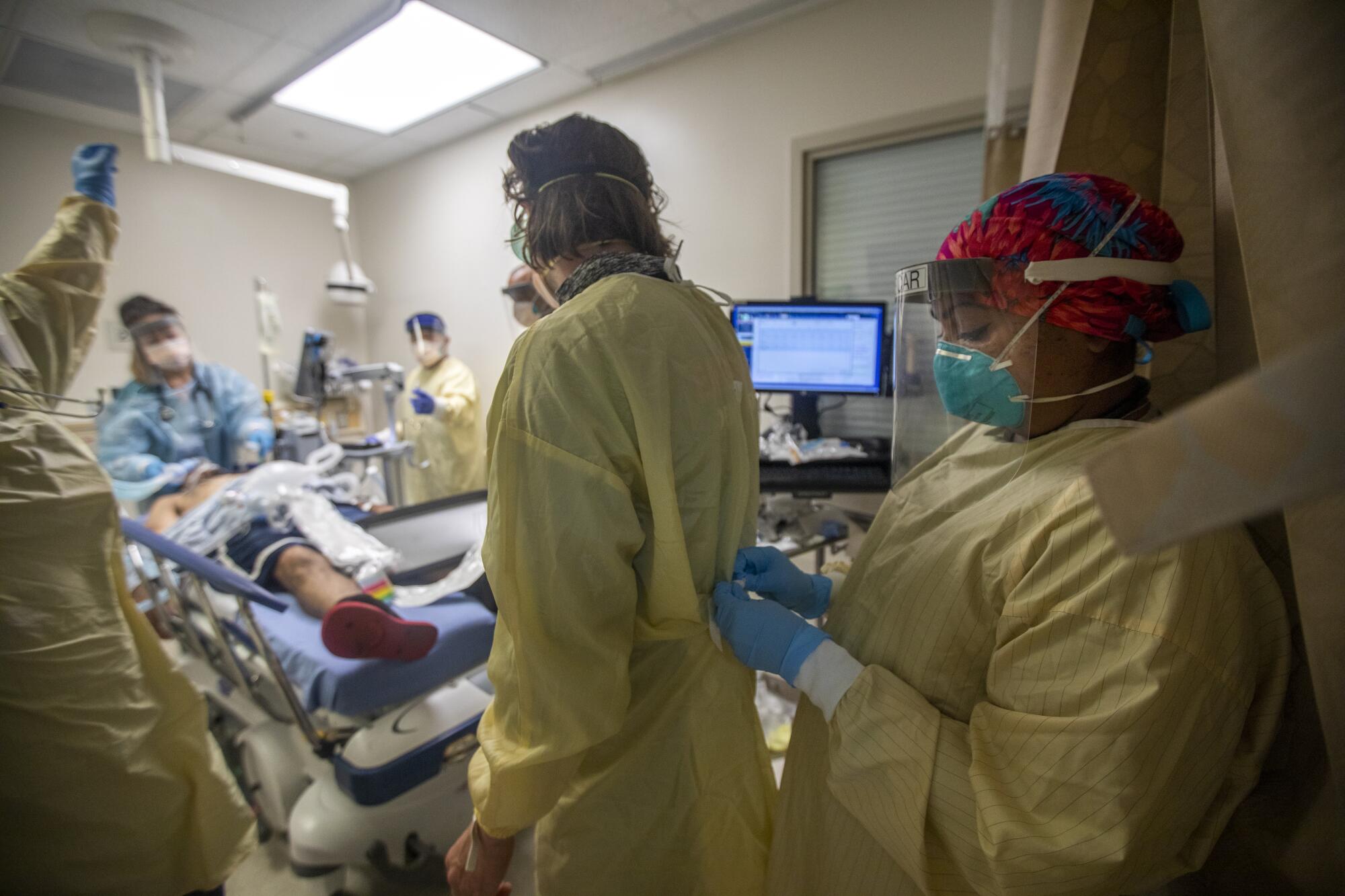
“That’s a no,” a nurse replied.
When the man had stabilized, Sircar stepped outside the hospital to talk to his wife. It felt too much like the grim winter that she and the rest of the hospital staff had endured: the surging numbers of patients, the pressure on “real estate” inside the hospital, the agonizing talks with relatives. Just like January or February, Sircar kept saying.
But it was August, long after a COVID-19 vaccine had become available, and her sadness had started to curdle with frustration as more and more patients who had forgone a vaccine ended up in the intensive care unit. Sircar called it an “existential” kind of sadness and exhaustion, that humanity seemed not to have learned anything after so much death.
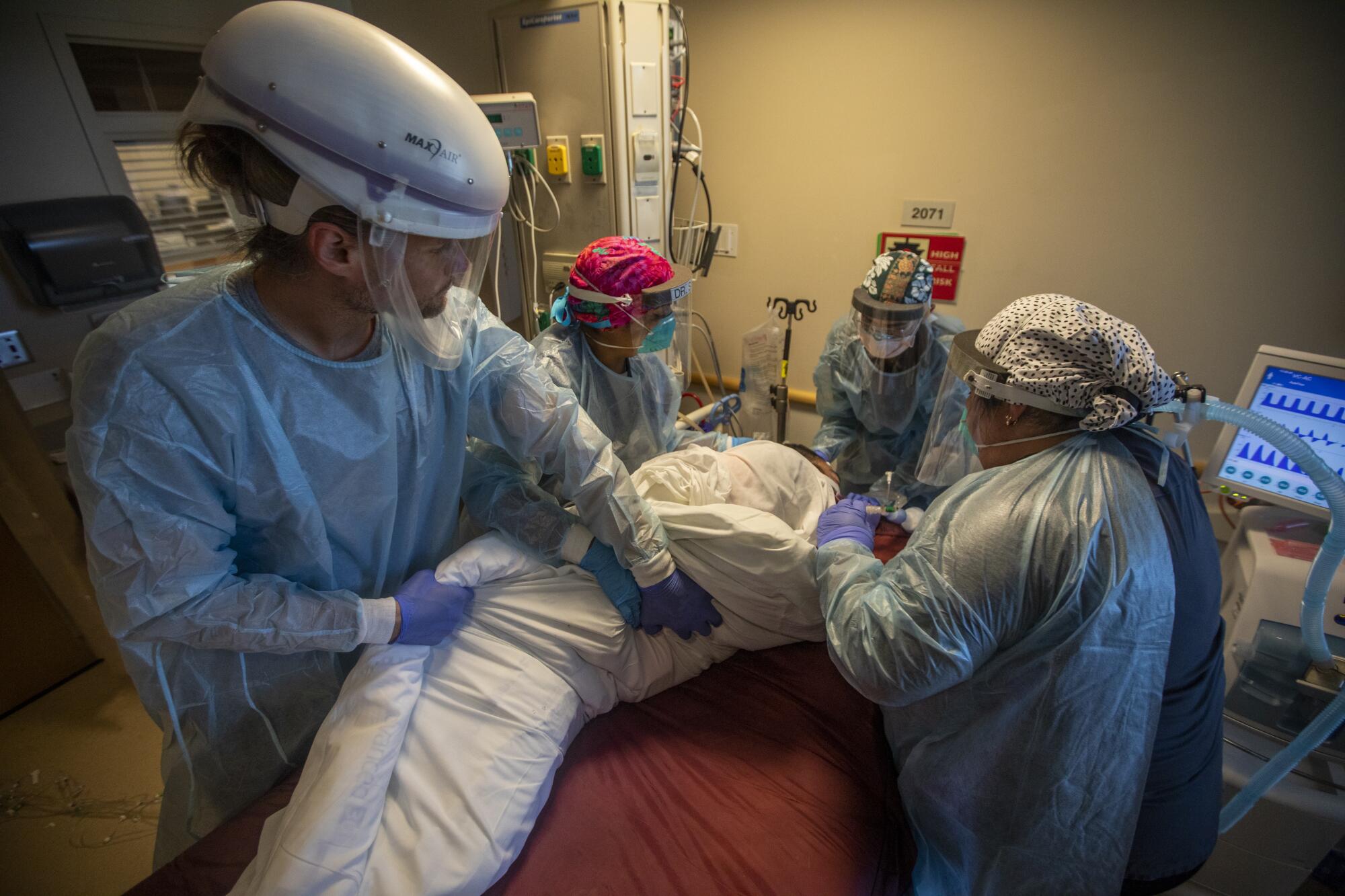
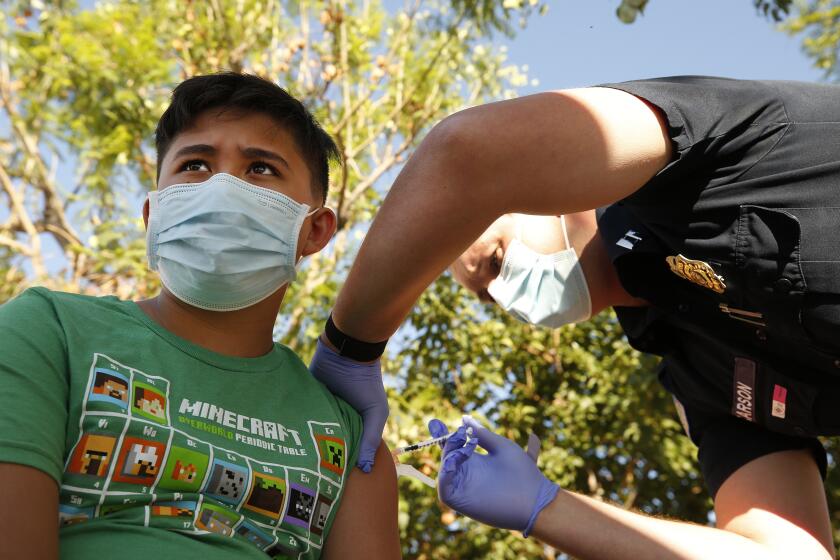
“The greatest weapon that we have right now is the vaccine. And people aren’t getting it,” she said.
COVID-19 cases have been on the rise in Los Angeles County in recent weeks, powered by the highly contagious Delta variant of the virus, the loosening of some pandemic restrictions, and strained progress in vaccination.
