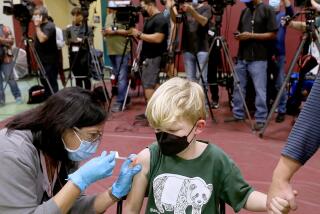
As Blue Shield steps back from controversial vaccine role, critics question results

- Share via
SACRAMENTO — As public health officials continue their push to vaccinate millions of hard-to-reach Californians against COVID-19, they are doing so largely without the help of Blue Shield of California, the company whose oversight Gov. Gavin Newsom said was essential to improving the state’s slow distribution of doses earlier this year.
The company’s reduced role announced last month closes a controversial chapter in the state’s ongoing efforts to combat COVID-19, one that began with questions about the Newsom administration’s handling of who should be first in line when supplies were limited and culminated in the governor’s surprising decision to put the insurance giant, a longtime political donor, in charge.
Newsom had said Blue Shield would speed up the state’s distribution of lifesaving vaccines and improve the slow accounting of unused doses. But now, with Blue Shield stepping back, the results of that decision remain unclear. Many of the county officials who initially criticized Blue Shield’s involvement remain skeptical of the vaccine program’s efficacy, while others say the company improved the state’s operations by standardizing how vaccine providers reported doses given, allowing officials to more accurately assess where to send more.
“Some may wish to rewrite history and say we just needed to give the existing plan more time. But we didn’t have time,” said Sami Gallegos, spokeswoman for the California Department of Public Health. “The crisis needed a solution and lives depended on us moving faster.”
Whether the state would move faster under the $15-million Blue Shield contract has been questioned by county officials since Newsom announced the change in late January. Amid the objections from vaccine providers, Blue Shield and the state did not finalize contracts until mid-March, when the number of doses sent to California was rapidly increasing.
San Joaquin County Board of Supervisors Chair Tom Patti is adamant that the state’s vaccine program led by Blue Shield slowed his region’s ability to get shots in arms. Patti, a Republican, said the county successfully fought for some modifications to the conditions Blue Shield and the state insisted on as a prerequisite for getting vaccines, but that the changes under the contract still resulted in San Joaquin having to scrap its own program targeting hard-to-reach populations.
“This entire process was an impediment and in no way did it help,” Patti said. “There was no benefit in any capacity.”
Some Fresno County officials expressed concern in February about the contract, saying they were worried that it mandated an online scheduling system that may make it harder to vaccinate agricultural workers in their region.
Six months later, Joe Prado, interim assistant director of the Fresno County Department of Public Health, said in a statement that the contract with Blue Shield provided “great assets,” such as a statewide vaccine marketplace that allowed counties to view and transfer their vaccine inventories among other counties.
Kat DeBurgh, executive director of the Health Officers Assn. of California., said it is difficult to assess how the state’s vaccination rates would have changed, if at all, without Blue Shield. The company is taking a limited role now as the needs around vaccines have shifted, she said. When Blue Shield stepped up earlier this year, DeBurgh said the state had a limited supply and high demand.
“We have a steady supply now and we are trying to make sure that demand increases,” she said.
Part of the impetus for the overhaul under Blue Shield was the revelation that the life-saving vaccines were sitting on shelves in some areas and the state’s flawed data system made it impossible to track how many doses were available at any one time. To counter that, the state began requiring most providers to use its My Turn appointment system, which itself was initially inundated with complaints of glitches and compatibility issues.
DeBurgh said the My Turn system eventually became very useful. Not all vaccine providers were required to use the system, easing some initial concerns.
“It got better over time,” she said. “It was one portal that allowed you to find out if you were eligible, schedule an appointment and get the vaccine. That was very helpful.”
Blue Shield’s involvement in determining where to send doses in the state and which healthcare providers would be part of California’s new vaccine network frustrated county officials who had up until that point run their own programs. The lack of buy-in from counties delayed the start of the program under Blue Shield, with nearly all counties initially refusing to sign a contract with the insurance company that outlined new rules to follow in order to receive doses from the state.
