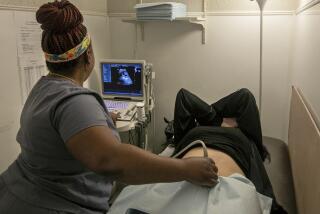
Study calls DNA test reliable in discovering fetal disorders

- Share via
It’s billed as a faster, safer and more accurate way of screening expectant mothers for fetal abnormalities like Down syndrome, and proponents say it has already become the standard for prenatal care.
But as a handful of California companies market their DNA-testing services to a growing number of pregnant women, some experts complain that the tests have not been proven effective in the kind of rigorous clinical trials that are required of new drugs.
Now, a study published Wednesday by the prestigious New England Journal of Medicine has verified that one of the tests can identify likely cases of Down syndrome and other genetic disorders caused by extra chromosomes in low-risk women with greater reliability than traditional noninvasive screening methods.
The genetic test, marketed by the San Diego DNA-sequencing firm Illumina Inc., did a better job of identifying cases of so-called trisomy disorders than did tests based on ultrasound exams and simple blood draws, said Dr. Diana Bianchi, the study leader and executive director of the Mother Infant Research Institute at Tufts Medical Center in Boston. The genetic test also had a much lower rate of false positives, she found. The research was funded by Illumina.
Fetal DNA makes up about 10% to 20% of the total DNA circulating in a pregnant woman’s bloodstream. These short segments come from the placenta and can be analyzed using massively parallel sequencing technology.
Down syndrome and other types of trisomies occur when a fetus has three copies of a chromosome instead of the usual two. The Illumina test, called verifi counts the DNA fragments that are most commonly associated with these disorders. If there are more than would be expected in a normal blood sample, the mother is warned of a potential problem and given the option of having a conclusive diagnostic test, such as amniocentesis or chorionic villus sampling.
During amniocentesis, a doctor uses an ultrasound scanner to guide a hypodermic needle into a pregnant woman’s uterus and then draws a small quantity of amniotic fluid, the liquid that surrounds and helps protect the fetus. In chorionic villus sampling, or CVS, ultrasound is also used to guide either a catheter or a needle into the placenta, where a small sample of tissue is removed. Both amniocentesis and CVS carry a 1% risk of causing a miscarriage.
A more accurate screening method with fewer false positives means that fewer women are exposed to an invasive procedure and the worry that accompanies it.
“The current testing scares the wits out of a very large number of women, relatively speaking, who when they go through further testing are found to have totally normal fetuses,” said Dr. Michael Greene, chief of obstetrics at Massachusetts General Hospital, who wasn’t involved in the study. “With this new test, the number of women who get inappropriately or improperly labeled as having an abnormal fetus is very small. So that’s a major advantage.”
The other DNA screening tests — made by Sequenom Inc. of San Diego, Ariosa Diagnostics Inc. of San Jose and Natera Inc. of San Carlos — work with technology similar to that of the Illumina test.
The American Congress of Obstetricians and Gynecologists and other professional societies have approved these new-generation tests for women at a higher risk of giving birth to a child with Down syndrome, including those who are over the age of 35 or who have a family history of the condition.
However, the Congress of Obstetricians and Gynecologists and others say there isn’t enough evidence to endorse the tests as a screening tool for low-risk women.
Bianchi said the Illumina study sought to address this lack of research. She and her colleagues recruited 1,914 low-risk women in 21 U.S. cities with singleton pregnancies. Each woman got both kinds of screening tests.
The DNA test for Down syndrome had a false-positive rate of 0.3%, which was significantly lower than the 3.6% rate of the standard tests, according to the study. Among the 1,365 women who were tested in the first or second trimester, 51 got false-positive diagnoses with the traditional test, compared with four false-positives from the Illumina test. The results were similar for the 544 women tested during the third trimester.
Bianchi said she hoped the study results would put to rest concerns about the test’s efficacy. A pioneer in the effort to test fetal DNA in maternal blood, she is on Illumina’s advisory board.
Greene said he was pleased to see a company invest in research to back up its claims. Currently, the U.S. Food and Drug Administration does not compel firms to do so.
“Many of the other companies are selling their tests like hot cakes without really demonstrating efficacy in a population like this,” he said.
Dr. Nancy Rose, chairwoman of the College of Obstetricians and Gynecologists’ genetics committee, called the study encouraging but said it involved a very small sample of women. Much more research would be necessary to justify any change in screening recommendations for low-risk women, she said.
“This is a first, very small report,” she said. “It’s encouraging, but that’s what it is.”
In an ideal world, the clinical trials would be conducted by independent organizations instead of the companies that have a huge stake in seeing their tests succeed, Rose said. But, she added, the reality is that there is little funding for such work.