At Providence Little Company of Mary, a 442-bed medical center in Torrance, doctors and nurses grimly greeted what they dubbed the “fourth wave.” In late May, there had been just two patients with the virus at the hospital. That Thursday morning in early August, there were 37. Only two were vaccinated, neither in dire condition.
Joseph Arthur has spent the past year opposing the COVID-19 vaccine on social media. His manager and band quit, and his remaining fans beseech him to stop.
Those numbers are still far below the winter surge, which resulted in nearly 200 patients being hospitalized with the virus at the Torrance medical center in early January. But the summer rebound has been demoralizing, in part, because much of it could have been avoided, nurses and physicians there lamented.
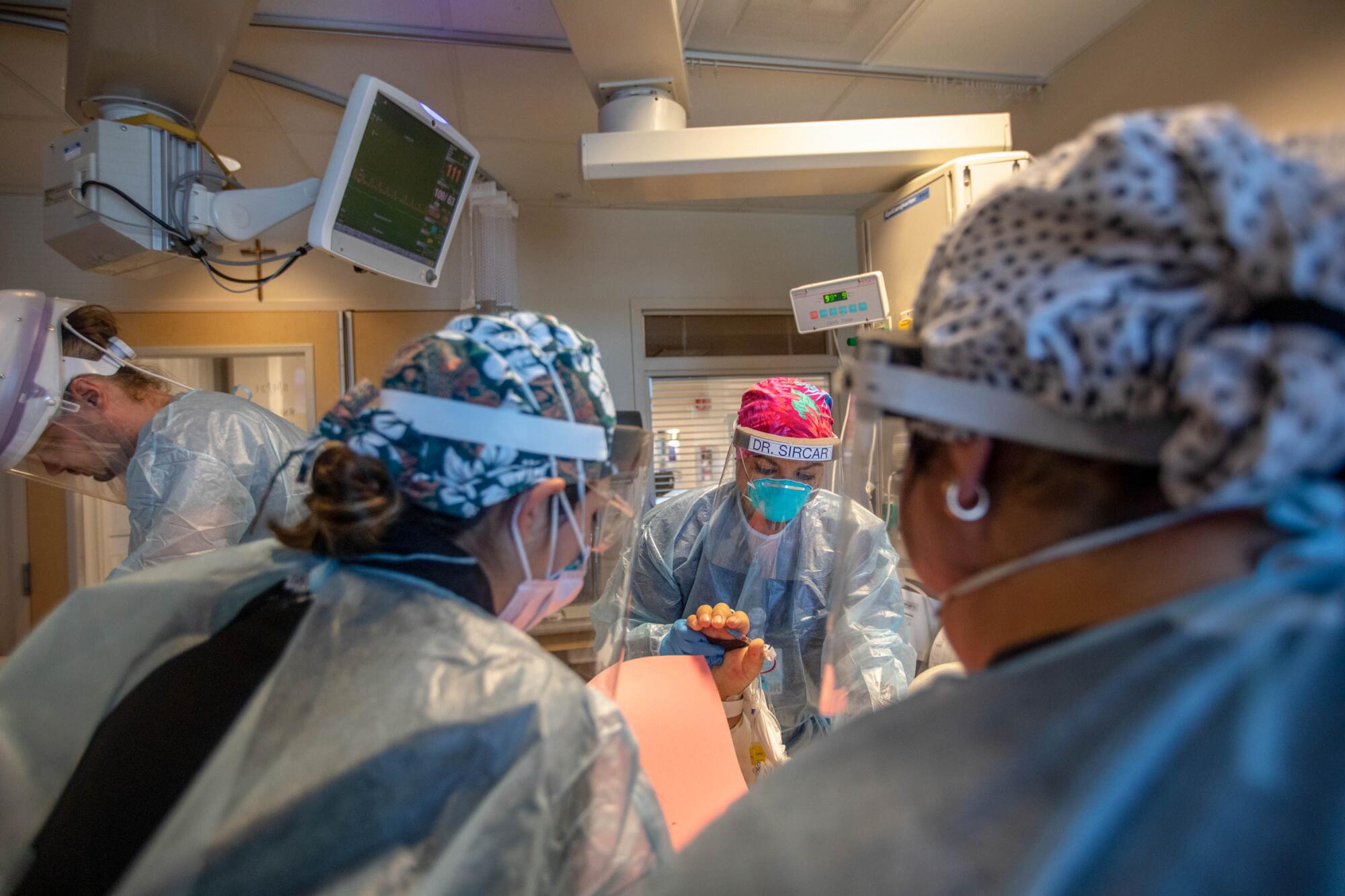
“I’m bummed,” said Dr. Alex Hakim, a critical care physician at the hospital. “And that’s the most eloquent words I can say about it. I’ve been extremely un-eloquent lately.”
