Should I get the Omicron booster now or wait a few weeks?

- Share via
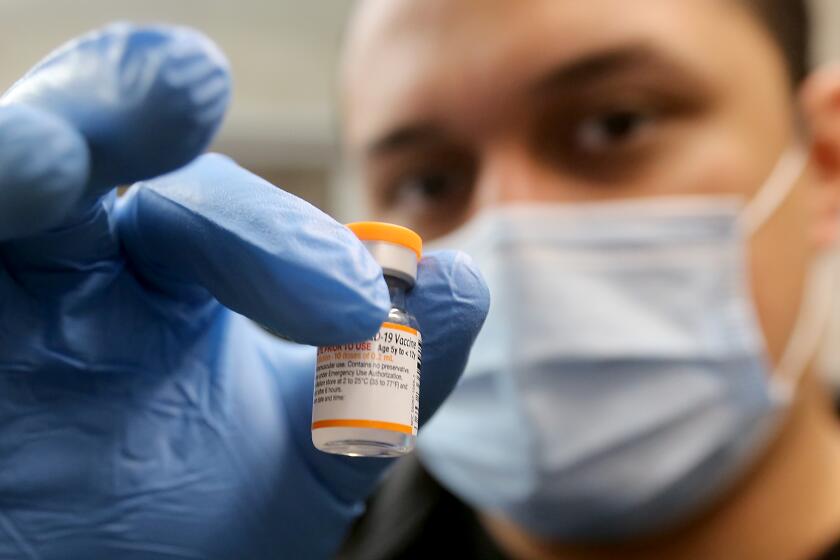
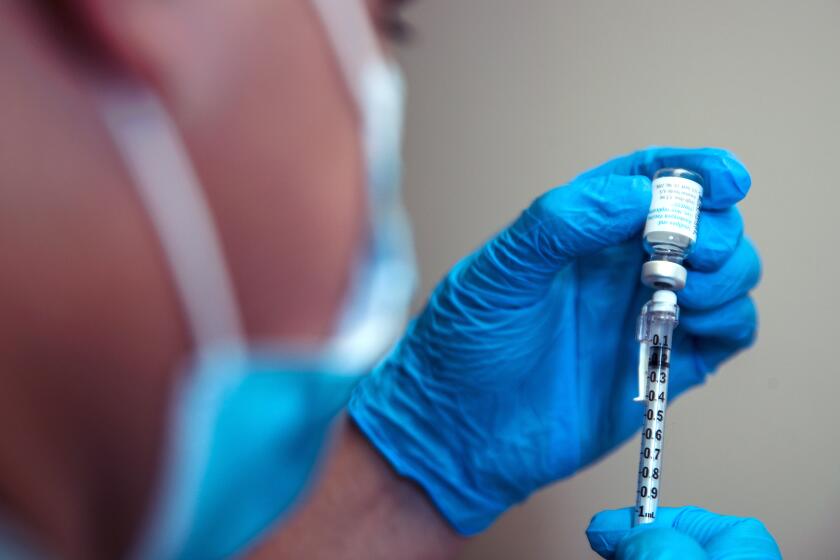
Omicron-targeting COVID-19 boosters are now available, but many are wondering: Should they get the shots immediately or wait to time them closer to the holidays?
The short answer is it depends — both on whom you’re asking and what factors might heighten your chance of serious health impacts. For those at lower risk of exposure or developing severe disease, holding off could make sense, according to some experts. But others say it’s best not to delay, especially with the potential for another coronavirus rebound this fall and winter.
“We do hear from people who say, ‘You know, I want to maximize my protection for the late fall and the winter holidays in particular. And I might wait.’ For people who are in relatively good health and younger, that may be an appropriate assessment,” said Los Angeles County Public Health Director Barbara Ferrer.
But she urged residents at higher risk for severe COVID-19 to get the new booster right away.
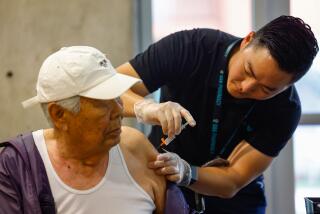
“Older people remain at high risk,” she said. “I wouldn’t delay for people who are at high risk.”
New boosters to protect against the latest Omicron variants of the coronavirus are arriving in Southern California this week. Here’s how to get one.
Dr. Robert Wachter, chair of UC San Francisco’s Department of Medicine, said getting the new booster “as soon as eligible seems like a pretty straightforward call to me.”
“While some may choose to wait for cases to begin ticking up later in the fall, ‘timing the market’ usually doesn’t work,” he tweeted.
