Scientists hope viruses hiding out in patients hold answers to long COVID
- Share via
Tracking microbes through a malodorous network of sewer lines led virologist Marc Johnson to the source of unusual coronavirus mutants.
After months of sampling effluent, the University of Missouri School of Medicine microbiologist found exactly where the mutants originated: from a regular user of restrooms at a specific Wisconsin business. Although unable to identify that individual, Johnson could still see from genetic data that viral particles were being freshly made and expelled for more than a year — many times longer than a typical two-week coronavirus infection.
And during that time, the mutations showed the virus was “running like hell,” trying to evade the person’s immune system, Johnson said. Laboratory analysis of his sewer samples exposed the battleground inside the patient’s body, where the virus was quickly evolving to maintain a stronghold.
“You can find lots of chronic infections — people that are probably infected for over a year — where the virus hasn’t changed at all,” he said. “And I don’t understand why in some patients it just goes crazy.”
As the COVID-19 scourge enters a fourth year, patients like the one Johnson uncovered by tracing back through miles of waste pipes and drains are nudging researchers closer to answers for key questions: Namely, where do worrisome new mutants come from? And what’s their role in long COVID, the mysterious post-infection ailment that afflicts more than 140 million people globally?
Scientists are exploring the possibility that some of the most infectious versions of the coronavirus — Omicron and its descendants — came from chronically infected individuals whose immune systems were weakened by disease, drugs or both. Research released in December shows the virus can persist throughout the body and brain for months. That suggests it may be able to hide out in human cells and tissues, not unlike the way HIV and the shingles-causing chickenpox virus do.
Traces in the blood and stool of patients experiencing protracted symptoms suggest that SARS-CoV-2 might be holed up in the gut, fat or other tissues that give shelter from the body’s immune defenses.
Researchers at the National Institutes of Health who conducted meticulous autopsies on the bodies of 44 COVID-19 victims found viral genetic material throughout patients’ bodies and brains for as long as 7½ months after symptoms began. In one case, virus particles isolated from the brain were grown in a lab dish, proving they were fully functional and capable of replicating.
“The predominant damage continues to appear to be in the lungs,” said Dr. Daniel Chertow, who led the research at the NIH’s emerging pathogens section, “but, oh, boy, we really need to better understand what type of damage is done in all these other places.”
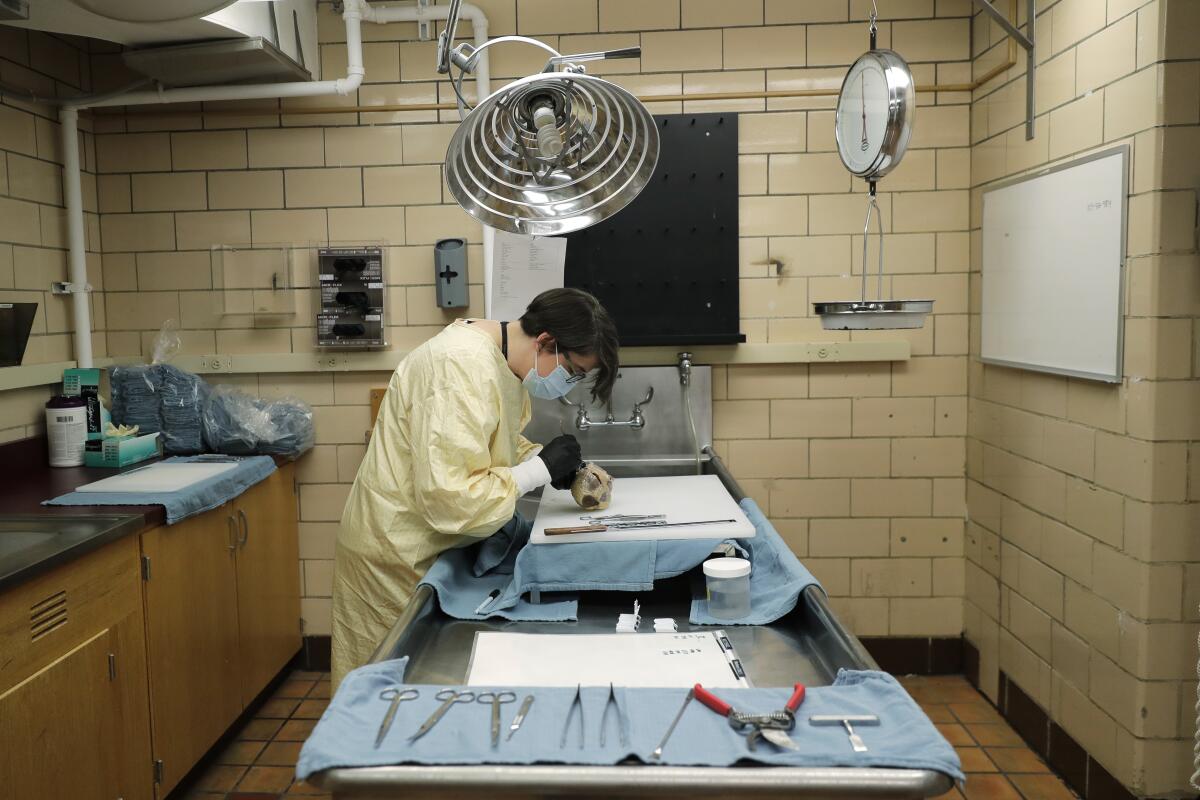
Dr. Maura Boldrini is studying the brains of people who died of COVID-19 to better understand how it causes neurological symptoms.
