British scientists find changes in coronavirus that may make it more infectious

- Share via
In the United Kingdom and several other countries, a disconcerting cluster of genetic changes has been detected in the coronavirus that causes COVID-19, prompting British Prime Minister Boris Johnson to all but cancel Christmas in Britain.
At least 1,619 samples of the virus collected from infected Britons contained a distinctive set of 17 genetic alterations, including three that appear to make the virus easier to transmit from person to person and improve its ability to sneak past the immune system’s defenses.
The changes in the coronavirus’s RNA were detailed in a report by British researchers who use time-stamped genetic sequences of the virus to track the pandemic’s progress. The COVID-19 Genomics UK Consortium said the “unexpectedly large” number of changes, and their potential influence on key parts of the virus, require “urgent laboratory characterisation and enhanced genomic surveillance worldwide.”
The same collection of RNA alterations has been detected in viral samples culled from four other countries, the British geneticists added.
Several of the changes appear to alter the virus’ spike protein, which the coronavirus uses to pick the lock to human cells and convert them into factories for its own production. Two of the changes appear to make cells in the respiratory tract and elsewhere more vulnerable to invasion, and they increased the virus’ infectivity and its virulence in mice.
While both mutations have been seen separately, they’ve only been seen together in the new clutch of cases, the British researchers said.
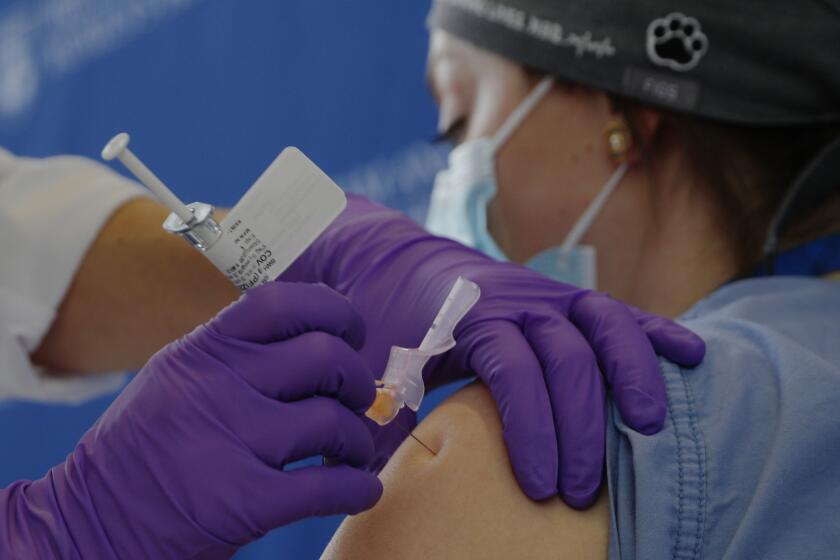
That’s a potential problem because all five of the COVID-19 vaccines furthest along in development train the immune system to target the spike protein. In theory, these genetic changes might alter the protein enough to erode the effectiveness of vaccines made by Pfizer and Moderna — both of which are being rolled out in the U.S. — as well as three others close behind them.
In a report last week, the British researchers wrote that “there is currently no evidence that this variant (or any other studied to date) has any impact on disease severity, or that it will render vaccines less effective, although both questions require further studies performed at pace.”
Over the weekend, a panel of vaccine experts pressed the U.S. Centers for Disease Control and Prevention on whether the British strain would alter the effectiveness of the Moderna vaccine that received emergency use authorization from the Food and Drug Administration on Friday. Officials assured committee members that Moderna and other vaccine makers will perform “deep sequencing” on these so-called “breakthrough cases” to detect whether such changes have occurred.
If the COVID-19 vaccine from Pfizer and BioNTech was good enough to get a nod from the FDA, the vaccine from Moderna and the NIH almost certainly is as well.
The developments caused Johnson to renew lockdown measures across much of England, including travel restrictions and the shuttering of pubs, gyms, theaters and hair salons. He said the moves were taken in response to findings that the RNA changes could make the virus “up to 70% more transmissible.”
“This is spreading very fast,” the prime minister said.
