What is herd immunity and why does it matter in the fight against coronavirus?

- Share via
Fewer tables in restaurants. Everyone wearing masks. Staggered start times at schools. The “new normal,” as outlined by California Gov. Gavin Newsom last week, will be a big change in the time of the coronavirus.
But the old concept of normal — sharing a drink in a crowded bar or standing shoulder to shoulder with fans at a packed sporting event — might not be back “until we have herd immunity,” the governor said.
How long until then? In short: It’s complicated.
Here’s what to know about herd immunity, our long-term goal in the fight against COVID-19.
What is herd immunity?
Herd immunity describes the condition of when almost everyone is protected from a virus because enough of the population is immune, said Dr. David Eisenman, director of UCLA’s Center for Public Health and Disasters.
Is a second wave of the coronavirus outbreak inevitable? Scientists say that depends on the nature of the virus itself as well as our own behavior.
Imagine an individual who has never come in contact with a particular virus and has never received a vaccine. If she lives in a population that has herd immunity, her chance of contracting the virus is still low because she is surrounded by people who are protected from it. Thus the virus’ chain of transmission is broken.
“The idea of herd immunity is you don’t have to immunize everybody,” said Eisenman, who is also a professor-in-residence of community health sciences at the UCLA Fielding School of Public Health. “Those people who are not immunized gain protection just by the fact that they have less of a chance of coming into contact with it.”
Herd immunity is vital to protect those who are unable to be vaccinated, like the immunocompromised or those who are allergic.
How do we achieve herd immunity?
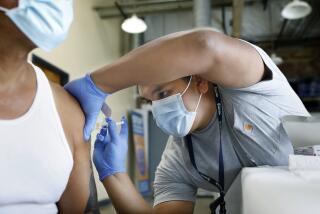
Individuals can gain immunity to a virus two ways: by contracting the virus and recovering, developing effective antibodies in the process, or by getting a vaccine.
The benchmark for herd immunity changes for different viruses based on their contagiousness, which is measured by a value called R0, pronounced “r-naught,” that indicates the average number of additional individuals who will get the virus from one infected patient. The World Health Organization estimated the novel coronavirus’ R0 to be between 2 and 2.5, based on initial data from China.
John Hopkins University’s Bloomberg School of Public Health predicts that we will need to reach at least 70% immunity to achieve herd immunity for the novel coronavirus, based on early estimates of the virus’ contagiousness.
A vaccine is a long way off. Can we develop herd immunity without it?
Probably not, Eisenman said. And if we did, it would involve a lot of suffering.
“It would mean that a lot of people have gotten infected and sick, and if that were to happen over a short period of time, that would be devastating,” Eisenman said. “It would mean we couldn’t reopen our economy. It’s just not really feasible to get it if we want to protect ourselves.”
To achieve the 70% herd immunity estimate without a vaccine in California, which has a population of nearly 40 million, almost 28 million people would need to contract the virus.
What do scientists wish they knew about the coronavirus? Which treatments actually work, what antibodies are good for, and which public health measures help.
What about the studies showing evidence that the coronavirus is more widespread than previously thought?
Recent studies from Stanford and USC have revealed a higher prevalence of the coronavirus than previously believed among residents in Santa Clara and Los Angeles counties, respectively. While the studies, which are based on detecting antibodies that indicate prior immune response, are valuable in discerning information about the virus, it is too early to jump to conclusions about reaching herd immunity, experts say.
“Those studies that are being done are not being done because the hypothesis is there’s herd immunity [in Northern California],” Eisenman said. “They’re doing those studies to find out what the infection rate is up there. ... They’re not operating under the hypothesis that there’s herd immunity; it’s just been expanded like that’s their primary hypothesis.”
Research from Stanford, published last week, estimated that between 2.5% and 4.2% of Santa Clara County residents had antibodies to the coronavirus in their blood by early April. The numbers estimated that between 48,000 and 81,000 people in the county had contracted the virus compared to the roughly 1,000 reported cases at that time.
Similarly, a study published by USC on Monday found that 2.8% to 5.6% of L.A. County adults have antibodies to the virus in their blood, translating to roughly 221,000 to 442,000 adults who had recovered from the infection by early April. L.A. County reported fewer than 8,000 cases by that time.
Both studies show that the virus’ reach was larger than previously thought, when diagnostic testing was limited to just patients with symptoms. But even the highest estimate of 5.6% is far from the herd immunity benchmark of close to 70%.