- Share via
For Filipino Americans like Giancarlo Santos, holiday parties are typically a free-for-all of revelry, with friends and family spilling into every corner of the house, and Christmas decorations twinkling everywhere.
This year, Santos will get to enjoy the decorations as he receives treatment for an aggressive type of cancer called diffuse large B-cell lymphoma. But holiday celebrations at his home in Chino will be strictly limited to his wife, Michelle, and their three children, who will be wearing masks and maintaining a safe distance from their 46-year-old father.
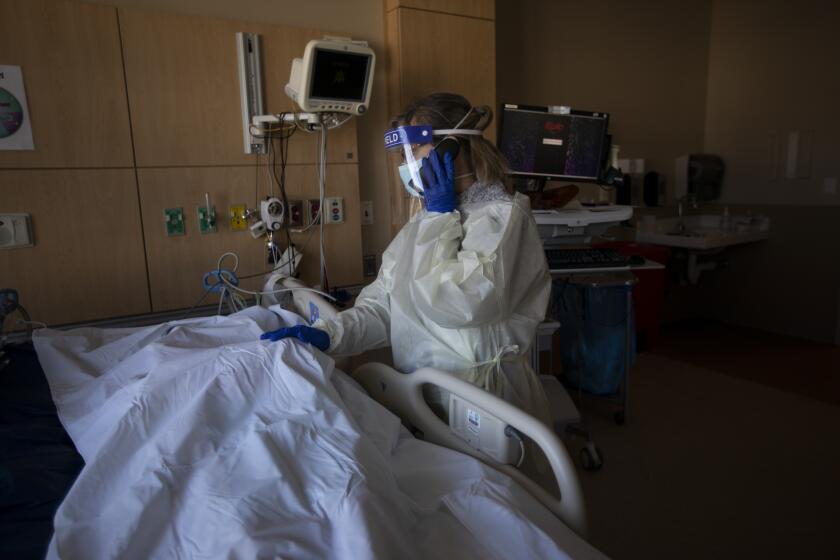
“I’m not normal; this is all abnormal,” Santos said from his hospital bed at Cedars-Sinai Medical Center in Los Angeles. His children “are ready for the pandemic to be over — hanging out with friends, going out, taking kickboxing classes,” he said. But they’ve met him halfway, getting vaccinated and wearing masks to protect their dad, whose disease has left his immune system unable to protect him from COVID-19’s deadliest ravages.
If only everyone in his life were willing to do the same.
The Path From Pandemic
This is the fourth in an occasional series of stories about the transition out of the COVID-19 pandemic and how life in the U.S. will be changed in its wake.
Almost three years into the pandemic, many Americans have decided that the health emergency is over. In late October, when the polling organization Morning Consult gauged Americans’ concern over COVID-19, only 11% said they considered it a “severe health risk” within their communities.
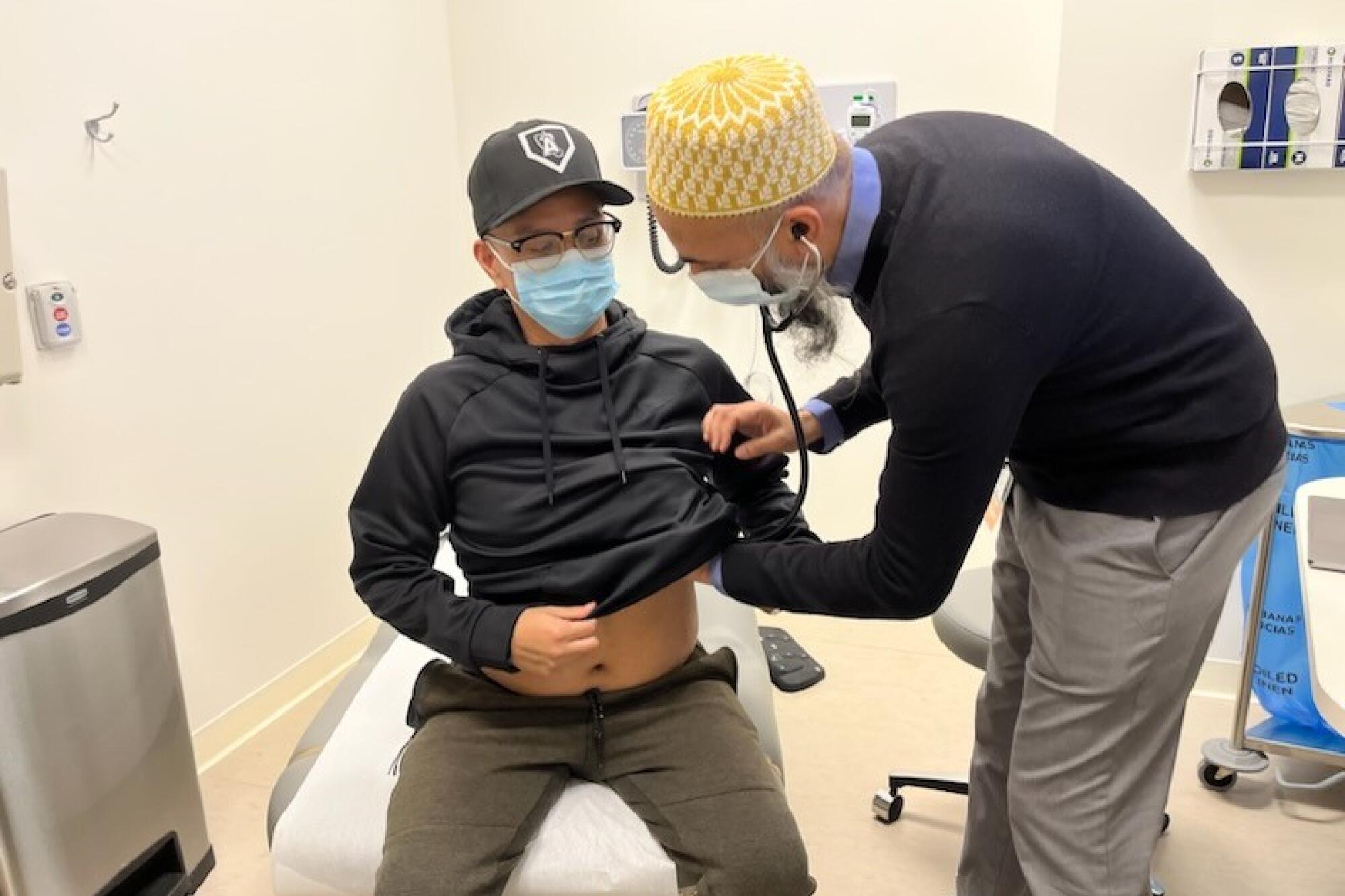
But for patients whose immunity is weakened or destroyed by medicines or disease, “it’s not over,” said Dr. Akil Merchant, an oncologist who oversees Santos’ care at Cedars-Sinai.
Indeed, for these Americans, the pandemic has taken a turn for the worse.
If the U.S. public health emergency ends, Americans would be vulnerable to a new coronavirus variant that sparks another COVID-19 surge.
The Omicron strain that is generally considered mild has dealt a significant blow to people with compromised immune systems. Two therapies that have been a mainstay of protection for these patients are no longer believed to be effective against two of the most dominant subvariants, BQ.1 and BQ.1.1 That leaves them with only two effective medications should they get sick.
That, in turn, puts them at the mercy of those around them as COVID-19 cases and deaths are ticking upward, mask use is falling, and updated booster shots are going unclaimed.
In a world that’s moved on from precautions, “they’re on their own,” said UCLA infectious disease specialist Dr. Otto Yang.
