Editorial: End the outdated, unscientific restrictions on gay blood donors
- Share via
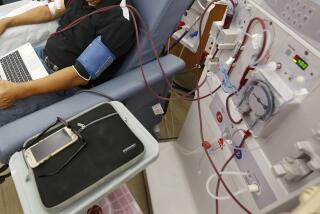
More than 30 years ago, as the AIDS epidemic exploded, the nation’s blood banks banned donations from men who had sex with other men.
The logic was sound at the time. Tests of the era couldn’t adequately detect HIV, the virus that causes AIDS. As a result, thousands of people unwittingly contracted HIV from tainted blood during transfusions. Banning donations from gay men was a drastic step, but necessary to protect the nation’s blood supply.
Things have changed in the intervening three decades, though — including the science of blood testing, which gets better virtually every year. Tests are now so accurate and rapid that blood banks can tell with near certainty if blood has been infected with HIV even if the donor had been exposed to the virus just 10 days previously. Today, the risk of contracting HIV from blood in the United States is only about 1 in 1.5 million.
Advances in testing mean that a blanket blood donor ban on gay and bisexual men is no longer necessary.
The advances in testing mean that a blanket blood donor ban on gay and bisexual men is no longer necessary. With that in mind, the U.S. Food and Drug Administration studied relaxing the ban and last last year it wisely acceded to calls — from this page, among others — to update its blood donation recommendations and stop calling for a lifetime ban on blood donations from men who have sex with men. The FDA continued to recommend a ban on donations from commercial sex workers and intravenous drug abusers. Although the agency’s recommendations do not have the force of law, blood banks typically adopt rules at least as stringent for liability reasons.
The recommendations adopted in December were not much of an improvement, however. Men could donate blood only if they hadn’t had sex with another man for 12 months. Why 12 months? Good question. There’s no science that supports a yearlong donor deferral for gay and bisexual men. It seems the FDA chose a 12-month waiting period not because that span of time is demonstrably safer but because that’s what other countries (including Britain and Australia) have done.
But a year without sex is a de facto ban for sexually active men, making the new rules just as senselessly discriminatory as the old ones. This became clear to the public in June after the deadliest shooting in the nation’s history, when a gunman opened fire at Pulse, a gay nightclub in Orlando, Fla., killing 49 people and wounding 53 others. When members of the local LGBT community turned out to give blood to help those injured in the shooting, many were barred from doing so.
The incident prompted 24 U.S. senators to sign a letter to the FDA, asking the agency to develop “better blood donor deferral rules that are grounded in science, based on individual risk factors, don’t unfairly single out one group of individuals, and allow all healthy Americans to donate.”
The FDA agreed to reconsider its call for a 12-month restriction. Instead, it said it would look at the feasibility of a system that evaluates potential male donors based on the risk posed by their individual behavior. This process is supported by gay rights advocates, some public health experts and the American Medical Assn., which say it makes more sense than a ban that discriminates against people who may be perfectly safe blood donors. We agree. The waiting period should be shortened to a more reasonable length and donors should be evaluated based on their behavior, not their sexuality.
This approach would rely on an extended pre-donation screening process in which donors would answer questions about things that might increase their risk of infection. People could lie, of course, but they can lie under the existing system as well. There’s no background check for blood donors.
But health experts say people who volunteer to give blood are typically healthier than their counterparts in the general population. Furthermore, the nation’s blood banks have always relied on the honesty of donors. For the most part, that has been sufficient, because people are not donating for money or other personal gain, but voluntarily to help others. Besides, every pint of donated blood is tested, and with testing accuracy improving all the time, there’s no scientific reason for waiting a whole year.
It’s time to end to restrictions that are based on fear rather than science. The FDA should shorten the recommended waiting period to a more practicable length and work toward developing a risk assessment model.
Follow the Opinion section on Twitter @latimesopinion and Facebook
More to Read
A cure for the common opinion
Get thought-provoking perspectives with our weekly newsletter.
You may occasionally receive promotional content from the Los Angeles Times.