Most of those autopsied were older and ill even before catching COVID-19, and all died before vaccinations became available. And while none were known to have had long COVID, the findings published in the journal Nature still demand follow-up.
“We absolutely need to, in great detail, try to understand what, if any, role persistence of viral RNA and other viral components might play in long COVID,” Chertow said.
No one knows whether the coronavirus or its remnants remain in everyone who’s had COVID-19, or whether it’s just a group of patients, said Dr. Timothy Henrich, an associate professor of medicine at UC San Francisco.
“We’re all making the hypothesis that it is a driver of long COVID, but we really haven’t definitively shown that,” Henrich said. “That is still something that needs to be done.”
Still, Chertow’s research has already encouraged experimental use of antiviral medications such as Paxlovid to see whether it can root out viral reservoirs and alleviate long haul symptoms. Even a relatively small number of infected cells could provoke the immune system to produce inflammation, blood clots and other problems associated with long COVID, according to Amy Proal, co-founder of PolyBio Research Foundation, a nonprofit in Boston that facilitates research into chronic, infection-associated conditions.
It’s “the most logical explanation because it accounts for pretty much everything else,” she said.
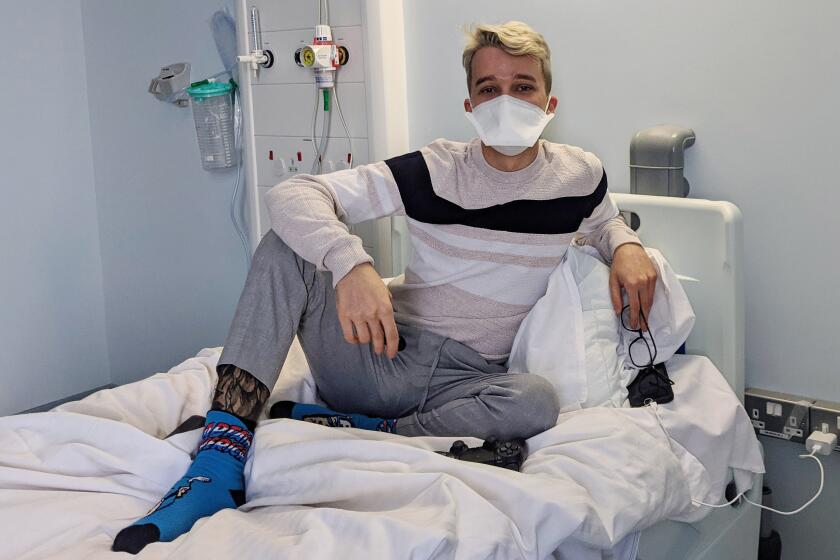
A young Briton agreed to be infected with the coronavirus for a scientific study of the most consequential virus on the planet.
Henrich, who helped develop sophisticated imaging techniques that can pinpoint HIV within tissues, plans to use the same approach to find COVID-19’s hideouts. Dozens of patients will undergo a series of whole-body scans that will look for signals of production or persistence of viral protein. Those will be compared with symptoms to see how the lingering presence of the coronavirus correlates to long COVID.
The group has started scanning patients to look for protective T-cells that could indicate an aberrant immune response to SARS-CoV-2. They’re examining biopsies of participants’ digestive tracts for viral vestiges, Henrich said.
A particular focus is lymphoid tissues that produce, store and carry T-cells that fight infection, and antibody-making B cells. The coronavirus may also be hiding out in long-lived nerve cells and heart muscle, where it may drive chest pain, brain fog, fatigue and other long COVID symptoms, said Dr. Diane Griffin, a virologist at the Johns Hopkins Bloomberg School of Public Health in Baltimore who has studied the body’s response to viral infections for more than 50 years.
“We have pretty good information from acute RNA virus infections that RNA does persist and that it does have consequences,” she said. “Basically, it’s hard to get rid of viruses.”
Proving that persistent viral infection causes long COVID will be difficult, Griffin said. Viruses in stealth mode suppress replication to avoid harming their host cells. Despite extensive distribution of coronavirus RNA throughout patients’ bodies, Chertow’s team saw little evidence of inflammation or that the immune system had tried to destroy infected cells outside the respiratory tract.
