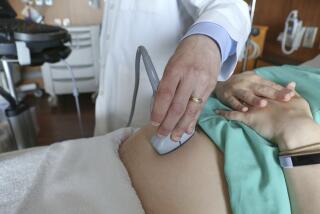
Weighing the risk and rewards of vaginal birth after a C-section

- Share via
In my first pregnancy 21/2 years ago, I was induced at 39 weeks, labored for 29 hours, and ended up with an emergency C-section when I failed to make any progress toward actually giving birth. Since then, I have paid close attention to the vaginal-birth-after-C-section debate because I knew the day would come when I would have to.
One week into this pregnancy’s third trimester, I am still unsure how to approach my delivery.
In March, a National Institutes of Health panel questioned the trend of hospitals and doctors denying women who have had a C-section the chance to try for a vaginal delivery. I agree that women should have the right to try for a VBAC; I’m just not sure if they should try for one. Rather, I’m not sure if I should.
We are quick to pooh-pooh insurance companies, doctors and hospitals who are risk-averse; it seems obvious that they are hard-hearted scaredy-cats and we are victims. It seems we should fight to be able to attempt a “normal” birth, or seize it when it’s offered.
But to know what we’re fighting for, we must be more honest with the terms we use. The women who have had C-sections and who are lobbying for a vaginal birth would like a vaginal birth, yes. But what they’re asking for, the more honest and maybe the more uncomfortable way to say it, is that they want to give it a shot. They want a TOLAC, a trial of labor after a C-section.
Calling a TOLAC a VBAC may be part of the problem with the debate: The terminology itself comes with an optimism to it, the idea that if only you were permitted to try, you would succeed.
I’m not arguing semantics to be difficult. It’s just that, in reality, only about 60% to 80% of women who have had a C-section and attempt a vaginal birth actually have one. The other 20% to 40% end up with another C-section — or, sometimes, a uterine rupture.
When a uterus ruptures, which it does in 1% of patients who are attempting a vaginal birth after a previous C-section, things go wrong fast — and they go wrong big. An obstetrician specializing in high-risk pregnancies told me that one-fourth of uterine ruptures end in hysterectomies, brain damage to the baby or even the baby’s death. Yes, this is only a quarter of 1%. But, as that doctor said to me, “The risk may be low, but it’s 100% when it’s happening to you.”
C-sections have risks too — infection, bowel problems, embolism, reaction to anesthesia and, of course, the risk of death that accompanies any major surgery. But even a second or third C-section in a youngish, healthy woman is fairly safe.
So why am I even considering an attempt at a vaginal birth? Why would anyone?
One friend of mine told me she wanted to attempt a vaginal birth after an earlier C-section because she had a primal need to give birth vaginally. Another one thinks it’s healthier for both her and her baby. And a third friend told me her doctor was so nonchalant that she saw no reason not to attempt one.
I too would like a chance at a “normal” experience — not just because my first delivery went so wrong but because I found my C-section terrifying. I concede that if I hadn’t just been through 30 hours of labor, it might have been less traumatic, but the smells, the sounds, the very fact of knowing what was going on …
Vaginal birth is no walk in the park, from what I hear. But I didn’t enter childbearing with the impression that it would be fun or painless.
The question that I — and everyone fighting for a trial of labor — must ask is this: If I attempt a vaginal birth and my baby suffers brain damage or dies, will it have been worth the risk?
The almost-unborn child is at the height of potential in his mother’s womb. Right now, I believe my unborn child can be anything he wants to be. Am I going to spoil his chances so that I wouldn’t ever have to smell my insides being soldered together again? Would I risk it all so that I don’t have to risk those awful 45 minutes again?
These questions are ones we must consider, and they’re left off the VBAC consent form that my doctor gave me a few weeks ago, the one that the hospital requires a woman to sign before she attempts a vaginal delivery following a C-section.
That’s not to say women suffer from a shortage of people offering advice. On one end are proponents of the all-natural-all-the-way approach telling us that our bodies were meant to give birth. On the other end are the trust-in-modern-medicine adherents who say that C-sections are easy and safe. In between are the personal moving narratives and the horror stories, each leading to a supposedly clear choice.
The one answer no one can provide is which option will give me, with the least amount of intervention, the reasonable guarantee of a healthy child and a healthy me.
Despite my research, I don’t feel qualified to make that decision. Nor do I feel that my doctor should make it for me. Someone’s got to, though, so I look to my gut, the mother’s intuition that parenting books say I should already possess.
Here is what I come up with: a fantasy in which my husband and I — a couple of months in the future — are leaning over our new baby, counting his fingers and toes. In this vision, he has been born in a delivery room, not an operating room.
In a few weeks, I’ll have a sonogram. My doctor will assess the locations of my uterine scar and placenta, and the position of my baby, and if all is right, he’ll tell me that my chances for a successful trial of labor are good. If they are, and I don’t have any other factors that might indicate a need for a C-section, I will take those chances.
That’s not to say I don’t worry that, after months of dissecting the data and interpreting the information that’s out there, I have less of a chance of success than other women attempting the same thing. Though I can’t find studies to prove it, I suspect that at least part of the success regarding a VBAC may be a function of the optimism I mentioned earlier. Increased knowledge has a way of decreasing hope sometimes.
My work now, then, is to stop gathering new information. It is time to wash some infant clothing, hang that new mobile in the nursery, install the infant car seat. In about 10 weeks, doing activities as mundane as these, I will feel the squeeze of contractions or the gush of broken water — spontaneous signs of labor that I never got to experience the first time. I will let my body do what I’ve been promised it will, and I will be grateful for the doctors who are on call in the case that nature isn’t.
Brodesser-Akner is a freelance writer living and gestating in Los Angeles.