Actual safety vs. hygiene theater: What will really protect you from the Delta variant?
- Share via
A more transmissible coronavirus variant is spreading across the U.S., and it has led a range of authorities to give conflicting advice about the use of face masks and other protective measures.
Worries over the Delta variant have prompted the World Health Organization to stress the continued importance of wearing masks — even for people who are vaccinated.
“We still live in a world that is only partially vaccinated that has a lot of susceptibility, a lot of vulnerability,” Dr. Bruce Aylward, a senior advisor at the WHO, said at a briefing Friday. “So what we’re saying is, once you’ve been fully vaccinated, continue to play it safe because you could end up as part of a transmission chain.”
Meanwhile, officials at the U.S. Centers for Disease Control and Prevention have so far stuck with their current guidance, which allows fully vaccinated people to go about their lives without wearing masks or practicing physical distancing in most circumstances.
California lifted its mask rules for fully vaccinated people on June 15. But the Delta variant has given some officials pause. On Monday, the Los Angeles County Department of Public Health “strongly” recommended that all residents wears masks in public indoor spaces, regardless of their vaccination status.
“Until we better understand how and to who the Delta variant is spreading, everyone should focus on maximum protection with minimum interruption to routine as all businesses operate without other restrictions, like physical distancing and capacity limits,” officials explained.
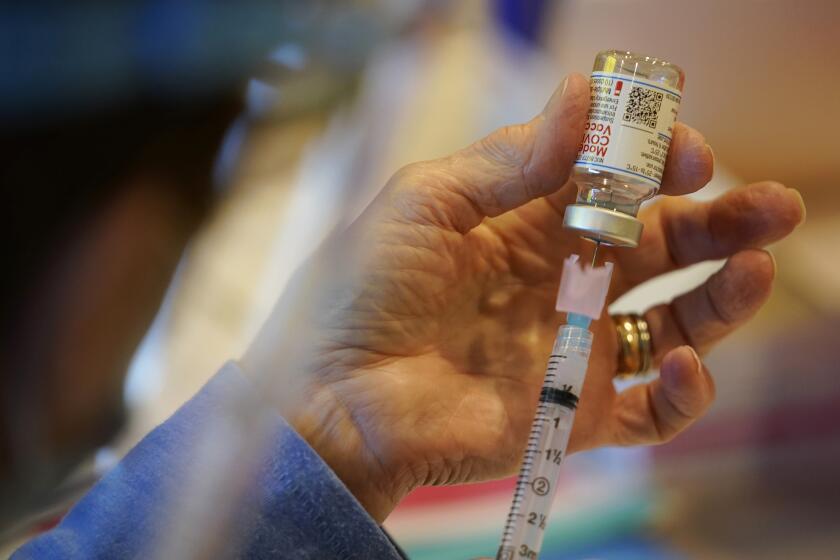
Lab tests and real-world experience offer reassuring evidence that COVID-19 vaccines offer a high level of protection against the Delta variant.
The Delta variant now accounts for about one in four coronavirus cases in the U.S., according to the CDC. In California, it made up 14.5% of the viral samples analyzed in June.
The Times spoke to three experts this week about what the Delta variant meant for COVID-19 safety precautions, which measures matter the most right now — and which don’t.
How worried should we be about the Delta variant in the U.S.?
Dr. Timothy Brewer, epidemiologist and infectious disease expert at UCLA: The difference between now and a week earlier is that everything had been getting better for several weeks now, moving in the right direction. There were pockets where things weren’t going quite as well as you wanted them to. But in the country as a whole — and in California in particular — everything was moving in the right direction, plus [the rate of positive tests] were down overall.
So this little uptick may be just the first sign that “Hey, we’re still not completely out of the woods yet.” We want to keep on top of this, not let it take off on us.
For every confirmed coronavirus infection in the U.S. during the spring and summer of 2020, 4.8 other cases went undetected, a new study finds.
With Delta on the rise, do you think the CDC’s recommendations makes sense?
Dr. Panagis Galiatsatos, pulmonary and critical care physician with Johns Hopkins School of Medicine: I think people are misunderstanding their purpose. They’re really meant for people who have achieved vaccination. For those who haven’t, there’s still a massive emphasis on them to continue wearing face masks and so forth.
