Most uses of medical marijuana wouldn’t pass FDA review, study finds
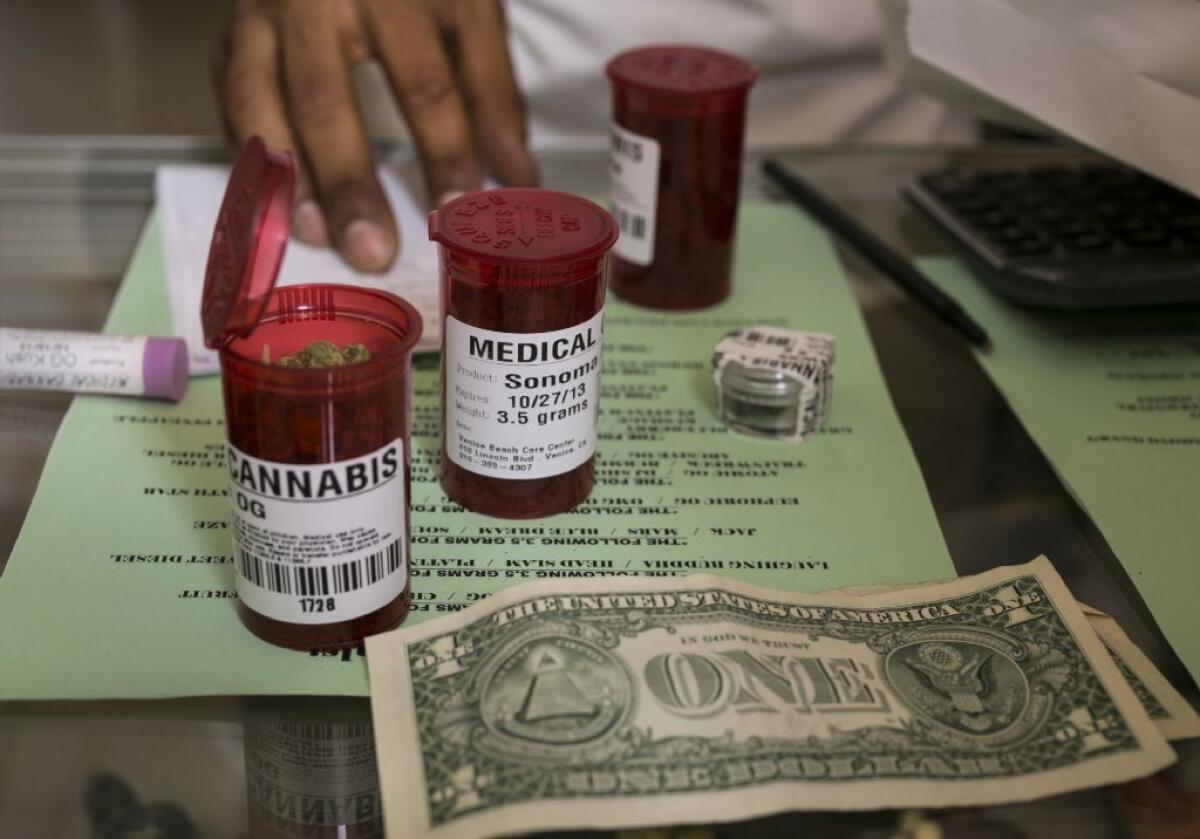
A new study finds that most of the conditions for which Americans use medical marijuana are not supported by solid clinical evidence.
- Share via
If medical marijuana were a regular drug, it would need the blessing of the Food and Drug Administration before it could be prescribed to patients. And in most cases, those patients would be out of luck.
A comprehensive review of dozens of clinical trials that have tested medical marijuana for 10 conditions finds that there’s very little reliable evidence to support the drug’s use. The review, by an international team of researchers, was published Tuesday in the Journal of the American Medical Assn.
Patients who use medical marijuana to treat chronic neuropathic pain or cancer pain would probably have the least to fear from an FDA review. The JAMA study considered 28 studies involving 2,454 patients and concluded that there was “moderate-quality evidence” from at least a dozen studies showing that cannabinoids – chemicals in marijuana that produce pharmacologic effects inside the body – reduced pain in such patients by modest amounts.
However, trials testing the pain-relieving effects of medical marijuana in people with fibromyalgia, HIV-associated sensory neuropathy, rheumatoid arthritis, multiple sclerosis and other conditions did not show that it worked.
The other condition for which medical marijuana proved useful was muscle spasticity in people with multiple sclerosis. After assessing 14 studies with 2,280 patients, the JAMA authors determined there was “moderate-quality evidence” to support its use in these patients, although many of the studies reported improvements that weren’t quite big enough to qualify as statistically significant.
The findings were even weaker for other conditions.
The researchers found “low-quality evidence” that medical marijuana could relieve nausea and vomiting in patients undergoing chemotherapy, that it could stimulate appetite in people with HIV to help them gain weight, that it could help people with insomnia and other sleep disorders get more rest, and that it could reduce the severity of tics in people with Tourette syndrome.
The JAMA authors also examined studies of medical marijuana to treat depression, anxiety disorder and psychosis, and to reduce eye pressure in glaucoma patients. There was no reliable evidence that cannabis was useful in any of these cases.
One of the things the studies showed most clearly is that people who use medical marijuana had a “much greater risk” of side effects, including serious problems like kidney, liver and psychiatric disorders. The most common adverse effects included dizziness, confusion and disorientation, according to the JAMA report.
The results show that something is amiss in the 23 states (plus the District of Columbia) that allow the use of medical marijuana, according to the authors of an editorial that accompanies the JAMA review.
The authors, from the Yale University School of Medicine, lamented the fact that state approval of medical marijuana had been based on “low-quality scientific evidence, anecdotal reports, individual testimonials, legislative initiatives, and public opinion.”
“Imagine if other drugs were approved through a similar approach,” they wrote.
To win FDA approval, drug makers typically have to show that a medicine works in not one but two randomized clinical trials. But for most conditions that qualify for medical marijuana treatment, “the evidence fails to meet FDA standards,” according to the editorial.
“If the goal is to make marijuana available for medical purposes, then it is unclear why the approval process should be different from that used for other medications,” the Yale authors wrote.
But that may not be the goal. “If the states’ initiative to legalize medical marijuana is merely a veiled step toward allowing access to recreational marijuana, then the medical community should be left out of the process, and instead marijuana should be decriminalized.”
For more medical news, follow me on Twitter @LATkarenkaplan and “like” Los Angeles Times Science & Health on Facebook.







