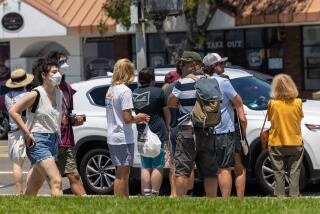California desperate for signs of turnaround after stunning coronavirus setbacks

- Share via
SAN FRANCISCO — Coronavirus cases surging. Hospitals filling up. Reopening of schools postponed. Battles over wearing masks in public intensifying.
July has brought a month of grim COVID-19 headlines for California, with a state once seen as a model of prevention enduring a new surge in cases as the economy rapidly reopened.
But will July end with more bad news or some tentative signs that the efforts to slow infections by closing down some businesses and institutions might be paying off?
Health officials are anxious for more signs of the latter, especially amid indications that other hot-spot states may be beginning to plateau.
“We are at the phase of just beginning to flatten the curve, albeit at a higher level than before,” Dr. Robert Kim-Farley, medical epidemiologist and infectious disease expert at the UCLA Fielding School of Public Health, said Sunday of California. “I would anticipate — depending upon the cooperation of the public — we would start seeing cases beginning to go down in the next couple of weeks.”
Kim-Farley said Sunday that, based on the information available now, it won’t be necessary to close more businesses and, in perhaps two to three weeks, parts of California might be at a point where some businesses can be reopened in a slow, phased manner.
The state’s hospital system has not been broadly overwhelmed in this latest surge, Kim-Farley said. And where there was an overwhelmed hospital system in a local hot spot, the issue in some cases was a shortage of medical staffing, rather than physical beds. Some of that has been relieved by transferring patients to other nearby counties, and by federal doctors and nurses being assigned to hospitals in the Central Valley and Southern California, he said.
Other hot-spot states are also starting to show signs of improvement. The rate at which coronavirus test results are coming back positive is starting to decline in Arizona and Texas, although “it’s a little bit more of a mixed bag in Florida and California,” Dr. Scott Gottlieb, former head of the Food and Drug Administration, said on CBS’ ”Face the Nation” on Sunday.
“We’re going to have to wait another week to see how those states net out. But there are unmistakable signs that the epidemic seems to be slowing in these states,” Gottlieb said. But he warned that the pandemic seemed to be heating up in other states in the South, the Midwest and the District of Columbia.
In Arizona, the seven-day positivity rate — the percentage of people who test positive for the virus of all who have been tested — was 22%, down from 28% in mid-July, according to the COVID Tracking Project. A Los Angeles Times analysis has found that California’s seven-day positivity rate has generally stayed between 7% and 8% since July 5. That rate is worse than it was in late May, when it was around 4%, officials note, but at least the rate is no longer on a sustained upward trajectory as it was in June. A higher positivity rate indicates the disease’s spread is worsening.
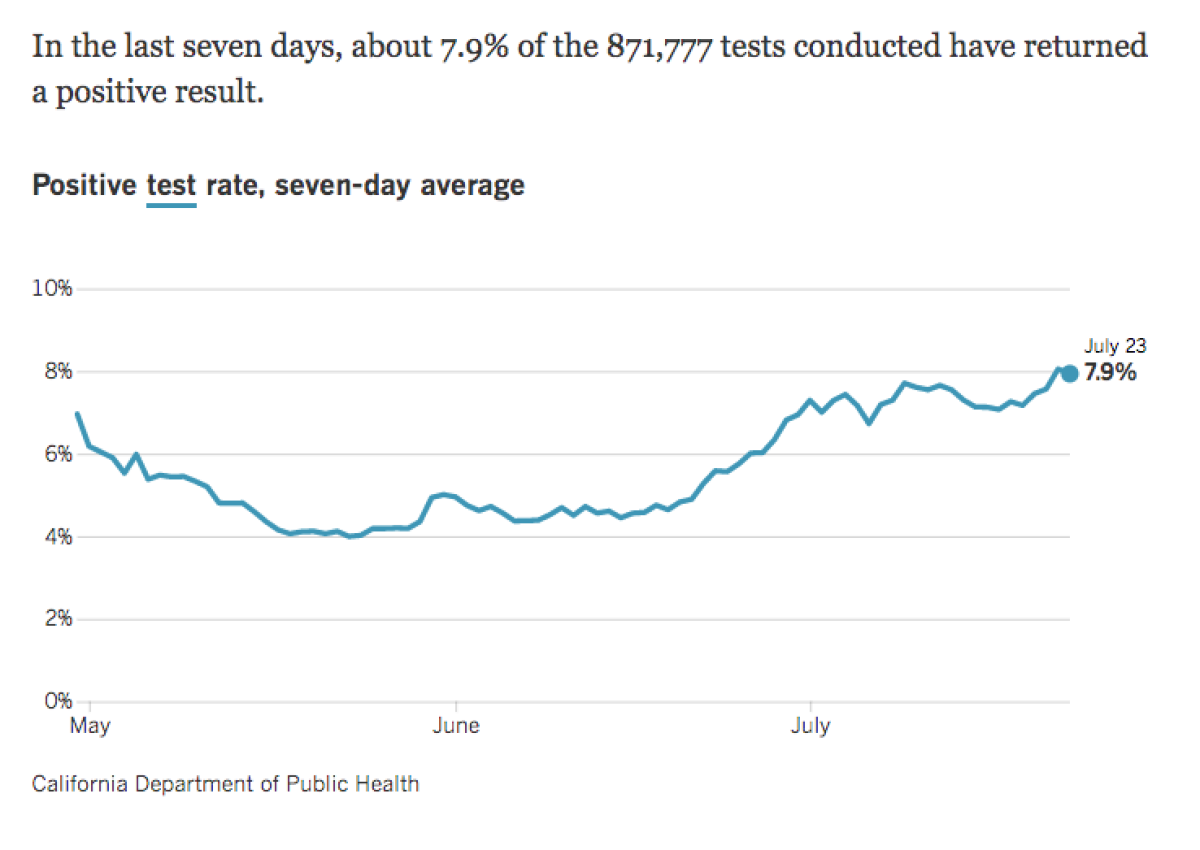
In L.A. County, the positivity rate has remained stable at about 8.5% since July 1. It was about 4% in late May. “The fact that we’re leveling off is encouraging,” said Barbara Ferrer, the L.A. County director of public health, last week. “We’d like to see it drop again.”