That’s not entirely new: Influenza and respiratory syncytial virus have long put these patients in peril as well, but Americans have never been asked to don masks or get vaccinated to help protect them against the viruses that cause those diseases.
Getting Americans to forfeit their perceived freedoms to protect the vulnerable has always been a big ask, said Johns Hopkins University bioethicist Jeffrey Kahn.
“We’re more oriented toward individual rights,” he said.
But even if there were broad support for collective measures to protect the immunocompromised, the coronavirus itself hasn’t cooperated, Kahn noted.
At the start of the pandemic, for instance, near-universal vaccination was touted as a way to protect the medically fragile by surrounding them entirely with immune people. That goal of creating “herd immunity,” however, has been put out of reach by a virus that continues to undermine vaccines’ protection.
“We find ourselves in a particular moment where the virus and the politics of the time have conspired to make it even harder” to convince Americans they should make sacrifices for the sake of others, Kahn said.
Deciding how many Americans we are willing to let die of COVID-19 each year is necessary to put the pandemic behind us.
People with impaired immune systems typically don’t produce a lot of antibodies after getting COVID-19 vaccines, which makes it easier for the coronavirus to sneak past one of the body’s first lines of defenses. Many immunocompromised patients also lack a robust army of B-cells, a second line of defense that blunts infection once a virus has established itself in the body.
The result: Even when they’ve been vaccinated, they’re more vulnerable to infection than their healthy peers. And once infected, they’re more likely to become severely ill or die.
A two-year study found that across 10 states, people with compromised immune systems were overrepresented among hospitalized COVID-19 patients by a factor of four. Even when vaccinated, these hospitalized patients were 40% more likely to require intensive care than fellow patients with healthy immune systems, and 87% more likely to die.
Transplant patients, who take powerful medications to prevent their immune systems from rejecting their new organs, have endured especially extreme peril. In the pandemic’s first 20 months, a study found that they died of COVID-19 at rates four times (for liver transplant recipients) to seven times (for kidney recipients) higher than the U.S. adult population as a whole.
The source and severity of these patients’ immune impairments varies widely, so they’re easy to miss as a group. But they’re all around us.
