A child’s illness spurs action on marrow transplants
- Share via
When Mina and Sam Chamberlin fell in love, they knew they might have to overcome some cultural barriers to make their interracial marriage work.
But they never imagined that their South Asian and white genetic backgrounds would in any way put their children in potential harm’s way.
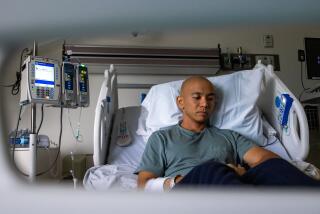
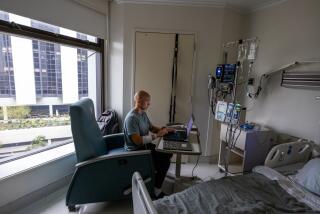
Then in September, the couple’s 4-year old daughter, Maya, was diagnosed with a rare blood disease known as HLH. Only a bone marrow transplant could save her life.
That would be a nightmare for any parent. But the Chamberlins’ quest for a bone marrow donor is made especially difficult because their daughter is of mixed races.
“It was so devastating,” said Mina Chamberlin, a medical doctor who lives in Torrance. “The probability of finding a match is very, very low. I can say it would be a miracle if we could find a perfect match.”
People of multiracial backgrounds make up one of the fastest growing minorities in the country. In Southern California, they represent the new face of an expanding melting pot.
It is not known how many racially mixed patients in the country are on waiting lists for bone marrow transplants. But an estimated 6,000 people search the bone marrow registry every day for a match, and about 4,000 transplants are performed every year.
Of the 7 million potential bone marrow donors nationwide, about 28% are from ethnic minorities, according to the National Marrow Donor Program, a Minneapolis-based nonprofit that provides assistance to transplant patients. Only about 7% of donors are of Asian and Pacific Islander descent; people of mixed race represent a little more than 3% of volunteers.
The pool of potentially mixed-race donors is made even more difficult because blood relatives of patients often don’t qualify, and trying to find a volunteer with the right racial combination can be extremely tough, experts said. Marrow transplants are also more complex than those involving organs.
“With organs you can be a partial match and it’ll still be successful,” said Jill Kendall, program director for the Be the Match donor registry program at City of Hope hospital in Los Angeles. “But bone marrow produces the white blood cells which is [part of] your immune system. It has to be a very close match if not identical match so your body doesn’t reject it.”
‘Worst nightmare’
The Chamberlins’ daughter was diagnosed in September. The family has been shuttling from one hospital to another all around Los Angeles ever since.
“I felt like I was going to lose her any minute when she was in the ICU, with breathing tubes in her mouth and IV medications hanging all around her,” said Mina, 40, who is now with Maya at a Cincinnati hospital that specializes in transplants. “It is a mother’s worst nightmare to see her child suffer like that. There is no greater pain.”
Despite the emotional toll Maya’s illness has taken on the family, her parents are grateful that they have good insurance through her father, an engineer with a telecommunications company. Mina is on leave as a fellow at the Harbor-UCLA Medical Center division of nephrology.
They are still hoping that a full donor will turn up before Maya must go ahead with partially matched marrow, which greatly diminishes her odds. Mina said her daughter seems to understand her dilemma.
“I was packing the other day and she said something extremely profound,” Mina said. “She said, ‘God can make me feel better if he wants to.’ That was the biggest evidence that she has some understanding of what’s going on.”
Mina was born in India and came to the United States when she was 14. She met her husband, Sam, who is white, at a friend’s engagement party in Chicago, where she was a medical student. They married in 2001.
“I am the first one in my family to have married out of race,” Mina said. “I knew he was the guy when my family didn’t scare him away.”
The Chamberlins have two children, Maya and Jaden, 2.
Initially, Maya’s little brother was believed to be her best hope for a bone marrow match. The Chamberlins were desperate after watching their daughter endure chemotherapy and endless steroid and seizure medications.
But there is only a 25% to 30% chance that a sibling will be a good match in such cases, and their hopes were soon dashed.
The severity of Maya’s illness means she might have to go ahead with a transplant from a partially matching donor, her parents said. It may be her best bet, given the odds of finding a more compatible donor.
“Ideally you want the full match,” Mina said. “But her status is urgent, she has a high risk for relapse. Hopefully we can find something by January.”
No matter what happens, the Chamberlins are on a crusade. They have held donor drives at temples, churches, restaurants, universities and anywhere else where there is a gathering of people.
“Our new goal in life, once this is over, is to make sure there are enough donors in the registry so nobody has to succumb to this disease,” Mina said. “I don’t think any kid, or adult, should have to die because there isn’t a donor.”
‘Totally painless’
Cultural barriers and a lack of understanding about the safety of the transplant process continue to make donor recruitment an uphill battle in some minority communities, particularly among Asians, experts say.
Many Asian immigrants tend to frown on the idea of giving away part of the body because of misconceptions that donating marrow could make people sick or infertile or even take away part of the spirit.
“People are willing to give a unit of blood because they know it will replenish itself, but they don’t see the connection with bone marrow,” Sharon Sugiyama, project director for Asians for Miracle Marrow Matches, or A3M, a Los Angeles-based nonprofit that works to expand the donor pool among minority populations. “But it is replenished and very little is taken.”
The good news for potential donors is that the testing and donation process have become less invasive. Once a donor is chosen as a match, he or she could be asked to donate stem cells or marrow.
The former works more like a plasma donation, for which blood is drawn, separated and returned to the body. A marrow donation is a surgical procedure that requires the drawing of marrow fluid from the back of the pelvic bone.
“They all warned me about possible discomforts,” said Ka Tong Gaw of Upland, who is ethnic Chinese and donated his stem cells to a teenager. “For me, it was a totally painless experience.”
The biggest reward for Gaw, 67, is that the Chinese American boy he helped bring back from the brink of death eight years ago is now in college, and they have kept in touch.
“It’s really worthwhile,” Gaw said. “It’s so little on my part, and it can actually save a life.”
This kind of success story keeps hope alive for people like Krissy Kobata. Half Japanese American, half white, Kobata has been waiting nearly two years for a donor.
Kobata, 27, who grew up in West Los Angeles, was diagnosed last April with Myelodysplastic Syndrome, or MDS, which means her bone marrow stopped producing healthy cells. Only a bone marrow transplant can reverse the condition.
Her older brother was her best shot for a match, but it didn’t happen.
Despite having a large and supportive extended family, most of them are not “hapas,” or people of mixed backgrounds. Their chances of helping her are as slim as the chances of people in the general population.
The doctors ran Kobata’s information against international databases in Japan, China, Korea and Europe. Still, nothing came up.
“I know someone who has been looking for 10 years,” Kobata said. “I don’t want to be looking for 10 years. It’s a fear I have for sure. But you try to stay positive and keep registering people. That’s all you can do.”