With new coronavirus wave, L.A. faring much better than New York. Can it last?

- Share via
Los Angeles County is doing significantly better than New York City so far in this latest spring wave of Omicron cases, and officials remain hopeful that California can avoid the significant increases in coronavirus hospitalizations seen on the East Coast.
The New York City health commissioner, Dr. Ashwin Vasan, said Tuesday that the city was entering a high COVID-19 alert level, warning that there is high community spread of the coronavirus and “pressure on the healthcare system is increasing.” He reiterated a call to wear masks in indoor settings and also urged seniors or others at high risk of severe COVID-19 to wear a mask in crowded outdoor settings and to avoid gatherings.
By contrast, L.A. County is poised to enter the medium COVID-19 community level this week, and “COVID-19 is not currently straining our healthcare system and our healthcare resources,” L.A. County Public Health Director Barbara Ferrer said Tuesday.
L.A. County remains far from meeting its own metrics for a new mask order, but a moderate increase in coronavirus case rates has officials concerned.
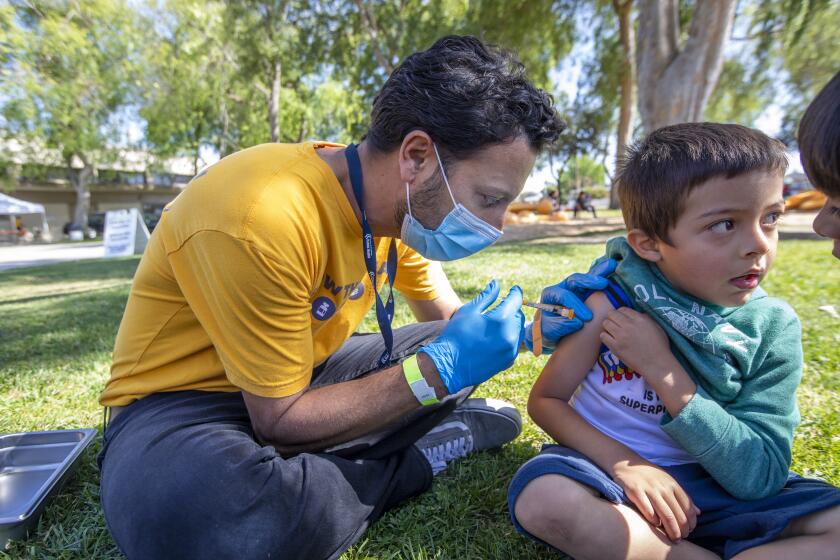
Ferrer has urged residents to wear high-quality masks — like KF94, KN95 and N95 respirators — while indoors, get vaccinated and boosted, get tested when feeling sick or potentially exposed to the coronavirus, and prefer to gather in well-ventilated areas, with outdoors offering the lowest risk.
But Ferrer added that she is optimistic that L.A. could potentially avoid reaching a high COVID-19 community level, which would prompt the Department of Public Health to require universal masking in indoor public settings.
Ferrer also reiterated that she felt people could enjoy gatherings and activities, while suggesting they take prudent precautions.
“While we are disheartened that the pandemic hasn’t ended, I am reassured that with the tools at hand, we can continue to enjoy our time with each other and our participation in those activities we love,” Ferrer said.
New York City’s per capita coronavirus case rate is 50% higher than L.A. County’s, at more than 300 weekly cases for every 100,000 residents, compared with L.A.’s more than 200 weekly cases for every 100,000 residents.
As L.A. County’s coronavirus cases continue to climb, infections are rising fastest among wealthier residents, a likely echo of previous waves in which a greater rate of higher-income people became infected with the virus first.
And New York City’s rate of new hospitalizations is triple that of L.A. County’s, tallying 10.2 new coronavirus-positive hospital admissions weekly for every 100,000 residents, compared with L.A. County’s rate of 3.1 new hospital admissions for every 100,000 residents. A rate of 10 or higher is reason for a greater degree of worry for increasing strain on the hospital system.
Several potential reasons might explain why New York City is experiencing a worse increase in cases and hospitalizations than L.A.
New York City has a lower booster rate among seniors ages 65 and older compared with L.A. County. About 58% of seniors have received a booster shot in New York City, compared to 67% of seniors in L.A. County.
And while mask use has been reduced nationwide as the Omicron surge faded, people who have visited both metropolises recently have observed that people have been more likely to wear masks in L.A. County than New York City, including when it’s not required.
Part of that is likely due to the fact that L.A. County reimplemented a mask mandate that lasted 7½ months as soon as the first signs of last summer’s Delta wave began emerging, and mask use became an ingrained habit for a number of Angelenos that persisted even after the mask order ended March 4.
By contrast, New York City spent much of the last half of 2021 without a mask order, and a statewide mask mandate for venues that didn’t check for vaccination status was implemented for a two-month period, starting in mid-December, at the direction of New York Gov. Kathy Hochul.
Health officials are urging precautions, including masking, as transmission levels tick up across the state.
Differing circulating Omicron subvariants might also be a factor. In California, the highly contagious Omicron subvariant, BA.2.12.1, seems to be accounting for only about 50% of circulating coronavirus cases, Ferrer said, citing state estimates, and that variant’s growth is being limited by the increase of another contagious subvariant, BA.2.3.