Almost 3% of Americans — roughly 7.2 million adults — have immune systems that have been deliberately suppressed to ready them for cancer treatment, to prevent rejection of an organ transplant, to treat autoimmune diseases like lupus and rheumatoid arthritis, or to tamp down dangerous levels of inflammation.
Then there are the more than half-million patients like Santos, who has a malignancy of the blood or lymph nodes that cripples a vital line of defense against infection. An additional 400,000 Americans with advanced or untreated HIV have T-cell depletion that can profoundly compromise their immune function.
COVID-19 patients who take months to overcome their coronavirus infections despite treatment can become incubators of dangerous new strains.
The immunocompromised are people like 55-year-old Louise Lerminiaux of Thousand Oaks, an advocate for transplant patients who has spent the pandemic zealously protecting herself and the kidney she was gifted 14 years ago. She shops for groceries at 7 a.m. when traffic is light, goes to movies in the afternoon to avoid crowds, and dons full protective gear when traveling to organ-transplant conferences.
Lerminiaux is never without a mask, and while she wishes others would keep wearing them as well, she knows her protection is in her own hands now.
“There is eye-rolling, for sure” when she wipes down surfaces on airplanes, she said. There are friends she’s let go because they won’t get vaccinated. She has seen what it’s like to be near death, she said, and “my life is more important.”

The thoughtlessness of fellow Americans has made life harder for Cindi Hilfman too. A kidney transplant patient who lives in Topanga, Hilfman, 56, said a man sneered at the face covering she wore when she traveled to Iowa for a funeral this summer.
“You’re clearly not from around here,” he said to her. “You know they don’t work, right?”
Hilfman knows that they do work, and that she can’t count on others for protection.
“I do see myself wearing my mask for years,” Hilfman said. “I’m not giving up that mask.”
For Santos, who coordinated hospital volunteers until he became ill, a weakened immune system has been a creeping threat. After being diagnosed in 2016 with follicular lymphoma, he was treated with chemotherapy and appeared to be in remission for five years.
A bout of back pain in the early days of the pandemic was the first sign that his cancer roared back as diffuse large B-cell lymphoma. Chemotherapy and a stem-cell transplant failed to produce a second remission, and in his weakened immune state, he developed a dangerous case of pneumocystis pneumonia.
Now awaiting a new type of cancer immunotherapy treatment, Santos said he has another chance at life. It’s a gift he must protect, even if it means missing Christmas celebrations that remind him of his childhood home in the Philippines and asking his kids to hold off on a full return to normal life, he said.

Long before the pandemic arrived, medical professionals who work with immunocompromised patients had counseled them to balance their own protection with their need for normality. But at this precarious stage of the pandemic, the first part of that equation must take precedence, experts say.
That’ll be more difficult given the dimming effectiveness of two key COVID-19 medications. The preventive drug Evusheld has been a potent adjunct to vaccine in protecting against infection, while the monoclonal antibody bebtelovimab has been used to treat mild or moderate COVID-19 in people who are at risk of becoming severely ill.
Thanks to the emergence of new coronavirus variants, Harvard infectious disease specialist Dr. Jacob Lemieux puts Evusheld‘s effectiveness at less than 25% “and dropping.” He assesses bebtelovimab’s ability to block disease progression to be 35% at best, and diminishing fast.
The antiviral Paxlovid, meanwhile, is of limited use to these patients because it can’t be safely taken alongside medications that are widely prescribed to immunocompromised patients.
As these pharmaceutical defenses against COVID-19 peel away, “it’s going to be tough times ahead” for people with weakened immune systems, said Dr. Camille Kotton, who specializes in treating people with immune impairment at Massachusetts General Hospital. Her patients aren’t immune to pandemic fatigue either, and she worries that many have let down their guard.
“At some point for them too, there’s a need to get on with life,” Kotton said.
Americans who still aren’t fully vaccinated against COVID-19 probably have some immunity from a past infection. They may not be so dangerous anymore.
And many Americans with weak immune systems haven’t taken full advantage of the armor that is available to them.
At Cedars-Sinai, Merchant is collaborating on a study of 1,000 patients who are severely immunocompromised. They “represent the whole spectrum” of COVID-19 beliefs, and their levels of protection reflect that, he said.
Roughly 10% of them have yet to receive a single dose of COVID-19 vaccine, and 25% have never received a booster shot. Fewer than 10% have gotten the newest booster, which is designed to target the Omicron strain.
“It’s actually shocking how few of our patients are getting boosted,” Merchant said.
Santos knows that any Christmas party involving his friends and family will include a handful of vaccine skeptics and COVID-19 deniers who’ve taken no steps to protect themselves or others. But with Americans racing to move on, he said another holiday season with face coverings and frequent coronavirus testing feels like too much to ask.
Defending COVID-19 safety measures “can ruin relationships,” Santos said. He tries to be respectful, he said, and his unprotected friends and family have honored his need to keep them at bay.
But he had hoped for a bit more empathy than that.
Getting vaccinated and sometimes wearing a mask are “an act of kindness, especially to those who are immunocompromised,” Santos said.