Italy’s staggering COVID-19 death toll poses uncomfortable questions

- Share via
ROME — Italy could soon reclaim a record that nobody wants — the most COVID-19 deaths in Europe — after the healthcare system again failed to protect older people and the government delayed imposing new restrictions.
This wasn’t supposed to happen. Italy was the first country in the West to be slammed by COVID-19 and, after suffering a huge wave of deaths in spring, brought infections under control.
Italy then had the benefit of time and experience heading into the fall resurgence because it trailed Spain, France and Germany in recording big new clusters of infections. Yet the virus spread fast and wide, and Italy has tallied 28,000 dead since Sept. 1.
“Obviously there needs to be some reflection,” Guido Rasi, former executive director of the European Pharmaceutical Agency, told state TV after Italy reported a pandemic-high record of 993 deaths in one day. “This number of nearly 1,000 dead in 24 hours is much higher than the European average.”
Italy added 761 more victims Friday, bringing its official total to 63,387, just shy of Britain’s Europe-leading 63,603 dead, according to Johns Hopkins University. Both numbers are believed to greatly underestimate the real toll, due to missed infections, limited testing and different counting criteria.
Time-honored traditions of mourning along the Texas-Mexico border are upended by the pandemic.
Still, Italy could overtake Britain despite having 6 million people fewer than the U.K.’s 66 million, and would trail only the much larger U.S., Brazil, India and Mexico. Italy has the world’s second-oldest population after Japan, and older people are the most vulnerable to the virus.
The average age of Italian victims has hovered around 80. In addition, 65% of Italy’s COVID-19 dead had three or more other health problems before they tested positive, such as hypertension or diabetes, according to Italy’s Superior Institute of Health.
But that doesn’t explain the whole picture. Germany has a similarly old demographic and yet its death toll is one-third of Italy’s despite its larger population of 83 million. Germany recorded its highest daily number of COVID-19 victims Friday — 598 — with 21,000 dead overall.
Analysts point to Germany’s long-term higher per-capita spending on healthcare, which has resulted in greater ICU capacity, better testing and tracing capabilities and higher ratios of doctors and nurses to the population. But Germany also imposed an earlier, lighter lockdown this fall and is now poised to tighten it.
“If you can act sooner, even a bit lighter in the measures, they work better than acting harshly a bit later or too late,” said Matteo Villa, research fellow at the Institute for International Political Studies, a Milan-based think tank.
Italy, he said, waited too long after infections started ticking up in September and October to impose restrictions and didn’t reinforce its medical system sufficiently during the summertime lull.
“If you look at France and the U.K., you can see Italy did fare much worse,” he said. “And if you look at a comparable population with similar demographics, which is Germany, Italy did a lot worse.”
With another wave of infections feared to be just around the corner with Christmas visits and the winter flu season, many are wondering how many more will die.
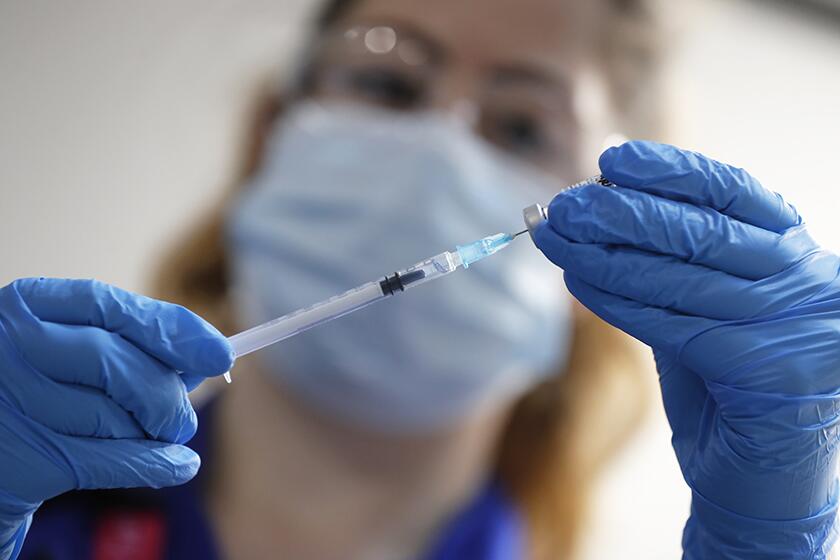
GlaxoSmithKline and Sanofi say their potential COVID-19 vaccine won’t be ready until late 2021 as they seek to improve its efficacy in older people.
