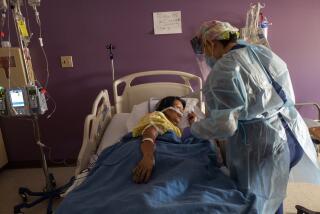Space, staffing worry county hospital
- Share via
For months, officials at Los Angeles County-USC Medical Center have been buzzing with excitement about the anticipated opening of their new home.
But that opening has been delayed repeatedly, most recently last week. Officials announced that the move to the new facility would be postponed from Oct. 17 to Nov. 7, citing challenging schedules for the hospital and state inspectors, as well as last-minute work not yet completed by sub-contractors.
Two main concerns loom over the $1.02-billion medical center’s opening: Are there too few beds, and will there be enough doctors to fully staff the expanded emergency room when it opens?
There are 824 licensed acute-care beds at the current County-USC hospital (most recently the facility has been filling about 590 of them), but there are only 600 such beds in the new building next door. Those 600 won’t offer much breathing space for the hospital if, say, a bad flu season overwhelms emergency rooms throughout Southern California. (On Thursday, 588 licensed beds were in use at the current center; if the old hospital had moved into the new facility last week, it would have been about 98% full.)
“Our concern is the peaks,” said Dr. Stephanie L. Hall, County-USC’s chief medical officer. Hall likened the situation to a glass of water filled close to the brim; adding more water causes a spill.
A shortage of beds would cause a backup of emergency room patients waiting for admission, causing wait times to lengthen, according to a report submitted to the county Board of Supervisors in July. The report warned that the “hospital opens at the tipping point,” and said that the newness of the facility might attract a 5% to 15% increase in patient arrivals.
Officials have been working on several measures to reduce the number of patients who are in the hospital at any given time.
Last month, the hospital, located two miles east of downtown Los Angeles in Boyle Heights, began moving some patients to the county-run Rancho Los Amigos National Rehabilitation Center in Downey, Hall said. There are 25 acute-care beds at Rancho, and if necessary, it can ramp up to hold 50.
County-USC has also worked to reduce inefficient down time. For example, several years ago, it took an average of three days from the time an X-ray was ordered to the time it was completed and read by a physician. Now, it takes less than 24 hours, said Pete Delgado, County-USC’s chief executive. The hospital has also reduced delays in giving prescriptions to patients waiting to be discharged.
Such measures have helped free up beds more quickly, allowing patients waiting in the emergency room faster access. In July 2006, it took an average of about seven hours for emergency room patients to get a bed once they were deemed sufficiently ill to be admitted; by June 2008, it was about three hours. A patient’s average length of stay has been reduced from 6.6 days in 2003 to 5.2 days this year.
Delgado said the increased efficiencies and the bed space at Rancho should allow the new County-USC facility to accommodate the volume of patients the hospital sees today.
“Don’t get me wrong, the hospital footprint is going to be tight,” Delgado said. “Going forward, if the market changes or something happens, we’re going to have to depend on the capacity in Rancho and other Department of Health Services hospitals.”
Doctors at neighboring hospitals have expressed concern about County-USC’s reduction in bed capacity. “There’s legitimate concern. The number of beds in hospitals in Los Angeles, in general, is inadequate, and that’s become clear when we have flu outbreaks,” said Dr. Brian Johnston, medical director of the emergency department at White Memorial Medical Center, just one mile south of County-USC.
During an outbreak of respiratory illness in February, Los Angeles County hospitals were diverting 9-1-1 patients away from their emergency rooms an average of about 30% of the time, significantly higher than the yearly average of 12.6% in 2007.
“We had a little really minor flu outbreak, and it brought the system to a standstill,” Johnston said. “That tells you there is no elasticity in the system.”
Johnston said the county Board of Supervisors made a mistake a decade ago when it approved a 600-bed hospital. A majority of the board said the county could afford to run only a smaller-sized hospital; Supervisor Gloria Molina had called for a 750-bed replacement.
“They are reducing the size of their [healthcare] system to fit the budget,” Johnston said.
Rob Fuller, executive vice president at Downey Regional Medical Center, said fewer hospital beds will translate to backups in emergency rooms and longer ambulance transport times throughout the region.
“The county says it will operate more efficiently,” Fuller said. “I’m personally skeptical. . . . There’s not a lot of spare capacity in the system.”
California is in the midst of a well-documented bed shortage in hospitals. Nationwide, there is an average of 3.4 beds per 1,000 residents, but in California, that average is two beds per 1,000. In some parts of the Los Angeles area, the ratio is less than one bed per 1,000, said Jim Lott, executive vice president of the Hospital Assn. of Southern California.
Lott said his organization will conduct a study after the new facility opens to see whether its 600-bed limit will have any effect on neighboring hospitals.
He said there is a “high degree of skepticism among hospital operators in Los Angeles” that County-USC will be able to manage its patient load.
“They are counting on being able to treat the same number of patients by effecting efficiencies, reducing length of stay and running the facility at 90% to 95% occupancy. Those are some really aggressive assumptions, and so we don’t know whether that’s going to work or not,” Lott said.
A second major concern is whether County-USC will have enough doctors to staff its new, much larger emergency room, which will increase from 94 beds to 131.
Dr. Edward Newton, chairman of County-USC’s department of emergency medicine, said he continues to wait for the county and USC to agree on a new contract (the county pays the university to hire some of the hospital staff).
Newton said he needs time to recruit emergency room doctors once the contract is signed.
“I just can’t go to a Home Depot and pick the first 14 people I see and say, ‘Come work at the emergency department,’ ” Newton said. He said he needs to recruit staffers who are “sufficiently trained to work in a Level 1 trauma center” and emergency physicians who are “qualified to supervise and teach residents.”
Newton said doctors generally need to give a month’s notice before they can begin working at a new job, but it can take even more time if, for example, a doctor hired from out of state needs to obtain a California medical license.
“We’re trying to work out other funding mechanisms where I can temporarily hire other people,” Newton said. “The bottom line here is I can only open as much space [in the emergency room] as I have people. But we’re working on solutions . . . that will enable me to open the whole emergency department.”
--
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.