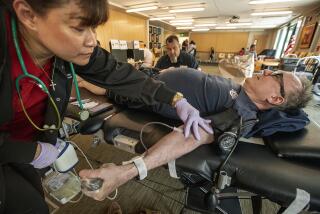
Federal health panel considers allowing gay men to donate blood
- Share via
Reporting from Washington — A federal health panel is considering changes to a long-standing ban on blood donations by most gay men amid a growing body of evidence that the sharpest restrictions may no longer be necessary.
Some lawmakers are calling for a fresh look at the policy, and key gay advocacy groups and organizations representing hemophiliacs and other heavy users of blood products also have narrowed their differences over the need to adjust rules for donors.
At issue in a two-day hearing starting Thursday by the Department of Health and Human Services’ Advisory Committee on Blood Safety and Availability will be the quarter-century-old donor policy, which bars any man who has had sex even once with another man since 1977 from ever giving blood.
The restrictions were put in place in the early days of the HIV- AIDS crisis after it became clear that gay men were at increased risk of getting and transmitting HIV and other infectious diseases.
The Food and Drug Administration estimates that gay men likely to donate blood have an HIV infection rate 15 times higher than the general population.
Pressure for a review of the policy has been building for several years. The push has been driven by improvements in testing, which can detect HIV in the blood within two weeks of a person having been infected.
There were nine known cases of HIV having been transmitted via blood products between 1994 and 2002, and none, in tens of millions of transfusions, between 2002 and 2007, the last year for which the Centers for Disease Control and Prevention has complete data.
In 2006, the American Red Cross and two other blood bank groups, which among them collect almost all of the blood in the U.S., recommended permitting gay men to donate blood if they abstained from sex for one year.
Two years later, the American Medical Assn. also urged an end to the broad ban, though it advised a five-year waiting period before donation.
In December, 10 House members asked the FDA to revisit the issue, and three months later, so did a group of senators led by Massachusetts Democrat John F. Kerry.
Kerry’s letter said there was “a clear and unscientific double standard” in the current policy because behavior that puts heterosexuals at higher risk for HIV — such as unprotected sex with an intravenous drug user, a person with HIV or a prostitute — warrants only a one-year deferral from donation.
The FDA last examined blood donation protocols in 2006, but left current restrictions in place.
The Gay Men’s Health Crisis, which issued a report this year calling for a review of the donor policy, said it was not seeking a complete elimination of the ban, but a fine-tuning that would factor in the risks posed by individuals, not an entire class of people.
“We’re not looking for a complete repeal or an overhaul. We’re looking for a revision that will allow some gay men to become donors,” said Nathan Schaefer, director of public policy for the New York-based Gay Men’s Health Crisis.
At the other end of the blood supply spectrum, advocates for hemophiliacs and other heavy users of donated blood, who have opposed previous efforts to soften donor restrictions, acknowledge that the current broad ban may no longer be scientifically supported. But they urge further study before making any changes.
The advisory committee is expected to make nonbinding recommendations to Health and Human Services Secretary Kathleen Sebelius and FDA leadership, FDA spokeswoman Shelly Burgess said.
“Change is coming,” said Mark Skinner, president of the World Federation of Hemophilia.
The question is “what comes first — policy revision or additional research,” Skinner said, adding he believes that more study is needed to figure out the proper deferral period for gay men.
In addition to dealing with the risk of HIV, Skinner said health authorities needed to figure out whether gay men or any other potential donor group was at increased risk of transmitting “the next HIV.”
AABB, a blood bank trade association, last year identified 68 pathogens that could potentially threaten the blood supply.
But Michael Busch, director of the Blood Systems Research Institute in San Francisco, said the newer pathogens that worried blood safety experts, such as dengue fever, SARS and the XMRV retrovirus, “have not been sexually transmissible.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.