What you need to know if ‘Modern Family’ has you considering breast reduction
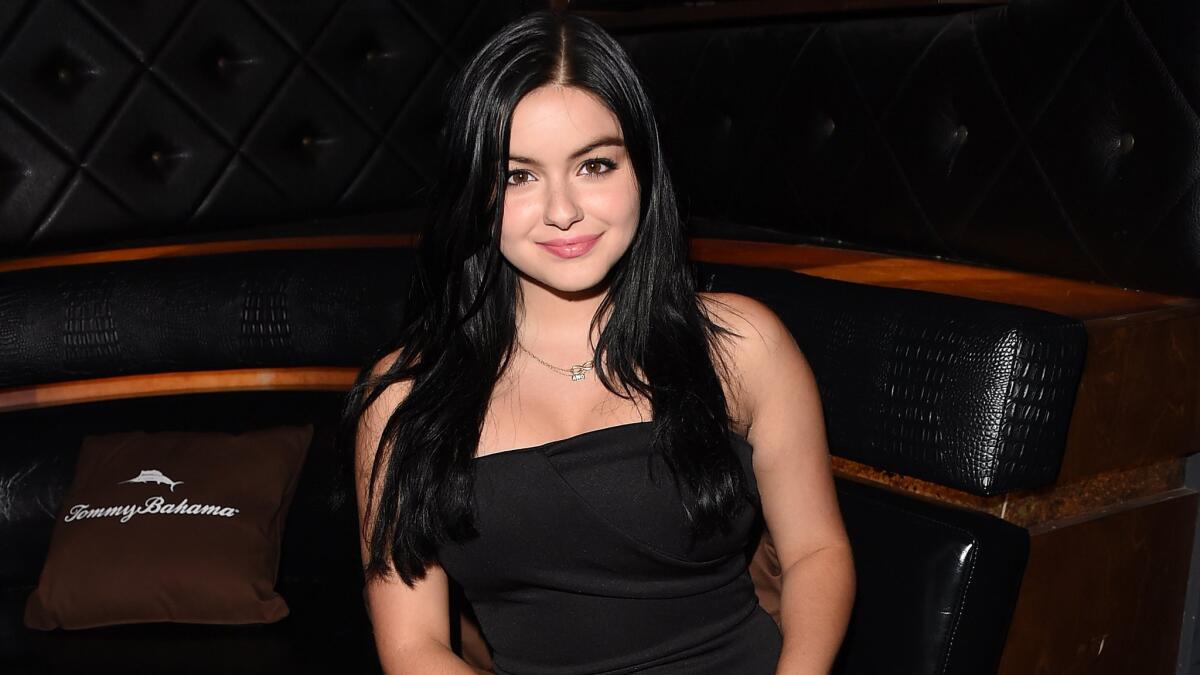
Ariel Winter, seen at a private event hosted by Tommy Bahama during a Taylor Swift concert in Los Angeles on Aug. 22, said she was up and running five days after breast-reduction surgery in June. Others have experienced complications.
- Share via
With 17-year-old “Modern Family” star Ariel Winter about to walk the Emmy red carpet for her first major public appearance since reducing her breast size in June, the media are abuzz with stories about such surgery: celebrities who’ve done it, teens who are doing it and the number of women “coming out” to say how the operation changed their lives.
Indeed, many plastic surgeons refer to breast reduction as a “happy surgery.” Studies rank the operation as having one of the highest patient satisfaction rates among plastic surgery procedures. According to the American Society for Aesthetic Plastic Surgery, more than 114,000 women underwent the procedure in 2014 — a 183% increase since 1997. Women report alleviation of neck and back pain, relief from constant skin irritation, improved ability to exercise and enhanced body image.
------------
For the Record
Sept. 17, 2:50 p.m.: An earlier version of this article incorrectly said Ariel Winter’s first post-surgery public appearance would be at the Emmys on Sunday.
------------
But something is missing from the glossy photos and glowing reviews, says one Los Angeles County resident. “I was shocked to read that Ariel Winter was up and running within five days, trying on dresses a week after her surgery,” says the woman, who also underwent breast reduction surgery in June, decreasing her bra size from a 36HH to a 36D. She asked that her name not be used to protect her privacy.
The experience she describes is different from the one Winter talks of in an interview with Glamour.com last month about her surgery and why she chose it. “Five days after my operation,” says the L.A. County woman, “I was heavily bandaged with drainage tubes. I have yet to go shopping for clothes and won’t until I’m completely healed. I’m still wearing the medical bra 24/7.”
Nearly three months post-surgery, her condition is not the norm — she contracted a bacterial infection, and, in her early 40s, she is decades older than the starlet. Even so, she says the media are doing the average woman a disservice by not painting a fuller picture of the recovery and possible complications.
“Yes, I’m glad I did it — and, yes, it has changed my appearance and is going to make my life better,” she says. “But what I wasn’t expecting was for my recovery to be so protracted and for it to be so painful. This wasn’t highlighted in the media.”
For those considering breast reduction, here is a glimpse into the process:
Reduction techniques
Dr. Michele Shermak, a surgeon at the Plastic Surgery Center of Maryland, compares breast reduction to fitting a pie into a smaller plate. “With breast reduction, we’re removing breast tissue, and we have to reshape the breast. It’s like shaping the pieces of a pie. We have to compress the pie down to a smaller area.”
Surgical techniques differ in where tissue is removed, where it is left behind and the incision pattern in the overlying skin. While it’s common to leave most of the tissue in the lower part of the breast, Dr. Kelly Killeen, a surgeon at Cassileth Plastic Surgery in Beverly Hills, says she tends to leave more in the middle to upper part of the breast, “because it gives ladies a more natural-looking cleavage and shape.”