By Sunday, France, Germany, Italy, the Netherlands, Belgium, Austria, Ireland and Bulgaria all said they would ban incoming flights from the U.K.
Samples of the SARS-CoV-2 virus that include some or all of 17 changes were first detected in samples from two Britons on Sept. 20. One was collected from a person in Kent in southeastern England, and the other came from a person in the London metropolitan area the next day.
By Friday, viral samples with roughly the same genetic fingerprint represented 6% of all viral samples sequenced in the United Kingdom since Nov. 1. (Researchers at the U.K. genetics consortium sequence roughly 10% of viral samples from all Britons who test positive for coronavirus infections.)
Emma Hodcroft, a geneticist working with a viral tracking group called Nextstrain, said the family of changes has also been detected in samples in Denmark and Australia, which were probably imported from Britain. Belgium and Italy are also following up on reports that the mutation has been detected within their borders.
Researchers in South Africa also have detected infections that bear some of the same changes, including ones in the virus’ spike protein.
Those who have followed the virus’ genetic journey during the pandemic were quick to note that not all alterations should set off alarm bells. As with any family tree, the virus spins off distinct lineages as it spreads across time and space, and each one is thought to pick up one or two changes a month.
As a result, the coronavirus has incorporated thousands of modifications since it emerged late last year.
Today, when a deadly virus explodes out of nowhere, geneticists are indispensable players in the international game of whodunit. Here’s how they help.
While such incremental changes can gradually shift a virus’ behavior over time, none has yet been seen to suddenly make this coronavirus more dangerous to those it infects or to boost its ability to jump from person to person.
But this case may be different, the British researchers warned.
The abrupt appearance of so many samples with so many of the same potentially significant changes “is, to date, unprecedented in the global virus genomic data for the COVID-19 pandemic,” they wrote.
While scientists have been aware of some of these genetic variants since September, they’ve circulated far more widely in recent weeks. The researchers hypothesized that the cluster of changes may have been prompted by the virus’ efforts to overcome the suppressive effects of antiviral drugs or antibody-rich blood plasma donated by people who have recovered from COVID-19.
The researchers noted that alterations tend to accumulate very quickly in people who take months to clear a viral infection, as well as in people with weakened immune systems. As their infections linger, those people become incubators for multiple versions of the virus that sicken them simultaneously, allowing them to swap and share their genetic variants.
Other scientists who have tracked the pandemic’s twists and turns said it’s not entirely clear that the genetic changes — either singly or collectively — have made the virus more transmissible.
Americans waiting their turn for a COVID-19 vaccine may not be pleased to see who’s in line ahead of them. Does a prisoner or smoker deserve it more?
The early assessments of transmissibility appear to be inferred in part from the growth of samples collected around Kent and London. But Dr. Marc Suchard, a UCLA biomathematician, cautioned that population density, different rates of mask-wearing and social distancing, and other factors can influence how fast a particular virus spreads.
“One might say the evidence is suggestive of increased transmissibility,” Suchard said. But nailing that down will require a careful scrubbing of epidemiological data and laboratory testing, he said.
Along the way, he added, scientists may discover that as the virus becomes better at spreading, it could also become less dangerous — a tradeoff that has taken the bite out of other epidemics.
Dr. Arturo Casadevall, a Johns Hopkins University microbiologist, said that if the genetic changes will have any effect on COVID-19 vaccines, it will be minimal.
“I am not alarmist about this,” Casadevall said.
Even changes that significantly alter the virus’ spike protein don’t affect plenty of other targets, called epitopes, that antibodies use to recognize and kill virus, he said.
“So for the virus to completely defeat vaccine, it would have to change in many, many places where the virus binds to cells,” he said. “And that is a very low probability event.”
That view is shared by Trevor Bedford, a geneticist at the Fred Hutchinson Cancer Research Center who has tracked the coronavirus’ genetic meanderings.
“I’m not concerned that these variants will significantly reduce vaccine efficacy in the 2021 rollout,” Bedford said in a Twitter thread. “The strong immune response to the mRNA vaccines would suggest that a large antigenic change would be needed to significantly reduce efficacy.”