Doctors have blamed systemic problems with Italy’s healthcare system, especially in hardest-hit Lombardy, for failing to respond adequately. They have cited the growth of private hospitals in Lombardy in recent years at the expense of public ones. Brain drain and bureaucratic obstacles have resulted in fewer doctors going into practice, while general practitioners have complained of a lack of support despite being the backbone of the system.
Nearly 80,000 Italian healthcare workers have been infected and 255 doctors have died.
“We asked for a lockdown at the start of November because the situation inside hospitals was already difficult,” said Dr. Filippo Anelli, head of the country’s doctors’ association. “We saw that it worked in the spring and allowed us to get out from under COVID. If this had been done, probably today the numbers would be coming down.”
But the Italian government resisted reimposing a nationwide lockdown this fall, knowing the devastating impact on an economy that was just starting to come back to life after the springtime shutdown.
Instead, on Nov. 3 the government divided the country into three risk zones with varying restrictions. But by then infections had been doubling each week for nearly a month and hospitals were already overwhelmed in Milan and Naples.
Italy also went into the pandemic poorly prepared. It had fewer ICU beds than the average of developed countries. And in recent weeks, investigative news reports have noted that Italy hadn’t updated its influenza pandemic preparedness plan since 2006 — which could help explain its critical shortage of protective equipment early on and its chaotic initial response to the pandemic.
A World Health Organization report, which was posted and then immediately taken down from the WHO website, noted that Italy’s 2006 plan was merely “reconfirmed in 2017” without being updated. The report said the plan was “more theoretical than practical” and that when COVID-19 hit, all hell broke loose.
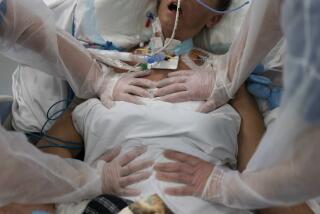
As intensive care units fill up and the death toll mounts, the Swedish government is mulling tougher measures to combat the coronavirus.
“Unprepared for such a flood of severely ill patients, the initial reaction of the hospitals was improvised, chaotic and creative,” said the report.
The United Nations health agency said it removed the report because it contained “inaccuracies and inconsistencies,” and then decided not to republish it because it developed other ways to assess countries’ responses.
Italy also ranked 31st — between Indonesia and Poland — in a 2019 survey of 195 countries compiled by the Global Health Security Index assessing abilities to respond to a pandemic or other healthcare crises. Italy scored particularly poorly in emergency response, preparedness, and communications with healthcare workers during a crisis.
Government officials admit they were caught unprepared but have strongly defended their response to the resurgence as scientifically sound and proportional to prevent the economy from collapsing. Domenico Arcuri, the government’s virus commissioner, said Thursday that the November restrictions were flattening Italy’s infection curve.
“Daily infections are coming down, hospital admissions are coming down, the number of people who unfortunately are admitted to intensive care [is] coming down,” Arcuri said.
That is small comfort to Marcella Polla, who announced the death of her 90-year-old aunt on Facebook on Dec. 6, saying she caught the virus in a hospital in October after complications following an angioplasty.
“My aunt was tough, made of Trentino fiber,” Polla wrote in explaining the extraordinary photo she posted of her aunt, holding herself up on a set of gymnastics rings this year. “I want to remember her like this, even though the thought of her and so many others dying alone and then being put in a body bag torments me.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.