Before Sircar and her co-workers launched their daily rounds, where doctors, nurses and specialists pore over the treatment plan for each COVID-19 patient in the ICU, a hospital chaplain offered up a reading. Sircar bowed her head.
“When disappointment in others clouds my vision, let me not judge but affirm my decision. For we all do what we think is best. And forgive ourselves as we forgive the rest,” Aviva Levin recited. “We thought that we were out of the woods. But we are still covered by the pandemic’s hood.”
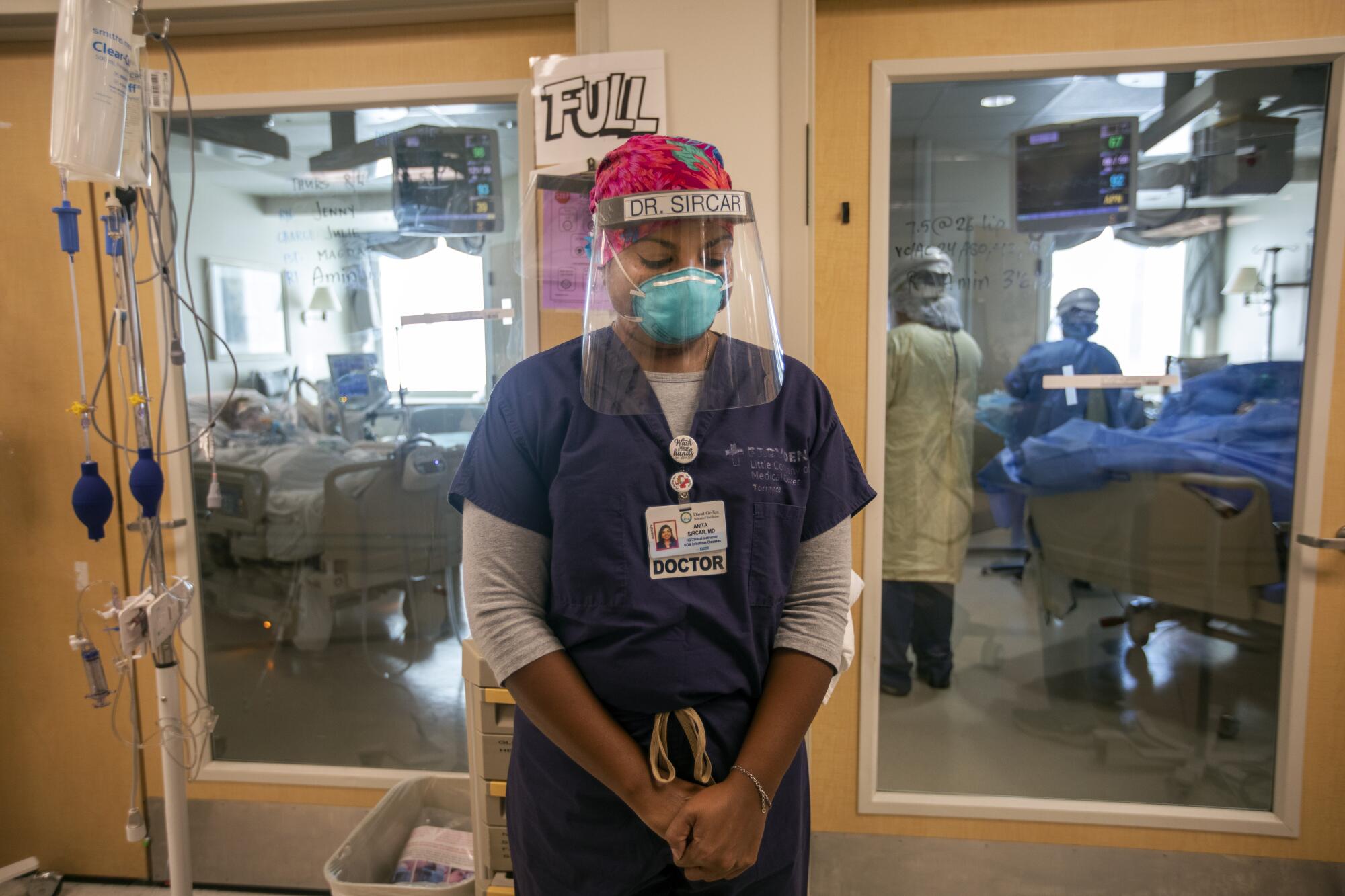
Levin said she had written those words just that morning, mindful of how the resurging numbers were grating on medical staff. “You see the PTSD [post-traumatic stress disorder] all over the place,” she said of the doctors and nurses. “But they keep showing up. They just keep showing up.”
Before Sircar returned to the South Bay, where she grew up, she devoted much of her medical career to battling infectious disease across the globe, with the nonprofit Doctors Without Borders and later with the U.S. Centers for Disease Control and Prevention. She has fought against Ebola in Guinea; cholera in Haiti; yellow fever in Angola; malaria in South Sudan.
But facing off with COVID-19 at home has been the most demanding, she said. As she strode from patient to patient, she ruminated that the virus would do anything to survive, mutating over and over to infiltrate the immune system.
And it seemed, to her, that humans were just not as bent on survival.
