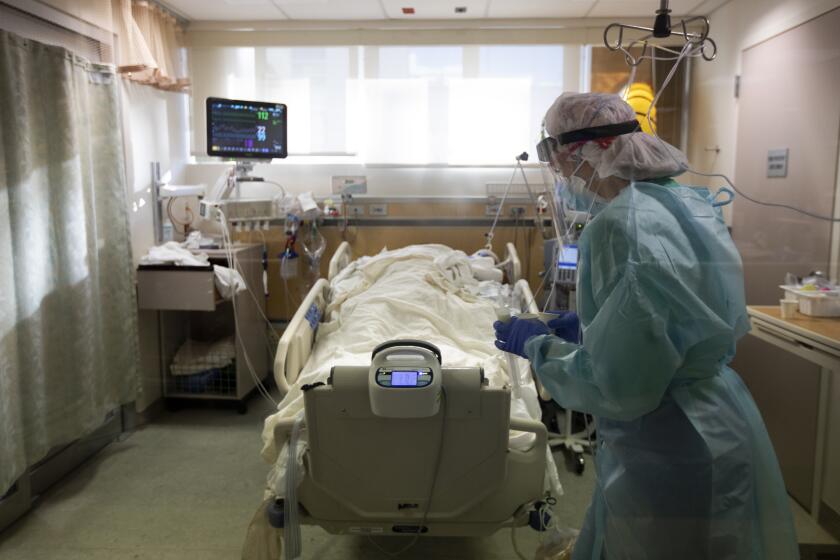
Rapid spread of U.K. coronavirus variant in Southern California sparks alarm

- Share via
The spread of the highly contagious coronavirus variant first identified in Britain is sparking worry about a future surge in Southern California, one of the nation’s two hot spots of the strain.
Scientists say it is essential to keep coronavirus transmission low and ramp up vaccinations quickly, and if the variant spins out of control, hospital systems could again become overwhelmed. The variant, known as B.1.1.7, has been identified in 467 people in 32 states. Florida has seen the most cases, with at least 147, followed by California, with at least 113.
B.1.1.7 is expected to become the dominant variant within weeks. L.A. County officials announced the second confirmed case Saturday and said it is “spreading in the county.” At least two cases have been identified in San Bernardino County.
San Diego County has California’s largest cluster of known cases of B.1.1.7, at least 109, plus 44 others that are linked epidemiologically to known cases of the variant, officials said last week. Health authorities in San Diego County announced last week the first death linked to B.1.1.7, a 71-year-old man who was a household contact of someone who was confirmed to have been infected by the variant. Two people have been hospitalized with the variant.
The median age of those sickened with B.1.1.7 is 30, but the strain has been identified in newborns and up to age 77, said Dr. Wilma Wooten, the San Diego County health officer.
The emergence of B.1.1.7 “requires us to remain vigilant, to not be complacent, to continue to take all the necessary precautions to slow the spread,” warned Nathan Fletcher, chair of the San Diego County Board of Supervisors.
Experts say the improving COVID-19 picture in California now is traceable in part to tough measures taken two months ago. Officials estimate that as many as 25,000 severe cases of the disease were prevented.
B.1.1.7 led to a rapid expansion of COVID-19 across the U.K., Ireland and Portugal and quickly became the dominant strain in those countries, Natasha Martin, associate professor in the UC San Diego Division of Infectious Diseases and Global Health, told the Board of Supervisors last week.
“This particular variant is estimated to be 50% to 70% more transmissible than previous variants, leading to surges in cases,” Martin said. “There is recent evidence that it may lead to higher mortality as well.”
California first detected the B.1.1.7 variant Dec. 30 in San Diego County. It’s now estimated to account for 5% of circulating strains, Martin said.
“The question is not whether this strain will become dominant, but how long it will take, and what effect it will have on our epidemic trajectory, given its increased transmissibility,” Martin said.
COVID-19 patients who take months to overcome their coronavirus infections despite treatment can become incubators of dangerous new strains.
The dominance of B.1.1.7 could dramatically worsen the pandemic in California. Currently in the state, the effective reproduction number — the average number of people to whom a contagious person transmits the coronavirus — is around 0.8. This means every infected person transmits the virus to fewer than one person, which explains why the pandemic is improving in the state. But should B.1.1.7 become the dominant strain, the reproduction number could become greater than 1, Martin warned.
Officials need to operate with caution in reopening the economy, she said. Even a decent vaccination plan is no match for the U.K. variant if people abandon wearing masks and practicing physical distancing, according to a simulation Martin presented.
If people reject such measures, as many did in the fall, San Diego County will likely see its case count — currently at about 1,500 new cases a day, the lowest in roughly two months — rise to as much as 7,000. That would be far worse than anything the county has experienced so far in the pandemic. The county topped out at about 3,600 new coronavirus cases a day for the seven-day period that ended Jan. 12.
