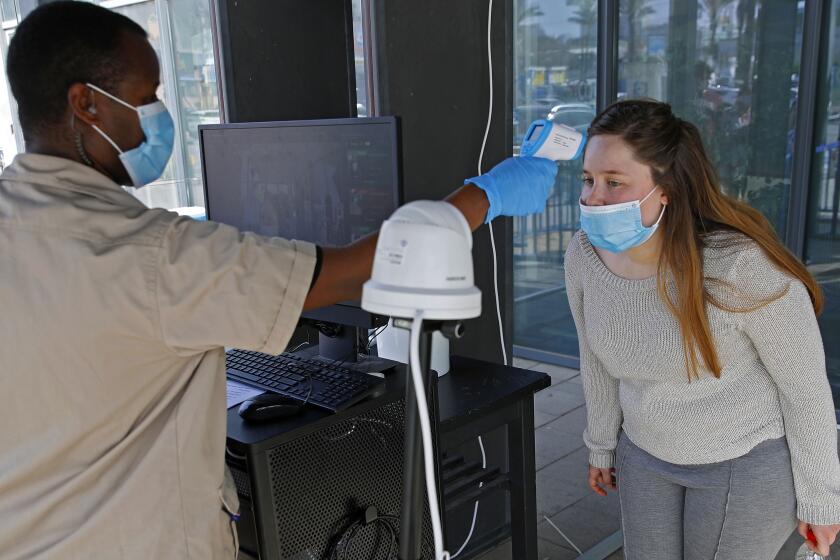
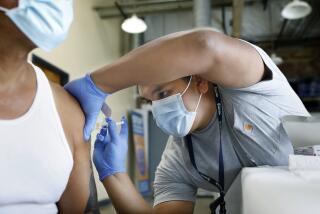
As the economy reopens, scientists still have a lot to learn about coronavirus immunity
- Share via
Who among us is immune to the coronavirus?
Six months and close to 7.5 million infections into the COVID-19 pandemic, scientists are just now inching their way toward answering that question.
For those who have weathered a bout with the virus, there are promising signs that protection follows.
But understanding the extent of true immunity is an exercise in humility, scientists caution. And the stakes couldn’t be higher: Public health efforts to defeat coronavirus — from antibody testing and “immune passports” to the use of convalescent plasma and the design of a new vaccine — depend on understanding who is immune, and why.
Dr. Anthony Fauci, the nation’s leading expert on infectious diseases, called the emerging evidence on coronavirus immunity “confusing,” “perplexing,” and a “a bit unusual.”
“Here’s the deal,” Fauci said in a recent interview. “One can say that if you have recovered from infection, it is highly likely you’ll be protected from reinfection for a finite period of time, varying from person to person because of biological variability. We don’t know how long that finite period will be. It could be years, or a year.”
Two studies published this week offered support for the hope that some people have, indeed, earned immunity to coronavirus, and that it can be roughly measured. But as the economy reopens, the same findings should temper the expectations of political leaders who are counting on armies of the recovered to lead a charge back to normalcy.
The new studies shed light on how many patients emerge from coronavirus infection with so-called neutralizing antibodies — the kind that can, in theory and for an unknown stretch of time, protect a person from re-infection.
Israeli scientists say they can mimic the effects of a vaccination campaign if certain people willingly get infected with the coronavirus and recover.
A new census of 382 sailors aboard the USS Theodore Roosevelt has found that at least 60% of those who were infected developed antibodies capable of protecting them to at least some extent. And in a very small group of study participants infected early, some still had the virus-blocking proteins in their blood 40 days after their symptoms had first appeared.
That’s a reassuring sign on two fronts. It shows that even young and otherwise healthy people, who tend to have mild or even no symptoms when infected with coronavirus, are making antibodies that could protect them from re-infection.
And it suggests that for some, that protection might have staying power.
These servicemen and women, caught up in a ship-wide outbreak, have given scientists a valuable glimpse of the coronavirus at work in a young, healthy population that lives and works closely together. Between mid-January, when the aircraft carrier set out from its San Diego home port, and late March, when it pulled into Guam for an emergency medical stop, roughly 1,000 of 4,800 aboard had been infected by coronavirus.
The early look at the sailors’ immune response was performed by a team from the Centers for Disease Control and Prevention and the U.S. Navy.
A second study out this week has found that between 83% and 93% of New Yorkers who had recovered from confirmed coronavirus infections and been well for at least two weeks had at least some neutralizing antibodies in their blood.
But the capacity of those antibodies to neutralize the coronavirus varied quite widely. In a little over half of the 370 recovered patients — between 52% and 56% — researchers found “relatively modest” antibody levels.
There was better news, and surprising news too. Roughly one in 10 of the recovered blood donors was found to have highly potent concentrations of infection-blocking antibodies. And the blood of recovered men had two to three times the coronavirus-neutralizing activity as samples from recovered women.
