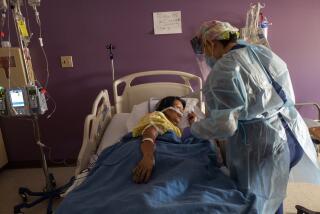What happens when an ICU reaches capacity?
- Share via
ATLANTA — The latest surge in coronavirus cases is overwhelming many intensive care units, causing hospitals and states to run out of ICU beds in some locations.
Kentucky and Texas broke records this week for COVID-19 hospitalizations, joining a handful of other states that reached the same milestone in recent weeks. Arkansas said it ran out of ICU beds for COVID-19 patients for the first time since the pandemic began.
Nearly 80% of the country’s ICU beds — or about 68,000 — were in use Thursday, according to the U.S. Department of Health and Human Services. And about 30% of those beds, or nearly 25,000, were filled by someone with COVID-19.
As states get hammered by the super-transmissible Delta variant, the surge has raised questions about what it means for individual patients in places where there are no available beds. Here are some answers:
What is an ICU?
ICUs are designed to care for the most acutely ill people. They employ more staff, specialists and equipment to keep patients alive. Machines monitor breathing and heart rates. “Crash carts” are ready with defibrillators and intubation tubes if people have trouble breathing or their hearts stop.
Typical patients have just undergone extensive surgery. Some could have major trauma from a car accident. And, of course, some could be sick with COVID-19. Their lungs are damaged and they need ventilators. Nurses look after them — but so do pulmonologists, respiratory therapists and infectious disease specialists, among others.
“It’s not just having staff — it’s having the right kind of specialists or the right kind of nurse to be able to care for that individual,” said Nancy Foster, vice president of quality and patient safety policy at the American Hospital Association.
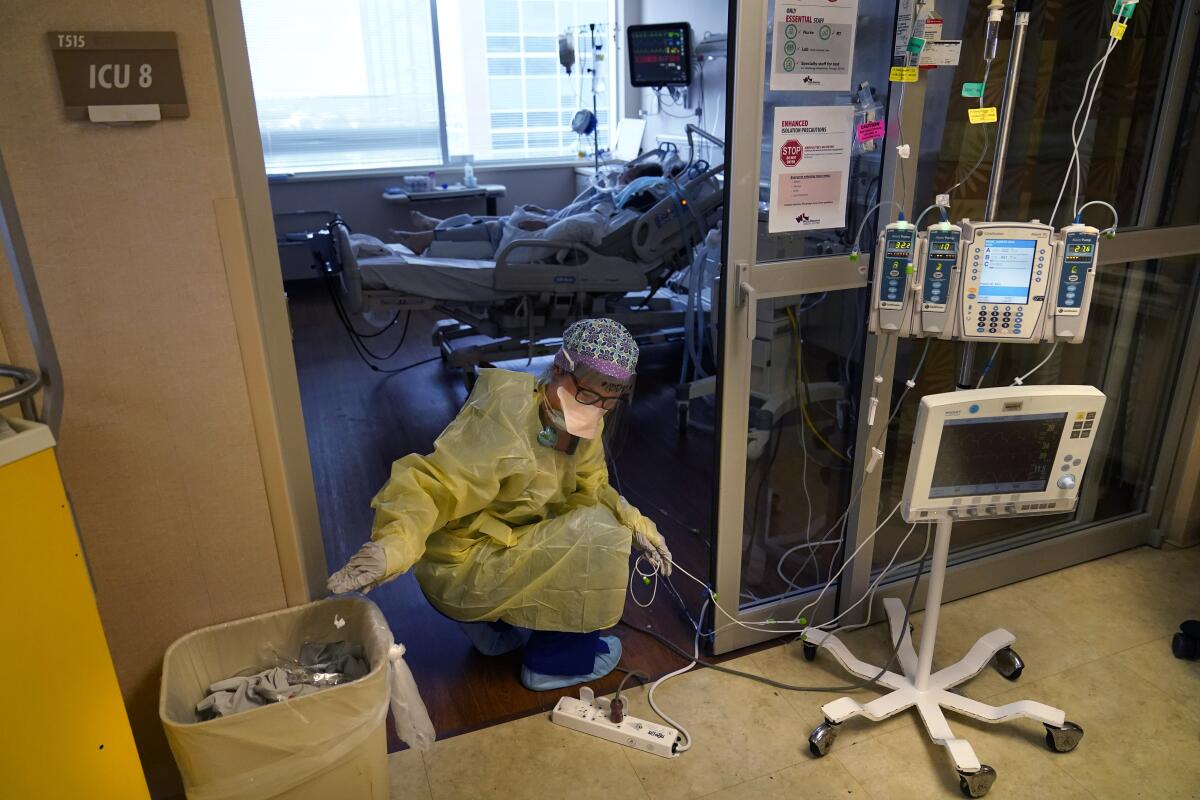
What happens when an ICU reaches or exceeds capacity?
