U.S., foreign health workers to flock to West Africa amid Ebola crisis

- Share via
reporting from JOHANNESBURG, South Africa — With dozens of local doctors and medical staff among the dead, U.S. and foreign experts are preparing to flood into West Africa to help fight the deadliest Ebola outbreak on record.
Although two Americans, Dr. Kent Brantly and health worker Nancy Writebol, have contracted the disease, health experts say foreigners taking careful precautions should not be at serious risk.
But more than 60 local medical staff, about 8% of the fatalities, have died in Sierra Leone, Liberia and Guinea — poor countries with weak, overloaded healthcare systems that are ill-equipped to handle the outbreak.
Ebola expert G. Richards Olds, dean of medicine at UC Riverside, compared local healthcare workers there to doctors who donned beaked masks, leather boots and long, waxed gowns to fight the plague in medieval Europe.
“This is one of the few cases in modern times of true healthcare heroism,” Olds said. “They’re taking some significant risks, as you can see, to help others.”
Among the dead are Liberia’s Dr. Samuel Brisbane, and Dr. Sheikh Umar Khan, a top Sierra Leone doctor who treated dozens of patients. Khan was described as a national hero by his country’s health ministry. Three nurses working with him died the same week he perished.
Dr. Tom Frieden, head of the Centers for Disease Control and Prevention, said Sunday the U.S. plans to send 50 public health officials to West Africa in the next 30 days to help fight the disease.
He said Brantly, who arrived in the U.S. on Saturday and is undergoing treatment, appears to be getting better. Writebol is expected to arrive in the U.S. this week. Both contracted the disease in Liberia.
The World Health Organization said Friday that it planned to fly hundreds more medical staff into West Africa to stem the spread of the disease and trace those who had contact with infected people.
Dubai-based airline Emirates, the Mideast’s largest carrier, said Sunday that it halted flights to Guinea because of concerns about the spread of the Ebola virus, which has killed more than 700 people since March.
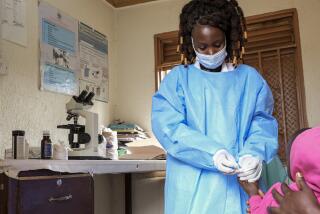
The protective gear required to confront the disease consists of rubber boots, medical scrubs, two pairs of rubber gloves, a waterproof, airtight yellow suit, a rubber apron, a rubber bib, a rubber hood and a mask. It is a suffocatingly hot outfit in West Africa’s tropical heat.
There’s a complex five-minute procedure to put the gear on, take it off and determine whether gowns can be reused. One mistake can be fatal.
Medical hygienists, who clean up after patients and dispose of fluids including blood, vomit and diarrhea, are the most at risk.
Olds said Ebola is less infectious than SARS, the airborne disease that spread from Asia around the world in 2003, but it is far more deadly.
Although Ebola is highly infectious, it’s not transmitted by air, and when a doctor or nurse sickens, it usually means something has gone wrong in the complex process of robing and disrobing.
In West African public hospitals, some employees are working 12-hour shifts. Whether it’s heat (the temperature inside suits can rise to more than 100 degrees), long hours, exhaustion, lack of staff or lack of training, fatal mistakes have been made.
Health workers from organizations such as Doctors Without Borders and other relief agencies also do outreach work in West African communities to try to persuade frightened people infected with the virus to come to treatment facilities. Most of the outreach work is done without protective clothing or masks.
Medical staff do not approach closer than two yards when assessing sick people. If they have to enter a house to see an ill person who can’t move, they don their gowns and protective layers.
Doctors Without Borders nurse Monia Sayah, who returned home to the U.S. recently after months working in Guinea treating patients, said she felt safe in her protective medical clothing, despite the fact many doctors and health staff had sickened and died.
Doctors Without Borders has never had an Ebola fatality.
“We have very strict measures to avoid infection. We use a set of behaviors. It’s very important the way we dress up and the way you dress down. We use a buddy system to make sure you don’t make a mistake when you are putting on or taking off the gown,” Sayah said.
Doctors Without Borders was also meticulous about minimizing the use of sharp objects in the treatment centers.
Intravenous needles were used only when absolutely necessary. Patients weren’t given knives and forks to cut their food. Instead the food was cut up for them outside the isolation unit.
Chlorine, among other disinfectants, was used in the treatment facilities to sanitize boots, clothing and other items, Sayah said.
Frieden said Sunday that Americans should not fear Ebola taking hold in the U.S.
“Any U.S. hospital following CDC’s infection control recommendations can safely manage a patient w/ Ebola hemorrhagic fever,” he said on Twitter.
Doctors Without Borders has been “caring for patients with Ebola in rudimentary facilities in Africa and has never had one of their health workers infected,” he said, adding that meticulous procedures prevented the virus from spreading.
Times staff writer Lauren Raab in Los Angeles contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.