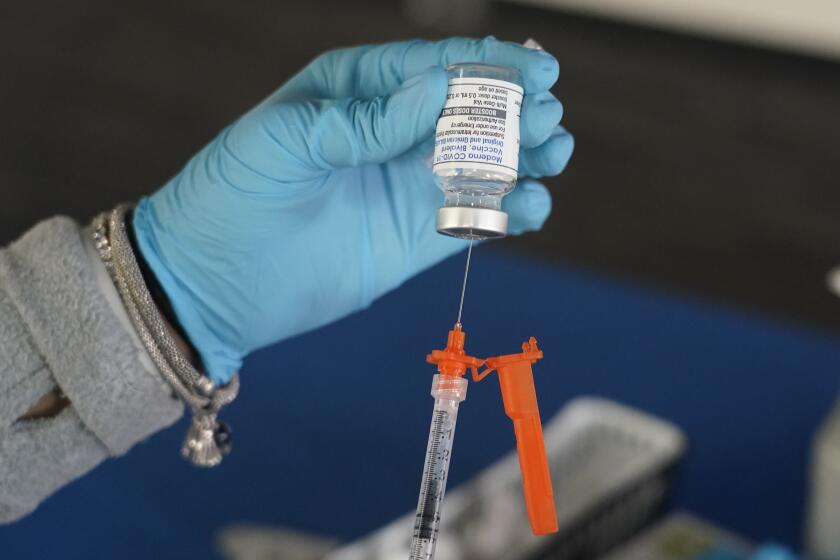
Dangerous weeks ahead in L.A. County as coronavirus suddenly surges. Here is why

- Share via
A few weeks ago, there was cautious optimism that this winter would not see a significant COVID-19 surge.
But in Los Angeles County, that outlook is in jeopardy. Coronavirus case counts are climbing rapidly, sending increasing numbers of Angelenos to the hospital and raising the possibility of a renewed public indoor mask mandate that could arrive shortly after the new year.
But why is the nation’s most populous county contending with such a significant spike?
Some factors that may be at work include a shorter incubation period for the latest Omicron strain, meaning there would be fewer days between when someone is exposed to the virus and when they become sick.
“People came back from Thanksgiving and pretty quickly were testing positive,” county Public Health Director Barbara Ferrer said. At her agency, “we had more people who tested positive right after Thanksgiving than we’ve ever had before,” with transmission occurring during holiday gatherings, rather than at work.
BQ.1 and BQ.1.1 are now the dominant versions of the coronavirus circulating nationwide. Their parent strain, BA.5, was said to have an incubation period of three to five days.
Also on the rise are coronavirus-positive hospital patients, raising the specter of an indoor public mask order in L.A. County.
California hospitals are starting to see significant increases in virus-infected patients. The number has doubled in the last three weeks — from 2,094 to 4,321 as of Tuesday — and is nearing last summer’s peak of 4,843.
And the burden is expected to grow. Statewide, there were an estimated 6,100 Californians hospitalized for either COVID-19 or flu as of Tuesday. That figure could reach 10,000 by late December or early January, according to Dr. Mark Ghaly, the California health and human services secretary.
“We are hearing from more concerned health systems and watching the data closely,” Ghaly said.
Reported case counts also likely understate the extent of infection. Officials in Santa Clara County, Northern California’s most populous, said wastewater data is showing at least one area — Palo Alto — with coronavirus levels at an all-time high, even higher than the first Omicron surge that roared to life a year ago.
Dr. Sara Cody, the county’s public health director, warned that this winter is shaping up to be “extraordinarily difficult,” pointing to sewage data suggesting coronavirus levels are “absolutely skyrocketing.”
Flu and respiratory syncytial virus, or RSV, are making things worse. According to the U.S. Centers for Disease Control and Prevention, the cumulative flu hospitalization rate nationally is higher for this time of year than every season since 2010.
The number of flu hospital admissions in the U.S. has doubled in a week. And the CDC estimates there have already been 4,500 flu deaths since the start of October.
The U.S. is seeing the highest recorded outpatient volume for flu-like illness in November since 2009, Dr. Peter Chin-Hong, a UC San Francisco infectious diseases expert, said at a recent town hall. The highest rate of outpatient visits are in babies and children up to age 4, he said.
Officials are urging everyone who is eligible to get the flu vaccine, which is recommended for those 6 months and older.
