Number of Latino doctors isn’t keeping pace with population, study says
- Share via
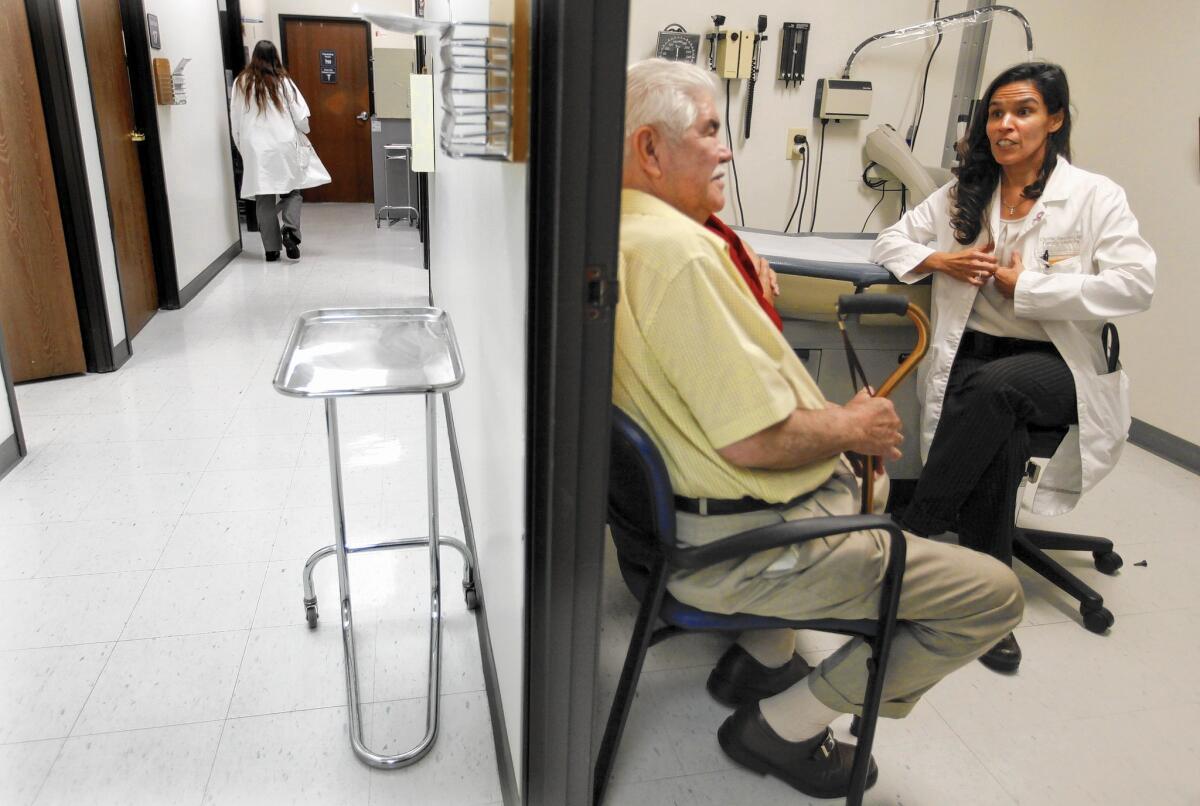
Every day, chronically ill Latino patients stream into Harbor-UCLA Medical Center’s family medicine clinic.
Some have neglected their health because they’re flummoxed or alienated by the medical system, Dr. Gloria Sanchez believes — in desperate need of care from providers who understand their words and their problems.
“Latino physicians tend to be that bridge, this critical piece of healthcare communication,” she said.
But such doctors are in short supply, said Sanchez, a professor and physician at the Harbor City facility.
Latinos as a group suffer disproportionately from poverty-related conditions such as diabetes and heart disease. Under the Affordable Care Act, more of them than ever have access to coverage.
But in a recent analysis published by the journal Academic Medicine, Sanchez and colleagues found that the number of Latino physicians was not keeping pace with population growth and suggested that correcting the imbalance could be key to addressing Latino health disparities.