Intriguingly, when they analyzed the genetic makeup of virus specimens collected from six patients, the NIH scientists found versions in the lung that were different from those collected in other tissues. In one patient, viruses found in two brain regions — the thalamus and hypothalamus — were significantly different, suggesting that certain mutations favored the pathogen’s persistence there.
“We know that these RNA viruses have the potential to evolve within a host,” Chertow said. “The more they’re able to replicate and the longer the time that they have to do that, and the higher the level of replication that’s taking place, the more these viruses have the opportunity to evolve.”
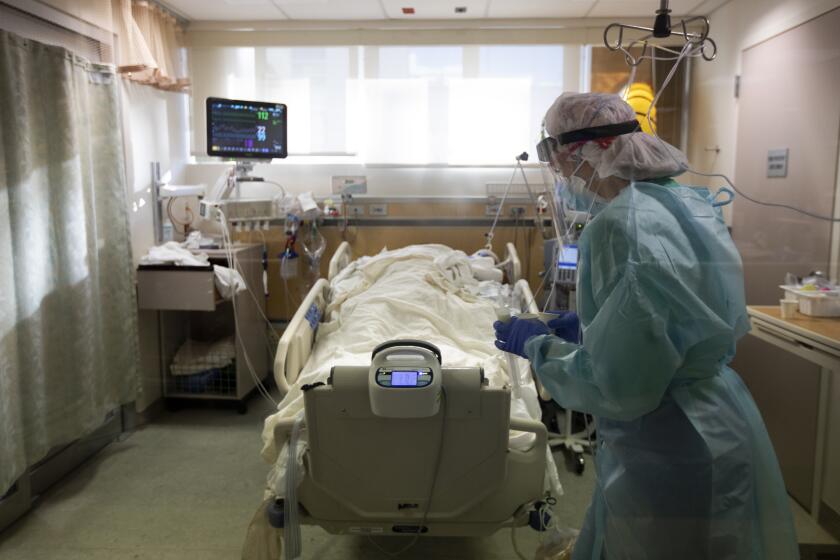
COVID-19 patients who take months to overcome their coronavirus infections despite treatment can become incubators of dangerous new strains.
That raises an interesting possibility: that as the virus evolves to inhabit different organs and tissues, the process may produce ever-more infectious and immune-evasive variants. No one knows yet if that’s the case, but Johnson’s analysis of wastewater at the University of Missouri is starting to yield clues.
Since the early days of the COVID-19 pandemic, researchers have known the disease is capable of infecting the digestive tract, resulting in gastric upsets and causing patients to shed traces of the virus in their feces. Johnson routinely scouts across some 100 Midwest sewer networks for unusual SARS-CoV-2 strains, called cryptic lineages because their source is unknown.
“They’re rare, but they’re out there,” he says.
When Johnson began the work in March 2021, he had no idea where it was going. Then, after Omicron drove COVID-19 cases in the U.S. to a record more than a year ago, he started actively looking for strains with distinct genetic changes.
He spotted one collected from a Wisconsin drain servicing 100,000 people. Its genetic signature was far more different than early versions of omicron, yet it hadn’t been reported in any patient. Importantly, its mutations began turning up in newer versions of Omicron. It was almost as if Johnson had seen where the virus was going — evolutionarily speaking — before it arrived.
“So we started saying, let’s figure out where it’s coming from,” he said.
Scientists are examining sewage for early signs of potential coronavirus outbreaks, turning waste into valuable health data.
For four months, he and his colleagues went from one manhole to the next in an undisclosed metropolitan area. Then they found the samples came from one building. Then one side of building. Then, half a dozen restrooms used regularly by about 30 people.
That’s where the investigation has stalled, Johnson said. Even so, he’s been able to deduce that the cryptic lineage is from an individual who was infected almost two years ago, since it evolved from a strain last detected in Wisconsin in April 2021.
In August, the variant’s concentration was 1.5 billion copies per liter of wastewater. By comparison, at the height of an enormous COVID-19 outbreak in a Missouri prison, a liter of wastewater contained only 100 million copies of the coronavirus.
“It’s crazy how much virus this person is shedding,” Johnson said.
In December, the same variant occurred in the Wisconsin restroom plumbing for the 13th straight month.
“Whoever this person is, they are apparently still going to work every day and have been for some time,” Johnson said. “It appears that they don’t know they’re infected. This can’t be good for them.”
Researchers are getting serious about understanding a disease patients call “long COVID.” Its symptoms include aches, fatigue, sleep problems and brain fog.
The lineage hasn’t turned up anywhere else, which suggests it isn’t spreading, Johnson said. But there’s no question that it can grow, as shown by the longtime high concentrations in the toilet drain.
“The question is why?” he said.
Johnson says studying cryptic lineages has challenged his thinking about the coronavirus’s ability to hang on in human tissues, especially those outside the respiratory system, and its potential to cause prolonged illness.
“I am now particularly open to the idea that there are secondary infections that we just don’t know about,” he said. “And maybe that helps explain some of these very odd long COVID symptoms.”