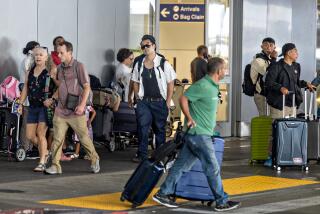He barely survived a bout of COVID-19. Now the Delta variant looms

- Share via
SAN DIEGO — The coronavirus played a nasty trick on David Arellano.
When doctors put him into a medically induced coma on April 13 because of a life-threatening case of COVID-19, the Alpha variant of the virus held sway. But by the time they started weaning him off sedatives on May 23, the strain gaining dominance was a new version, first identified in India, called the Delta variant.
The new variant, Arellano quickly learned, is mutated enough that the antibodies his body built to fend off his previous coronavirus infection don’t work so well against it.
His immune system — and the immune systems of all those who fought off the virus before Delta arrived — is aimed at the past, like bottles of expired medicine.
It is particularly disheartening news for a man who nearly died on a ventilator at Sharp Grossmont Hospital after COVID-19 attacked his lungs, then turned into pneumonia.
“It’s very disappointing because I, at the time, knowing that I have the actual COVID antibodies [thought,] ‘OK, I’m protected,’” Arellano said. “In reality, I’m not, because I’m still vulnerable to the Delta variant, and I don’t feel that I really have any protection.
“It’s scary; I do not want to go through this again.”
Though data are scarce on how many Delta-related reinfections have occurred among those with natural immunity to previously dominant variants, researchers have increasingly observed Delta’s evasive abilities.
A study published last month in the medical journal Clinical Infectious Diseases reviewed 106 recent papers that examined the levels of antibody effectiveness after natural infection and vaccination. The researchers concluded that while natural immunity seemed to protect well against the Alpha variant — first detected in the United Kingdom — it “lost significant potency” against Delta and variants of concern identified in Brazil and South Africa.
The analysis found that antibodies created by mRNA vaccines such as the two-dose shots from Pfizer and Moderna were able to create significant concentrations of protective antibodies “against all variants of concern.”
But it is also becoming increasingly clear that a single dose of mRNA vaccine, which offered significant protection against previous variants, is just not enough to protect against Delta.
Another study, published last week by British researchers in the New England Journal of Medicine, documented significantly better antibody protection among those who received two doses of the Pfizer and AstraZeneca vaccines. Single-dose effectiveness against the Delta variant is estimated at 35.6% for the Pfizer vaccine but jumps to 88% after a second shot.
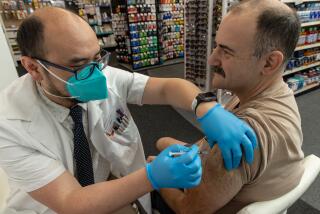
Arellano has not had an opportunity to get his first shot. He suspects he got infected while returning from a trip to Costa Rica with his fiancee, Betty Lemos, in late March. Though he said they wore their masks at all times, they were surprised to find themselves surrounded by crowds of unmasked young adults on spring break while changing planes at Dallas Fort Worth International Airport.
Both started experiencing symptoms shortly after getting home.
Neither qualified for vaccination before leaving for their trip, and though age-based criteria changed by early April, Arellano was already infected. Lemos, who said she had a very mild case, was able to get her shots by mid-April.
Bad timing has kept Arellano from following suit. Doctors, he said, have not cleared him to get his first shot because his body has not yet recovered enough from the ravages of weeks spent in a hospital bed on a ventilator.
And so he waits for the OK, all along knowing that, while his previous infection does convey some protection against Delta, it is not nearly as strong as what he would get by being fully vaccinated.
And it’s not as though he can just hide out at home in the meantime.
