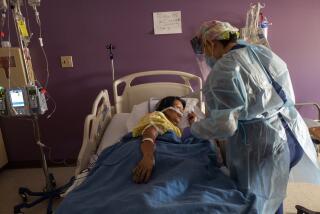Nurses, doctors sick. Ambulances, blood in short supply. Omicron hits L.A. healthcare hard
- Share via
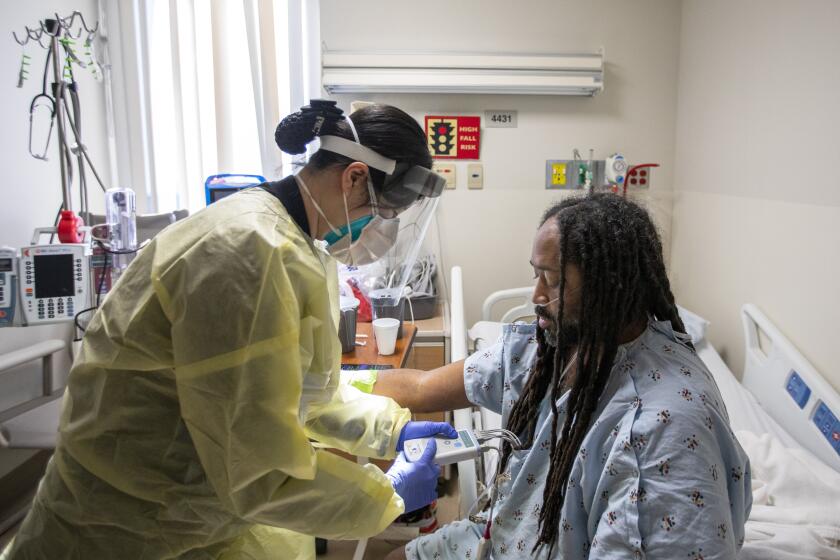
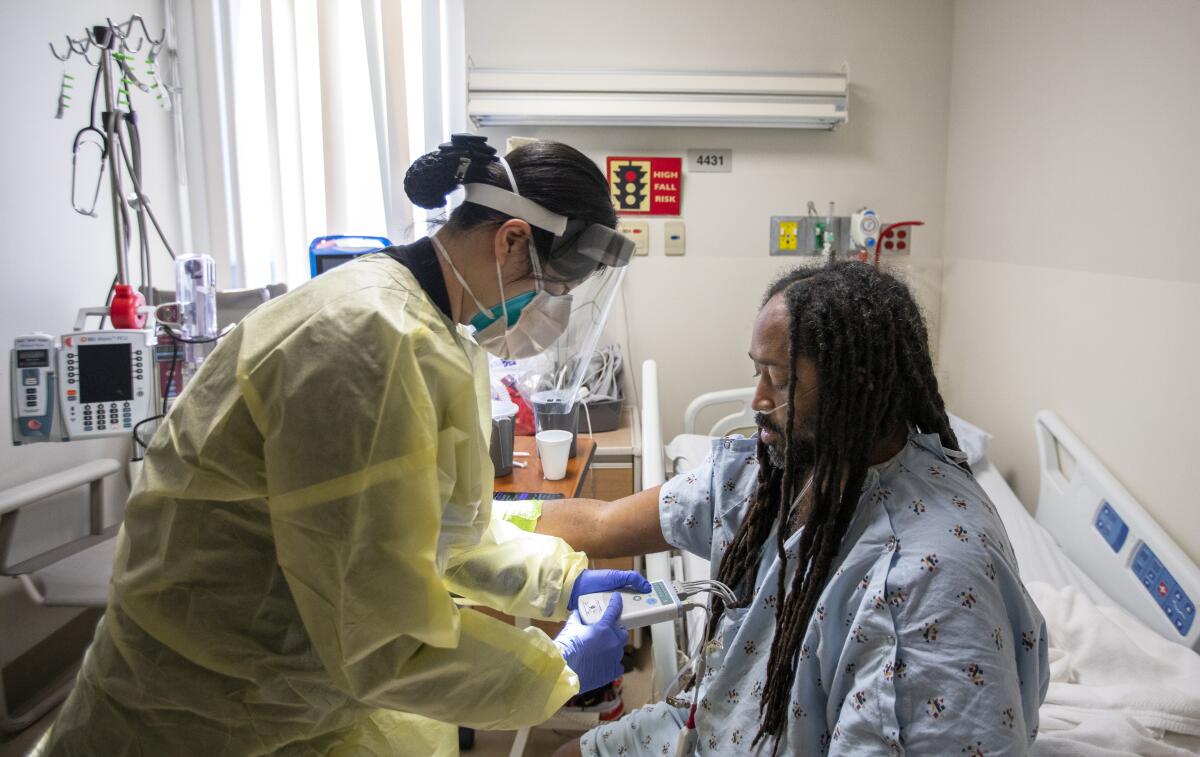
Los Angeles County’s hospitals are straining to provide medical care, hobbled by staffing shortages far worse than last winter’s coronavirus surge.