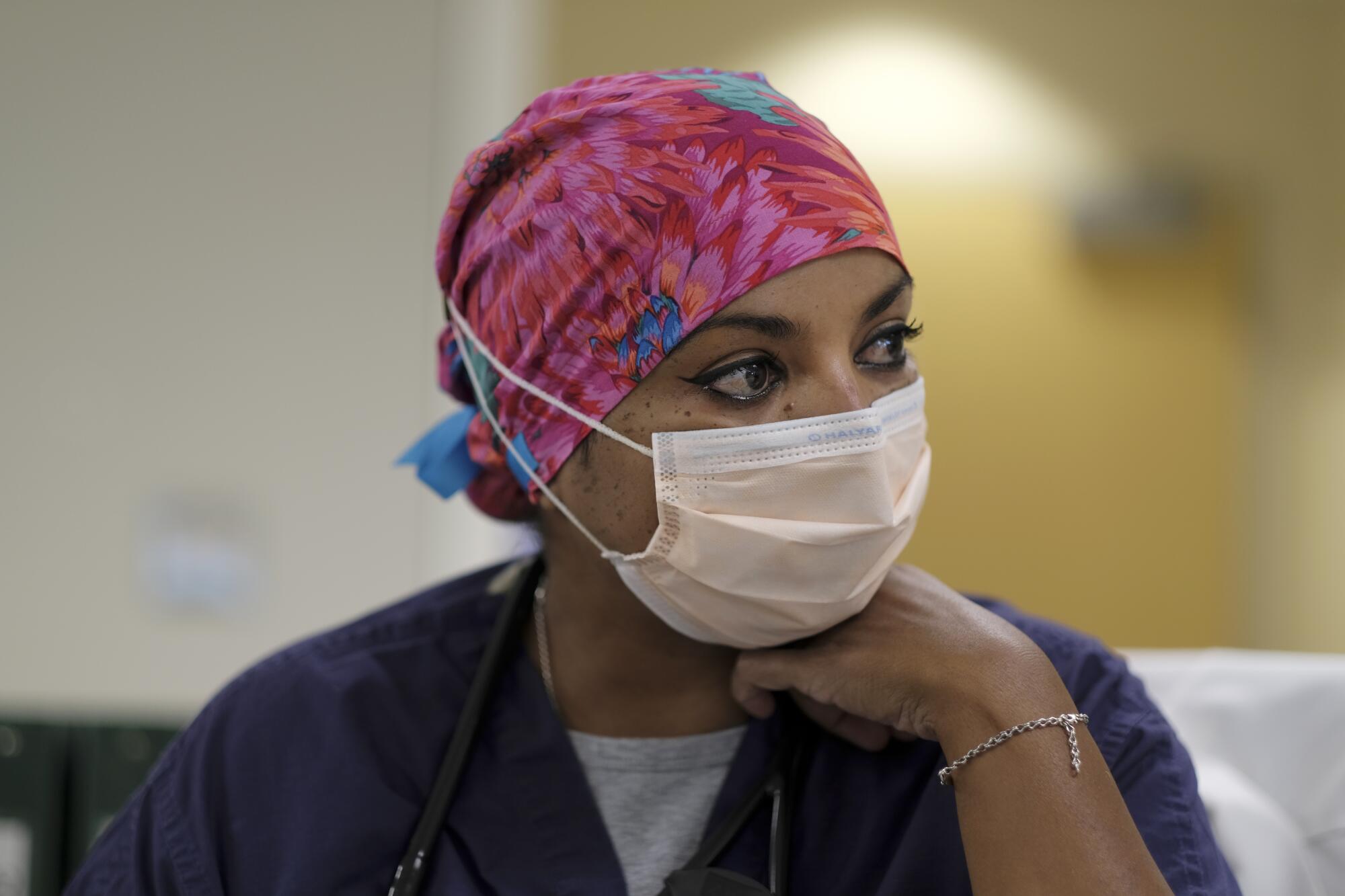
“Here you have a human population that will not get vaccinated, that won’t wear a mask,” she said before checking on her next patient. “This virus is outwitting us because we’re not willing to adapt at the speed that this virus is adapting.”
Even some of her own aunts have shunned her urgings to get vaccinated, said Sircar, saying they don’t feel like they have enough information about the shot. Sometimes she feels like it was futile to spend years building her expertise in infectious disease when so many people put their trust in lurid misinformation on Instagram and Facebook.
“That’s really disheartening for all of us who are in this profession,” Sircar said. “Doctors, nurses, scientists, epidemiologists — their word is nothing compared to a celebrity or a politician who says otherwise.”
As doctors and nurses hustled urgently around the man in the emergency room, trying to stabilize him amid seizures, gastrointestinal bleeding, pneumonia and low levels of oxygen, another COVID-19 patient was sitting up in the room next door, scrolling through his smartphone. When Sircar stopped in to see him, he was short of breath, but chatted readily.
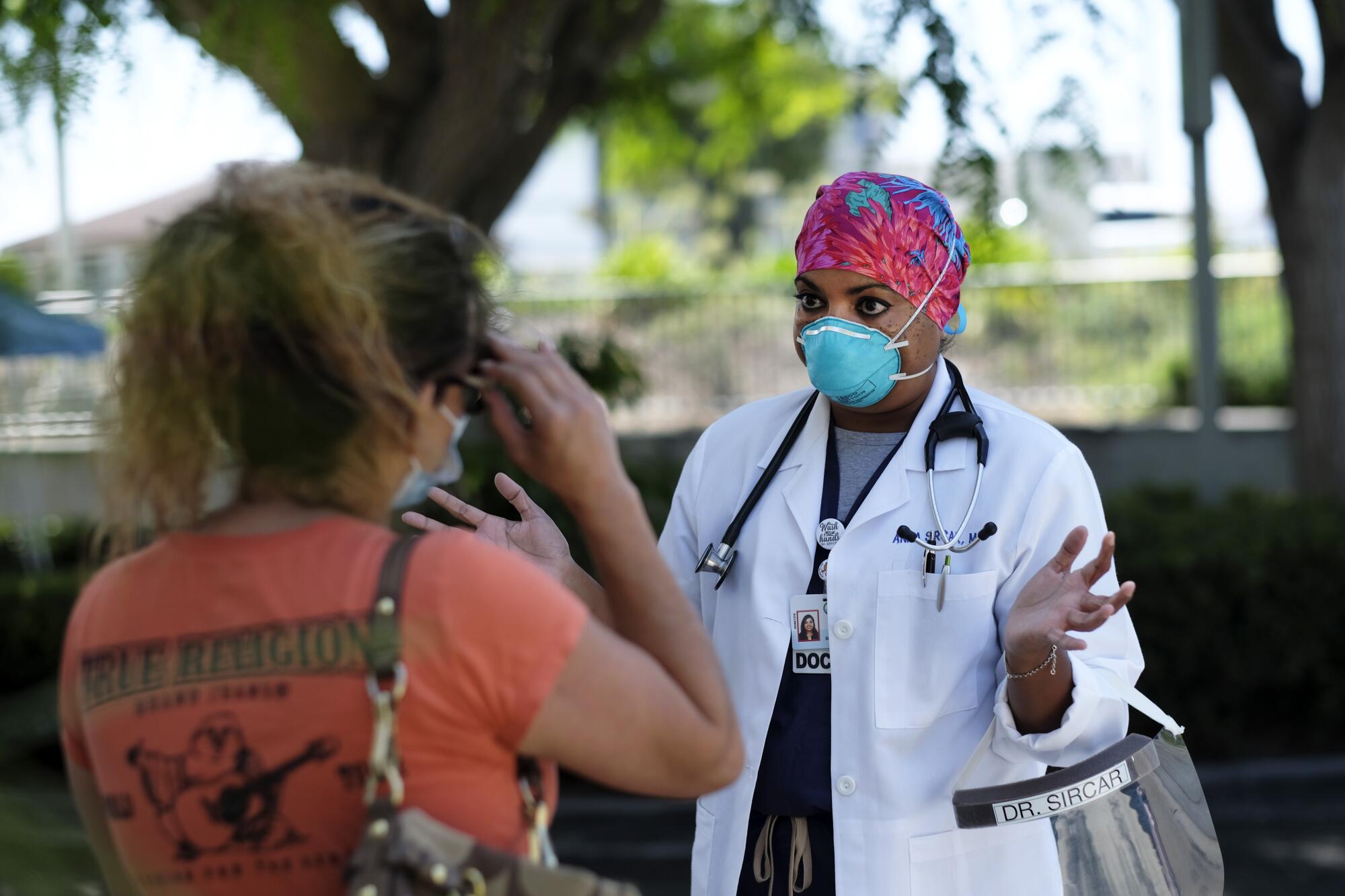
“It would have been much worse if I were not vaccinated,” said the man, who is immunocompromised. He asked not to be named because he didn’t want to worry his co-workers.