Hospitals also are starting to feel the effect of viral waves that are sickening workers. UC San Francisco has reported a sharp rise in coronavirus levels among its staff, mostly from exposures in the community and not at work, Dr. Ralph Gonzales, an associate dean at UC San Francisco, said at the campus town hall.
“We’re now reaching critical staffing levels that are going to make things challenging,” Gonzales said.
And children’s hospitals across California remain stressed. Even amid optimism that RSV is starting to crest, flu and COVID-19 are rising among children.
“Many hospitals around the state are at or beyond capacity to care for infants and children with respiratory illnesses,” Dr. Joan Zoltanski, chief medical officer for UC San Francisco Benioff Children’s Hospitals, said at the town hall. Already, the children’s hospital in San Francisco has had to erect a tent to care for more patients.
The crisis at children’s hospitals began in October, when RSV began surging. Pediatric emergency rooms in San Francisco and Oakland are almost continuously at high occupancy, and patients who normally would be admitted are having to be treated in the ER, Zoltanski said.
“Hospitals across the state are working to add pediatric beds as quickly as possible, but the number of children who need hospitalization is currently outpacing their ability to expand,” the California Department of Public Health said in a statement Tuesday.
Hospitals typically have about 35% to 40% of open pediatric intensive care unit beds, but that number is down to about 20% statewide, the department said. It’s even lower — below 12% — in some regions.
Based on death certificate data, at least 36 fatalities from flu and 14 from RSV have been reported in California since October. Three of the RSV deaths have been among children. Those numbers are most likely an undercount.
For the week ending Wednesday, L.A. County reported an average of 3,929 new coronavirus cases a day — double the rate from Thanksgiving. On a per capita basis, that’s a rate of 272 cases a week for every 100,000 residents. A rate of 100 or more is considered high.
A year ago, the county was recording 113 new cases a week for every 100,000 residents.
“We’re having this increase starting a little bit earlier,” Ferrer said in an interview with The Times.
Public health officials have long marked Thanksgiving and the wider winter holiday season as a potential starting point for a surge. With so many gatherings scheduled over just a few weeks, and many held indoors due to colder weather, conditions are ripe for a coronavirus rebound — as has happened each of the past two years.
The multigenerational nature of such events also plays a role, as older residents are more at risk of developing severe COVID-19 illness.
With coronavirus cases and hospitalizations rising in Los Angeles County, officials are voicing new confidence in the effectiveness of the updated COVID-19 booster shot.
Ferrer said she’s concerned that many people have stopped worrying about COVID-19. But if there’s any time to start paying attention, it’s now, as “we are seeing a rapid acceleration again,” she said.
“Putting on these masks, we could reduce disruptions pretty dramatically in your own lives, your family’s lives, as well as your work and school lives. So I think it would make a difference,” Ferrer said.
Ferrer said some people have told her they’d rather take the risk of infection, even during periods of high transmission, than wear a mask again. But there are others who’d readily agree to put a mask back on if required, she said.
“I would say it’s pretty equally split between people who say, ‘I’m done and I want to move on,’ and other people who say, ‘I just need you to be decisive about what it is we’re supposed to do,’ ” Ferrer said.
Officials also stress that it’s important to get updated COVID-19 vaccine boosters — which were introduced in September — and are urging more doctors to prescribe antiviral drugs like Paxlovid for eligible patients.
“That also would accomplish one of our biggest goals,” Ferrer said, which is reducing how many people are falling severely ill.
And she urged people to not be dismissive about the fact that it’s older people who are most likely to die from COVID-19. Preventive measures such as wearing a mask can reduce illness, she said.
Holiday events can result in coronavirus outbreaks, but taking certain precautions can reduce the risk. Strategies include taking events outside and wearing a mask when not actively eating and drinking, Ferrer said.
Hospitalizations among those 70 and older have surpassed the summer peak. Coronavirus cases for all age groups are up nearly 50% in just one week.
At smaller gatherings in homes with friends and family, hosts may consider having everyone take a rapid coronavirus test before the event, Ferrer said. It will help identify those who are most likely to be infectious, even if they’re asymptomatic.
But a testing-only strategy alone is not perfect, because there are situations in which some people are contagious but not yet testing positive on a rapid coronavirus test.
And of course, officials say residents should stay home if they’re sick.
“This is about real people, real lives, real families and real communities across the state, so doing your small part helps the state certainly. But more importantly, it helps you and your family have the safest holiday season that you can,” Ghaly said.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.