Many healthcare workers, burned out by the pandemic, have quit, and many who remain have tested positive for the virus and are at home isolating. And healthcare facilities are busier this year because there’s more demand for non-COVID-19 care.
Among L.A. County’s four public hospitals, hundreds of coronavirus-positive health workers are in isolation, which “has made it virtually impossible to ... maintain services that are at a level of care needed to support safe patient care,” Health Services Director Dr. Christina Ghaly told the county Board of Supervisors this week.
“The numbers are due to the much higher rates of community transmission than what we have experienced at any previous point in this pandemic,” Ghaly said. “There’s just a lot more virus out there in the community. And healthcare workers, just like anybody else, are getting infected.”
Experts say it’s a necessary solution to staffing shortages, yet many workers say the policy could be dangerous.
It’s not just nurses that are in short supply. “It affects physicians, respiratory therapists, radiology techs, lab staffs — the whole gamut of what is needed to run a hospital safely,” Ghaly said.
In the face of the latest surge in cases, Kaiser Permanente Southern California is temporarily postponing all elective surgeries that require an inpatient stay in the hospital after an operation, it announced Wednesday.
The hospital system will continue to perform emergency surgeries, urgent procedures including those involving cancer patients or people whose medical condition would be worsened by a delay, and elective outpatient surgeries that do not require an overnight stay in the hospital, its regional director of medical quality, Dr. Nancy Gin, said.
“We will continue to do everything we can to minimize the impact on our members and the public,” Gin said.
Ambulances are also facing longer delays before they can drop off patients. Companies who contract with the county to provide emergency transport through the 911 system “have experienced severe staffing shortages and are having difficulty responding to calls in a timely manner,” Ghaly said. Many employees are out sick, while other workers are not vaccinated, and “as a result, they are not able to work in line with public health orders.”
L.A. County has identified the 20 most hard-hit emergency rooms, and county employees have been dispatched to the top 10 — all privately run hospitals — to assist with offloading ambulances; the other eight are expected to receive federal help within the next two weeks, Ghaly said.
On Saturday, California sent a strike team to augment the 911 ambulance companies. “We requested five; we received one, with one still pending and three [to be determined,]” she said.
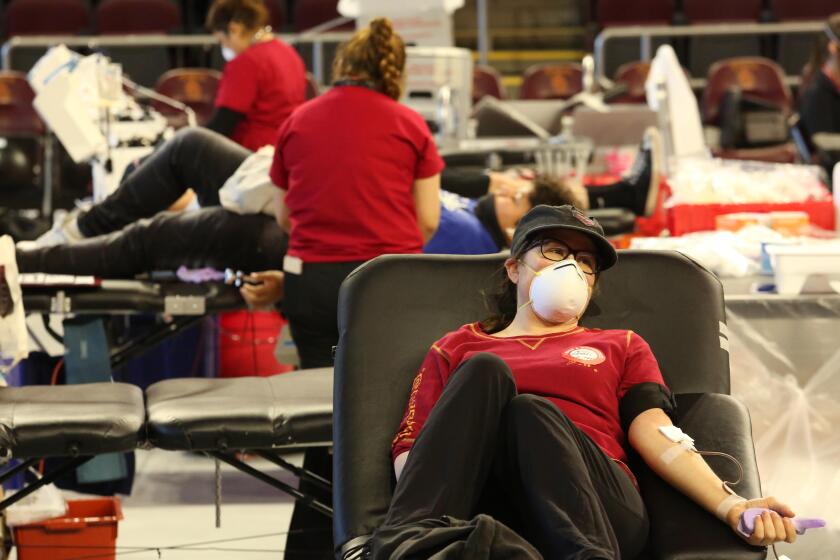
The pandemic and an unusual flu season have exacerbated the shortage, the Red Cross says, and blood donations are needed more than ever.
Besides the hospital surge, Ghaly warned that blood supplies across L.A. County are reaching a critical shortage. The American Red Cross is calling the nationwide blood shortage the worst in more than a decade.
“The demand for blood is high, but the donation volume is still down,” said Ghaly, who urged people to donate by going to redcrossblood.org. “Trauma centers just cannot operate without blood. If there’s not blood, they will need to close, and that is not a situation that we want to find ourselves in.”