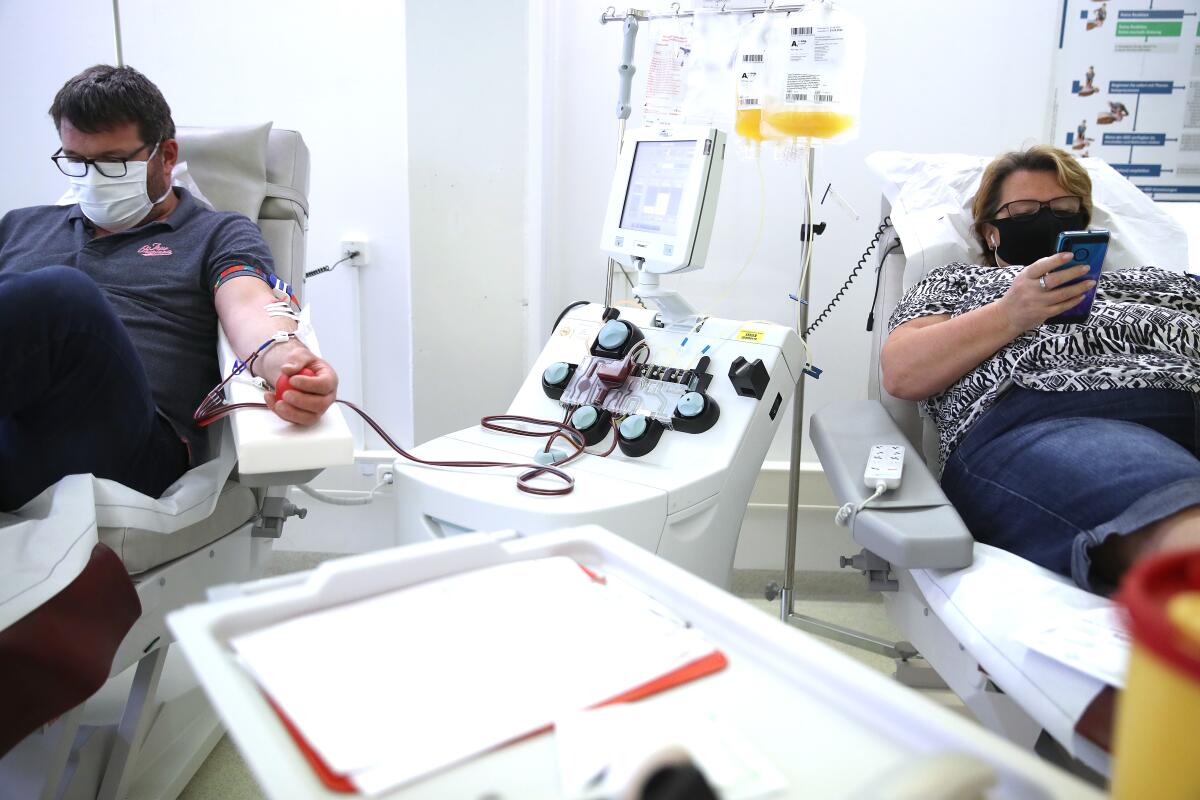
The findings suggest that this minority of recovered patients is very likely to enjoy some protection from reinfection themselves. It also bodes well for hopes that infusions of their blood plasma can protect others from infection, and reduce the risk of critical illness or death in people who are already sick.
Scientists racing to stave off a tidal wave of coronavirus infections show renewed interest in a little-known medicine: convalescent plasma.
The study also raised hopes that two newly fielded blood tests will not just provide a yes-or-no judgment on past infection, but a gauge of a recovered individual’s immunity as well. Researchers found that readings provided by the Vitros immunoassay from Ortho-Clinical Diagnostics aligned closely with lab-based tests measuring a sample’s virus-fighting properties. Abbott Labs’ Architect immunoassay provided a less precise reading of neutralizing antibody activity in each sample, they found.
The study was posted on Wednesday to the website MedRxiv, where preliminary scientific findings are widely shared for comment.
Both new reports confirm and amplify research released in late April by doctors in Shanghai. They found that in 175 people who had been only mildly ill with COVID-19 coronavirus, a little over half produced relatively high levels of neutralizing antibodies, while 30% made very low levels that scientists fear may not be helpful.
But these studies have left scientists with some maddening uncertainties. When it comes to coronavirus antibodies, does quantity or quality matter more? Could a recovered patient be immune even without neutralizing antibodies? Do coronavirus patients who were very sick, or sick for a long time, have stronger immunity than young and healthy patients who had milder symptoms, or none at all?
The human body produces many different kinds of antibodies in response to infection, and the neutralizing variety may not be the only ones that hobble a virus. The immune system has other defensive weapons to muster for such a fight, including its killer T cells and B cells. Their powers against this coronavirus are not well understood — and even if they were, the antibody tests now being fielded aren’t designed to measure them, or other immune factors.
Some of these overlooked antibodies may lie dormant, awakening only when challenged by the virus’ return, said Dr. Jeffrey Henderson, an infectious diseases specialist at Washington University in St. Louis. The body’s cellular immune response may have done such a good job that the humoral immune system that forges antibodies never even came into play, he said.
With coronavirus, he added, “we’re keeping an open mind.”
The same openness extends to other long-held assumptions. Scientists have always observed that sicker patients make more and better antibodies. But that assumption may be upended by this coronavirus, said Larry L. Luchsinger, a stem cell researcher at the New York Blood Bank who spearheaded the study of recovered blood donors there.
Now Luchsinger and his team hope to go back to the 370 blood donors to learn more about their reported symptoms to test the proposition.
They may find that there’s no pattern at all: Young people who scarcely noticed their infections may be just as immune as older patients who barely escaped with their lives. Or perhaps neither is immune. Or maybe one gained three months of immunity while the other got three years.
And that’s still only part of the story, Luchsinger said.
“The big underlying question is, how much neutralizing activity you even need?” he said. “This is the way immunology works. We are humbled.”