Will everyone in California eventually get coronavirus? What we know

- Share via
With tens of thousands of new coronavirus cases being reported in California each week, it might seem inevitable that everyone will get infected at some point.
But that’s not necessarily the case, officials and experts say. Even with the near-constant drumbeat of transmission this spring and summer, millions of Californians have still been able to avoid catching the virus.
For some, that might be a matter of circumstance — their work or living situations allow them to rarely venture into crowded settings. Others may still be avoiding nonessential activities to lessen their exposure risk.
Many might chalk it up to luck.
“The storyline is, ‘Everybody’s gotten it.’ But the reality is a lot of people haven’t,” said Dr. Peter Chin-Hong, a UC San Francisco infectious-disease expert.
While there’s no silver bullet, residents can still take reasonable precautions to lessen their chance of getting infected.
“Everyone needs to be vigilant to avoid exposure and prevent severe disease,” especially during periods of high community transmission, said Dr. Robert Kim-Farley, an epidemiologist and infectious-disease expert with UCLA’s Fielding School of Public Health.
Since the hyper-transmissible Omicron variant appeared in early December, the coronavirus has affected nearly every family and social circle.
Vaccines
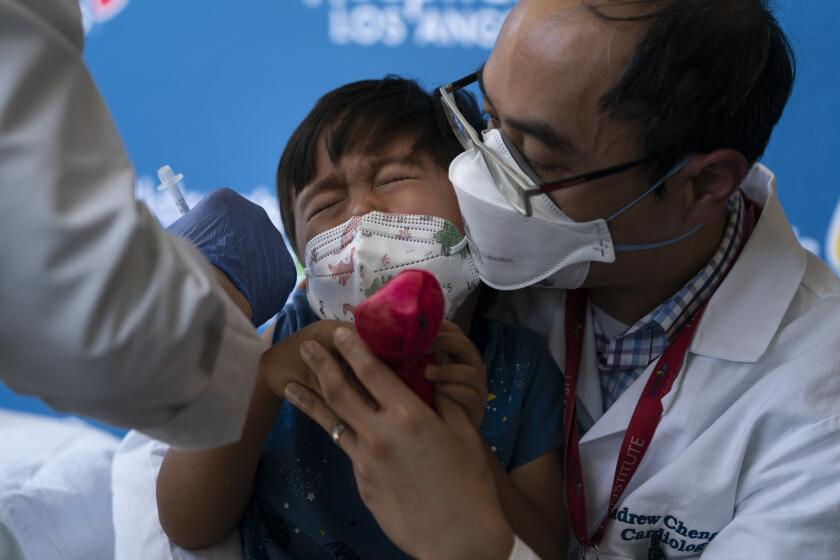
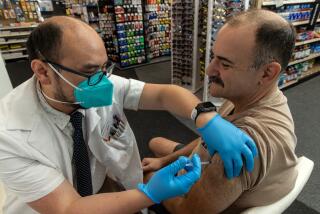
Getting vaccinated and boosted remains one of the best ways to stave off infection — and especially to avoid the most serious health impacts of COVID-19, officials and experts say.
The vaccines “are, in fact, doing exactly what we need them to do: They’re preventing severe illness and death,” Los Angeles County Public Health Director Barbara Ferrer said.
“I want folks to feel confident that their actions are making a difference,” she said Tuesday during a presentation to the county Board of Supervisors. “They protect our entire community from the worst impacts of the pandemic.”
According to the latest state data, unvaccinated Californians were five times more likely to get COVID-19 than their vaccinated and boosted counterparts. They also were eight times more likely to be hospitalized with COVID-19, as well as to die from the disease.
“Some of the new things that are keeping transmissions at bay potentially are the fact that kids now under 5 are getting vaccinated, kids 5 and over can get a booster, there’s more Paxlovid going around. All of that might keep community viral load lower than it would have been,” Chin-Hong said.
But although most Californians have already completed their primary vaccine series, demand for boosters has been lower. Vaccination rates for children ages 5 to 11 have also lagged well behind other age groups, and the youngest children only just became eligible for the shots.
