Op-Ed: The sustainable development goals and surgery: Is a ‘moon shot’ the answer?
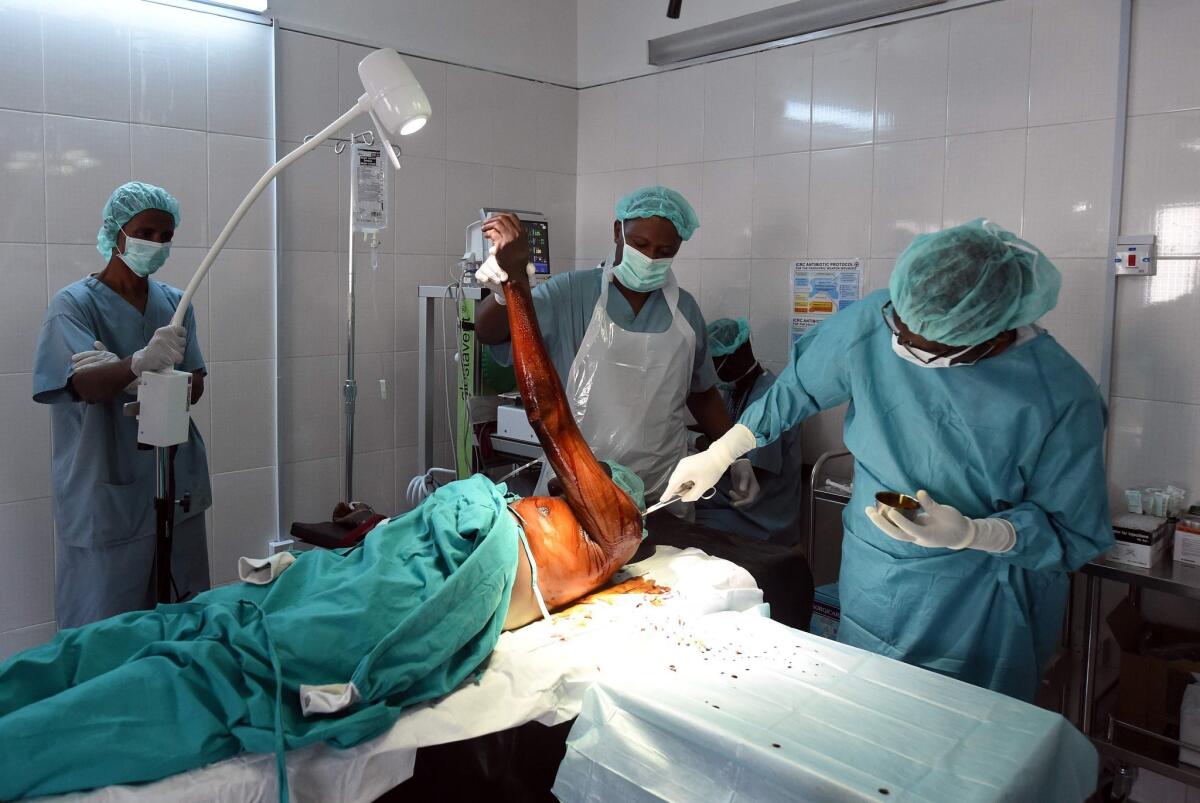
A man undergoes surgery in a hospital ward after being injured in an attack by Boko Haram militants in Maiduguri, capital of northeastern Nigeria’s Borno state in February 2016.
- Share via
One pleasant weekend in September more than 150 world leaders converged on the United Nations to adopt the Sustainable Development Goals, or SDGs -- the world’s new 17-point agenda to “end poverty, hunger and inequality, take action on climate change and the environment, improve access to health and education … [and] build strong institutions and partnerships.” To achieve, in other words, sustainable development.
The admirable aspirations set forth by this agenda, however, will fail to materialize without robust health systems worldwide. The interdependent relationship between health and socioeconomic development has been well documented. In the words of American anthropologist and humanitarian Dr. Paul E. Farmer, as the Ebola outbreak that ravaged West Africa proved, most of the world lacks access to the basic “staff, stuff, space and systems” necessary to combat disease and repair the human body. In fact, more than 5 billion people – the vast majority of the world’s population – lack access to safe, affordable and timely surgical and anesthesia care. This is particularly unfortunate since roughly a third of the global burden of disease requires surgical and/or anesthesia decision-making or treatment. More than 17 million people will die this year of surgically related conditions, surpassing the combined deaths from AIDS, tuberculosis and malaria. Why does a lack of surgical and anesthesia care affect so many? It is because surgery and anesthesia are not disease entities. They are treatment modalities that address the breadth of human disease – infectious, noncommunicable, maternal, child, geriatric and trauma-related disease and injuries. Treating the sick very often requires surgery and anesthesia.