There’s also an issue when you take these recommendations and make them universal, where a region with a vaccination rate of 20% gets to do the same things as a region with 70%.
If you’re in a region that has a high enough vaccination rate and life is good, no COVID cases, great. If you’re in a region with 20% vaccinated and still-high rates of COVID cases, you probably shouldn’t take your foot off the pedal. You should still enforce those infection control policies.
Plus, very few businesses seem to be checking the vaccination status of unmasked patrons.
Brewer: Right. That was actually my concern about going to this kind of approach when it was originally announced, because it really shouldn’t be up to businesses to decide and enforce public health practices.
Either the county or the state should be saying, “Look, we still need to wear masks indoors until our vaccination rates are high enough,” or “Look, we really think our vaccination rates are high enough that you don’t need to be wearing masks.” But to say, “If you’re not vaccinated, you should be wearing a mask, and if you are, you don’t have to,” I don’t think that’s particularly helpful.
What do you think about Los Angeles County urging residents to mask up indoors, regardless of whether they’ve had their shots?
Dr. Monica Gandhi, infectious disease expert at UC San Francisco: There’s research showing really quite high rates of immunity in Los Angeles, between vaccination and natural immunity from infection. So I was surprised by the Los Angeles Public Health Department saying that.
But it wasn’t a mandate, it was just a recommendation.
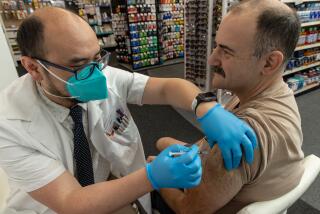
If scientists discover that immunity to the coronavirus starts to wane months or years after vaccination, a booster shot could be deployed.
How would you decide when new restrictions are warranted?
Galiatsatos: From my standpoint, I’d look to see if you have a population that has a high amount of COVID admissions into the hospital. That’s probably my favorite surrogate.
Keep in mind, if enough people are vaccinated, you may still have a lot of cases, but those cases are typically no more than just a bad cold. The vaccine worked. That’s why I’m saying your barometer has to be the hospitalizations, because that’s what the vaccines are intended to prevent.
If you have a lot of hospitalizations, to me that’s a surrogate to say there’s probably a low amount of vaccinated people. So if you’re seeing an uptick in your hospitalizations, put back those indoor policies for face masking, at a minimum.
What other restrictions should be reinstated?
Galiatsatos: My second request would be limiting how many people can be indoors. Because the more people you put indoors, the more likely one of those individuals is bringing in the coronavirus or bringing in one of the variants.
Physical distancing in itself sounds great on paper, but it is hard to implement in a public setting.
What about moving more indoor activities outdoors again?
Galiatsatos: We’re dealing with, you know, 110-degree weather outside. You don’t want to focus on one public health concern and turn a blind eye to another — where suddenly I’m not getting COVID cases anymore but I’m getting heatstroke cases over and over again.
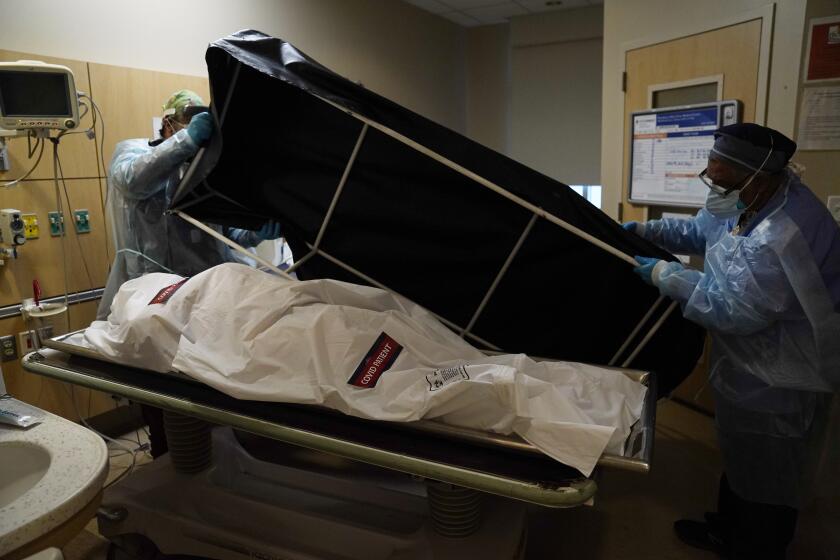
Two decades of progress in closing a yawning gap between the life expectancy of Black and white Americans has been erased by COVID-19.