Following the decision by federal health officials to authorize children as young as 6 months to receive the COVID-19 vaccines, Californians are able to book appointments for their tiniest charges.
The fact that vaccine protection wanes over time underscores the importance of staying up to date on the shots, experts say.
According to research published this month in the New England Journal of Medicine, two shots of COVID-19 vaccine without an additional booster offer essentially no lasting protection against infection with Omicron. That highly transmissible strain, as well as its family of subvariants, is responsible for essentially all new coronavirus infections at this point.
At the same time, any immunity appears to offer significant and lasting protection against serious illness, hospitalization and death, researchers found. And if you haven’t had either the virus or the vaccine, doctors urged, it’s better to get the jab.
“The fact that I and a fair number of people who continue to be careful and are fully vaccinated and boosted remain COVID-free tells me that it’s possible we will continue to be that way, so I don’t buy the inevitability argument,” said Dr. Robert Wachter, chair of UC San Francisco’s Department of Medicine. “On the other hand, there are plenty of people who I know who have been just as careful as I have and have gotten it in the past few months, so I think there’s some randomness to this.”
The Omicron strain of the coronavirus keeps generating new subvariants. Here’s a look at how they stack up.
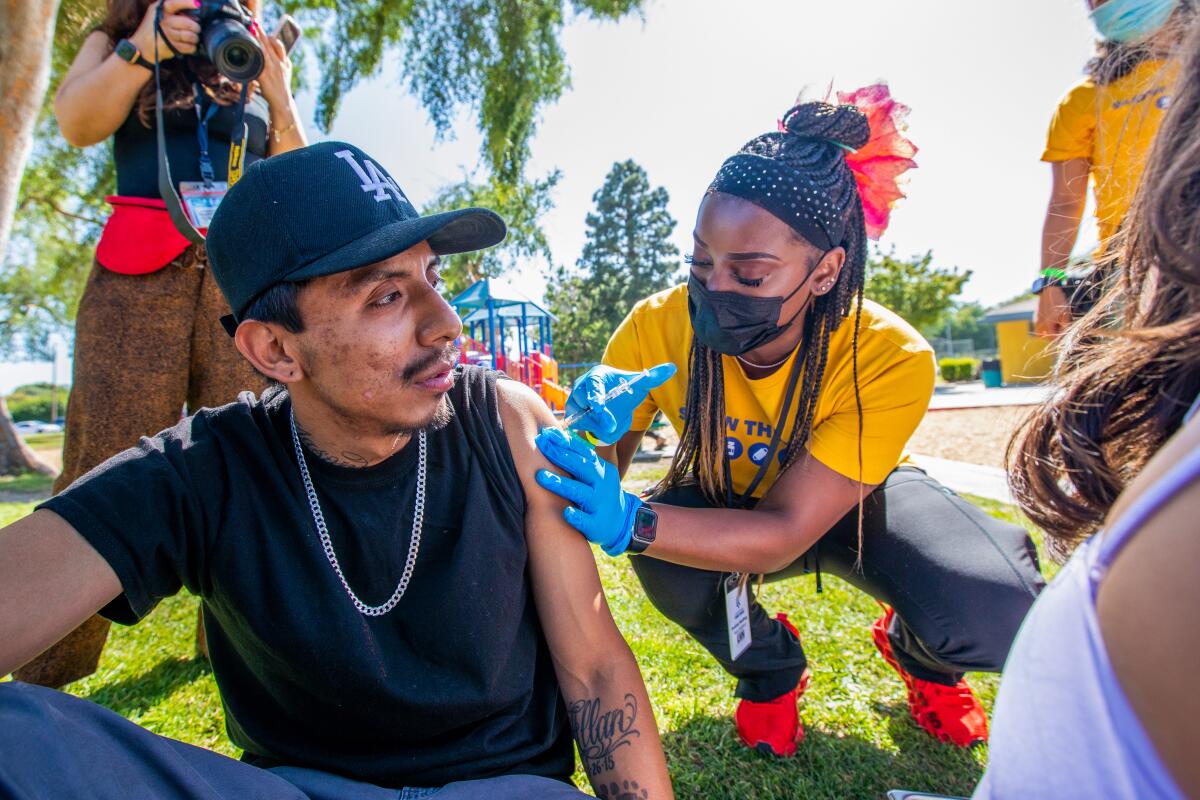
Masks
Although masks are no longer required in most indoor public settings, health officials still encourage their use, saying they can literally provide an extra layer of protection.