There remain worrisome numbers statewide. The effective transmission rate of the coronavirus across California is hovering around 1.1 to 1.3, meaning each person infected in the state, on average, transmits the illness to 1.1 to 1.3 people — setting the stage for worsening disease transmission, according to data shared Friday by the secretary of the California Health and Human Services Agency, Dr. Mark Ghaly.
The transmission rate is now worse in Northern and Central California than in much of Southern California, according to models posted by state public health officials. Spread of COVID-19 is probably stable in L.A., San Diego, Orange, Riverside, San Bernardino and Imperial counties, but probably increasing in Ventura County, the San Francisco Bay Area and the Central Valley.
Dr. George Rutherford, a UC San Francisco epidemiologist and infectious diseases expert, presented data Friday at a town hall meeting that indicated the transmission rate in San Francisco, Santa Clara, Contra Costa and San Mateo counties was around 1.3 or 1.4. “This is far, far, far from satisfactory,” Rutherford said.
There are also some concerns about a shortage of a key antiviral drug — remdesivir — that has been used to shorten patients’ recovery time. Bay Area “hospitals & many more around the country are beginning to run out of #remdesivir,” Dr. Peter Chin-Hong, professor of medicine and an infectious disease specialist at UC San Francisco, tweeted.
Last week, California on Wednesday and Thursday recorded more than 150 deaths on each of those days — the worst single-day fatality numbers since the pandemic began. Deaths tend to be a lagging indicator of an outbreak, and experts say they believe the deaths are tied to infections that probably occurred in June when people left their homes in droves and went back to old pre-COVID activities such as parties, or worked in places that had failed to institute new health and safety precautions.
Despite the surge, California has seen far fewer deaths — more than 8,400 — from COVID-19 than New York, which has recorded more than 32,000 deaths and was the nation’s worst early hot spot. But officials have warned that the situation here could quickly deteriorate.
San Francisco has remained in what officials last week called its red zone, given its rapid increase in hospitalizations, and officials warned that an overwhelming of hospitals as New York saw in the springtime was still possible.
“It’s plausible we could get in a New York-like situation in the late summer or early fall. That’s why everyone needs to do their part to flatten the curve,” said Dr. Grant Colfax, the director of public health in San Francisco.
The number of new patients with COVID-19 requiring hospitalization in L.A. County, which had been rising, has become flat and is maybe even starting to decrease, said Dr. Christina Ghaly, the L.A. County director of health services.
It’s plateaued at a substantially worse number than in April, but the data nonetheless suggest an improvement. The number of ICU beds in L.A. County available for use has also remained stable, ranging from 130 to 160 beds on any given day.
“I hope this week marks a turning point, and that we’ll start to see the results of our corrective actions to slow the spread of COVID-19,” said Dr. Muntu Davis, health officer for L.A. County, on Thursday.
It can take three to four weeks after exposure to the virus for infected people to become sick enough to be hospitalized, and four to five weeks after exposure for some of the most vulnerable patients to die from the disease.
Gov. Gavin Newsom said last week that state officials were preparing hospitals for what could come.
At a news conference held in a Sacramento warehouse housing personal protective equipment, Newsom said Wednesday he was extending a contract with Chinese firm BYD to buy 300 million more surgical masks and 120 million additional N95 face masks to protect medical workers and others while also seeking bids from companies that could provide protective gear in future months. The so-called bridge contract is worth $315 million.
The governor said the step was necessary because California was sending out 46 million masks per month and had an inventory of 111 million N95 masks.
“We were able to bend the curve many months ago in the state of California,” Newsom said. “That bought us time to purchase and procure the kind of equipment you see behind me and put together our plans.”
The California Hospital Assn. is asking the Newsom administration to seek additional federal help in providing staff and to rethink existing nurse-patient ratios as conditions worsen.
Newsom said the state had a strategy “to address the prospect of a surge in hospital utilization, the need to develop alternative care sites outside of our hospital system to help isolate and quarantine individuals.”
The governor acknowledged that he continued to hear complaints from medical workers who were not getting enough medical masks and other protective equipment despite increased deliveries by the state.
He said one advocate for nurses told him recently that many were getting only two or three masks a week, although medical standards require more.
“That’s unacceptable,” Newsom said. “We still hear those stories, and we have got to address that issue.”
Lin and Dolan reported from San Francisco, McGreevy from Sacramento.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.