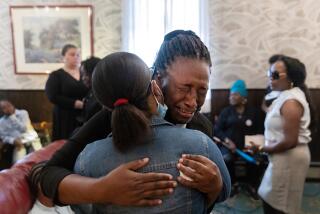Coronavirus poses added challenges for hospital patients who are deaf or hard of hearing
- Share via
A nurse at Health Central Hospital in Ocoee, Fla., activated a video screen with an internet link to connect Jennylee Bruno to an American sign language interpreter. Minutes later, Bruno’s worst fear was confirmed: The shortness of breath, sense of fire in her lungs, and dry cough were a case of the coronavirus.
The doctor told Bruno, a deaf author and mother of five, that they could only help ease the pain. Then the video feed froze, unfroze, and froze again. Bruno sobbed from her bed.
“I felt like they were giving me a death sentence,” she said of that day in March. “I wanted to ask, am I going to die, what can we do, is there a cure, what about medications, what’s the plan?”
As some hospitals are overwhelmed with coronavirus cases, deaf and hard of hearing patients in California and across the country face greater barriers accessing accommodations that allow them to understand what doctors and nurses are saying.
The increased use of masks has hindered those who rely on lip reading and facial expressions to communicate. Many hospitals have restricted interpreters and visitors, and are instead offering patients video conferencing with remote interpreters, an aid that may run into technical issues.
“The calls and emails that we have received reflect deaf and hard of hearing people being alone in hospitals without ways to communicate with the hospital doctors or staff or even to make calls to family outside of the hospital,” wrote Howard A. Rosenblum, the CEO of the National Assn. of the Deaf, in an email.
Nearly 4 percent of the U.S. population identifies as either deaf or having difficulty hearing. Under the Americans with Disabilities Act, hospitals must facilitate effective communication with services like in-person or video remote interpreting, captioning, written notes or speech-to-text apps.
Public health officials reported 399 new coronavirus infections, bringing the county’s total to 10,854.
Prior to the pandemic, many deaf patients complained about the use of video interpreting in emergency rooms. The feed can be blurry or freeze, and patients may be unable to focus on a small screen in a crowded room. Nurses may also not know how to operate the equipment.
“When you have a new staff member who hasn’t been able to be trained to use the system, they’ll be overlooked,” said Kavita Pipalia, the president of the California Assn. for the Deaf. “The one who ends up suffering is the patient.”
Bruno spent almost two weeks isolated in a coronavirus ward. The 51-year-old can read lips, but everyone around her wore a mask.
Nurses during the day wrote short notes to her on a white board. The video interpreting feed would freeze constantly, so staff gradually stopped using it, she said.
“There’s a lot of people there and they have no time to wait for an interpreter,” said Bruno.
A study of COVID-19 patients and the people they likely infected suggests the coronavirus can spread for more than two days before symptoms appear.
Orlando Health — Health Central Hospital noted that all patients who require communication assistance are provided access to qualified interpreters. “When infection prevention protocols prohibit person to person contact, interpreters are made available to patients via phone or video remote,” it said in a statement.
The National Assn. of the Deaf and other advocates have published guidelines on communication access in hospitals during the pandemic, advising patients to bring their own tools, like a printed page that says they are deaf, hard of hearing or deaf-blind, or to download video interpreting or speech-to-text smartphone apps.
Hospitals, the guidance said, should at least have white boards or yellow pads on hand. For some deaf-blind patients, tracing alphabetic letters on palms with a finger may be an option.
In Austin, Texas, Lore Kinast, 51, has a plan should she, her husband or their 21-year-old daughter — all of whom are deaf — go to a hospital with coronavirus symptoms.
Lip reading would be impossible with masks. Passing a paper back and forth requires close proximity. So they would bring an iPad and type in extra-large font to communicate with staff from a safe distance.
Kinast, who works at the National Deaf Center on Postsecondary Outcomes in Austin, hopes there would be a white board for nurses to respond back but recognizes resources might be stretched.
“Most people don’t know how to deal with deaf people on a good day,” said Kinast. “With so much turnover with staff at facilities, it may be that they don’t know what to do if a deaf person arrives on scene.”
Ellen King, a severely hard of hearing 66-year-old resident of Northern California, has also given a potential hospital visit some thought. King lip reads and uses a hearing dog at her job at a psychiatric hospital. She might not bring her hearing aids if she were to be admitted to a hospital for fear of losing them.
King would plan to show nurses a handout with small health-related graphics, including a pain scale, that she could point to.
“I may be considered not credible,” she said. “If I am less than fully conscious and have no hearing aids, I’m at a very big disadvantage because I might not be able to follow instructions.”
I am the mother of a 20-month-old with a terminal disease.
Some patients, like Jennifer Dotson of Puyallup, Wash., have commended efforts to find accommodations. Dotson, 44, spent several nights at the University of Washington Medical Center in Seattle in March after experiencing shortness of breath.
Dotson has severe hearing loss, so the hospital initially allowed her husband to stay with her so that he could speak in a loud voice and help her understand what was happening.
Once she was diagnosed with the virus, she said, staff limited their time in her room due to a shortage of masks. Doctors communicated with her over FaceTime, positioning themselves close to the camera so she could watch their lips.
“They still had to really simplify their words/information they were sharing for me to figure out what they were saying, but this solution was the best situation to get their point across to me,” Dotson wrote in an email.
Interpreters allowed on site face challenges too because masks hide their expressions. Demand for masks with a transparent window has increased, according to Anne McIntosh, the president of Safe’N’Clear, a company that in recent years partnered with the manufacturer Prestige Ameritech to develop a mask of this kind.
Some interpreting agencies say that interpreters must supply their own protective gear. Patricia Hughes, the CEO of Lifesigns, an interpreting agency that operates in Southern California, said that hospitals are not making protective equipment available.
Acquiring equipment for interpreters has been challenging, said Joshua Pennise, who oversees on-site and video remote sign languages interpreting for Sorenson Communications, an agency that employs more than 4,000 interpreters. The company has told interpreters they will be reimbursed for equipment they purchase.
“They are able to opt out no penalty on any specific assignment,” said Pennise.
But for some, a sense of responsibility outweighs worry.
When she receives an assignment, Lynne Martirano, a freelance interpreter in her early 60s in Putnam County, N.Y., evaluates what she knows about the facility and her own health.
‘I may be considered not credible. If I am less than fully conscious and have no hearing aids, I’m at a very big disadvantage because I might not be able to follow instructions.’
— Ellen King, Northern California resident
She recently interpreted for a pregnant deaf woman who was worried about giving birth while communicating with a remote interpreter.
“I consider not working because of this virus every day,” said Martirano. “I consider it all the time but am aware this young woman … is going to go into labor at some point. What if I were her going into that?”
The same stands true for Keimi Malave, a freelance interpreter for a hospital in Manhattan. Malave accepts assignments for patients who don’t have the technology for remote interpreting and can access masks, visors and gloves that are kept locked up at the hospital.
“They’ve called me quite a few times to come to the hospital because other interpreters have refused to go in,” she said. “Even though I don’t want to put myself in that position, who does? Somebody has to do it, and if it’s not me, who is it going to be?”
Bears, bobcats and other critters are roaming free in California’s most popular national park, closed to visitors since March 20
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.