“Masking when in crowded indoor settings and being vaccinated and boosted are still the best protections. Also, if one becomes infected and symptomatic, medicines such as Paxlovid will significantly reduce the severity of the disease, especially for persons at higher risk,” Kim-Farley said.
The California Department of Public Health recommends people use medical-grade face coverings, such as surgical, N95, KN95 or KF94 masks. Wearing an old, loose, cloth mask alone is less effective, but placing one on top of a surgical mask can be more effective than a surgical mask alone as it tightens the fit.
Though the magnitude of this latest coronavirus wave sparked concerns that governments would return to mask mandates, that has not been the case.
The exception was Alameda County, which in early June became the first California county to reinstitute a mask order covering most indoor public settings. But officials rescinded that Saturday, citing improved conditions.
Three weeks after becoming the first California county to reinstitute a mask mandate in most indoor public settings amid climbing coronavirus cases and hospitalizations, Alameda County has rescinded the order.
Health officials in Los Angeles County have said they would reimpose a public indoor mask mandate should the region fall in the high COVID-19 community level for two consecutive weeks. That category, the worst on a three-tier scale defined by the U.S. Centers for Disease Control and Prevention, indicates not only significant community transmission but also that hospital systems may grow strained by coronavirus-positive patients.
Based on recent hospitalization trends, L.A. County would likely not reach that category until the end of July. But that timeline hinges on real-world conditions.
“We cannot predict with certainty what the future hospitalization trend will look like. Hospitalizations could level off, they could even begin to decline, and that would be a great relief, or they could begin to increase more rapidly,” Ferrer said. “With the continued proliferation of new Omicron subvariants and sublineages, it’s very difficult for us to accurately predict the rate of future hospitalizations.”
Masks may not be required in many places but they’re still encouraged, officials say, as new COVID cases continue to climb.
Testing and ventilation
Another strategy to reduce infection risk is to ask that friends and family members test themselves before attending group functions. A test administered close to an event’s start could alert someone they are infected and allow them to avoid unwittingly spreading the virus.
Ventilation is also important. Holding events outside or opening windows and doors can also help lessen the chance of spread.
“It does remain important for all of us to use the measures that work to reduce our COVID-19 risk,” Ferrer said. “That includes, of course, vaccinations, boosters, masking, moving activities outdoors, maximizing ventilation if you’re indoors, and testing and staying home if you’re sick.”
Despite the latest surge in coronavirus cases, the impact on hospitals has been relatively minor and COVID-19 deaths have remained fairly low and stable.
Travel
The CDC recommends residents consider planning their journeys for off-peak times when public transportation and transit hubs are less crowded.
If possible, opening a window can also improve ventilation.
The agency also recommends that everyone 2 and older wear a mask while aboard public transportation or in indoor transit settings such as airports.
California health officials echo that recommendation. In L.A. County, masking is required in indoor public transit settings.
Personal choice
Depending on personal preference or risk factors, some residents may also opt to avoid certain activities — such as dining indoors, seeing a movie or working out at the gym.
But more than two years into the pandemic, officials and experts say taking precautions can reduce the transmission risk in many settings.
Chin-Hong said his approach “is not that I’m going to prevent by all costs myself from getting infected” but he’s “taking a measured approach towards adjudicating my risk.”
And, as Wachter noted, “We’re humans. We’re social creatures. We were meant to get out and do things.
“All of us have to make choices about the level of risk that we’re willing to take,” he said. “And that’s true when we get up and get out of bed in the morning; it’s true when we get on an airplane; it’s true when we get in the car.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.