California’s coronavirus hot zone: Hospitals full, ambulances diverted, patients moved out

- Share via
The summer coronavirus surge caused by the highly contagious Delta variant is showing signs of slowing in some parts of California but worsening in others.
The Central Valley is becoming California’s COVID-19 hot spot, with hospitals filling and health officials raising alarms, saying things could get worse before they get better.
Here is an overview of what’s going on.
What is the situation in the Central Valley?
The San Joaquin Valley, the Sacramento area and rural Northern California are now the regions of the state being hit the hardest by COVID-19 hospitalizations on a per capita basis, according to a Los Angeles Times analysis. The regions have lower vaccination rates than in the highly populated coastal areas of Southern California and the San Francisco Bay Area.
The worst may not be over. According to COVID-19 computer models published by the state Department of Public Health, the number of patients in intensive care units in the San Joaquin Valley is expected to increase for the rest of September, and hundreds more people could be dead by the end of the month.
In the San Joaquin Valley, the number of monthly COVID-19 deaths has tripled, from 93 in July to 311 in August. Just in the first six days of September, 78 additional deaths were reported.
The San Joaquin Valley still has an effective transmission rate of the coronavirus above 1, according to the state Department of Public Health, meaning for every person infected, the virus is being transmitted to slightly more than one other person, meaning the spread of the virus is increasing.
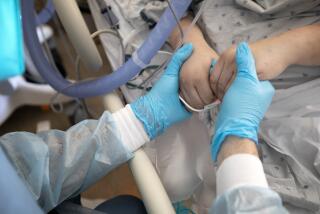
How bad is it for hospitals?
Demand is so intense at hospitals that ambulances have been instructed to not transport patients unless they meet criteria sufficient to warrant them being taken to a hospital — the kind of step Los Angeles County was forced to take during its winter surge.
Fresno County has also been forced to transfer severely ill patients far out of the region — as far away as Watsonville in Santa Cruz County, a 140-mile drive from Fresno.
And there is such a demand for coronavirus testing that Fresno County has run out of rapid tests, meaning that instead of people being able to learn whether they may be infected within minutes, they may have to wait 24 to 72 hours for test results.
Fresno County is also suffering a nursing shortage. But there are few nurses to spare. Even L.A. County’s public hospital system is unable to staff all of its beds due to shortages.
Officials in Fresno County are trying to recruit traveling nurses, but they’re in such high demand they can command wages of as much as $200 to $250 an hour, and sometimes they’ll leave hospitals in Fresno County after a day of working because they’ve received a better offer somewhere else, Lynch said.
Fresno County officials say federal and state authorities have so far been unable to provide much staffing help. U.S. Defense Department medical staff helped relieve Fresno County in the winter but are not available now, Lynch said. State officials have also said they have limited ability to send staff, Lynch said.
What is going on?
Vaccination rates are lower than in some other parts of California.
In Fresno County, 63% of residents 12 and older have been vaccinated with at least one dose. By contrast, in L.A. County, 75% of residents in the same age group have received at least one dose, as have more than 87% of vaccine-eligible residents in San Francisco and Santa Clara counties in the Bay Area.
For pandemic planning purposes, the state defines the San Joaquin Valley as comprising Calaveras, Fresno, Kern, Kings, Madera, Mariposa, Merced, San Benito, San Joaquin, Stanislaus, Tulare and Tuolumne counties.
The region with the second-lowest percentage of available ICU beds is Greater Sacramento, where 14.8% of staffed adult ICU beds were open as of Monday. The comparable figures are 19.7% in rural Northern California, 21.8% in Southern California and 24.6% in the Bay Area.
What is the statewide perspective?
Over the last month, new daily coronavirus cases in California have been generally stable, hovering between 12,000 and 15,000 a day, according to the analysis. And as of Monday, COVID-19 hospitalizations across California had fallen for six consecutive days — by 8% — from the summertime high recorded on Aug. 31.
Hospitalization rates are still relatively high throughout California for those suffering from COVID-19.
Nonetheless, COVID-19 hospitalizations are no longer rising as sharply as they once were in most parts of California. And in the state’s two most populous regions, hospitalizations have been ticking downward for the last two weeks, falling 12% in Southern California and 17% in the San Francisco Bay Area.
Although improving, coronavirus transmission remains high, and the risk of infection is significant, especially among unvaccinated people, who are far more likely to be hospitalized or die than vaccinated people. Virtually all of California’s counties — as well as 95% of counties nationwide —are considered by the U.S. Centers for Disease Control and Prevention to have “high” or “substantial” coronavirus transmission rates, the two worst categories on the agency’s four-tier scale.
Overall, California is weathering its fourth pandemic wave far better than some places nationwide, likely thanks to its overall vaccination rate — one of the highest in the nation, with 82% of residents 12 and older having received at least one dose — and indoor mask mandates imposed by counties where most Californians live.
What has been a COVID-19 bright spot?
Santa Clara County, Northern California’s most populous county, shows what can happen in an area with high vaccination rates. The county — home to Silicon Valley — has reported that 88% of residents 12 and older have received at least one dose of vaccine.
Yet, COVID-19 deaths in Santa Clara County in the summer have not increased as much as expected, given the increase in cases, said Dr. Sara Cody, the Santa Clara County public health director and health officer.
Santa Clara County has reported 30 COVID-19 deaths this summer, according to its website, a rate of 1.6 deaths for every 100,000 residents. L.A. County, by contrast, reported 1,026 deaths over the summer, a rate of 10.2 deaths for every 100,000 residents.
“I think that this can be attributed to the protective effects of ... the vaccinations in the population at large,” Cody said in a public meeting last week. “So far, our deaths really have been blunted, I think, from the very high vaccination rates.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.