“This scenario ... would overwhelm our health systems,” Martin said. “There is some emerging data that the B.1.1.7 [strain] is more lethal. So we could expect even more deaths than we’re seeing now for every case.”
Reducing the amount of circulating virus would delay the expansion of B.1.1.7, Martin said.
“I can’t stress this enough — with the emergence of B.1.1.7 and other strains which may be more transmissible and potentially more lethal — now is the time to double down on reducing transmission and expanding vaccination,” Martin said.
Concern about the strain, as well as the high number of daily cases, led Wooten last week to retain a San Diego County order that prohibits restaurants from allowing outdoor dining between 10 p.m. and 5 a.m.
Dining locations comprised about 20% of confirmed community outbreaks over the last 10 months, according to San Diego County.
Wooten told the supervisors she was uncomfortable allowing restaurants to reopen for outdoor dining service late at night because those that did often transitioned into parties, with households mixing and people drinking and not wearing masks.
“I am uncomfortable — with the number of cases that we still have — with changing that particular order at this time,” Wooten said.
San Francisco has also kept in place an order requiring customers to leave outdoor dining areas by 10 p.m.
That’s a different stance from L.A. County, which Friday allowed outdoor dining to resume, including during late-night hours. L.A. County Public Health Director Barbara Ferrer said Monday that the U.K. variant is thus far not dominant in the county. She urged people to continue to wear masks, practice physical distancing and stay at home as much as possible — and, if dining outdoors at restaurants, to adhere to the new rules.
Those rules include dining at a table only with members of your household, with no more than six people and spaced at least eight feet from other tables. Outdoor dining areas must have at least two noncontiguous sides that are completely open to increase the flow of breezes to dissipate exhaled virus particles, and guests are urged to wear masks when their servers approach.
“That’s what we’re trying to do right now: Keep the numbers as low as possible while we wait to get more vaccines and really accelerate the pace of vaccinations,” Ferrer said.

The vaccines that are currently available are believed to be effective against B.1.1.7.
Officials have also voiced concern about a variant identified out of South Africa, B.1.351, and a closely related variant from Brazil, P.1. The South African strain has been detected in two cases in South Carolina — in different parts of the state and not believed to be epidemiologically linked — and one in Maryland. The Brazilian strain has been identified in a single case in Minnesota.
Current vaccines have been found to be less effective against the South African variant, although “it still was not below the cutoff where you would expect some degree of efficacy,” said Dr. Anthony Fauci, the U.S. government’s top infectious diseases expert.
Nonetheless, scientists and government officials are working on an additional booster shot in case officials feel it’s needed to protect against new strains.
“This is a wake-up call to all of us,” Fauci told reporters during a briefing Friday. “We will continue to see the evolution of mutants. So that means we ... will have to be nimble to be able to adjust readily to make versions of the vaccine that actually are specifically directed toward whatever mutation is actually prevalent at any given time.”
We must also ramp up vaccination efforts as quickly as we can, Fauci said. “Viruses cannot mutate if they don’t replicate,” he noted.
Researchers once believed t would take months or even years for the virus to develop resistance to vaccines. The speedy evolution is largely a result of the virus’ unchecked spread.
It’s no coincidence that the rise of mutations is occurring in nations where the coronavirus has run rampant.
“Letting virus run wild, like [the U.S. and] Brazil did, endangers everyone,” Dr. Ashish Jha, dean of the Brown University School of Public Health, tweeted.
The emergence of the U.K. strain could mean that the summer — rather than being a quiet period for the coronavirus — could result in a higher prevalence, Dr. Scott Gottlieb, former commissioner of the U.S. Food and Drug Administration, told CBS News’ “Face the Nation” on Sunday.
“What’s going to likely happen is that the prevalence is going to be high in certain regional hot spots. So we’ll have hot spots of infection and maybe epidemics in parts of Florida, parts of Southern California, because of B.1.1.7. They’ll never really get out of it, but the rest of the country will see prevalence come down,” Gottlieb said.
Gottlieb said that the South African and Brazilian variants — unlike the U.K. strain — don’t seem to be more transmissible than the original virus. That means “we have time to get control of those variants and develop new boosters that could protect against them,” Gottlieb said.
Michael Osterholm, director of the University of Minnesota’s Center for Infectious Disease Research and Policy, offered a far more dire forecast than Gottlieb’s in an interview Sunday on NBC News’ “Meet the Press.” Osterholm compared the U.K. variant to a forming hurricane and predicted a new surge in six to 14 weeks.
“And if we see that happen — which my 45 years in the trenches tells me we will — we are going to see something like we have not seen yet in this country,” Osterholm said. “That hurricane’s coming.”
Paul Sisson of the San Diego Union-Tribune contributed to this report.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.