By contrast, BA.2.12.1 is more prolific on the East Coast, with the subvariant making up nearly 75% of cases in New York and New Jersey, according to the U.S. Centers for Disease Control and Prevention. BA.2.12.1 is the variant likely to be fueling the East Coast’s “significant increases in cases and now in hospital admissions,” Ferrer said.
In L.A. County, coronavirus cases have been climbing for seven weeks, but hospitalizations have not kept pace at levels officials would’ve expected in previous waves.
It took roughly seven weeks to get from a post-Delta low of about 800 cases a day to a winter Omicron surge high of 42,000 cases a day, a pandemic record. In this wave, L.A. County has moved from a post-winter surge low of about 600 cases a day to 3,000 cases a day
Over a roughly similar time period leading into the winter Omicron surge, coronavirus-positive hospitalizations in L.A. County rose from about 600 to more than 4,800, causing strain on the facilities. This time, coronavirus-positive hospitalizations have remained low — dipping from 350 in late March to a low of 209 in late April; as of Monday, they were back up to 327.
In the county’s public hospital system, coronavirus-positive hospitalizations remain steady and low. Most who are hospitalized with a positive coronavirus test within the Department of Health Services’ hospitals are there for a reason other than their coronavirus infection, such as a heart attack or stroke, not for treatment of COVID-19, said Health Services Director Dr. Christina Ghaly.
“With these new tools — vaccinations, boosters and now therapeutics — you reduce the chance of infected people ending up in the hospital. And that’s why, even though we’ve seen this 200% increase in cases — we’ve seen a tiny increase in hospitalizations,” Ferrer said.
“And I think that is the good news. And if we can continue to keep a check on how much transmission there is and make sure people have good access to vaccines, boosters and therapeutics, we have a chance, I think, a good chance, at never going into that high community level that so many places on the East Coast are now experiencing,” Ferrer said.
“That would be my hope ... that we’re able to use all these tools to keep ourselves out of an accelerating risk for the healthcare system,” Ferrer said.
Ghaly said that with all the new antipandemic tools available, “the risk of overwhelming the hospital system at this point is significantly less likely, because of the wider availability of the vaccine and the level of immunity that’s present among the community. And that risk really doesn’t feel, at this point, that prevalent or likely.”
People who are diagnosed with a coronavirus infection should be aware that, if they’re at higher risk, they may be eligible to take anti-COVID medications that reduce the risk of severe illness and death, such as Paxlovid. The antiviral oral drug treatment is now widely available in California for free; prescriptions can be provided by healthcare providers or by going to a “Test to Treat” site at designated pharmacies.
To be sure, there remain plenty of signs of concern, and Ferrer has said everyone should take seriously their responsibility to try to avoid getting infected and spreading the coronavirus to other people.
Beyond the threat of hospitalizing vulnerable people who get infected, there is the possibility of contracting long COVID following an infection, in which symptoms such as chronic fatigue or brain fog can persist for months or years. A coronavirus infection could result in increased risk for conditions such as heart disease and diabetes.
And then there’s the discomfort of undergoing an illness that can still be deeply unpleasant, even if it doesn’t require a hospital stay, and the requirement in L.A. County that infected people isolate for at least five days, and as many as 10 days, after confirmation of a coronavirus infection.
Coronavirus cases in L.A. County continue to increase, rising from about 2,600 cases a day to nearly 3,000 cases a day, a 16% week-over-week increase. The latest case rate is 206 weekly coronavirus cases for every 100,000 residents, above the threshold rate of 200 that will likely place L.A. County into the CDC’s medium COVID-19 community level later this week.
The placement in the new tier, however, won’t result in any changes, as L.A. County already goes beyond what the CDC recommends for counties in the medium COVID-19 community level.
Case rates have risen rather dramatically among teens and younger adults, with the sharpest jump among youths ages 12 to 17, followed by adults younger than age 50. “High case rates among these individuals, as we’ve seen in the past, are likely to significantly contribute to continued transmission in both schools and at work sites,” Ferrer said.
“It doesn’t look like we’ve plateaued,” Ferrer said. “And certainly those people that are out and about the most have the highest case rates; then that makes it easier for them to spread to everybody else,” Ferrer said.
Case rates are particularly high in the wealthiest communities, a pattern seen earlier in the pandemic in which richer people get hit by a wave first, followed by poorer people. “Given the past trends, and the increase that we’re seeing in transmission at work sites, we are concerned that the rates in the lower-resourced communities may once again rise higher than the case rates in the wealthier communities,” she said.
Ferrer said there were 195 work sites reporting clusters of coronavirus cases between May 9 to 15, a number that’s climbing. Most were in the retail-trade sector — concentrated in food and beverage stores; building material and garden equipment and supply dealers; and electronics and appliance stores — as well as in the manufacturing, finance and insurance industries.
California on Tuesday was reporting an average of 10,100 cases a day, up 17% over the prior week, for a rate of 181 weekly coronavirus cases for every 100,000 residents. The rate of increase was more modest than the previous week-over-week increase of 23%.
The San Francisco Bay Area still has California’s highest coronavirus case rate, at 290 weekly cases for every 100,000 residents. Southern California has the state’s second-highest rate, at 160; Greater Sacramento, 153; rural Northern California, 103; and the San Joaquin Valley, at 102.
In Southern California, San Diego County’s rate is 182; Santa Barbara County, 163; Ventura County, 153; Orange County, 121; San Bernardino County, 113; and Riverside County, 111.
A case rate of 100 and above is considered a high rate of transmission, the worst tier on the CDC’s transmission level criteria.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.