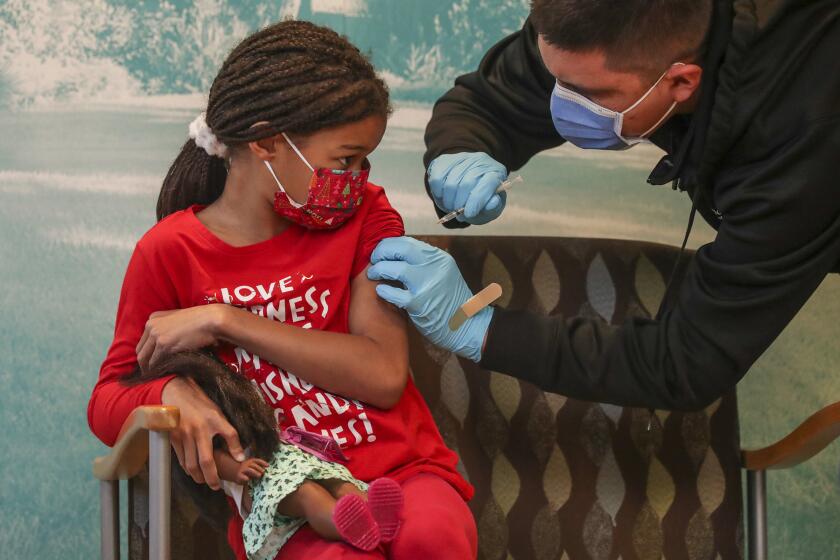
California surpasses 9 million coronavirus cases, equal to nearly 1 in 4 residents

- Share via
California has reported a total of 9 million coronavirus infections, fueled by this winter’s Omicron surge.
The overall case count, tracked by The Times, is now larger than the combined populations of San Diego, Orange and Riverside counties and is the equivalent of nearly 1 in 4 Californians testing positive at some point during the pandemic.
Even more stunning is how rapidly the caseload has ballooned since the arrival of the hyper-infectious Omicron variant late last year. Of the 9,001,924 total cases that had been compiled as of Monday, 3.9 million — 44% — were reported since Dec. 1.
In fact, half of California’s 9 million confirmed cases occurred in the last six months. It has been more than 25 months since California’s first cases were publicly reported.
But the torrent of infections has since slowed to a trickle.
Over the last week, California reported an average of 4,587 new coronavirus cases per day — down 61% from two weeks ago. At the height of the Omicron surge, the state’s daily case count topped 123,000, by far the most of the pandemic.
After topping out at 2,200 cases a week for every 100,000 residents, California is now recording 82, which is considered a “substantial” rate of transmission. Some experts say the risk of infection is dramatically reduced once an area falls into the “moderate” category: below 50 cases a week for every 100,000 residents.
The case rate in Los Angeles County is 86; in San Francisco, it’s 44; and in Orange, it’s 38, according to The Times’ coronavirus tracker. San Diego County’s rate is 137; San Bernardino’s, 81; Riverside’s, 70; and Ventura’s, 44.
The reduction in transmissions is bringing much-needed relief to healthcare systems. The number of coronavirus-positive patients hospitalized statewide Monday — 3,016 — is the lowest since late July, the early days of the Delta surge.
COVID-19 deaths are starting to decline but remain significant. Over the last week, an average of 163 fatalities were reported each day — pushing the total to nearly 86,000. To put that into perspective, it’s essentially the entire population of Newport Beach.
Though the Omicron variant has proved, on the whole, to be milder than strains that preceded it, officials stress that COVID-19 remains far deadlier than other seasonal respiratory diseases.
In December, L.A. County recorded 396 COVID-19 related deaths, versus 163 caused by pneumonia and flu, according to Public Health Director Barbara Ferrer.
Health officials still recommend masks in indoor public settings, but school operators will be able to require masks or make them optional.
Recent weeks have seen officials throughout California move to relax some of the preventative measures put in place to halt COVID-19’s advance — such as requirements to wear masks in indoor public settings or to flash a vaccine card as a condition of patronizing certain kinds of businesses.
California lifted its universal indoor mask mandate for vaccinated residents in mid-February. The state went further last week, saying masks are no longer required for unvaccinated residents. Indoor masking will no longer be mandatory at schools and child-care facilities after Friday.
Masks are still required on public transportation, including planes, as well as in healthcare settings, nursing homes, homeless shelters, jails, prisons and emergency shelters.
While conditions have improved, health officials continue to strongly recommend that everyone — especially those at high risk for severe COVID-19 illness — mask up indoors.
“COVID-related illness can be quite dangerous for many, since even those initially experiencing relatively mild illness can go on to develop long COVID,” Ferrer said in a statement Monday. “Taking sensible precautions remains the best way to keep everyone as safe as possible.”
The best precaution, health officials say, remains vaccination. California’s high baseline — with about 7 in 10 residents fully vaccinated — has been cited as evidence for why mandates can be lifted.
L.A. City Council to consider easing vaccination verification mandate for restaurants, gyms, bars, movie theaters, hair salons and other businesses.
During a news briefing last week, Ferrer said that while cases are declining, officials need to be prepared for another potential surge.
“It’s still with us. It has ebbs and flows, and we need to take advantage of the good times that we’re about to be in, where we really are seeing much less risk across the board for so many, and then be prepared should there be a new variant of concern or we experience another surge,” she said.
Though it’s too soon to declare the pandemic over, officials are mapping out what it will look like to live with COVID-19, as opposed to a constant battle against the disease.
“I do think that we will get to a place with this disease where we live with a relatively low level all year long, and that maybe we have some surges during respiratory virus season,” Dr. Rochelle Walensky, director of the U.S. Centers for Disease Control and Prevention, said in an interview broadcast Sunday on CBS’ “60 Minutes.” People would still die from COVID-19, Walensky said, but “not to the tune of 2,000 and 3,000 deaths a day.”
During the Omicron surge, the U.S. peaked at 2,600 COVID-19 deaths a day. Most recently, the nation is averaging 1,200.
Data show vaccines are effective against hospitalizations, although effectiveness against infection does wane. But that’s not surprising.
California officials in mid-February detailed their strategy for the next chapter of the pandemic, laying out a seven-part plan dubbed SMARTER, for shots, masks, awareness, readiness, testing, education and “Rx,” or medicating with anti-COVID drugs.
As part of this framework, state officials have set preparedness benchmarks, such as ensuring the capacity to administer at least 200,000 vaccines and 500,000 tests a day, stockpile 75 million high-quality masks and analyze at least 10% of positive coronavirus test specimens to track trends or the emergence of new variants.
“Certainly we have tools and a level of understanding that should no longer cause us to be afraid of what’s coming but really to be prepared for it,” Dr. Mark Ghaly, California’s health and human services secretary, said Friday during a discussion hosted by the Sacramento Press Club.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.