“I just told them that I’ve not been well,” he said.
Outside the emergency room of the Torrance hospital, Sircar greeted the wife of the man who had just been intubated. He was stable, she assured the woman, but “he’s very, very sick. He’s about as sick as a COVID patient can get.”
“We’re doing everything we can to turn that around. The one thing that he has on his side, that’s an advantage, is that he’s young,” Sircar told the woman standing outside, whose eyes were unreadable behind her sunglasses. One of her daughters was sitting silently on a nearby curb.
But not being vaccinated, Sircar said, was a big disadvantage.
The woman said she was still struggling to believe what was happening. Her husband was against vaccination, she said, which is why she and her older children had not gotten the shots. Sircar urged them to get to a CVS, Walgreens or anywhere else they wanted to get the vaccine, and reassured the woman that she would call if the woman’s husband worsened.
As the doctor stepped back into the noontime hubbub of the hospital, she exhaled a single word: “OK.”
Already there was talk of reinstating a tent to screen patients outside the hospital, something it had stopped doing when COVID-19 cases had fallen. Sircar worried that if the numbers continued to surge, the hospital might have to hold off on any surgeries that were not absolutely essential.
“This is only the beginning of this fourth wave,” Sircar remarked on a brief break, sipping from a water bottle.
“This is only the beginning of this fourth wave.”
— Dr. Anita Sircar
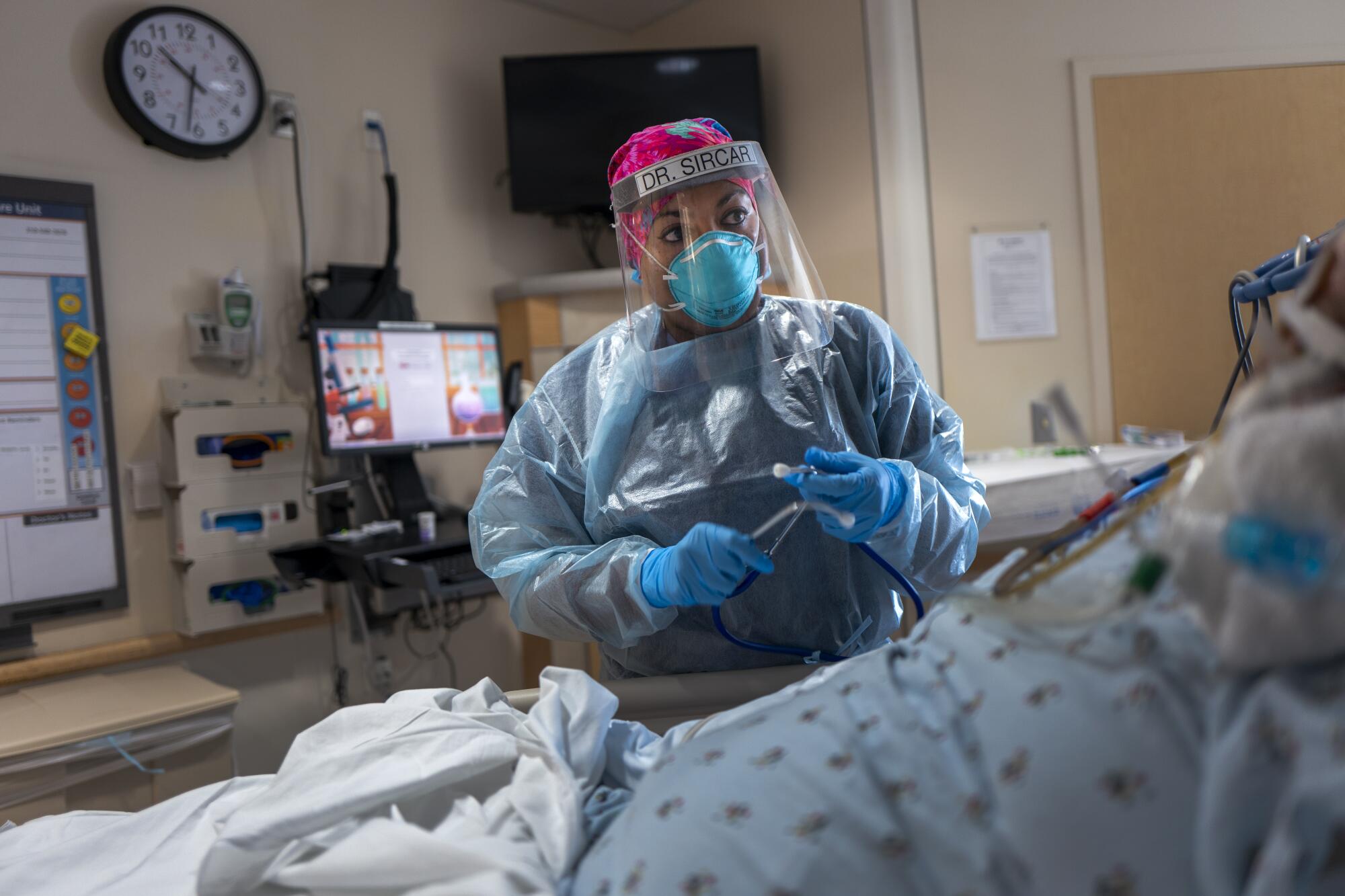
When she examines a COVID-19 patient, she has already seen their lab results and eyed the white clouds that mean trouble on a chest X-ray. She notes the blood pressure and oxygen saturation levels on the monitor; listens with a disposable stethoscope to the rhythm of the heartbeat for anything astray. She examines and traces their legs for signs of a blood clot.
