New data reassuring for COVID-19 vaccination in pregnancy

- Share via
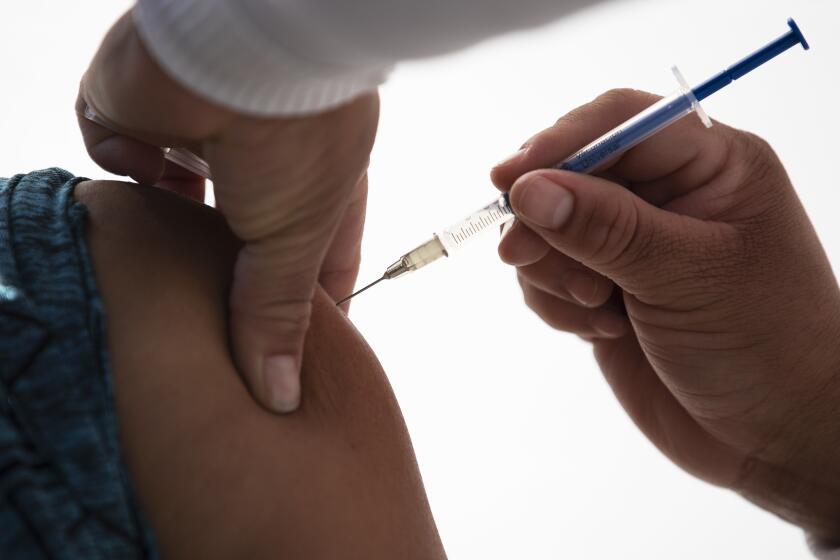
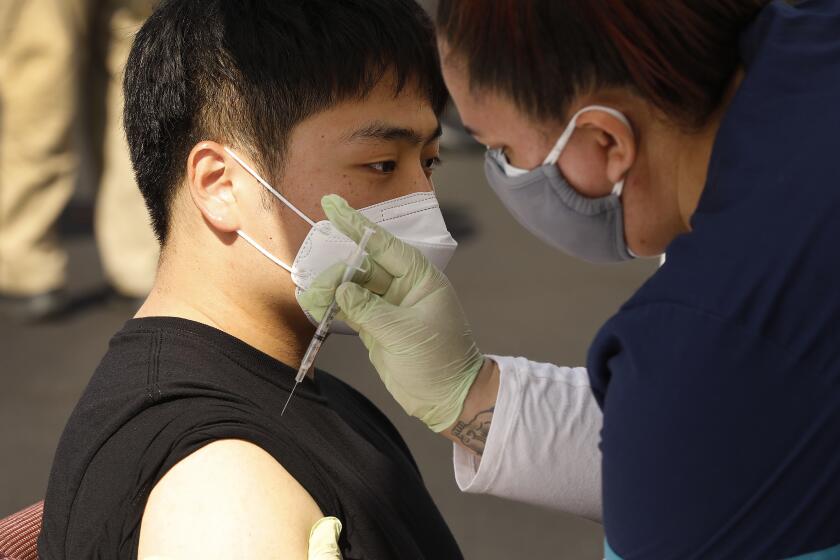
One of the largest reports on COVID-19 vaccination in pregnancy bolsters evidence that the shots are safe, although the authors say more comprehensive research is needed.
The preliminary results are based on reports from more than 35,000 U.S. women who received either the Moderna or Pfizer-BioNTech shots while pregnant. Their rates of miscarriage, premature births and other complications were comparable to those observed in published reports on pregnant women before the pandemic.
The new evidence from researchers at the U.S. Centers for Disease Control and Prevention was published Wednesday in the New England Journal of Medicine.
None of the women involved received Johnson & Johnson’s one-shot vaccine, which became available after the study. That vaccine is now in limbo as U.S. authorities examine reports of blood clots in a few women.
Separately, the American Society for Reproductive Medicine on Tuesday endorsed vaccination in pregnancy, based on evidence it has been evaluating for over a year.
“Everyone, including pregnant women and those seeking to become pregnant, should get a COVID-19 vaccine. The vaccines are safe and effective,” the society said in a statement.
A society representative said the group has not evaluated the latest evidence on Johnson & Johnson’s vaccine.
An American College of Obstetricians and Gynecologists representative said that the CDC report is promising but that longer-term follow-up is needed. That group has said previously that COVID-19 vaccination should be available to pregnant women and to those who are breastfeeding.
There’s little data to guide women who are pregnant, or trying to become pregnant, about whether to take a COVID-19 vaccine. Here’s what to consider.
Although pregnant women were excluded from studies that led to emergency authorization for the vaccines, evidence showed no harms in women who were unknowingly pregnant when they enrolled.
In addition, thousands of pregnant women in the U.S. have chosen to get vaccinated since the Food and Drug Administration authorized emergency use of the shots.
Dr. Laura Riley, chair of obstetrics and gynecology at New York’s Weill Cornell Medicine, said the new results are reassuring.
“It is great to have data to share with our patients who continue to weigh the risks and benefits of vaccination,” she said. “They know the potential complications of COVID infection in pregnancy and now there is some safety data in human pregnancies.”
Pregnant women who become infected with the coronavirus face elevated risks for complications, including intensive-care hospitalization, premature births and death.
With so many Americans becoming immunized, it’s natural to look ahead and wonder how long this protection will last. The answer: No one knows.
The study authors, led by the Dr. Tom Shimabukuro of the CDC, said continued monitoring and more evidence is needed, including on women who get COVID-19 vaccinations in the early stages of pregnancy.
Their study included information on 35,691 pregnant women in the U.S. who participated in a voluntary smartphone-based vaccination surveillance system. All of them received either the Moderna or the Pfizer-BioNTech vaccine between mid-December and late February.
It also included reports on pregnancy complications from almost 4,000 women enrolled in a U.S. vaccine safety registry. Of these, 86% — or 712 — resulted in a live birth, mostly among women vaccinated in the third trimester.
Most women reported injection site pain, but more serious reactions were less common. Pregnant women seemed more prone to injection site pain with both vaccines but less likely to experience other reactions than non-pregnant women.
In the vaccine registry, about 13% of pregnant women reported miscarriages, fewer than 1% stillbirths, 9% premature births and 2% birth defects. Those rates are all within the same range observed in reports in pregnant women before the pandemic.