This year’s Ramadan bears an extra test for Muslim healthcare workers on the coronavirus front lines

- Share via
When Dr. Imran Siddiqui went to bed Thursday night, he set the alarm for 4:30 a.m.
As the director for both the Desert Valley Medical Group in Victorville and a nearby nursing home, Siddiqui’s days have been long and stressful since the COVID-19 pandemic began its deadly assault on California more than six weeks ago. But it’s faith as much as duty that will require him to rise early each morning for the next month.
Because in addition to being a doctor, Siddiqui is a devout Muslim, and like thousands of other faithful first responders, he will be waking before dawn for a large breakfast, then going without food and water throughout the daylight hours of Ramadan, the Islamic month of fasting that ends May 23.
“My weakness in Ramadan is not food, it’s not water,” Siddiqui said. “It’s coffee. I need to have a cup of coffee in the morning. Or two cups.”
The fast is obligatory, one of the five pillars of Islam. Yet for frontline healthcare workers, observing it could be extra difficult this year. The novel coronavirus has overwhelmed emergency rooms and intensive care units, infecting more than 9,000 U.S. healthcare providers and killing more than two dozen, according to a study released earlier this month by the Centers for Disease Control and Prevention.
Uneven reporting across the country, the CDC added, means the real numbers are almost certainly much higher.
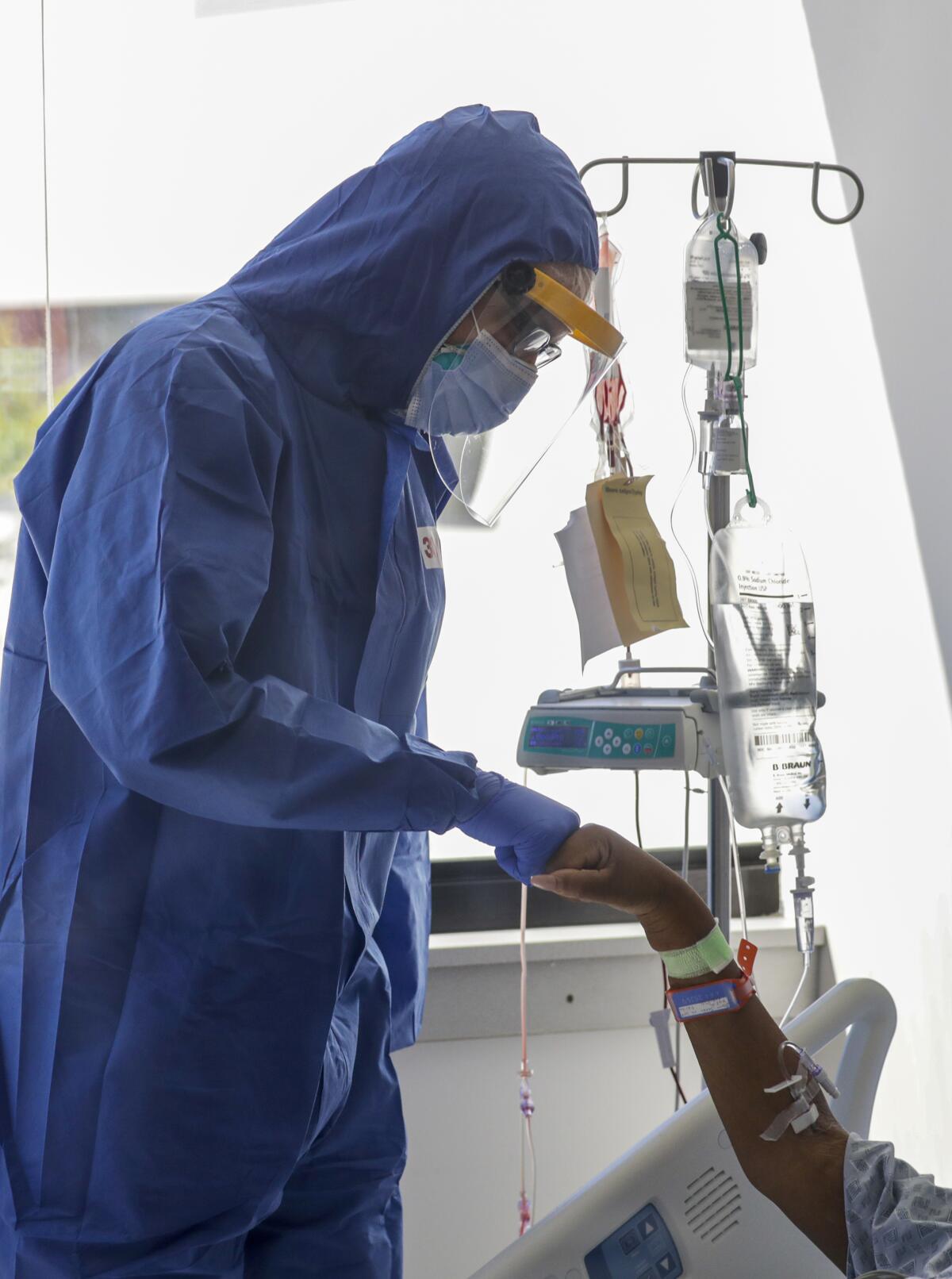
And that has some doctors and Islamic scholars questioning whether working long hours in a challenging environment without food and water is wise.
“This has been a discussion,” said Dr. Faisal Qazi, a neurologist and an assistant professor at Western University and UC Riverside. “In Ramadan fasting, you’re not hydrated, so it’s different than other forms of intermittent fasting.”
The use of personal protective equipment, including masks, could increase the chances of dehydration. Religious officials in the United Arab Emirates have said that those treating COVID-19 patients there are exempt from fasting, but most Islamic leaders in the United States insist healthy caregivers here should have little problem fasting.
“This COVID-19 situation doesn’t really change that normality,” said Dr. Aasim I. Padela, an emergency medicine physician at the University of Chicago Medical Center and director of the Initiative on Islam and Medicine. “Now what has been a concern is that frontline workers like me who are fasting and making very critical decisions or surgeons who are making critical decisions … people are saying it might be more difficult, I might become more dehydrated because I have to wear all these extra layers of protection.
“That’s a credible concern although there’s no data that I know of to show that.”