Sometimes she wiggles a ring off of an intubated patient to keep safe for their family members, mindful that their fingers may swell. She removes dentures, piercings and contact lenses to head off possible infections. She peels back socks to check for any injuries, since an intubated patient cannot tell her they broke a toe on the way to the ambulance.
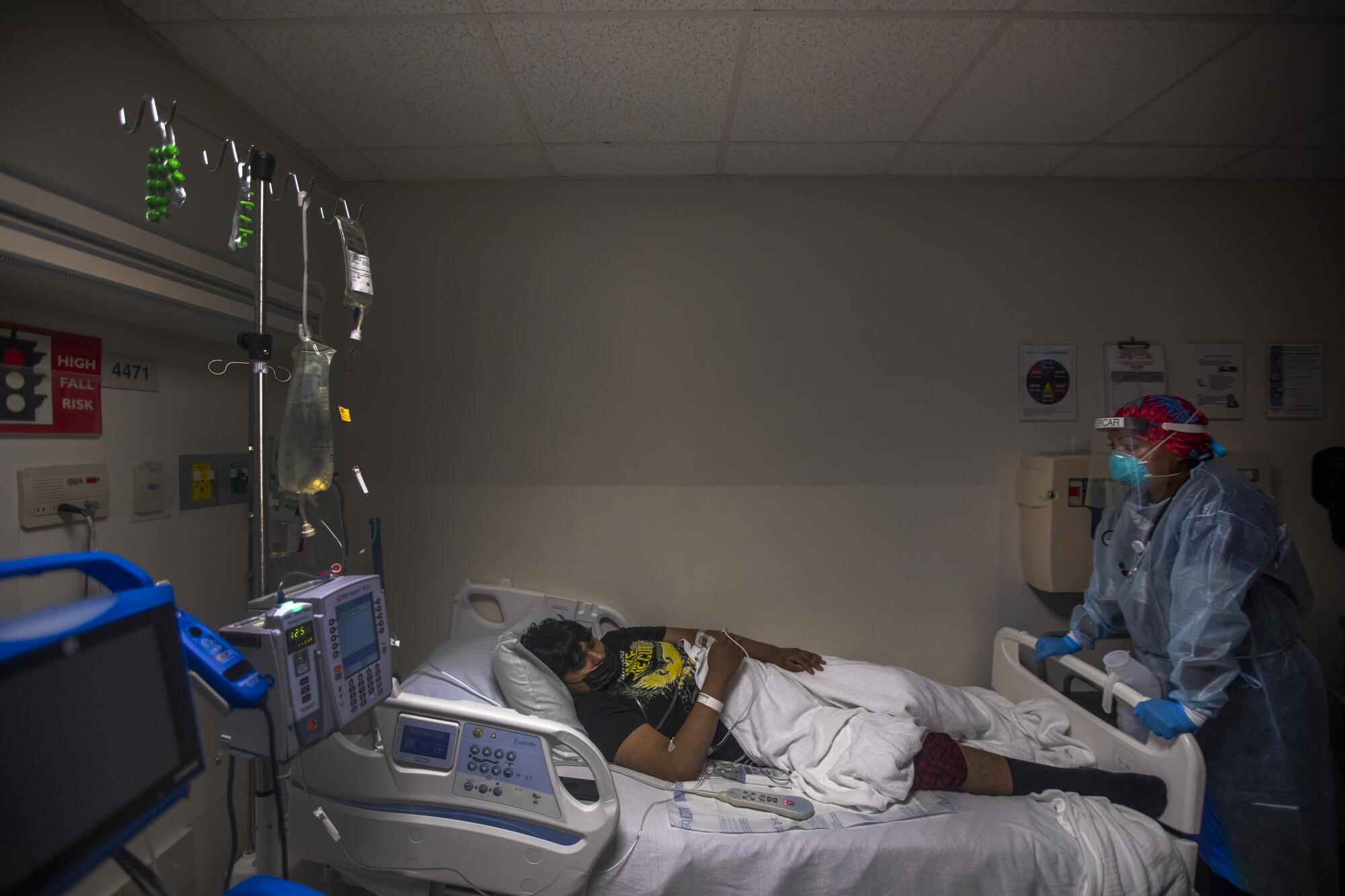
In a dim room in the ICU, she lifted the eyelids of a 54-year-old man who was sedated and on a ventilator, a gang of tubes extending from his mouth. She said good morning and introduced herself, even though it was unclear what he could hear.
Her wrist was circled with a silver bracelet with a prayer for protection in Arabic, a gift from a friend during the pandemic. Around her neck was the Hindu symbol of the Om, another personal emblem of protection.
The surging numbers have forced Sircar to reassess one of the few freedoms she had allowed herself when COVID-19 seemed to be retreating. In May, she moved back in with her elderly mother and her sister, rejoining them after more than a year living in a separate apartment. She had moved out to avoid endangering her immunosuppressed mother.
Her mother is now vaccinated, but Sircar still avoids sitting in the same room or driving in the same car with her. She changes out of her scrubs, doffs her shoes and showers before venturing through the shared house. She leaves home early and comes back as late as she can, trying to minimize the risk.
Even that has begun to feel fraught as more and more people are hospitalized with COVID-19. She has begun to think about moving out again before fall, when the numbers could surge higher.
Earlier this summer, she took time off for the first time since the eruption of the pandemic. Sircar said that as she forced herself to stop logging on to check on patients, it took three days for her to come down from the adrenaline that has powered her through suffering and death and the day-to-day work of ensuring that people survive.
“The weight of the entire year, the exhaustion just hit me,” Sircar said.
