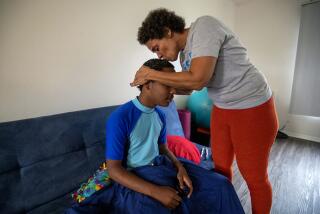
A breakdown next door
- Share via
A
week ago Sunday, my husband and I spent the day knocking on doors and apologizing to our neighbors.
The night before, I had called 911 for an ambulance to transport our schizophrenic son to the hospital. Again. He didn’t want to go. Again.
He pushed me away from the phone and began raging at the 911 operator as we ran from the house. Almost immediately, there were two police officers on our front lawn. Our son stood in the kitchen, shouting at them to leave. They called for backup; four, then six officers on the front lawn. Patrol cars blocked traffic on the narrow street in front of our North Hollywood home. Our son called 911 again, screaming, shouting: “There are police officers here, make them go away!”
I tried to reason with the police: “We just need an ambulance.” But by this time, it was out of my hands.
Two more officers arrived and ordered me to the edge of my yard, away from the view of the kitchen window. Another pair of officers pulled me aside, asking me what had happened. “I called an ambulance,” I said, watching two more officers stride across the brown lawn. One, her dark hair pulled back in a tight bun, carried a shotgun wrapped in what looked like bright green cloth. She paused to smile at me, “Just bean bags, not lethal,” and stood at the ready under the mulberry tree.
We could see our son pacing back and forth in the kitchen, his long hair flying. By now there were more than a dozen police officers on the front lawn. They asked if there was an entrance in the rear. We directed them to the back patio, warning them not to trip over our elderly dog asleep in the breezeway.
We have been through this so many times before. We’ve heard all the arguments from well-meaning people about how Big Pharma is bad and that we should try diet or therapy or other things. But from here in the mental health trenches, the reality is very simple. When our son takes his prescribed psychotropic medications, no one would ever suspect the depth of his illness. But when he is off his meds, he is unable to eat, sleep, bathe or make sense. He is overtaken by delusions: The Red Hot Chili Peppers have used his name without his permission; sitting on his guitar case is the same as playing the guitar. He regularly becomes violent when we suggest he should resume his medication or stop smoking pot.
Oh, yes, pot. Research has shown that marijuana use is toxic to schizophrenics, that it exacerbates psychosis. It was an astounding surprise to me that marijuana could be so dangerous. But it sets our son into a blink-of-an-eye downward spiral that starts with the idea that he should set his prescribed medications aside. He then starts dressing in rags and refusing to bathe. He becomes increasingly incoherent -- responding, as one doctor put it -- to “unseen stimuli.” The cycle generally ends with an involuntary hospitalization. His newly minted “medical marijuana” card has complicated everything.
As more and more officers arrived, my cellphone rang. Our son. I held the phone away from my ear so my husband and I could both hear it. “How could you do this to me? I hate you! Stop being my mom!”
There was still no ambulance, but now officers had pulled the screen from the dining room window and climbed inside. There were shouts, thumping and thrashing as they tackled our son. Four officers carried him down the front steps, howling and spitting. They pulled a hood over his head, handcuffed him, hobbled him with an ankle leash of thick webbed nylon and set him on the curb.
Finally the ambulance arrived. Firefighters in yellow reflective coats stood watch as a pair of paramedics struggled to place monitors and a blood pressure cuff on our son.
“I need help. I need to get to the hospital!” he wailed as they muscled past his resistance to get a pulse.
The ambulance pulled away from the curb and a police officer gave us directions to a local hospital emergency room where he was to be evaluated.
Our son had his first psychotic break in his freshman year of college, and he has been in and out of hospitals ever since. It is always the same. We follow the ambulance, wait to see him admitted or transferred, worry over him.
This is his sixth hospitalization in less than a year and comes just eight days after his previous discharge. At 24, he is no longer covered by our insurance, but this may be to his advantage. We’ve been told he can now access services through the Los Angeles County Department of Mental Health, and we’re hopeful there may be more options for him now.
With severe mental illness, nothing is certain. Except that we owed our neighbors an apology for the disruption.
It felt odd, standing on doorsteps of neighbors we hardly know, telling them we were sorry. All those who answered their doors were quick to wave our apology away: “No, no, no problem.”
For all of them, including those who did not answer, we left a note.
We were hesitant to share our story with our neighbors, but giving up the pretense of privacy offers us a chance to be free of the burden and shame of this mystifying illness.
By being open, we may even be able to help someone. Our letter to our neighbors included information about NAMI, the National Alliance on Mental Illness, an all-volunteer grass-roots organization dedicated to helping individuals and families living with mental illness.
NAMI has helped us understand we are not alone. Millions of Americans, an estimated one in five families (22%), are living with mental illness. As a matter of fact, two of the responding police officers on Saturday night, including the blond female officer assigned to keep me company, told us that they too had family members with serious mental illness.
Our odyssey has taught us many things, but none more important than these: Mental illness is no one’s fault. Treatment works. There is hope.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.