How a healthcare revolution came to one red state while the Obamacare battle raged on

Winnie Abbott walks a short trail at City Park in Cave City, Ark. The 80-year-old great-grandmother recently had her knee replaced by a surgeon participating in a statewide effort in Arkansas to improve care.
- Share via
Reporting from Batesville, Ark. — Winnie Abbott desperately wanted a knee replacement when she came to Dr. Jeffrey Angel’s office here in the foothills of the Ozark Mountains.
“I’ve suffered so long,” Abbott, an 80-year-old great-grandmother, quietly told the orthopedic surgeon. “I need to do something.”
Before Angel would operate, though, he had some requests for Abbott. She should take a class about the procedure and designate a family member to be her “coach” to help with recovery. And if she had problems after surgery, she needed to call a 24-hour number at Angel’s office rather than just go to the emergency room.
“We have a program,” Angel explained gently. “Because nobody wants to end up back in the hospital.”
This comprehensive approach to patients – focused not just on what happens in the doctor’s office but on how patients recover at home and how much their care costs – hasn’t always been the rule in American healthcare.
But across the country, far from the vitriolic debate over Obamacare, it is driving a quiet revolution that is changing how doctors replace knees, communicate with patients, prescribe drugs, even deliver babies.
Few places have embraced this revolution more fully than Arkansas, which embarked on one of the most sweeping efforts in the nation to improve healthcare quality and control costs.
“Our goal was to change the way people thought about stewardship of healthcare resources,” said Dr. William Golden, the medical director of Arkansas’ Medicaid program, a key player in the statewide effort. “We wanted to get people away from looking only at their little piece of the system.”
Arkansans live on average nearly three fewer years than other Americans and five fewer years than the residents of top states such as Minnesota and Hawaii.
But unlike most unhealthy states, Arkansas moved aggressively to upgrade its healthcare system after President Obama signed the 2010 Affordable Care Act.
Democrats and Republicans in the statehouse undertook an unusual bipartisan initiative to broaden the state’s Medicaid program through the health law. Since 2013, Arkansas has tied with Kentucky for largest percentage decline in uninsured.
By contrast, no other Southern state elected to guarantee its residents health insurance.
Less noted, Arkansas state leaders also looked hard at how doctors and hospitals across the state were delivering care.
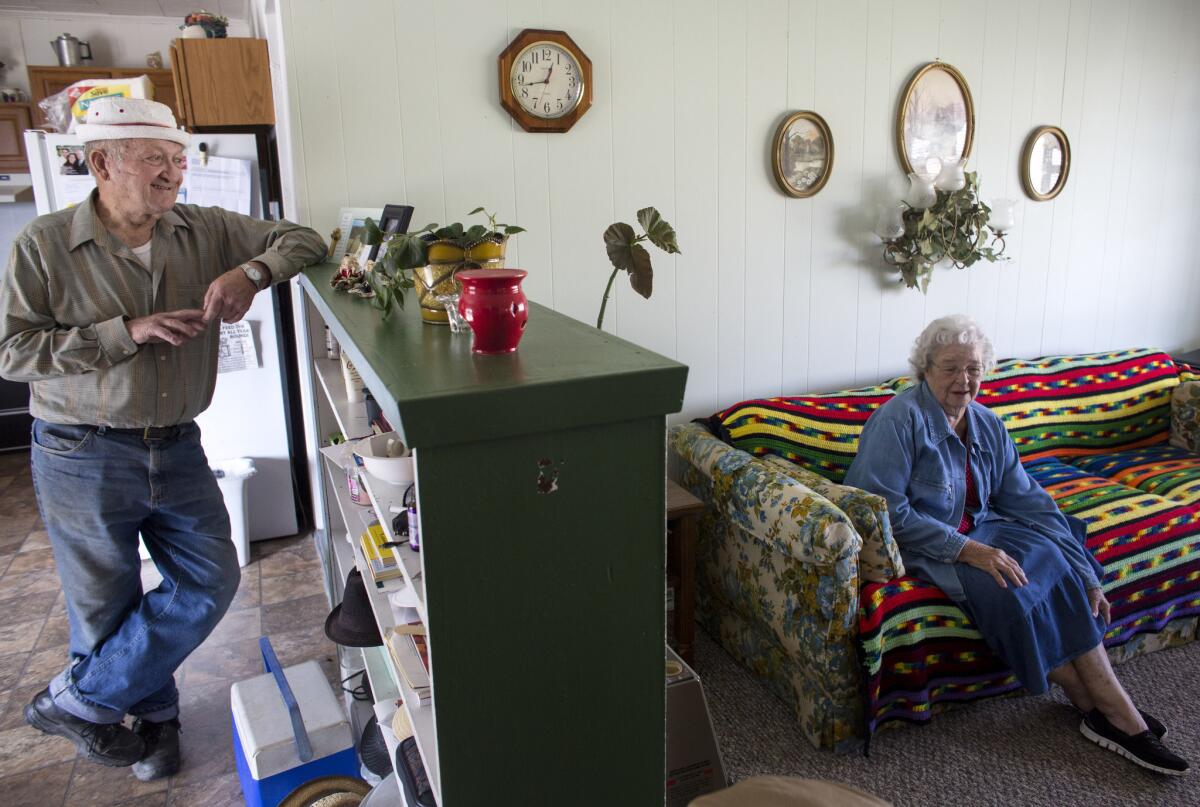
Winnie Abbott underwent knee replacement surgery last year and her husband, John, a pastor at a local church, was assigned to be her “coach” helping with exercises and other tasks. “It certainly changer our routine,” said John of the recovery period at their home in Cave City, Ark.