A maxed-out ICU can become a staffing and logistical nightmare.
Nurses who might normally take care of one patient now must keep three or four people alive. Non-ICU staff are brought in to assist. Patients can back up in emergency rooms waiting for an ICU bed to open. And hospitals are forced to creatively convert space into makeshift ICU units.
At Phoebe Putney Memorial Hospital in Georgia, the crush of COVID-19 patients has led to the recruitment of scores of employees who don’t normally work on patient floors. They included Scott Steiner, the health system’s president and chief executive.
On Sunday, Steiner helped turn COVID-19 patients on their stomachs so their ravaged lungs could possibly take in more oxygen. The maneuver can require six people, depending on a patient’s weight.
“This is all hands on deck,” Steiner said.
On some campuses, the surge has displaced beds reserved for procedures such as colonoscopies or carpal tunnel surgery, said Roberta Schwartz, executive vice president of the Houston Methodist hospital system, where coronavirus patients filled nearly half the ICU beds earlier this week. A post-operation recovery bay was turned into ICU space.
Schwartz likened an inundated ICU to a home that is overwhelmed with overnight guests and the host is blowing up air mattresses to accommodate.
“It’s not very comfortable, but it works,” she said. “And a blow-up mattress is better than a sleeping bag, which is better than a tent outside.”
How does it affect patients?
Patients may have to linger in emergency rooms waiting for an ICU bed, and that spills over to other patients.
This week, some Texas hospital systems temporarily closed their off-site emergency rooms and sent staff to their hospitals overstretched by COVID-19.
Patients who arrive at hospital emergency rooms could wait several hours — and sometimes days — to get into an already overwhelmed ICU.
“We basically do ICU in the emergency room,” said Schwartz of Houston Methodist. “You may hold down there for 45 minutes, and you may hold for three days.”
“You’re going to get great care if you can come to one of our facilities,” Schwartz added. “But ideally you want to get people up to the appropriate unit as quickly as you can.”
In rural areas, ICUs can be scarce to begin with. Fewer than 3% of ICU beds nationwide are in small rural hospitals, according to the American Hospital Assn.
Requests often come into larger hospitals’ ICUs to take transfers.
“We can’t take many of those patients because we are at capacity,” said Dr. Steppe Mette, chief executive of the medical center at the University of Arkansas for Medical Sciences. ”All of our ICUs are full. And our emergency room is full of patients needing ICUs.”
How does it affect staff?
Increasingly, staffers are burning out.
This week in the ICUs of South Florida’s Memorial Healthcare System, staffers were at one point caring for 107 COVID-19 patients who were the “sickest of the sick,” said Dr. Aharon Sareli.
Many failed to respond to steroids or other treatments. They needed ventilators and were facing the failure of multiple organs. Many were expected to die.
“It’s physically and emotionally extremely draining for the staff,” Sareli said.
Hospitals are already experiencing a labor shortage of nurses and other medical staff. Some staff are leaving, and those who are staying are disgruntled and losing compassion.
“I think they’re also a bit stunned that 18 months in we’re still doing it, and it’s worse than ever,” said Steiner of Phoebe Putney Memorial Hospital in Georgia. “Some are just mad because so many people are not vaccinated.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.