Whenever you opt to roll up your sleeve, it’s important to note that it takes two weeks for the full effect of the booster to hit.
Peak effectiveness of the Omicron booster will likely be in the four or five months following the shot, with the maximum efficacy one month after the injection, UC San Francisco infectious-disease expert Dr. Peter Chin-Hong said.
During the pandemic’s first fall-and-winter wave, coronavirus cases in California began increasing in November and accelerated sharply in December. Last year, cases began spiking in December.
Ferrer urged eligible people to get the updated booster ahead of the holidays, expressing hope that a widespread uptake of the shot will reduce the severity of an expected end-of-year COVID wave.
“As we get deeper into the fall, we’re going to encourage that everyone who is eligible to get their bivalent booster before the fall holiday season begins does so,” Ferrer said. “We’ve survived two significant winter surges of this virus, but both have left a devastating impact on our community.”
Ferrer noted the first fall-and-winter COVID surge occurred before vaccines were widely available, while the second occurred when vaccines did not fully match the variant of the coronavirus that was circulating.
“We hope that with this new bivalent vaccine, we might reduce our chances of a third huge winter surge of COVID since we have a pretty good match with what’s circulating,” Ferrer said.
Vaccination providers need to make sure they’re administering the right vaccination to the right person, panel of health expert cautions.
Along with individual risk factors, a person’s plans also may play a role in their booster timing. If someone is about to embark on a trip abroad or head to a big event where there’s an elevated risk of exposure, getting boosted at least two weeks in advance could help reduce the likelihood of infection.
The question of how best to time a vaccine isn’t unique to COVID-19. Take the flu shot, for instance.
Getting the annual shot too early may lead to its peak effectiveness waning before the end of flu season. Get it too late and you risk being exposed without any protection.
In the context of flu, the U.S. Centers for Disease Control and Prevention says “vaccination should ideally be offered during September or October.” Some have suggested that an ideal time to get the flu shot is mid- to late October.
New booster shots have arrived and social distancing guidelines have eased, but coronavirus infections aren’t going away anytime soon.
Officials have pointed out that the decision to make the updated COVID-19 booster available in September is expected to reduce hospitalizations and deaths. Modeling studies indicate that distributing boosters starting this month could prevent 137,000 more hospitalizations and 9,700 more deaths compared with beginning a booster campaign in November.
Another wrinkle to consider is when a person was last infected with the coronavirus. The CDC suggests waiting three months after testing positive or the onset of COVID-19 symptoms, whichever came first, before getting the updated booster. But the agency also said other factors could alter that timing, such as the level of COVID-19 in the community and the person’s risk factors for severe disease.
One of the few hard-and-fast rules when it comes to timing is that a person must be at least two months away from their last vaccination or booster dose before getting the updated booster.
But even then, some experts suggest people should wait longer — at least three months — before getting the new booster, as doing so could provide better longer-term protection.
An analysis of death certificates from January to April showed COVID-19 deaths were nine times those caused by motor vehicles and more than five times the rate for flu and pneumonia.
Most people age 50 and older who got their second booster shot did so fairly quickly after federal authorities gave the green light at the end of March. According to data the CDC recently presented, many got the additional shot in April and May.
And for most individuals ages 5 to 49, “it has been six months or more since their last COVID-19 vaccine” or booster, the CDC said in a slide presentation earlier this month.
The updated booster from Pfizer and BioNTech is available for those 12 and older, while the offering from Moderna is an option only for adults 18 and older. Children age 5 to 11 are eligible for a conventional booster shot.
CVS, Walgreens, Rite Aid, Walmart and Ralphs are offering the new booster, the companies say on their websites. Updated boosters are also being offered by local public health departments across California.
An autopsy must still be conducted, health officials said.
Officials say it’s safe to get the COVID-19 booster and the flu shot at the same time, preferably in separate arms.
In an advisory, however, L.A. County health officials said some people — particularly adolescent or young adult males — may want to consider waiting four weeks after getting the Jynneos vaccine, used to protect against MPX, before getting a Pfizer, Moderna or Novavax COVID-19 vaccine.
But recently getting a Pfizer, Moderna or Novavax COVID-19 vaccine need not require a delay in getting the Jynneos vaccine if it’s recommended to prevent developing MPX illness in the context of an outbreak, the advisory said.
Health officials in California recently started to use the name MPX — pronounced mpox — because of widespread concerns the virus’ original name is stigmatizing and racist. The World Health Organization is in the process of formally renaming the disease, which will take several months.
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.