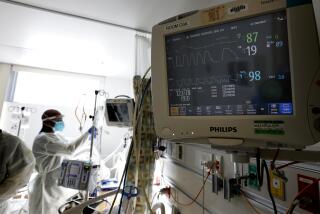
Instead of a hospital stay, he was given a cellphone with medical staff on speed dial

- Share via
After dealing with a persistent cough and diarrhea and cycling through various over-the-counter medications, Lincoln Heights resident Javier Muniz finally went to urgent care at the L.A. County-USC Medical Center last month.
Physicians at the hospital, which has since been renamed the Los Angeles General Medical Center, realized that Muniz’s medical history included living with HIV. The 46-year-old was diagnosed with giardiasis, an intestinal infection, and was hospitalized for four days while doctors treated his symptoms, drew blood and performed a CT scan.
Hospital officials asked Muniz if he wanted to be one of the first people to participate in LA General’s newly expanded Safer at Home program, which was launched during the pandemic to treat about 4,500 COVID-19 patients at home. In September, the program began including patients with other medical conditions.
A case of shingles can mean two weeks of burning agony for a younger patient. But in older people like Sen. Feinstein, it’s far more likely to last longer.
As of May, at least 556 patients with 37 different diagnoses have participated in the program. They’ve been cared for remotely by a team of several dozen nurses and five physicians, according to hospital officials.
LA General is one of the largest public hospitals in the U.S. and historically has treated medically underserved patients in the region.
“What this is, is concierge-level medicine, which is what rich people are accustomed to getting, but instead we’re giving it to the patients coming to LA General, both because it’s safer for the patients to not have to be in the hospital and it’s a much more patient-centered experience,” said Brad Spellberg, chief medical officer of LA General.
Slightly more than half of the patients were referred from the emergency department and avoided admission altogether; a little fewer than half were hospitalized but discharged much earlier, according to Spellberg.
On average, the program has saved about three hospital days per patient, compared with the typical stay of around five days.
Muniz was sent home with a pre-programmed cellphone that allowed him to communicate with his medical team via audio or video call, as well as equipment including a thermometer and pulse oximeter. Nurses called him several times a day to track his progress, to make sure he was taking his medication properly and on time, and to answer any questions that Muniz had.

“When I’m hospitalized, I get stressed out,” he said. “It makes me just want to leave. It’s scary trying to figure out what’s wrong with oneself and waiting in a room isolated. It’s just not comfortable. Being hospitalized you’re also away from family and friends, and the restrictions on visits make it hard to stay connected to your loved ones.”
The program primarily serves patients with 10 different diagnoses, including skin and bone infections, kidney infections, bacterial and viral pneumonia, asthma and congestive heart failure. But hospital officials have developed a checklist with guiding principles that allows the program to be expanded to other diagnoses, according to Christopher Lynch, medical director of Safer at Home.
The team is looking to expand to 20 diagnoses in the future. The program is covered by the hospital at no cost to the patient.
The program also arranges transportation if needed for patients to their homes or to temporary housing, such as the hospital’s Restorative Care Village, which shelters housing-insecure people who may need a place to recover after receiving medical care, according to Josh Banerjee, associate medical director for the Transitions of Care department at the hospital.
The goal of the program is to send every patient home with a pre-programmed cellphone so they’re able to easily communicate with medical professionals and have their wounds and other injuries examined via video call.
When asked about negative outcomes with the program, hospital officials said there hadn’t been any. They said those enrolled in Safer at Home have had a hospital readmission rate that is “significantly lower” than the rate for all other discharges from the hospital.
The COVID-19 death rate in the U.S. fell by nearly 50% in 2022, a decline credited to widespread vaccinations as well as a rise in natural immunity.
To qualify for the program, patients need to have stable vital signs and be clinically improving. They also need to be able to tolerate taking medications by mouth and can’t have a condition that can only be treated at the hospital.
Muniz said that, as of Tuesday, he was feeling a lot better and would opt for the program again in the future.
“They’re consistently taking care of me,” he said. And, he said, “I’m in the comfort of my own home.”
More to Read
Sign up for Essential California
The most important California stories and recommendations in your inbox every morning.
You may occasionally receive promotional content from the Los Angeles Times.