Britain becomes first country to approve gene-therapy treatment for sickle cell disease
- Share via
LONDON — Britain’s medicines regulator has authorized the world’s first gene-therapy treatment for sickle cell disease, in a move that could offer relief to thousands of people with the crippling disease in the U.K.
In a statement on Thursday, the Medicines and Healthcare products Regulatory Agency said it had approved Casgevy, the first medicine licensed using the gene-editing tool CRISPR, which won its makers a Nobel prize in 2020.
The agency approved the treatment for patients with sickle cell disease and thalassemia who are 12 years old and older. Casgevy is made by Vertex Pharmaceuticals (Europe) Ltd. and CRISPR Therapeutics. To date, bone marrow transplants, an extremely arduous procedure that comes with very unpleasant side effects, have been the only long-lasting treatment.
“The future of life-changing cures resides in CRISPR-based technology,” said Dr. Helen O’Neill of University College London.
“The use of the word ‘cure’ in relation to sickle cell disease or thalassemia has, up until now, been incompatible,” she said in a statement, calling the MHRA’s approval of gene therapy “a positive moment in history.”
Both sickle cell disease and thalassemia are caused by mistakes in the genes that carry hemoglobin, the protein in red blood cells that carry oxygen.
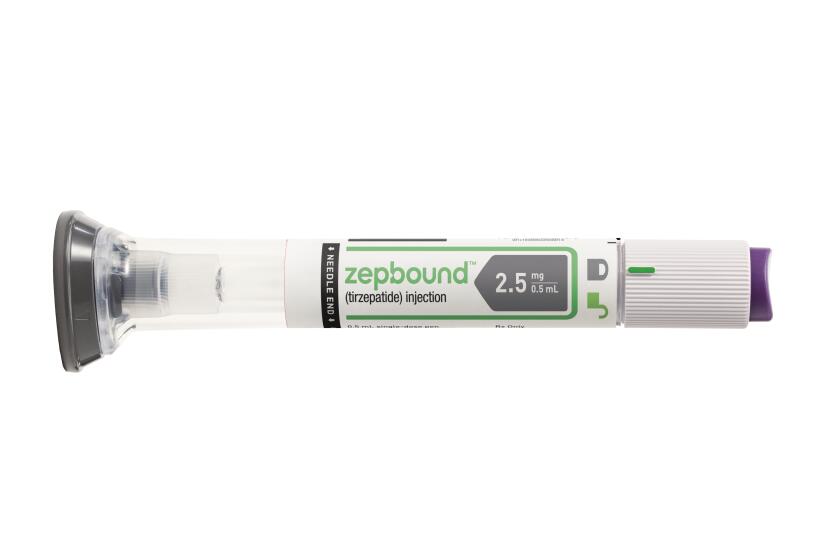
Federal regulators say the new version of the popular diabetes treatment Mounjaro can be sold as a weight-loss drug.
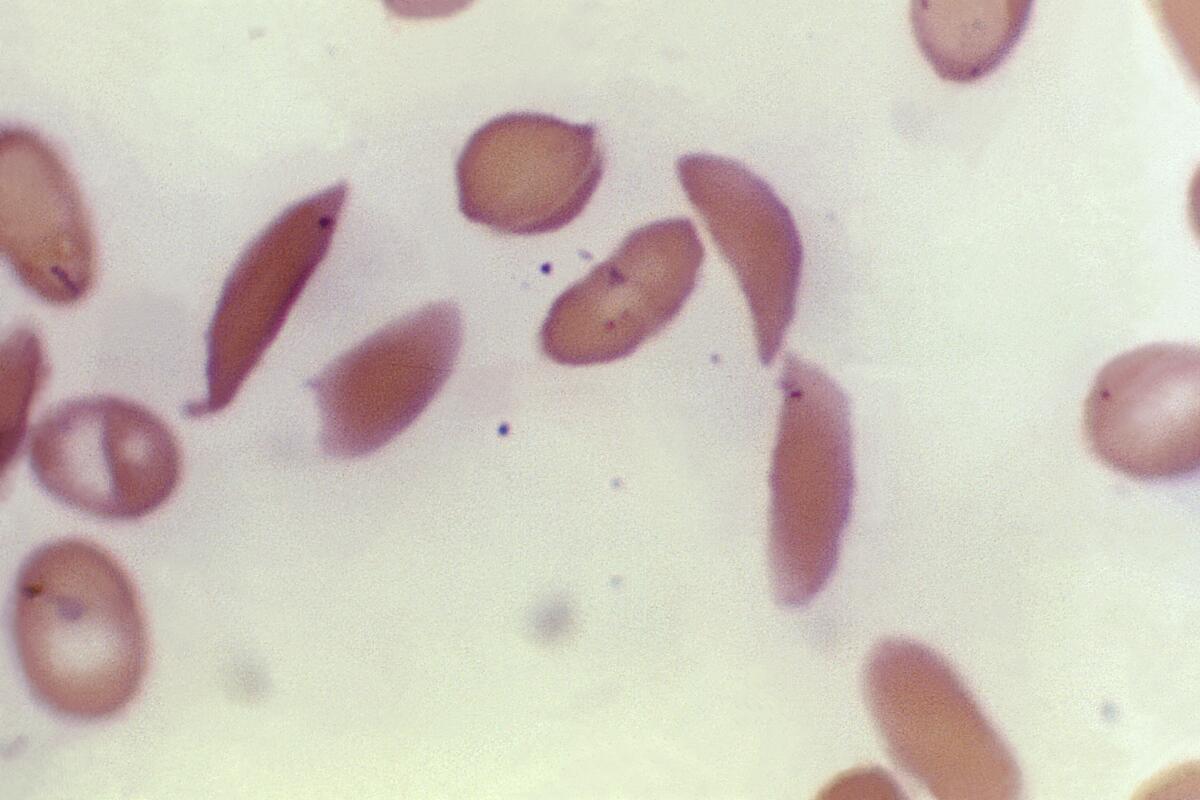
In people with sickle cell — which is particularly common in people with African or Caribbean backgrounds — a genetic mutation causes the cells to become crescent-shaped, which can block blood flow and cause excruciating pain, organ damage, stroke and other problems.