Many county officials argued that the state’s decision to outsource oversight of how vaccines were allocated beginning in February came after they had worked out internal hiccups and the biggest hurdle — lack of supply — was falling away.
California received 1.5 million doses in December and 3.4 million in January outside of federal programs that shipped directly to pharmacies and other providers, according to data provided by the California Department of Public Health. That increased to 4.6 million doses sent to California in February, 5.9 million in March and 8.4 million in April at the peak.
“The problem that existed was there wasn’t enough vaccine,” Santa Clara County Executive Jeff Smith said. “In my opinion, what Blue Shield did is they moved around the deck chairs on the Titanic. They provided no extra value to our response.”
Blue Shield officials said the company helped build up California’s capacity so that it could deliver 6 million doses a week, up from 1.6 million before the contract. However, that maximum capacity was largely unneeded since the most vaccine the state ever received in a week was 2.4 million doses.
“It was really frustrating,” Smith said. “It took a lot of time and effort that was diverted to deal with the contract with [Blue Shield]. Ultimately, we improved our own supply of vaccine by going through the federal government directly.”
Lucresha Renteria, executive director of Mendocino Coast Clinics, which serves 10,000 people across northern Mendocino County, said the system under Blue Shield became too “bureaucratic and messy,” requiring her to navigate multiple forms and websites to receive doses.
“The system kept changing, and it made it difficult to figure out how to order vaccines,” Renteria said.
Renteria said when she ordered vaccines, she received double what she asked for. After a month, she said the clinic opted to order through the county public health department instead.
“I know the state thought they were doing this to make it better, but we just needed a few months to figure it out with our public health department,” she said. “By the time they implemented the [contract], we had already figured it out. They were solving for a problem that didn’t exist anymore, and the bureaucracy created more problems.”
As part of the contract, the state asked Blue Shield to ensure that 95% of residents in urban areas were within 30 minutes of a vaccine site and that those in rural areas were less than an hour from access to a provider. Blue Shield said they surpassed that target, with 99% of Californians within those distances.
“Our reward has been to help save lives,” Blue Shield President Paul Markovich said in a statement.
Under Blue Shield’s contract, the company can bill for out-of-pocket costs incurred up to $15 million and won’t profit off the deal, the company noted. A spokesperson for the state public health department said the company has not yet billed any of its expenses.
Critics have argued that Blue Shield stands to gain more than goodwill and reimbursed expenses under the state contract. The company routinely has business before California government that has major financial impacts. For example, included in a state budget bill signed by Newsom last month was a long-sought wish-list item for Blue Shield that requires health plans to share patient records and data through a Health Information Exchange by 2024.
Blue Shield, a longtime donor to Newsom, said in a press release that the company is “thrilled” with the new law, which is expected to reduce healthcare costs by allowing providers to see a more complete picture of a patient’s health history.
“Blue Shield has a lot to gain from the development of a statewide [Health Information Exchange] because it would help it compete against California’s biggest health plan, Kaiser Permanente,” said Michael Johnson, a former Blue Shield executive turned critic of the company.
State officials say Blue Shield will remain in an “advisory role” for the duration of its contract with the state, which ends in December. That role allows the state to increase Blue Shield’s involvement or seek advice from company officials if a COVID-19 variant requires the state to ramp up distribution of additional vaccine doses, according to a spokesperson from the department of public health.
The overall cost to the state to create and run the vaccine network is pegged at $202 million, according to the most recent budget estimates released in May.
That’s an increase from the Newsom administration’s estimate in March when administering the vaccine network was estimated to cost $151 million, the bulk of which was tied to information technology support. The state also brought in management consulting firm McKinsey & Co. for $13 million from February to April to assist Blue Shield and the state with the vaccine delivery system.
Sarah Dukett, legislative advocate for the Rural County Representatives of California, said it’s likely that some areas of the state won’t notice a difference with Blue Shield stepping back.
“I don’t think they did a bad job or a good job, I just don’t think it drastically changed the priorities on the ground in rural counties,” Dukett said. “The biggest problem was always supply, so I’m not sure the impact [Blue Shield] ultimately had.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.