Institutional racism, inequity fuel high minority death toll from coronavirus, L.A. officials say
- Share via
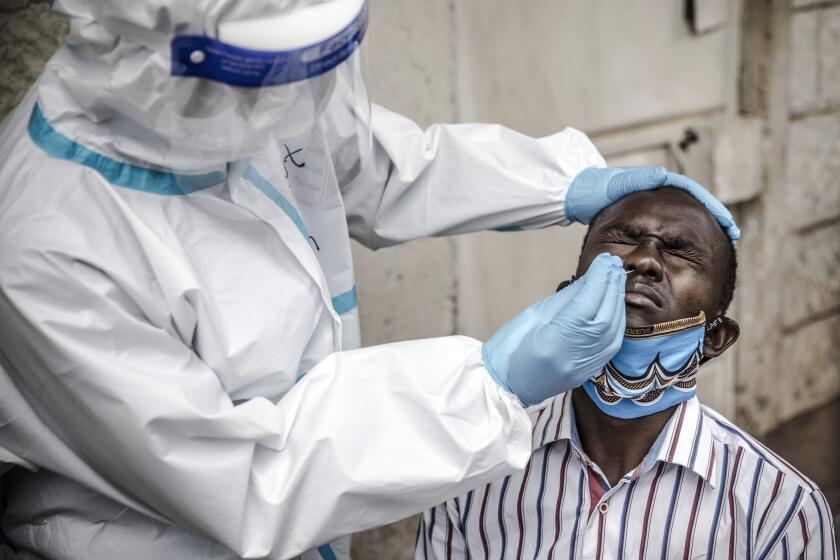
Extensive racial and economic disparities are emerging among victims of the coronavirus in Los Angeles County, and officials attribute the trend in part to systemic inequities and institutional racism.
Officials reported a rate of 89 deaths per 100,000 people among native Hawaiian and Pacific Islanders and 18 per 100,000 among black people. The rate was 15.5 for Latinos, 12 for Asians and nine for white people.
“These rates are significantly higher than the mortality rate for other races and ethnicities, and although some of the numbers are small, they are still very concerning,” Los Angeles County Public Health Director Barbara Ferrer said Friday at a news briefing.
People who live in areas with high poverty rates have nearly four times as many deaths from COVID-19 — 29 deaths per 100,000 people, compared with eight per 100,000 people in communities with low poverty rates, she said.
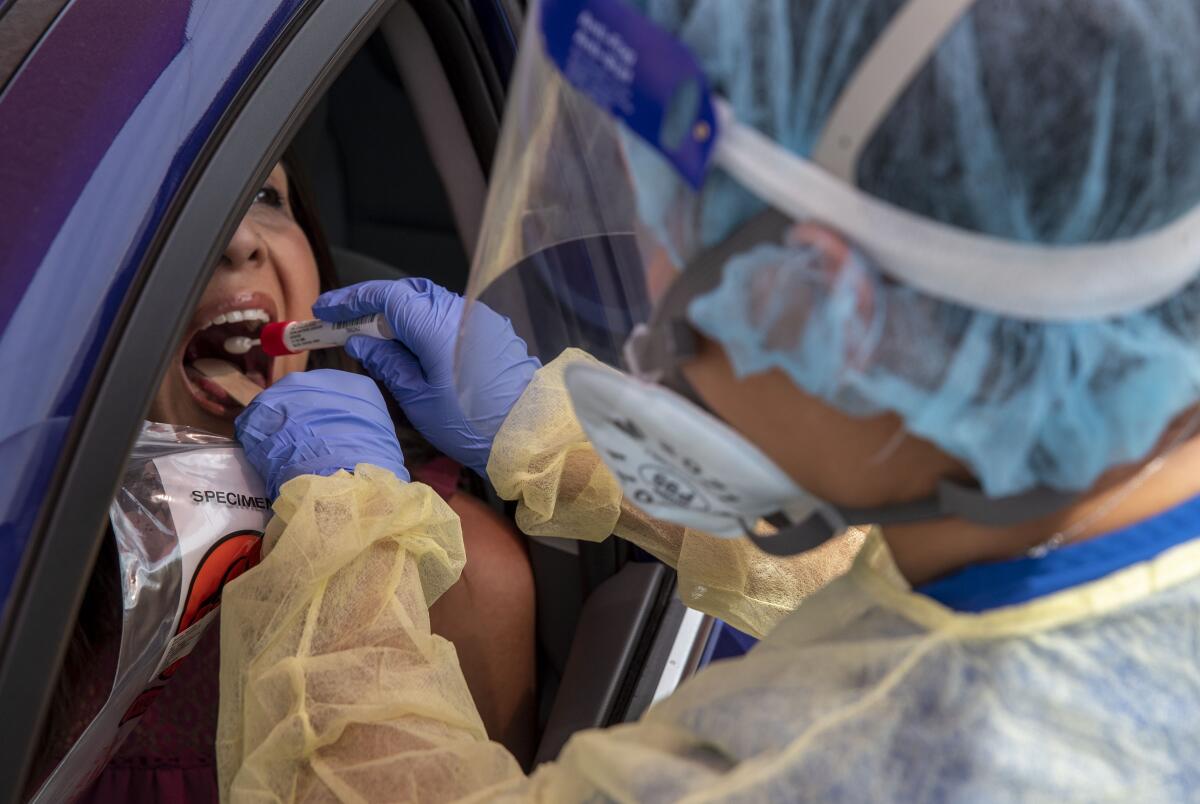
Public health officials have been working to address the disparities by opening more testing sites in hard-hit communities, participating in virtual town halls, releasing public service announcements, and ensuring that more racial and ethnic minorities are sampled in a new round of serology testing researchers are undertaking, she said.
Wealthy areas saw an early surge in coronavirus cases in L.A. County. More accessible testing and international travel provide a likely explanation.
“Systematic injustices including discriminatory policies and institutional racism have led to the unequal distribution of wealth, resources and opportunities, and this is in fact contributing to the staggering disproportionality we see in the outcomes around COVID-19,” Ferrer said. “Only through a collaborative approach will we see improvements for our tremendously impacted communities.”
Of the 1,352 L.A. County residents who had died as of Friday for which race and ethnicity data were available, 39% were Latino, 29% were white, 18% were Asian, 12% were black, 1% were Native American or Pacific Islander, and 1% identified as another race.