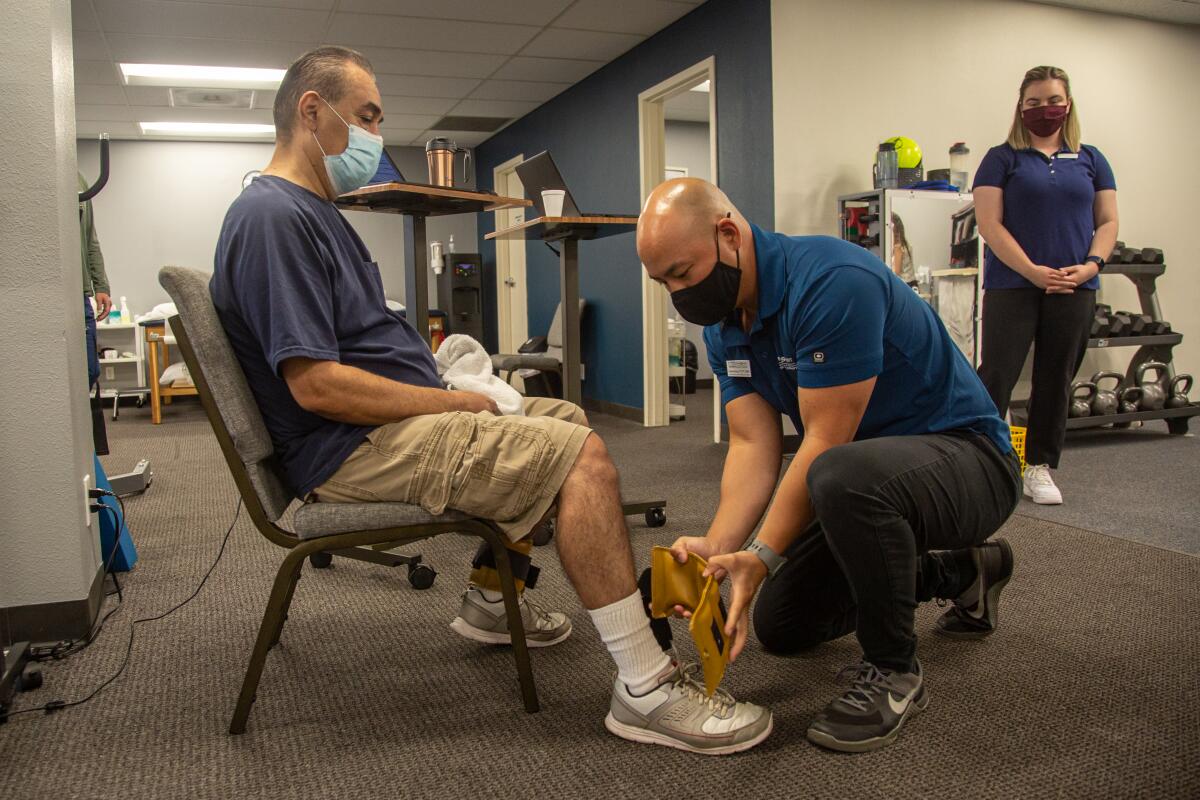
To recover, he needs to make regular rehab visits to a physical therapy center in El Cajon, not to mention myriad follow-up appointments with doctors who assess his recovery progress and will make the call on when he is vaccine-ready.
He has no choice but to venture out into the world, one that increasingly wants nothing to do with mask-wearing, even at a time when Delta has pushed San Diego County’s new case totals past 700 per day.
And he knows that, once he is cleared for vaccination, the protection will be far from immediate. Depending on which type of vaccine he receives, he will have to wait three or four weeks for his second shot, and full immunity will not arrive until two weeks after that.
That’s a five- or six-week wait, a clock that ticks down quite slowly for someone whose doctors told him when he was discharged from the hospital that he nearly did not make it through his first coronavirus bout.
Moving through the world carrying that kind of weight, Arellano said, is a particular kind of heavy.
“It’s not only uncomfortable, but it’s literally spooky,” he said.
The specific details of Arellano’s situation — being sedated because of COVID-19 infection when it became his turn to get vaccinated, then unable to do so during the months-long recovery process — make his predicament rare. But Dr. Eric McDonald, San Diego County’s chief medical officer and a key figure in the region’s response to the COVID-19 pandemic, noted that there are plenty of people who can’t be vaccinated for various reasons, whether because they’re undergoing cancer treatment or because they suffer from diseases related to the immune system.
“Getting vaccinated is not just about yourself,” McDonald said. “He is a good example of somebody who, for good medical reasons, has to wait until he can get vaccinated to have better protection than he has now.”
Those who are able to get their shots and are refusing to do so confound Arellano.
Many in recent weeks and months have said they would prefer to just become infected and get it over with rather than get vaccinated. Most, they say, come through just fine with minimal symptoms and no trip to the hospital.
And that’s technically true. County records show that, while the hospitalization rate has been 4.7% for the unvaccinated since Jan. 1 compared with 1% for the fully vaccinated, it also means that 95.3% of the 115,382 unvaccinated people who have tested positive this year have not needed significant medical intervention.
Last week, as Arellano readied to do the complex stretches and lifts that have been necessary to rebuild a body that could not stand when he regained consciousness, he said he once understood that line of reasoning but can no longer accept it. Rolling the dice on this disease just does not seem worth it from where he stands.
Today, more than three months after they put him under, Arellano said he still lives with pain daily. He still travels with an oxygen tank just in case, and he cannot forget the indignities that awaited him after his doctors finally took him off sedation medications. Most don’t realize, he said, just how helpless a person is after weeks or months of paralysis. Muscles are so wasted that there is no room for personal dignity. Even going to the bathroom and bathing require the help of trained professionals.
Formerly a ramp worker at San Diego International Airport who was furloughed in 2020 because of the pandemic’s effects on the travel industry, Arellano said, he was not in bad shape when COVID-19 struck. His job kept him moving all day, guiding planes to their gates and moving baggage where it needed to go. But that did not spare him from a severe infection.
“I’ve always been healthy, had no preexisting diseases, and it got me, it got me hard,” he said. “You could be one of those people who get infected by this virus, and then there is no time to reconsider getting the vaccine.”
Sisson writes for the San Diego Union-Tribune.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.