In any case, Islamic law allows followers to opt out of a fast under certain circumstances, such as illness or other hardship, and make it up later in the year. The strain of working in a COVID-19 ward would certainly qualify for an exemption.
“Fasting is hard,” said Muzammil Siddiqi, religious director for the Islamic Society of Orange County. “But some things are much harder. If it is for their work, for their health, that will be an acceptable excuse.”
Dr. Muna Beg won’t be looking for an out. An ICU doctor who treats COVID-19 patients at two hospitals in Alameda County, Beg has been observing the Ramadan fast since she was 7. And while the first few days are always tough, after that “for Muslims in Ramadan, it’s Zen-like,” she said. “It’s a very personal experience.”
“I don’t have a clinical study to support this, but I can definitely attest to the fact that if you’re in a place where I’ve eliminated food or whatever my crutch might be, I find that hypersense of awareness does make me more present.”
Siddiqui agrees.
“You are more and more focused. You don’t waste time,” he said. “I feel like our religion is a boost. I don’t know if it’s a spiritual thing or if it’s something in the air, but it’s a little bit energizing.”
Muslim medical personnel have been on the front lines of the fight against COVID-19 all over the world. The first four doctors to die from the virus in England were Muslim immigrants, and in New York City, a hotbed of the coronavirus outbreak in the United States, more than 10% of the pharmacists, clinical laboratory technicians and doctors are Muslim, according to the Institute for Social Policy and Understanding.
The percentage is even greater in Michigan where healthcare workers have paid a high price with more than a thousand employees of the Henry Ford Health System testing positive.
“The first two weeks in April were as challenging as it’s been,” said Dr. Mohammed Rehman, a neurologist who has seen his time in the ICU nearly double this month. “But I also saw a lot of people come together during this.”
Rehman also sees the Ramadan fast as something that will strengthen, not weaken, him.
“It was meant to reconnect you back with your faith, it’s not meant to put a burden on that you can’t even function anymore,” he said.

The greater challenge could center on the five prayers — at dawn, midday, afternoon, sunset and night — that Muslims are called to make each day. Since it’s inconvenient to bring a prayer rug into a hospital now and inappropriate for a doctor to strip out of their PPE, Padela will substitute a towel or clean sheet for a rug and pray in his protective clothing and mask.
Beg, the Alameda County ICU doctor, will sometimes use a chair rather than risk contaminating her PPE by praying on the ground.
“The whole world is stretching their PPE further than I wish it was,” she said. And if she can’t leave a patient to pray at the right time, she’ll combine two prayers when she can get away.
“The way my mom always taught me about Islam is God is not cruel,” she said. “So whatever situation you’re in, you should be able to be adaptable.”
COVID-19 has put limits on that though. In normal times, many Muslims would gather with family or in mosques for the evening prayer, but social distancing regulations have forced mosques to close, leaving the faithful to pray at home.
“I can’t even visit my parents now,” Rehman said. “I can’t go anywhere. So the community events, I would say, I will miss this year quite a bit.”
The coronavirus is not just punishing those who are infected and those who are treating them. Siddiqui said it’s also punishing the families. Each night he has to strip in the garage and put his medical clothes in the washer, then take a shower before he can greet his wife. And whatever plans they have for the evening are often interrupted by calls from the hospital or nursing home.
“‘Doctor, this patient’s coughing, he’s feverish. Should we test for COVID? What do you want us to do?’” Siddiqui said, imitating the kinds of calls that have become a nightly routine.
“It’s not just coming to work. The mental toll that this has taken on me and my colleagues is unprecedented. I feel like just, you know, crying almost.”
For the next 30 days, he’ll be handling that stress with both a renewed faith and an empty stomach.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.