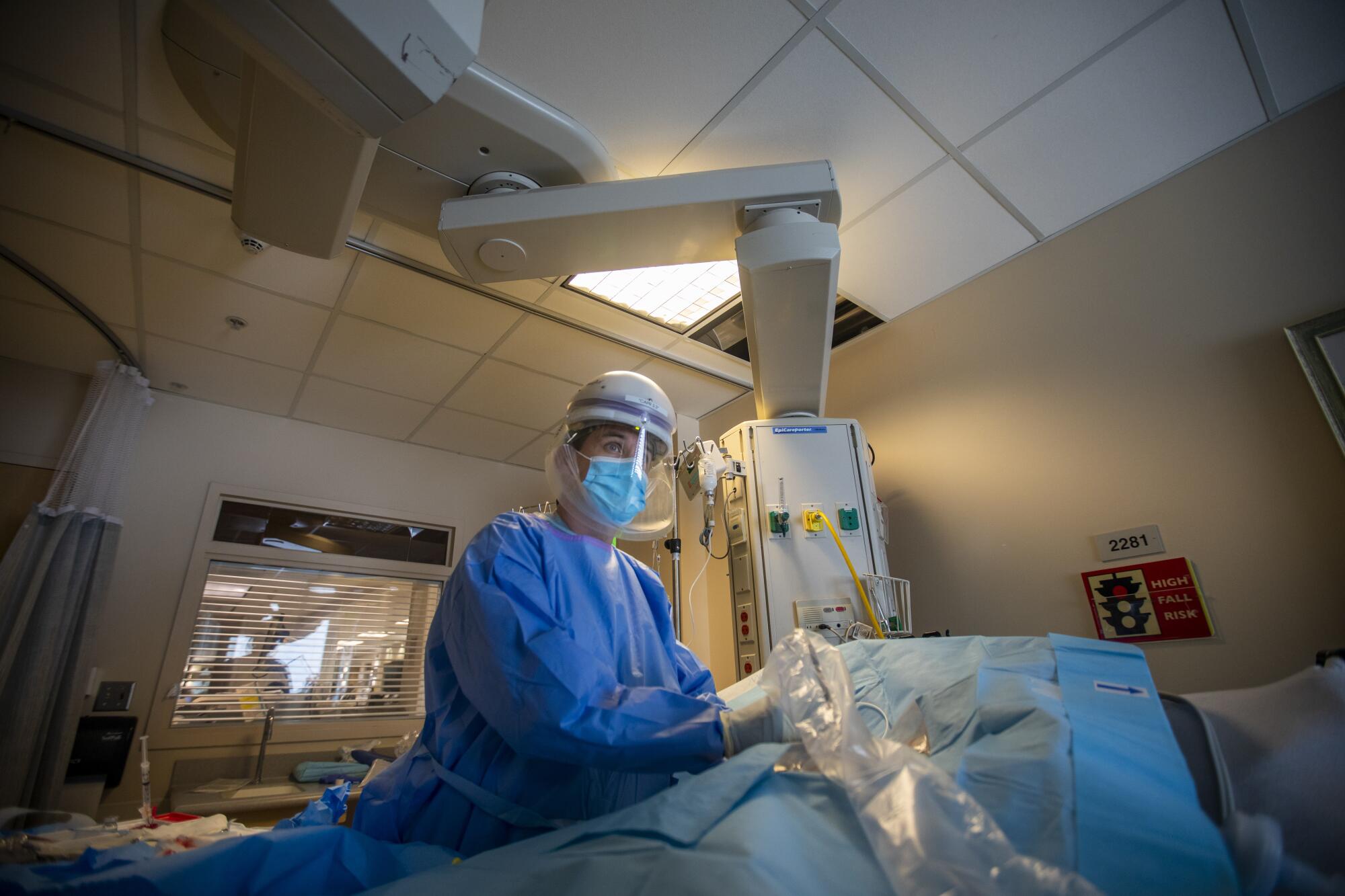
At the hospital that Thursday afternoon, Sircar turned her attention to the COVID-19 patients outside of intensive care or the emergency room. She tied on a fresh disposable gown and pulled on yet another set of blue gloves before stopping in to see Angel Cordero, the 19-year-old who had joined his mother and father in the hospital with COVID-19.

Cordero said he had held off on going to the hospital until his symptoms worsened, to the point in which he was coughing so hard that his chest hurt. Cordero said he and others in his family had been planning to get vaccinated, but hadn’t had a chance because of long hours at work for his family.
“It’s the worst experience ever,” he said, when asked what he would want people to know about what he was going through. “I should have got vaccinated. I should have got, way earlier, vaccinated.”
COVID-19 hospitalizations have essentially doubled across much of California over the past two weeks — a troubling trend officials say illustrates the pandemic’s continued potency amid an ongoing surge in infections.
Sircar, standing at the foot of the bed, gently walked him through what to expect. She ran through the battery of medicines he would be getting to tackle his pneumonia and coached him to avoid lying on his back. She sat on the edge of the bed to demonstrate how he should sit up to eat his hospital meals, explaining that it would remind his lungs to breathe.
“Can you sit at the edge of the bed for me?” she asked.
Cordero slowly pulled himself up, a web of cords pulling along the bedsheets. Sircar held the stethoscope against him to listen to his breaths. Not terrible, she told him.