Unfortunately, “hospitals” in most of the world are ill-equipped to treat sick patients: a third to three-quarters of hospitals in low-resource settings lack consistent access to electricity, running water, oxygen and other equipment basics. Sadly, in many regions of the world, “hospitals” are buildings in which people go to die -- a fact not lost on the poor, who have no other option. Further, the few surgeons, anesthesiologists and obstetricians who do work in low- and middle-income countries are often drawn to Boston or Boise rather than Bihar or Bangladesh. Finally, as healthcare expenses are the leading cause of impoverishment worldwide, those lucky few able to reach and receive care are most likely left destitute – a perverse trade-off between illness and impoverishment.
Recently in American healthcare politics we have used the metaphor of the “moon shot” for curing disease; a metaphor that, by the way, was actually accomplished in 1969. The majority of the world’s poor do not need a “moon shot.” They need functional infrastructure, a trained workforce, supplies that arrive on time and processes necessary to assure a mother is saved from postpartum hemorrhage, a child from a perforated appendix, or her father from a fractured femur.
In the era before World War II, international health was focused on keeping armies disease-free, and workers and colonists healthy enough to be productive for the motherland. After World War II, the old colonial paradigm was rejected in favor of an era of renewed global collaboration. The World Health Organization was born and the major disease threats of the time – smallpox, polio, cholera, malaria – were systematically targeted to varied success. Encouraged by the wins, a buoyant world community pledged in Alma Ata in 1979 (10 years after Apollo 11 landed on the moon) to achieve universal primary healthcare by the end of the century. The end of the 20th century came and went without universal primary healthcare, but at least we had sent a man to the moon.
As the initial enthusiasm for universal primary care receded, the inability to find financing mechanisms led to a narrower view of what could be achieved. Low-cost interventions such as immunizations were funded at the expense of important, but higher-priced solutions such as building clinics and hospitals capable of both providing immunizations and other treatments. Building comprehensive primary care and hospital systems were seen as too expensive and, in the case of surgery, too complicated for the realities of the global health landscape. Only recently in the 21st century, after lessons learned from the HIV/AIDs epidemic, has the public health community come to recognize that the more expensive can sometimes be the more valuable. Surgical interventions, for example, are now deemed amongst the most “cost-effective” public health interventions around, competing with more traditional favorites such as immunizations.
Regardless of the historical reasons for these failures in health and surgical system strength -- and there is plenty of blame to go around -- what we know for sure is that a focus on true, comprehensive health systems strengthening has never before been part of the global health agenda. The stakes now could not be higher, the urgency never more acute given our global community. A fever in Sierra Leone is felt in San Francisco and within a few hours; weak health systems anywhere affect humanity everywhere. The other hard reality is that in this new world health order, the poor lose first and the poor lose the most. The world’s poorest economies could lose $12.3 trillion over the next 15 years because of the burden of surgical illness. And low- and middle-income economies will lose a staggering 2% of gross domestic product per year by 2030 if surgical and anesthesia capacity is not integrated as an equal partner in health system strengthening.
Fortunately, the world is paying attention. Last year, the World Bank, World Health Organization, and Lancet Commission on Global Surgery released major policy documents outlining paths to universal access to strong health systems inclusive of surgical and anesthesia care. Surgical indicators are appropriately collected and will be reported on major global platforms, including the World Bank’s World Development Indicators, and major surgical strategic planning processes are underway in Cape Verde, India and Zambia. The momentum is building.
The past century in global health has taught us that we do not need to travel to the moon to achieve the Sustainable Development Goals. We need to invest in strong health systems, and surgery and anesthesia care represent a major cross-cutting foundation for these systems. The goals will only be possible when ministries of health prioritize integration of surgery and anesthesia within national health plans, and when international funding agencies switch from vertical disease-based funding to funding that strengthens health systems that include surgery and anesthesia, and when the World Bank and the World Health Organization make a commitment to tracking indicators related to surgery. The future of the Sustainable Development Goals depends on including surgery and anesthesia as partners in healthcare at every level.
John Meara MD DMD MBA is the Kletjian Professor of Global Surgery at Harvard Medical School and co-chair of the Lancet Commission on Global Surgery. Nakul Raykar MD MPH is the Chief Fellow of the Program in Global Surgery and Social Change at Harvard Medical School.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.