Blood shortages forced the Los Angeles County Department of Health Services to shut down one of its trauma centers to new patients for hours earlier this week — a step it had not taken in over three decades, officials at the department said Wednesday.
The trauma center at Harbor-UCLA Medical Center closed to new patients for more than two hours Monday, a department spokesperson said. It had to reach out to other hospitals in the DHS system for blood in order to reopen.
The strain on hospitals in L.A. County is exacerbated because other facilities are refusing to care for coronavirus-positive patients. Outpatient dialysis companies are sending coronavirus-positive patients to hospitals, said Ghaly, adding that practice is inappropriate.
In addition, congregate residential care facilities, including those that care for mental health patients, are sometimes refusing coronavirus-positive patients, Ghaly said, “causing huge backlogs of patients filling up precious hospital beds.”
County officials are working to establish a motel voucher program to provide quarantine and isolation locations for residents who don’t require a certain level of medical oversight.
The county and state have deployed staff to establish three hospital surge units at: Mission Community Hospital in Panorama City, Providence Little Company of Mary Medical Center in San Pedro and Antelope Valley Hospital in Lancaster.
Los Angeles County health officials are urging residents to postpone nonessential gatherings and avoid some activities, especially with people who are unmasked, unvaccinated or at higher risk of severe illness.
To reduce transmission risk among visitors, L.A. County’s public hospitals have also restricted visiting hours, including the duration and number of visitors allowed.
Hospitalizations of coronavirus-positive patients in L.A. County are rising rapidly, growing to 3,912 as of Tuesday, six times the number compared to last month. But the latest tally is still a fraction of the record 8,098 coronavirus-positive patients recorded Jan. 5, 2021.
There were 536 COVID-19 patients in L.A. County intensive care units as of Monday, triple last month’s number. That is still less than one-third of last year’s peak, when there were 1,731 on Jan. 8, 2021.
Still, some officials expect the number of hospitalized coronavirus-positive patients to climb. As of Tuesday, California hospitals had 12,317 coronavirus-positive patients; that’s a little more than half the record of 21,938 set Jan. 6, 2021.
One model cited by Gov. Gavin Newsom on Monday indicated it’s plausible that the number of coronavirus-patients hospitalized in California could reach 23,000 by Feb. 2 — exceeding the pandemic record.
Newsom said that as of Wednesday morning, there were about 52,400 people hospitalized for all reasons, including COVID-19, in California. That’s nearing the peak of 53,000 set during last winter’s surge, a number California is expected to hit later this week, the governor said.
Data show that 4.5% of those who are infected with the Omicron variant are hospitalized, Newsom said Monday. That’s better than past surges: L.A. County estimated that during last year’s peak, 15% to 20% of coronavirus cases led to hospitalizations, and during the summer Delta wave, 5% to 6% of infections resulted in hospitalizations.
Newsom said the average length of stay in the hospital for Omicron patients is 3.6 days, fewer than for previous variants.
But the sheer number of Californians becoming infected with Omicron means that hospitals will likely continue to be stressed, even though a lower percentage of those infected need hospitalization.
“The totality of those getting this variant are such that it’s going to put tremendous strain on our hospital system. It’s not unique to California,” Newsom said.
The arrival of Omicron has pushed daily caseloads to their highest levels and sent a stream of new coronavirus-positive people to the hospital.
The governor said the demands on hospitals this winter are “manageable, but it’s challenging. It’s difficult.”
Emergency rooms statewide are undergoing immense strain. On Sunday, there were 55,000 total emergency department visits statewide, according to data Newsom presented; a year ago, there were 27,000.
The difference is that the demand for non-COVID emergency care is worse than last year, when much of California was under regional stay-at-home orders. On Sunday, there were 12,500 emergency department visits related to COVID-19; last year at this time, there were 11,500.
Evidence continues to show that many infections with Omicron result in mild or moderate illness. Still, people should still do as much as they can to avoid getting infected, L.A. County Public Health Director Barbara Ferrer said, particularly since Omicron survivors might be at risk of long COVID. There also is worry about children developing multisystem inflammatory syndrome, a rare but serious condition that can be deadly.
“We do know that weeks after last winter’s surge, we saw a huge increase in MIS cases, so it remains prudent to do everything you can to avoid getting infected,” Ferrer said.
Pediatric hospitalizations have risen recently. On Jan. 1, there were 79 coronavirus-positive children in L.A. County’s hospitals, 58 of them among children under 5, who are too young to be vaccinated. There were only four coronavirus-positive children younger than 5 hospitalized across L.A. County on Dec. 4.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.