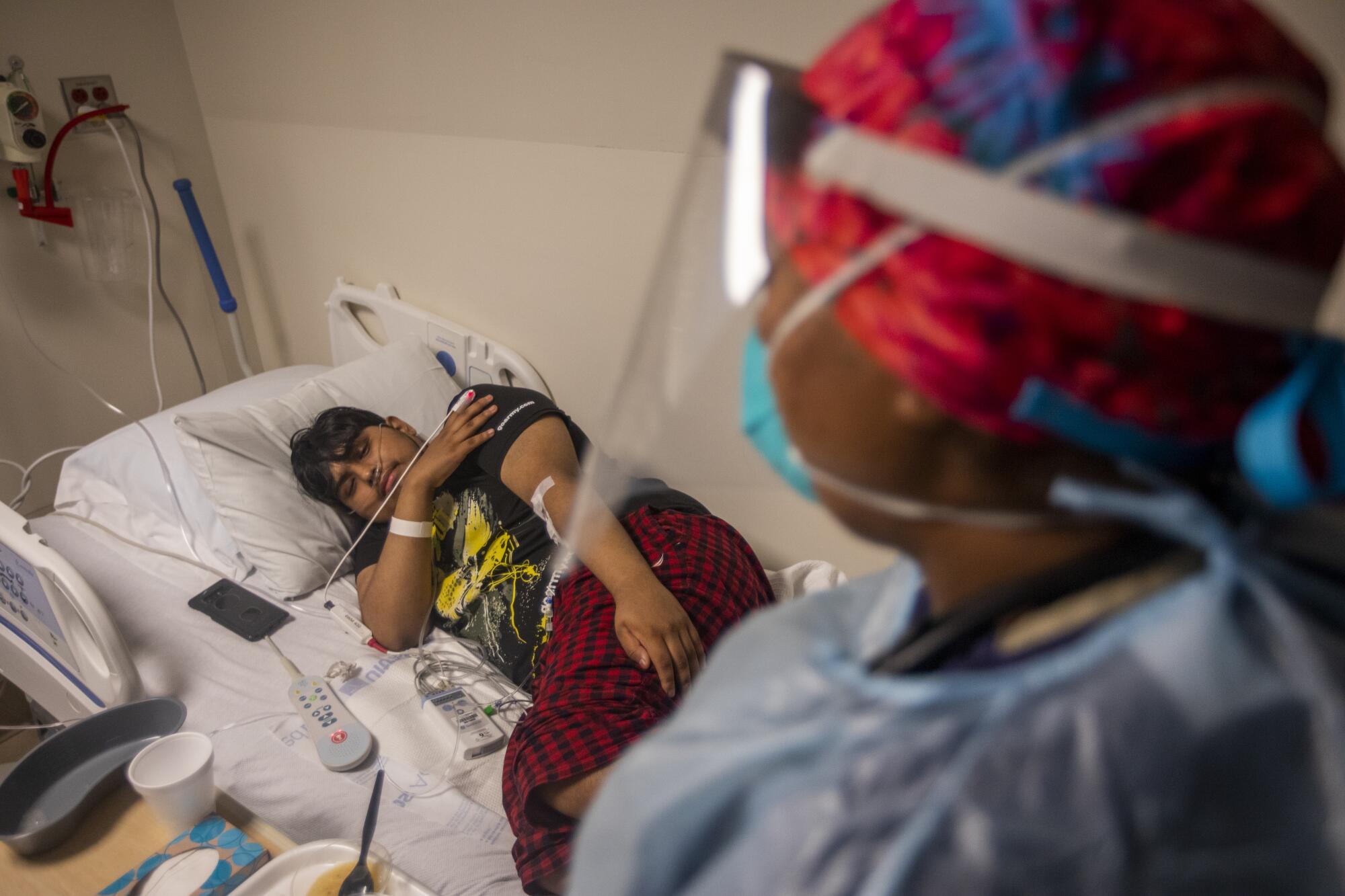
She held up a device called an incentive spirometer, describing it to Cordero as kind of a toy to exercise his lungs. To use it, she explained, he would suck on the mouthpiece like he was drinking a milkshake. He tried, then began to cough.
When he could take those deep breaths without coughing, Sircar told him, she would know he was heading toward recovery. “Do you have questions for me?” she asked. “Is there anything I can do to make it better for you?”
“I just want to see how my parents are doing,” he said.
“OK. We’ll go check on them.” Sircar paused. “Are you scared?”
“Yeah, about my dad,” he said, his voice starting to waver.
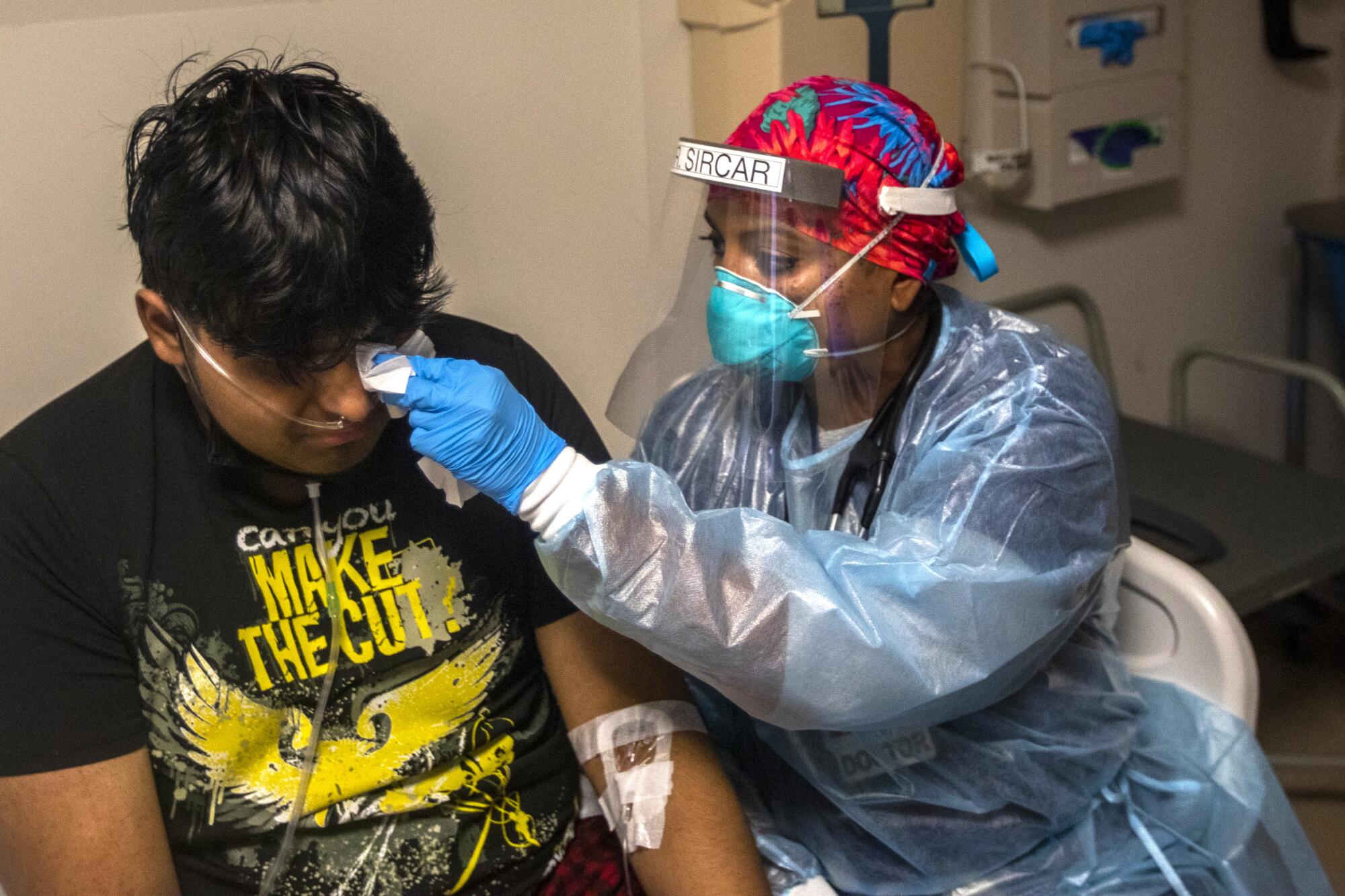
Sircar reassured Cordero as he began to cry, telling him she had seen hundreds of COVID-19 patients, that doctors had gotten much better at treating the virus.
“But you’ve got to work on taking care of you. Right?” she said, holding a tissue to his eye. “Because when your dad gets home, you’re gonna have to take care of your dad a little bit, right? So we want you to be healthy to be there for him.”
“OK?” she said gently. “This is not the end. OK?”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.