Screening mammograms don’t prevent breast cancer deaths, study finds
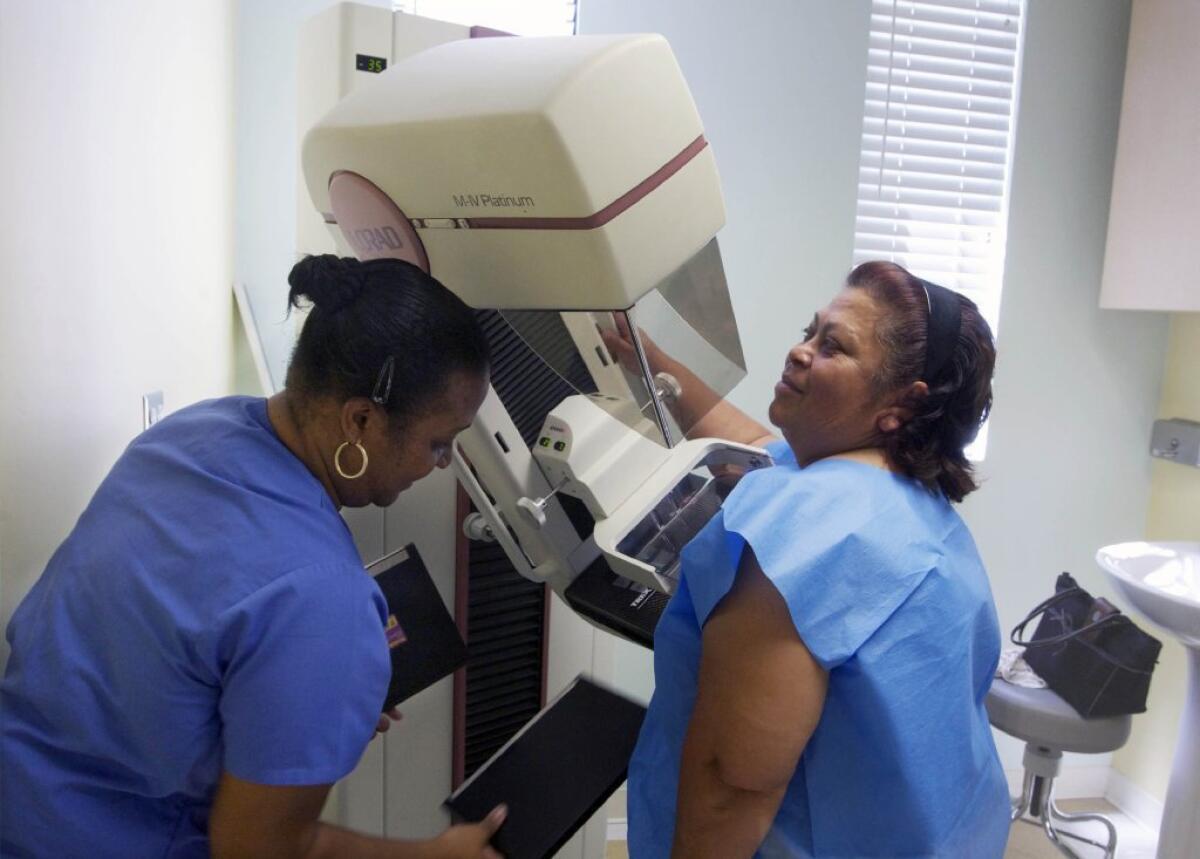
A new study casts fresh doubt on the value of screening mammograms. Counties where the tests were more common had more cases of small breast cancers but not fewer deaths from the disease, researchers found.
- Share via
The increased use of mammograms to screen for breast cancer has subjected more women to invasive medical treatments but has not saved lives, a new study says.
After reviewing cancer registry records from 547 counties across the United States, researchers concluded that the screening tests aren’t working as hoped. Instead of preventing deaths by uncovering breast tumors at an early, more curable stage, screening mammograms have mainly found small tumors that would have been harmless if left alone.
“The clearest result of mammography screening is the diagnosis of additional small cancers,” researchers reported Monday in the journal JAMA Internal Medicine. “These findings suggest widespread overdiagnosis.”
The researchers, from Harvard and Dartmouth, examined data from the National Cancer Institute’s Surveillance, Epidemiology, and End Results registry. Counties were included in the study if they reported the percentage of women ages 40 and above who had a screening mammogram between 1998 and 2000.
Among the more than 16 million women who lived in these counties, 53,207 were diagnosed with breast cancer in 2000 and then tracked for the next 10 years. During that time, about 15% of them died of breast cancer and an additional 20% died of other causes.
The researchers found that the extent of screening in the 547 counties ranged from 39% to 78%. Ideally, the counties with more widespread screening would see a payoff in the form of lower rates of breast cancer deaths.
Instead, the researchers found “no evident correlation between the extent of screening and 10-year breast cancer mortality,” they wrote.
For every 10-percentage-point increase in screening rates, the incidence of breast cancer rose by 16%, according to the study. That worked out to an extra 35 to 49 breast cancer cases for every 100,000 women.
Most of those tumors were considered small, measuring less than 2 centimeters across. But there was no corresponding decrease in larger tumors the result that would have been expected if mammograms were catching cancers before they grew to a more threatening size.
The researchers also examined breast cancers according to their stage at diagnosis, a marker of a tumor’s aggressiveness. More screening was associated with a higher incidence of early-stage breast cancers but no change for later-stage tumors, according to the study.
How can this be?
“The simplest explanation is widespread overdiagnosis, which increases the incidence of small cancers without changing mortality,” the study authors wrote. “Even where there are 1.8 times as many cancers being diagnosed, mortality is the same.”
The study did not consider cases where mammograms were used to find breast cancers in women who had symptoms of the disease, such as a suspicious lump.
The results are sure to be troubling to those who have faith in the idea that if mammograms are good, more mammograms must be better. If that were the case, the researchers should have found lower breast cancer mortality rates in counties where screening was more widespread, according to a commentary that accompanied the study.
Critics are sure to point out that the researchers can’t tell whether the women who got screening mammograms were the ones diagnosed with the extra cases of small breast cancers, the commentary authors wrote. The study design also leaves open the possibility that a higher incidence of small breast cancers in some counties prompted more women there to get screened, instead of the reverse.
The researchers agreed that people should “be wary” of studies like theirs that examine populations instead of individuals. “However, decisions must be made based on the evidence that is available,” they wrote, and “overdiagnosis is currently not observable in individuals, only in populations.”
The commentary authors, from the University of Washington and the Fred Hutchinson Cancer Research Center in Seattle, also noted that this type of study helped link smoking to lung cancer and Pap tests to reduced rates of cervical cancer.
The new study adds to earlier evidence that overdiagnosis is a real problem with screening mammography, though the magnitude of that problem remains unclear. Some studies have estimated that more than half of breast cancers diagnosed as a result of screening mammograms are overdiagnosed, while others put the figure below 10%, according to the commentary.
“Sadly, we are left in a conundrum,” the commentary authors wrote. “Women will increasingly approach their physicians with questions and concerns about overdiagnosis, and we have no clear answers to provide.”
Despite this uncertainty, the study authors endorsed mammograms as a valuable tool to screen women for breast cancer.
“We do not believe that the right rate of screening mammography is zero,” they wrote.
For more medical news, follow me on Twitter @LATkarenkaplan and “like” Los Angeles Times Science & Health on Facebook.







