Hospitals must work together to prevent superbug spread, CDC says
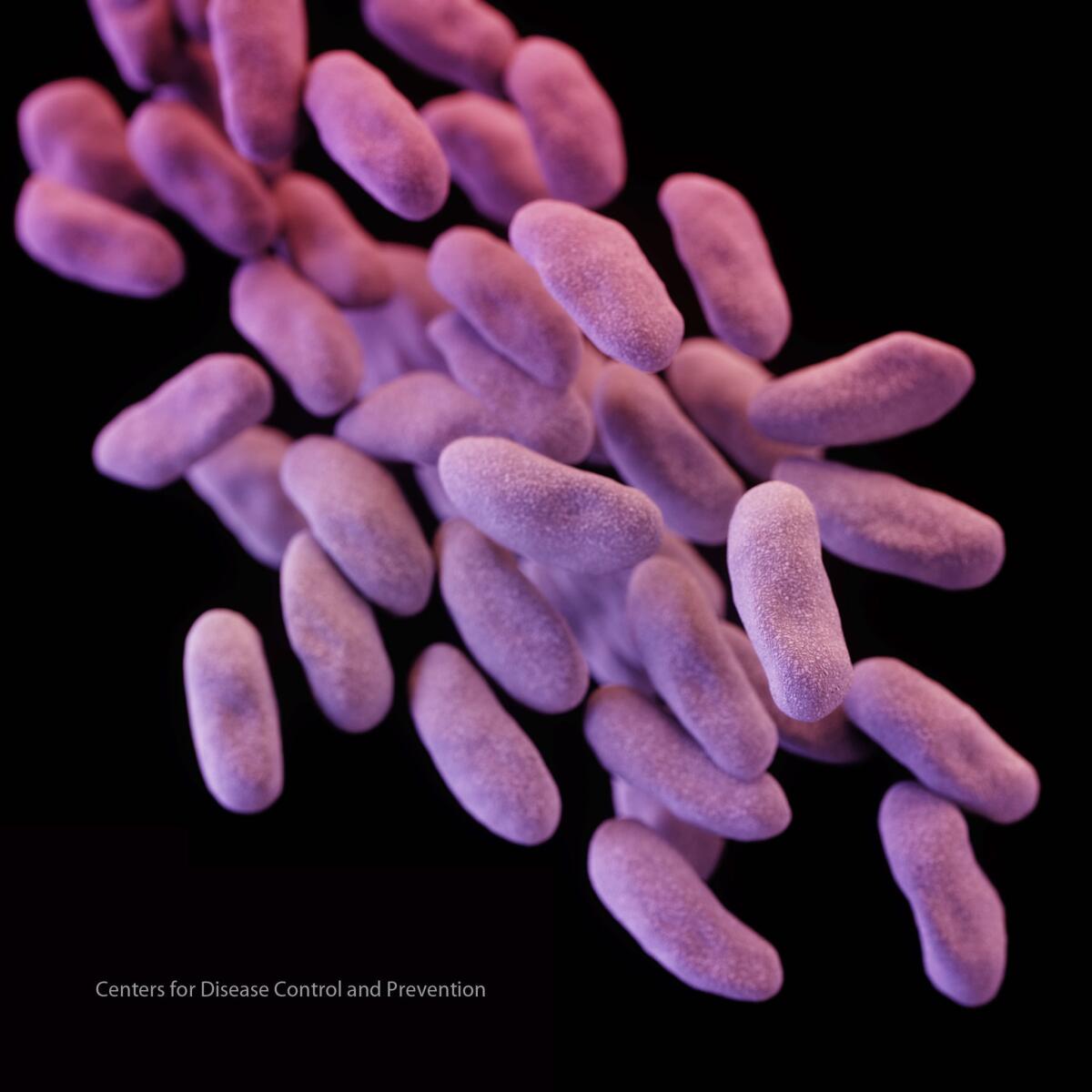
A new analysis from the U.S. Centers for Disease Control and Prevention estimates that better nationwide infection control and antibiotic stewardship could prevent 619,000 healthcare-associated infections with antibiotic resistant superbugs such as Carbapenem-resistant Enterobacteriaceae (CRE), pictured here.
- Share via
Superbugs -- germs that have evolved to become resistant to antibiotics and other medical treatments -- are on the loose, infecting more than 2 million people in the U.S. every year and killing at least 23,000.
But a new analysis from the U.S. Centers for Disease Control and Prevention suggests that coordinated efforts to combat antibiotic-resistant infections could reduce the number of infections in healthcare facilities by more than half a million over the course of five years.
“If you’re a hospital doing a great job but the hospital down the street isn’t, your patients are at risk,” said CDC director Dr. Tom Frieden, during a phone call with reporters Tuesday afternoon. “Facilities that go it alone can’t protect their own patients.”
Combating deadly antibiotic-resistant infections, which spread easily through and between healthcare facilities and are increasingly difficult to treat, has been a major push for the public health agency.
Frieden has been warning of the dangers of careless antibiotic prescribing practices and unsafe infection control for years; in March, President Obama also issued a five-prong plan for combating superbugs. Angelenos were reminded of the urgency of the situation in February, when there was an outbreak of carbapenem-resistant Enterobacteriaceae, or CRE, associated with contaminated duodenoscopes at Ronald Reagan UCLA Medical Center.
The CDC’S new analysis, a mathematical simulation, was released Tuesday as a CDC Vital Signs report and in the agency’s Morbidity and Mortality Weekly Report. Researchers looked at four types of healthcare-associated infections: CRE, multidrug-resistant Psuedomonas aeruginosa, invasive methicillin-resistant Staphylococcus aureus (MRSA), and C. difficile.
In 2011, they wrote, there were an estimated 310,000 infections caused by these bugs. Without increased interventions, cases would be expected to climb 10% over five years to around 340,000 per year. But with immediate implementation of nationwide interventions, medical facilities could prevent 619,000 infections over the five-year period, the team calculated, and might save more than 37,000 lives (as well as an estimated $7.7 billion in direct medical costs.)
The researchers also examined how coordination of infection-control efforts between healthcare facilities affected outcomes during a simulated introduction of CRE in networks of healthcare facilities. In a small network of 10 facilities with no augmented intervention, they found that CRE spread to 12.2% of patients after five years; if facilities made efforts on their own, the cases fell somewhat, to 8.6%.
But when facilities coordinated extensively, communicating when patients transferring between facilities had CRE infections and putting in place infection controls to prevent its spread, prevalence was reduced to only 2.1% after five years, the team wrote. A second simulation, in a larger network modeled after healthcare facilities in Orange County, generated similar results.
The coauthors said such coordination could be implemented in a variety of ways, but called on state and local health departments to facilitate coordination between healthcare facilities, writing that they were uniquely suited to lead the approach.
Frieden urged Congress to fully fund CDC programs to combat antibiotic resistance.
“Now it’s up to Congress to support it,” he said Tuesday. “We really are limited by lack of resources to roll this out rapidly.”
For more on science and health, follow me on Twitter: @LATerynbrown
ALSO:
Superbug outbreaks: FDA issues more scope-cleaning guidance to hospitals
Obama to drug-resistant superbugs: We are coming after you
Serious infections tied to medical scopes go far beyond issues with a single device