In people with thalassemia, the genetic mutation can cause severe anemia, and patients typically require blood transfusions every few weeks and injections and medicines for their entire life. Thalassemia predominantly affects people of South Asian, Southeast Asian and Middle Eastern heritage.
Casgevy works by targeting the problematic gene in a patient’s bone marrow stem cells so that the body can make properly functioning hemoglobin.
Patients first receive a course of chemotherapy, before doctors take stem cells from the patient’s bone marrow and use gene-editing techniques in a laboratory to fix the gene. The cells are then infused back into the patient for a permanent treatment. Patients must be hospitalized at least twice: once for the collection of the stem cells and then to receive the altered cells.
California’s Medicaid program is making it easier for people with diabetes to obtain the supplies they need to manage their blood sugar.
“This is so exciting. It’s a new wave of treatments that we can utilize for patients with sickle cell disease,” said Dr. James LaBelle, director of the pediatric stem cell and cellular therapy program at the University of Chicago. He said Britain’s approval suggested that U.S. authorization was probably “imminent.”
Casgevy is being reviewed by the U.S. Food and Drug Administration, which is expected to make a decision early next month, before considering another sickle cell gene therapy.
LaBelle said officials at the University of Chicago are “already moving forward to build not only the clinical infrastructure but also the reimbursement infrastructure to get these patients this treatment.”
Britain’s regulator said its decision to authorize the gene therapy for sickle cell disease was based on a study done on 29 patients, of whom 28 reported having no severe pain problems for at least one year after being treated. In the study for thalassemia, 39 out of 42 patients who got the therapy did not need a red blood cell transfusion for at least a year afterward.
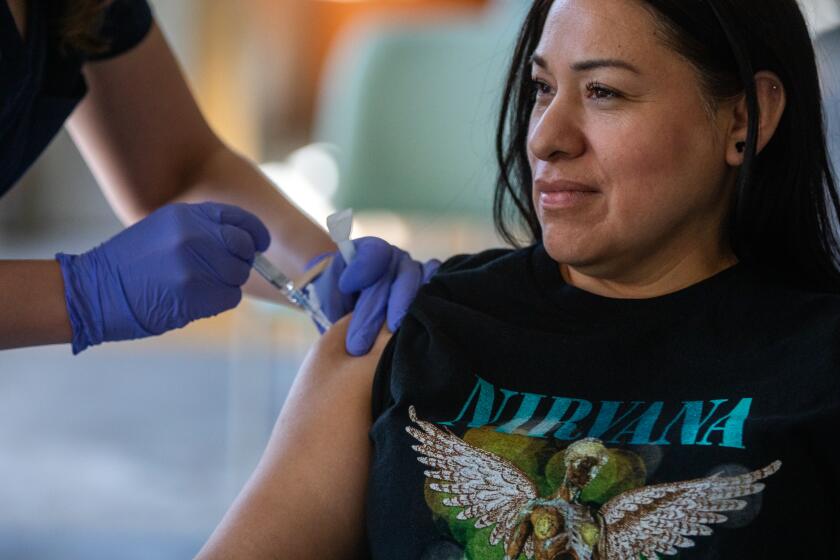
Only 5% of Californians have received the updated COVID-19 vaccine since it became more widely available earlier this month, and health officials say that’s not good enough.
Gene-therapy treatments typically cost thousands of dollars, and experts have previously raised concerns that they could remain out of reach for the people who would benefit most.
Last year, Britain approved a gene therapy with a list price of $3.5 million for treatment of a fatal genetic disorder. England’s National Health Service negotiated a significant discount to make it available to eligible patients.
Vertex Pharmaceuticals said it had not yet established a price for the treatment in Britain and was working with health authorities “to secure reimbursement and access for eligible patients as quickly as possible.”
In the U.S., Vertex has not released a potential price for the therapy, but a report by the nonprofit Institute for Clinical and Economic Review said prices up to around $2 million would be cost-effective. By comparison, research this year showed expenses for current sickle cell treatments, from birth to age 65, add up to about $1.6 million for women and $1.7 million for men.
Start your day right
Sign up for Essential California for the L.A. Times biggest news, features and recommendations in your inbox six days a week.
You may occasionally receive promotional content from the Los Angeles Times.
Medicines and treatments in Britain must be recommended by a government watchdog before they are made freely available to patients in the national healthcare system.
Millions worldwide, including about 100,000 in the U.S., have sickle cell disease. It occurs more often among people from places where malaria is or was common, such as Africa and India. Scientists believe being a carrier of the sickle cell trait helps protect against severe malaria.