Ferrer noted that a recent analysis by the Advancement Project of California “noted similarly concerning findings.”
That report found that the largest number of cases was initially reported in wealthier communities of Los Angeles, but that cases are now centered in areas with higher levels of poverty, including South and Southeast L.A., communities in the San Fernando Valley and in Pomona, Santa Clarita, Palmdale and Lancaster. It also found that case trajectories have been more steady in white communities but have grown more steeply in communities of color starting in mid-April.
To close the gap, officials must work together to improve access to testing and coordinate care and appropriate communications, Ferrer said.
Many countries saw the coronavirus as a ‘rich man’s disease’ imported by overseas travelers. It has since hit marginalized groups the hardest.
Black and Latino Californians ages 18 to 64 are dying more frequently of COVID-19 than their white and Asian counterparts relative to their share of the population, a Los Angeles Times analysis of state health department data conducted in late April found.
When accounting for each group’s percentage of the population, blacks and Latinos under the age of 65 had a higher share of fatalities than even older blacks and Latinos. The trend is particularly noticeable among those ages 18 to 49, The Times’ analysis found.
During a four-day period, a team of community workers and volunteers with San Francisco’s Latino Task Force and infectious disease specialists at UC San Francisco tested 4,160 residents and workers for the novel coronavirus in a census tract of the city’s Mission District.
They found that 2.1% of those tested were positive; yet it was the details of the group’s demographics that were more revealing.
Although Latinos made up 44% of those tested, they accounted for more than 99% of the positive COVID-19 cases. In addition, 40% of those tested earned less than $50,000 per year. That group accounted for nearly 90% of the positive cases.
More than half of those who tested positive — 53% — had no symptoms of the illness.
Times staff writer Susanne Rust contributed to this report.

More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.