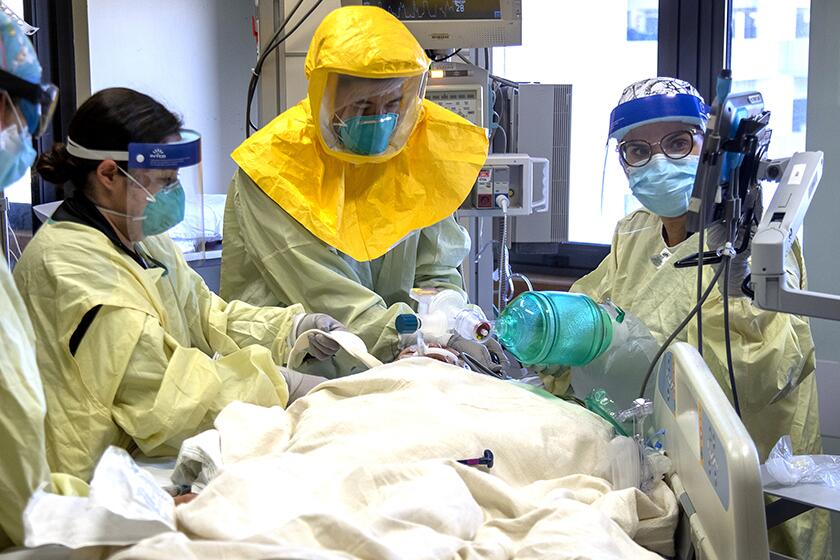
COVID-19 vaccine rollout painfully slow to nursing homes and other long-term care facilities

- Share via
No group has suffered more during the COVID-19 pandemic than staff and residents of nursing homes, where high concentrations of elderly people with serious health problems created the perfect killing ground for the virus.
Still, the effort to vaccinate people in those homes is rolling out at a frustratingly slow pace, according to experts nationwide.
For the record:
6:04 p.m. Jan. 9, 2021A previous version of this story misspelled the last name of Lake Minnetonka Care Center administrator Jeff Sprinkel as Sprinkle.
As of Friday, only about 17% of the more than 4 million vaccine doses distributed to long-term care facilities had been injected, according to the federal Centers for Disease Control and Prevention.
“Clearly nobody cares if old people die,” said Dr. Michael Wasserman, past president of the California Assn. of Long Term Care Medicine, which represents doctors, nurses and others working in nursing homes. “We could get all of these places vaccinated quickly if we approached it the right way.”
Wasserman blames the federal government for failing to set up a streamlined plan and directly oversee delivery of the vaccine.
Instead, crucial decisions about who gets the shots first have been left up to state and local governments, and the work of administering the shots has been left to large national pharmacy chains — CVS and Walgreens — that do not have the same relationship with nursing homes as the specialized pharmacies that already serve the industry.
Researchers share which numbers they’re watching to forecast when California’s deadly COVID-19 surge will end.
The slow rollout is “certainly a cause for alarm,” said David Grabowski, professor of healthcare policy at Harvard Medical School. “I think, like a lot of other parts of the pandemic, the federal response was too slow.”
Among the obstacles is bureaucracy: the sheer amount of labor required to fill out forms and upload data to ensure that consent was obtained and that each dose is tracked.
“It’s just crazy,” said Jeff Sprinkel, administrator of the Lake Minnetonka Care Center, a home with only about 20 residents in Deephaven, Minn.
When a crew showed up to administer the shots in late December, they had six people with them, more than could safely fit in the small break room used for the vaccinations given social distancing requirements. And three of those people were there only to “input information into their database,” Sprinkel said.
It took 7½ hours for the team to vaccinate everyone, a task that could have been completed by a single nurse in the same time without all the paperwork, Sprinkel said.
And because the vaccines come in batches, about eight doses were left over after everyone who qualified for the first round of shots had been vaccinated.
“I contemplated having my family vaccinated, giving it to my wife, but I imagined that hitting the news, it would make us reviled,” Sprinkel said. Instead, the doses went to waste.
Another obstacle has been the surprising degree of hesitance among nursing home staff to take the vaccine. A survey last month by the Kaiser Family Foundation found that 29% of healthcare workers nationwide were “vaccine hesitant,” a figure slightly higher than the percentage of the general population, 27%.
“We haven’t treated staff very well in this pandemic,” Grabowski said.
Roughly 40% of COVID-19 deaths nationwide have been among residents and staff at long-term care facilities, yet workers there have been chronically short of the masks, gloves and gowns needed to keep them safe from the virus, and most have been denied hazard pay even though they have done some of the most dangerous work.
“I think they’re pretty distrustful now,” Grabowski said. “I get why they might not be anxious to step forward.”
Another factor slowing the rollout is the number of active cases at nursing homes, which has been climbing steadily along with the post-holiday surge of cases in the general public.
“If you have a nursing home with 100 residents and 20 had COVID last week, they might elect not to have the vaccine,” said Dr. Christian Bergman, an academic geriatrician at Virginia Commonwealth University. “You wouldn’t be able to monitor for any adverse event, and they likely would have protection for 90 days, so we’re not giving them to those people.”
The lifesaving vaccines didn’t begin to be administered in Virginia until Dec. 28, Bergman said, and then the shots stopped abruptly for New Year’s Eve and New Year’s Day, slowing things down from the start.
Despite the glitches, most homes in the state hope to have their first doses administered by the middle of January. “That will help a lot in stopping the spread,” Bergman said.
So far, data documenting the progress of the vaccine effort in California nursing homes are hard to come by. State and Los Angeles County health officials did not respond Friday afternoon to requests for the numbers.
But interviews with local industry experts suggest things aren’t going much quicker in California than elsewhere in the country.
Raffaela Meyer, vice president of operations at Skilled Nursing Pharmacy, which specializes in providing medicine to nursing homes in California, said there are problems up and down the state.
Her company has so far not been tapped to administer the vaccines, but many of her clients have said they aren’t scheduled to get their first doses until the end of January. In Los Angeles County, where public health officials opted out of the program run through CVS and Walgreens in order to handle vaccinations directly, homes have seen the opposite problem.
“A lot of our nursing homes in L.A. County have hundreds of extra doses,” Meyer said. Once opened, those vaccines have a limited shelf life, and the nursing homes don’t know what to do with them.
“I am on calls every week with L.A. County; they don’t have any answers. On calls with [state health officials], they don’t know either,” Meyer said.
Most of the homes with extra doses are skilled nursing facilities, places for people who need the highest level of medical care.
They have been the top priority to get vaccines, along with front-line hospital staff, because of the devastating toll the virus has taken there.
One way to use their extra doses, Wasserman said, would be to share them with assisted living facilities, whose residents are just as old and often nearly as sick but haven’t been included in the first group to get vaccinated.
“They’re on fire with new cases right now,” Wasserman said.
He worries that frustration with the delays will lead to pressure to distribute the vaccine to the general public before states and local governments get around to vaccinating people in assisted living facilities.
“And who gets shoved to the back of the bus then? Elderly residents and the poor women of color who take care of them,” Wasserman said.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.