“It’s not affirmative action. It’s an issue of quality of care,” said David Hayes-Bautista, director of the Center for the Study of Latino Health and Culture at UCLA’s David Geffen School of Medicine and a study coauthor.
Combing through three decades of census data, Sanchez, Hayes-Bautista and other researchers found that the number of people in the U.S. who identified themselves as Latino or Hispanic grew 243% from 1980 to 2010, from just under 15 million to more than 51 million.
In 1980, there were 135 Latino doctors for every 100,000 Latinos in the U.S. By 2010, that number had fallen to 105. The ratio of non-Hispanic white doctors to non-Hispanic white patients, in the meantime, increased from 211 to 315 per 100,000.
When the researchers looked at the five states with the largest Latino populations in 2010 — California, Texas, Florida, New York and Illinois — the Golden State’s Latino-doctor-to-patient ratio ranked lowest, with 50 physicians per 100,000 people.
“I thought the numbers could have been better,” Sanchez said.
On a recent Friday, patients at the Harbor-UCLA clinic said they appreciated that so many doctors there spoke Spanish — and that they found it difficult to get by in medical settings where that wasn’t the case.
Irma Torres, 75, remembered one conversation with her 70-year-old husband, Miguel, when he was hospitalized for a heart condition.
“I asked him, ‘What did the doctor say?’” she recalled. “And he said, ‘I don’t know.’”
Angelina Campos, a 55-year-old who suffers from high blood pressure and migraines, was at the clinic to have her injured knee checked by Sanchez.
Campos said she preferred doctors who were fluent Spanish speakers, but that sometimes it was hard to get an appointment because wait times could be very long. She said she sometimes relied on her pharmacist to translate, after the fact, what an English-speaking doctor had told her.
“I feel more comfortable with a Latino caregiver,” Campos said.
Dr. Faustina Nevarez, an obstetrician at Kaiser Permanente Los Angeles Medical Center, said that internal studies by Kaiser had shown that Spanish-speaking patients were more successful controlling their diabetes, depression and blood pressure when they were able to consult with Spanish-speaking doctors.
In focus groups conducted for a 2009 analysis, most Spanish-speaking patients at Kaiser Permanente Southern California said that they had English-speaking doctors and that they understood “approximately half” of what their doctors told them. Many worried about misinterpreting physician instructions.
Sanchez, 42, said she often encounters patients who don’t seem to have understood what other medical providers told them.
“They’ve been to the emergency room multiple times,” she said. “Whatever was said, it’s not getting across.”
Sanchez said doctors also benefit when they can converse in patients’ native languages.
“With all the demands on doctors — we only have about 15 minutes with a patient — to not have to take the extra step of a phone translation is huge,” she said.
Hayes-Bautista said programs that once helped Latino students reach medical school and thrive have been dismantled. The elimination of race-based admissions at California’s public universities, he said, probably contributed to a drop in Latino enrollment that began in the 1990s.
Improving the Latino doctor-to-patient ratio isn’t the only way to improve care, he said, but it is a cost-effective option. Studies have shown that Latino doctors are more likely to speak Spanish than non-Latino doctors, and also are more likely to practice medicine in underserved areas.
Sanchez said that growing up in a struggling family herself — her father was a Mexican migrant laborer who settled in Orange County — gives her insight into her patients’ plights.
“It’s a shared experience of insecurity and disparity,” she said. “You stress over things that others take for granted. You’re just trying to survive, and when you live life at that level, the complexities of going to the doctor are insurmountable.”
Sanchez counsels her patients to speak up when they don’t understand what a doctor is telling them. Many won’t, finding it awkward to communicate through a translator — or to question a doctor’s recommendation when it’s not in a language they speak.
“They’re embarrassed and scared,” Sanchez said. “They don’t want to be a bother.”
Twitter: @LATerynbrown
Times staff writer Javier Panzar contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.











