Modified COVID-19 vaccines may get nod from FDA without repeating full trials
- Share via
The U.S. Food and Drug Administration issued new guidance Monday that streamlines the vetting process for COVID-19 vaccines that are modified to target new coronavirus variants.
The recommendations, detailed in a 24-page document on the FDA’s website, are intended to speed up the review process amid worries that the new variants — some more contagious, some more able to evade current vaccines — will undermine efforts to halt the virus’ spread.
“We know the country is eager to return to a new normal and the emergence of the virus variants raises new concerns about the performance of these products,” Dr. Janet Woodcock, the FDA’s acting commissioner, said in a statement. “By issuing these guidances, we want the American public to know that we are using every tool in our toolbox to fight this pandemic, including pivoting as the virus adapts.”
The recent emergence of a spate of variants has led to rising concerns that the first generation of vaccines — which were developed based on an early version of the coronavirus — may not be well-equipped to protect people against the mix of viruses currently in circulation.
For example, several vaccines have been less effective in South Africa, where a strain known as B.1.135 dominates, than in other parts of the world where that variant is not as prevalent.
A vaccine from Johnson & Johnson’s Janssen Biotech unit reduced the risk of moderate to severe cases of COVID-19 by 72% when tested in the U.S., but was only 57% effective in South Africa. Similarly, a vaccine from Novavax that was nearly 90% effective at reducing the risk of all types of COVID-19 in Britain was only 49% effective in South Africa.
Also concerning: A COVID-19 vaccine developed by AstraZeneca and Oxford University was 75% effective at reducing the risk of mild to moderate illness when tested in South Africa before the B.1.351 strain was widespread. But after it took over, the vaccine was no better at preventing mild to moderate illness than a placebo.
And in laboratory tests, antibodies generated by people who had received a vaccine developed by Pfizer and BioNTech did a better job of thwarting a coronavirus variant from the United Kingdom than it did against the South Africa strain.
Researchers once believed t would take months or even years for the virus to develop resistance to vaccines. The speedy evolution is largely a result of the virus’ unchecked spread.
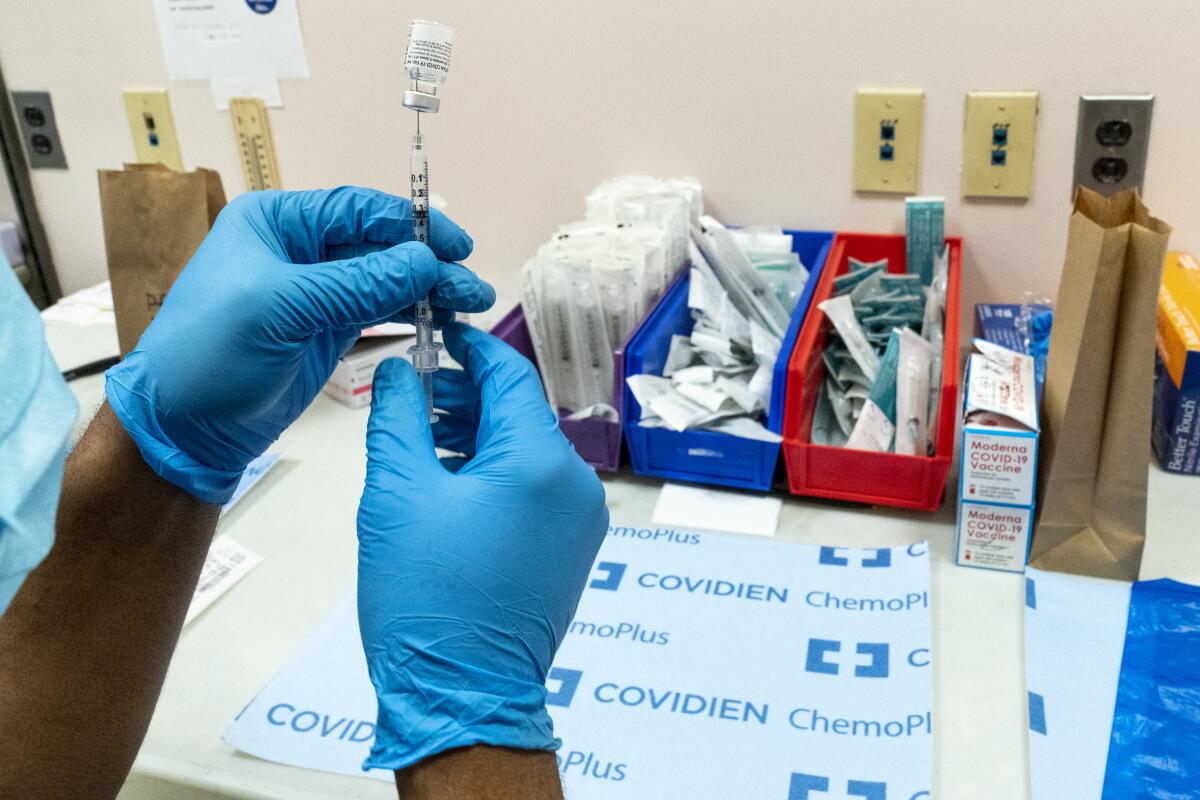
Vaccine makers have responded to the threat posed by new variants by adjusting their recipes so the immune system will better recognize them.
The new guidance is part of a flurry of recommendations for developers of vaccines, tests and therapeutics in light of these new variants. It allows modified vaccines to be authorized under an amendment to their existing emergency authorizations, officials said.
The FDA would like companies to submit clinical data showing that the modified version of their vaccine is more effective against new variants than their original vaccine. The agency is also asking vaccine makers to test their modified vaccines in people who have never been vaccinated and in people who were previously vaccinated.
Dr. Peter Marks, director of the FDA’s Center for Biologics Evaluation and Research, said trials to test the immune response prompted by a tweaked vaccine would probably involve a few hundred individuals, and might take about two or three months.
Compare that with a typical Phase 3 clinical trial, which can involve tens of thousands of patients and can take several months longer.
The emergence of new virus variants will complicate efforts to end the COVID-19 pandemic, scientists say. But they’re confident we’ll still get there.
Such a speedy vaccine alteration is the norm for viruses like influenza, said Dr. Diane E. Griffin, a viral immunologist at the Johns Hopkins Bloomberg School of Public Health.
It’s possible that in the future, modified vaccines could be authorized without the need for additional clinical studies, the FDA noted. But that is not yet the case.
The agency emphasized that the two vaccines currently authorized for use in the U.S. — the one made by Pfizer and BioNTech and another developed by Moderna and the National Institutes of Health — are still effective against the mix of variants now circulating in the U.S.
That said, “it’s reasonable to think these companies are thinking about these changes or are thinking they may need to make changes,” Griffin said. “This just helps them to know what kind of information the FDA would want and what they wouldn’t need.”