“Everyone recognized that we had to change,” said Dr. Joe Thompson, the state’s former surgeon general, who helped bring together insurers, doctors and leading employers, including Wal-Mart. “Quite simply, the way we were paying wasn’t getting us the results we wanted,” he said.
For decades, Arkansas physicians, like doctors all over America, had been paid the same way: They billed for every patient visit and procedure. Whether patients got better or whether they ended up back in the hospital after surgery made no difference.
Arkansas decided to try something different.
Private insurers, employers and the state Medicaid program agreed to pay primary care clinics a bonus if they could control the cost of care while hitting quality targets, such as ensuring diabetics got regular blood sugar tests and women got recommended cancer screenings.
Similarly, orthopedic surgeons, obstetricians and other providers would be rewarded based on the cost and outcomes of procedures they performed such as knee replacements, tonsillectomies and deliveries.
“Arkansas is being much more innovative than many, many states,” said Michael Chernew, a health economist at Harvard Medical School who is studying the coordinated state effort. “It’s very ambitious.”
In Batesville, an aging industrial town in the shadow of a hulking poultry plant, that meant some adjustments for Angel.
The 54-year-old surgeon had a busy orthopedic practice, with a steady flow of broken bones, sore backs and knee and hip replacements.
He worked to stay abreast of changes in healthcare. In an office decorated with Arkansas football paraphernalia, Angel works in front of a bank of computer screens, toggling between patients’ medical records, electronic images of X-rays and communications with other providers.
But when replacing hips and knees, Angel had focused mainly on what he did in the operating room, leaving recovery and rehabilitation to others.
Under the new system, the state’s largest insurers, Arkansas Blue Cross Blue Shield and Arkansas Medicaid, began tracking how many of Angel’s patients contracted infections, how many suffered blood clots and how many were readmitted to the hospital.
The health plans also tallied the total bill for his patients’ care, including not just his surgery, but any rehab, extra hospital stays or follow-up emergency care.
“We were a little anxious at first,” Angel said. “Were we going to be able to perform? What if our patients didn’t do what we said?”
After reviewing every part of their practice, Angel and his partners set up new protocols for all his patients.
They now require higher-risk patients to take steps to improve their health before surgery to reduce risk of complications. Obese patients are required to lose weight, for example. Diabetics have to control their blood sugar.
The doctors standardized procedures for managing patients’ pain and planning their recovery, key steps that improve outcomes.
And they set up the 24-hour hotline, so patients could call with questions about their recovery instead of heading to the emergency room, a costly and frequently unnecessary option that patients often used when they simply couldn’t reach the doctor’s office.
Angel also reviewed which rehab facilities helped patients most; he cut places with the worst results and sent many patients directly home, a recovery option that research suggests is often better, as well as less costly.
At the same time, Angel scheduled more regular follow-up visits with all his patients after surgery to head off potential complications.
“We feel like we have much more responsibility for the patient now,” he said.
Angel hasn’t always hit all his targets. But he cut the share of his knee replacement patients who ended up back in the hospital nearly in half between 2013 and 2015 and cut readmissions for hip replacement patients more than 80%.

Winnie Abbott sips water at El Acapulco in Cave City, Ark. Mexican food is a favorite of Abbott’s.
Abbott, who had her knee replaced in October, is almost fully recovered. “I can walk through Walmart now, and that’s pretty big,” she said. Before the surgery, she could barely get from her kitchen to her living room.
Abbott also had a smoother recovery than she did a decade earlier when she got a serious blood clot after having her right knee replaced. This time, with quicker follow-up from Angel, doctors were able to remove a stitch that got infected before she needed emergency care.
The broader payment reform effort is paying dividends for Arkansas, as well.
Between 2013 and 2014, Medicaid costs actually declined for patients in primary clinics participating in the initiative, according to a state analysis. That saved money and led to bonus payments for 19 physicians’ offices around the state.
Doctors also cut use of unnecessary tests and antibiotics after tonsil surgery. And hospitals slashed the share of patients being readmitted for complications after congestive heart failure from 14% to 1%.
The record was more mixed for other specialists, such as orthopedic surgeons. But the model is expanding with more insurers joining the program, and state leaders looking to bring in more physicians.
The federal Medicare program, meanwhile, is now implementing a similar payment initiative for hip and knee replacements around the country. And other states are making plans to follow Arkansas’ lead.
In Batesville, Angel concedes that adapting to the new system hasn’t been easy. But, he said, he has no regrets.
“When you see how much better this is … how much happier patients are, you don’t mind the hard work.”
Follow @noamlevey on Twitter
ALSO
What makes a community healthy?
Las Vegas tries new tactic to improve city’s notorious healthcare
Trump promised a ‘beautiful’ healthcare plan, but it’s pretty basic
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.