The two main incision patterns are the “anchor shape” and the “lollipop.” The anchor pattern is the standard technique, where an incision is made around the areola, down the midline and across the bottom of the breast. With the lollipop pattern, an incision is made only around the areola and straight down the midline of the breast, without the third horizontal incision.
“For a very large breast reduction, over 500 or 600 grams, the [anchor shape] is best; a lollipop is best for a smaller breast reduction, between 300 and 500 grams,” says Dr. David Kulber, director of the Plastic Surgery Center of Excellence at Cedars-Sinai Medical Center. “It’s definitely case by case. It depends on scarring versus shape.”
The cost of breast reduction varies widely depending on geographic location and complexity of the procedure. According to the plastic surgery society, the average physician fees for the procedure were $5,521 in 2014 — but this doesn’t include fees from medical facilities, anesthesiologists or laboratories. The total cost for a breast reduction through Cassileth Plastic Surgery in Beverly Hills can range from $9,500 to more than $20,000.
Depending on a patient’s insurance plan, breast reduction may be a covered benefit if a patient can document a medical need. “Patients have to demonstrate that their breasts are large in proportion to their frame and that they have needed medical care because of the size of their breasts — for neck or back pain, rashes under breasts, chronic headaches or difficulty with physical activity,” says Killeen.
Risks and complications
With any surgery, there is inherent risk to going under anesthesia, though the risk is low. Risks of the actual procedure include decreased sensation or loss of sensation in the nipple, infection, poor wound healing, asymmetry and the death of fat tissue in the breast. A scary, but very rare, complication is death of the skin on the nipple, which results in subsequent removal of the nipple.
“Most complications that happen with breast reduction are minor things, not major complications that land you in a hospital,” says Killeen.
Studies looking at breast reduction complications report widely differing rates, ranging from 14% to 52%. “It’s hard to understand what the complication rate is because it’s so variable,” Kulber says. “There is a big difference between a 300-gram reduction versus a 1,300-gram reduction. With bigger reductions, the surgery is more involved. With a smaller reduction, between 300 and 500 grams, the complication rate is less than 5%.”
Kulber adds that many women with large breasts are overweight, so they will also have a higher rate of diabetes and heart disease, which increases the risk of complication.
Shermak was the lead author of a study that reported a trend of higher infection rate and poor wound healing for women who underwent the procedure in their 40s and 50s. Women over age 50 had a significantly higher rate of post-operative complications. While women on hormone replacement therapy fared better, those who’d had a hysterectomy fared worse, suggesting that declining estrogen levels might play a role in poorer healing.
For younger women, one of the main concerns is post-operative difficulty in breast-feeding, though experts disagree on how real the concern is. Some studies have indicated a lower rate of breast-feeding success after reduction surgery, while others have indicated that the success rate is similar to that of women in the general population.
Even with her rocky recovery, the L.A. County woman says she would do the surgery again — which is typical of most patients, says Killeen, adding that breast reduction surgery is one of her favorite operations to perform. “I get to do this procedure that makes people feel better. But the wonderful icing on the cake is that they end up with beautiful, perkier, more youthful-looking breasts in better proportion to their body.”
::
What is the right age for breast reduction surgery?
In looking at potential complications, one might think there is an ideal window of opportunity — after childbearing, to eliminate worries about breast-feeding complications, but before the hormonal decline of menopause. Yet experts say it doesn’t happen that way.
“Women truly get it done at all ages; you don’t have to choose a time,” says Dr. Michele Shermak, a plastic surgeon in Maryland. A 2011 study she led indicated that women in their 40s and 50s had a higher rate of infection and poor wound healing after the procedure, but she emphasizes that higher complication rates in middle-age women reflect mere nuisances, rather than health-threatening emergencies.
Beverly Hills surgeon Dr. Kelly Killeen agrees, saying there is not a cut-off age. Instead, women should ask themselves whether they are healthy candidates. “If a 60-year-old woman is healthy as a horse, her heart looks beautiful on her annual exams and her labs are perfect — why not? Why would you deny her the benefits of breast reduction if she is a good candidate for surgery?” Killeen says.
On the other end of the spectrum are young women like “Modern Family” star Ariel Winter, large-breasted teens who experience medical symptoms and low self-confidence . Though there have been recent claims that an increasing number of teens are undergoing the surgery, data show otherwise. According to the American Society for Aesthetic Plastic Surgery, fewer teens had the surgery in 2014 than in 2005 and, over the last decade, the percentage of breast reduction patients 18 and under has remained steady.
Beyond potential breast-feeding difficulties, surgeons have additional concerns for teenagers considering the procedure. Shermak has operated on 16-year-olds, though she says it’s important to determine whether they are emotionally mature enough to make informed medical decisions.
“Not every teenage girl is ready for it,” she says. “They have to be educated; it’s not like a magic wand. They are going to have scars, they are going to have a recovery. This is not magic — it’s a process, and there are some long-term changes.”
There is also the possibility that a teenager’s breasts will continue to develop after surgery, though Dr. David Kulber, director of the Plastic Surgery Center for Excellence at Cedars-Sinai, says this still shouldn’t preclude them from having the surgery if they are experiencing symptoms. “If you’re operating on a 16-year-old, their breasts may grow and they may need another surgery. But letting them suffer until they’re 21 — I think that’s unacceptable.”
Elise Harrison, a resident of Maryland, had the operation in her mid-40s without complication. Nearing her 50s, she feels better about her body than ever before. Her only regret is that she didn’t have the operation when she was younger. She says, “I would have had more confidence and higher self-esteem earlier in life.”
ALSO:
Nuns in red: What it’s like to ride the AIDS/LifeCycle
New super-foods, from baobab to turkey tail, come with promises and caveats
Biceps curls combined with lunges build your balance too