Many businesses continue to be aggressive about disinfecting surfaces and other things that do little to stop coronavirus spread. Are there any examples of this so-called hygiene theater we should drop?
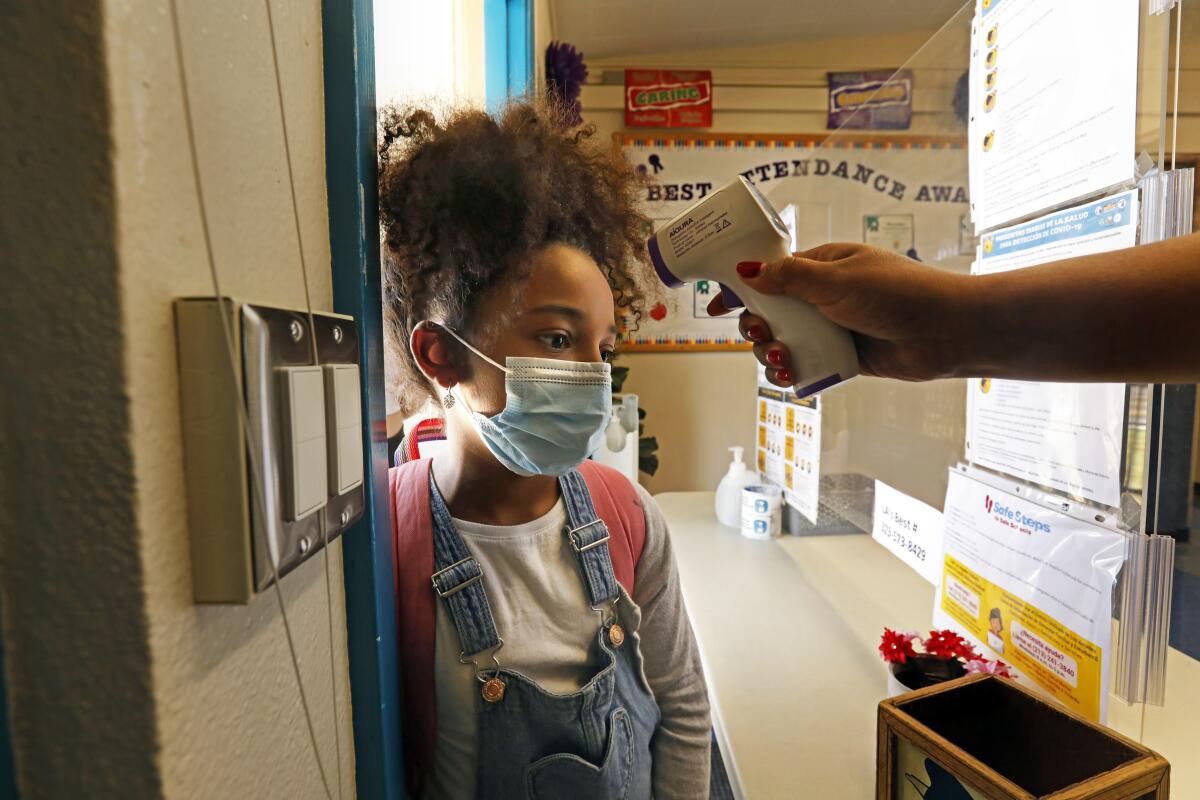
Galiatsatos: The temperature check is by far the bane of my existence. Temperature checks establish body temperature, not if you have a fever.
Let me give you an example: I drove my daughter to camp. She wanted the windows down, so it got very hot. Then she had a body temperature scan. Her body temperature was elevated, and they were like, “She has a fever.” I said,” No, she just has an elevated body temperature, because we’ve been sitting in a car that’s equilibrated with the outdoor weather.”
The whole concern about COVID has been its asymptomatic spread. Using temperature checks to prevent that is like trying to catch a golf ball using a volleyball net. You’re giving people a false sense of security.
These interviews have been edited for length and clarity.